Abstract
The new guideline on acute coronary syndrome (ACS) of the European Society of Cardiology (ESC) replaces two separate guidelines on ST-elevation myocardial infarction (STEMI) and non-ST-elevation (NSTE) ACS. This change of paradigm reflects the experts view that the ACS is a continuum, starting with unstable angina and ending in cardiogenic shock or cardiac arrest due to severe myocardial ischemia. Secondary, partly non-atherosclerotic-caused myocardial infarctions (“type 2”) are not integrated in this concept.
With respect to acute care in the setting of emergency medicine and the chest pain unit structures, the following new aspects have to be taken into account:
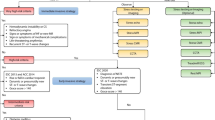
1. New procedural approach as “think A.C.S.” meaning “abnormal ECG,” “clinical context,” and “stable patient”
2. New recommendation regarding a holistic approach for frail patients
3. Revised recommendations regarding imaging and timing of invasive strategy in suspected NSTE-ACS
4. Revised recommendations for antiplatelet and anticoagulant therapy in STEMI
5. Revised recommendations for cardiac arrest and out-of-hospital cardiac arrest
6. Revised recommendations for in-hospital management (starting in the CPU/ED) and ACS comorbid conditions
In summary, the changes are mostly gradual and are not based on extensive new evidence, but more on focused and healthcare process-related considerations.
Zusammenfassung
Die neue Leitlinie zum akuten Koronarsyndrom (ACS) der Europäischen Gesellschaft für Kardiologie (ESC) ersetzt 2 separate Leitlinien zum ST-Hebungs-Infarkt („ST-elevation myocardial infarction“, STEMI) und zum ACS ohne ST-Hebungen („non-ST-elevation“, NSTE-ACS). Dieser Paradigmenwechsel spiegelt die Expertenperspektive wider, dass das ACS ein Kontinuum darstellt, das mit einer instabilen Angina pectoris beginnt und mit einem kardiogenen Schock oder Herzstillstand aufgrund einer schweren Myokardischämie endet. Sekundäre, teilweise nichtatherosklerotisch bedingte Myokardinfarkte („Typ 2“) sind in dieses Konzept nicht integriert. Im Hinblick auf die Akutversorgung im Rahmen der Notfallmedizin und der Chest-Pain-Unit-Strukturen (CPU) sind folgende neue Aspekte zu berücksichtigen:
1. Neuer prozessualer Ansatz als „think A.C.S.“, d. h. „abnormales EKG“, „klinischer Kontext“ und „stabiler Patient“
2. Neue Empfehlung für einen ganzheitlichen Ansatz bei gebrechlichen Patienten
3. Überarbeitete Empfehlungen zur Bildgebung und zum Zeitpunkt der invasiven Strategie bei Verdacht auf NSTE-ACS
4. Überarbeitete Empfehlungen zur Thrombozytenaggregationshemmer- und Antikoagulanzientherapie bei STEMI
5. Revidierte Empfehlungen für Herzstillstand und außerklinischen Herzstillstand
6. Überarbeitete Empfehlungen für das Management im Krankenhaus (beginnend in der Notaufnahme/CPU) und für ACS-Komorbiditäten
Zusammenfassend lässt sich sagen, dass die Änderungen größtenteils schrittweise erfolgen und nicht auf massiven neuen Erkenntnissen beruhen, sondern eher auf gezielten und prozessbezogenen Überlegungen zum Versorgungsprozess.

Similar content being viewed by others
References
Byrne RA, Rossello X, Coughlan JJ et al (2023) 2023 ESC Guidelines for the management of acute coronary syndromes. Eur Heart J 44(38):3720–3826
Apple FS, Wu AH, Mair J et al (2005) Future biomarkers for detection of ischemia and risk stratification in acute coronary syndrome. Clin Chem 51(5):810–824
Searle J, Danne O, Müller C, Mockel M (2011) Biomarkers in acute coronary syndrome and percutaneous coronary intervention. Minerva Cardioangiol 59(3):203–223
Collet JP, Thiele H, Barbato E et al (2021) 2020 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Eur Heart J 42(14):1289–1367
Giannitsis E, Blankenberg S, Christenson RH et al (2021) Critical appraisal of the 2020 ESC guideline recommendations on diagnosis and risk assessment in patients with suspected non-ST-segment elevation acute coronary syndrome. Clin Res Cardiol 110(9):1353–1368
Chung K, Wilkinson C, Veerasamy M, Kunadian V (2021) Frailty scores and their utility in older patients with cardiovascular disease. Interv Cardiol 16:e5
Rockwood K, Song X, MacKnight C et al (2005) A global clinical measure of fitness and frailty in elderly people. Cmaj 173(5):489–495
Ekerstad N, Pettersson S, Alexander K et al (2018) Frailty as an instrument for evaluation of elderly patients with non-ST-segment elevation myocardial infarction: a follow-up after more than 5 years. Eur J Prev Cardiol 25(17):1813–1821
Yoshioka N, Takagi K, Morita Y et al (2019) Impact of the clinical frailty scale on mid-term mortality in patients with ST-elevated myocardial infarction. Int J Cardiol Heart Vasc 22:192–198
