Abstract
Background
Physical frailty and cognitive impairment are prevalent globally, particularly in China, which is experiencing an unprecedented aging of its large population.
Objectives
Examine the association between physical frailty and the level and rate of change of cognitive function, globally and by domain, among community-dwelling Chinese older adults, and quantify the mediation effects from activities of daily living (ADL) limitations and depressive symptoms.
Design
Longitudinal.
Setting
China Health and Retirement Longitudinal Study (2011–2018).
Participants
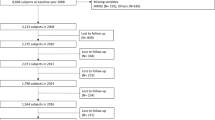
5,431 eligible adults aged ≥ 60 years with valid information on physical frailty.
Measurements
Physical frailty, cognitive function, ADL limitations, and depressive symptoms were respectively assessed by frailty phenotypes, the Telephone Interview for Cognitive Status (episodic memory, executive function, and orientation), performance in six daily tasks, and the eight-item Center for Epidemiological Studies Depression Scale. Latent growth curve models were used to address the objectives.
Results
Compared to adults who were non-frail, those who were pre-frail (β = −0.06) and frail (β = −0.13) reported significantly worse global cognitive function and episodic memory (pre-frail: β = −0.05; frail: β = −0.14), executive function (pre-frail: β = −0.04, frail: β = −0.10), and orientation (pre-frail: β = −0.06; frail: β = −0.07) at baseline; those who were frail were more likely to experience faster decline in global cognitive function (β = 0.12) and episodic memory (β = 0.08). ADL limitations (β = −0.07) and depressive symptoms (β = −0.14) significantly mediated the association between physical frailty and the level of cognitive function, but not its rate of decline.
Conclusions
Intervention strategies that help maintain cognitive function may benefit from early screening and assessment of physical frailty. For pre-frail and frail older Chinese adults, programs designed to help improve or maintain activities of daily living and reduce number of depressive symptoms may contribute to better cognitive performance.

Similar content being viewed by others
References
National Bureau of Statistics of the People’s Republic of China. China Statistical Yearbook. Published 2018. Accessed January 26, 2022. http://www.stats.gov.cn/tjsj/ndsj/2018/indexeh.htm
Zhang Y, Xu Y, Nie H, et al. Prevalence of dementia and major dementia subtypes in the Chinese populations: A meta-analysis of dementia prevalence surveys, 1980–2010. Journal of Clinical Neuroscience. 2012;19(10):1333–1337. doi:https://doi.org/10.1016/j.jocn.2012.01.029
Shimada H, Doi T, Lee S, Makizako H, Chen LK, Arai H. Cognitive frailty predicts incident dementia among community-dwelling older people. Journal of Clinical Medicine. 2018;7(9). doi:https://doi.org/10.3390/jcm7090250
Clegg A, Young J, Iliffe S, Rikkert MO, Rockwood K. Frailty in elderly people. In: The Lancet. Vol 381. Elsevier B.V.; 2013:752–762. doi:https://doi.org/10.1016/S0140-6736(12)62167-9
Fried LP, Tangen CM, Walston J, et al. Frailty in Older Adults: Evidence for a Phenotype. Vol 56.; 2001. https://academic.oup.com/biomedgerontology/article/56/3/M146/545770
Kojima G. Quick and simple FRAIL scale Predicts incident activities of daily living (ADL) and instrumental ADL (IADL) disabilities: a systematic review and meta-analysis. J Am Med Dir Assoc. 2018;19(12):1063–1068. doi:https://doi.org/10.1016/j.jamda.2018.07.019
Kojima G, Iliffe S, Walters K. Frailty index as a predictor of mortality: A systematic review and meta-analysis. Age and Ageing. 2018;47(2):193–200. doi:https://doi.org/10.1093/ageing/afx162
Ma L, Zhang L, Sun F, Li Y, Tang Z. Cognitive function in prefrail and frail community-dwelling older adults in China. BMC Geriatrics. 2019;19(1). doi:https://doi.org/10.1186/s12877-019-1056-8
Robertson DA, Savva GM, Kenny RA. Frailty and cognitive impairment-a review of the evidence and causal mechanisms. Ageing Research Reviews. 2013;12(4):840–851. doi:https://doi.org/10.1016/j.arr.2013.06.004
Yuan Y, Lapane