Lee KK, Bularga A, O’Brien R et al (2021) Troponin-guided coronary computed tomographic angiography after exclusion of myocardial infarction. J Am Coll Cardiol 78(14):1407–1417
Thygesen K, Alpert JS, Jaffe AS et al (2019) Fourth universal definition of myocardial infarction (2018). Eur Heart J 40(3):237–269
Giannitsis E, Garfias-Veitl T, Slagman A et al (2022) Biomarkers-in-cardiology 8 RE-VISITED-consistent safety of early discharge with a dual marker strategy combining a normal hs-cTnT with a normal copeptin in low-to-intermediate risk patients with suspected acute coronary syndrome—a secondary analysis of the randomized biomarkers-in-cardiology 8 trial. Cells 11(2)
Lindner T, Slagman A, Senkin A et al (2015) Medical history of elderly patients in the emergency setting: not an easy point-of-care diagnostic marker. Emerg Med Int 2015:490947
Möckel M, Searle J, Hamm C et al (2015) Early discharge using single cardiac troponin and copeptin testing in patients with suspected acute coronary syndrome (ACS): a randomized, controlled clinical process study. Eur Heart J 36(6):369–376
Riedlinger D, Möckel M, Müller C et al (2018) High-sensitivity cardiac troponin T for diagnosis of NSTEMI in the elderly emergency department patient: a clinical cohort study. Biomarkers 23(6):551–557
Searle J, Slagman A, Stockburger M et al (2015) Use of copeptin in emergency patients with cardiac chief complaints. Eur Heart J Acute Cardiovasc Care 4(5):393–402
Slagman A, Searle J, Müller C, Möckel M (2015) Temporal release pattern of copeptin and troponin T in patients with suspected acute coronary syndrome and spontaneous acute myocardial infarction. Clin Chem 61(10):1273–1282
Vafaie M, Slagman A, Möckel M et al (2016) Prognostic value of undetectable hs Troponin T in suspected acute coronary syndrome. Am J Med 129(3):274–282.e2
Montalescot G, van ’t Hof AW, Lapostolle F et al (2014) Prehospital ticagrelor in ST-segment elevation myocardial infarction. N Engl J Med 371(11):1016–1027
Möckel M (2023) Perspectives on cardiovascular biomarkers: one fits all biomarkers are out, personalization is in. Biomarkers 28(4):353
Möckel M (2020) One fits all hs troponin or more personalized dual markers strategies in the primary diagnostic assessment of patients with suspected acute coronary syndrome? Biomarkers 25(8):611–612
Möckel M (2022) Actual guidelines on non-ST-elevation acute coronary syndrome: how do they help in the emergency department? Eur J Emerg Med 29(1):2–4
Dörler J, Edlinger M, Alber HF et al (2011) Clopidogrel pre-treatment is associated with reduced in-hospital mortality in primary percutaneous coronary intervention for acute ST-elevation myocardial infarction. Eur Heart J 32(23):2954–2961
Lapostolle F, Van’t Hof AW, Hamm CW et al (2019) Morphine and ticagrelor interaction in primary percutaneous coronary intervention in ST-segment elevation myocardial infarction: ATLANTIC-morphine. Am J Cardiovasc Drugs 19(2):173–183
Desch S, Freund A, Akin I et al (2021) Angiography after out-of-hospital cardiac arrest without ST-segment elevation. N Engl J Med 385(27):2544–2553
Desch S, Freund A, Akin I et al (2023) Coronary angiography after out-of-hospital cardiac arrest without ST-segment elevation: one-year outcomes of a randomized clinical trial. JAMA Cardiol 8(9):827–834
Lemkes JS, Janssens GN, van der Hoeven NW et al (2019) Coronary angiography after cardiac arrest without ST-segment elevation. N Engl J Med 380(15):1397–1407
Lemkes JS, Janssens GN, van der Hoeven NW et al (2020) Coronary angiography after cardiac arrest without ST segment elevation: one-year outcomes of the COACT randomized clinical trial. JAMA Cardiol 5(12):1358–1365
Hassager C, Schmidt H, Møller JE et al (2023) Duration of device-based fever prevention after cardiac arrest. N Engl J Med 388(10):888–897
Bharadwaj A, Potts J, Mohamed MO et al (2020) Acute myocardial infarction treatments and outcomes in 6.5 million patients with a current or historical diagnosis of cancer in the USA. Eur Heart J 41(23):2183–2193
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
M. Möckel declares speakers honoraria and consulting fees from BRAHMS GmbH, Roche Diagnostics and AstraZeneca and research support from Roche Diagnostics.
For this review article no studies with human participants or animals were performed by any of the authors. All studies mentioned were in accordance with the ethical standards indicated in each case.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Möckel, M. The new ESC acute coronary syndrome guideline and its impact in the CPU and emergency department setting. Herz 49, 185–189 (2024). https://doi.org/10.1007/s00059-024-05241-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-024-05241-6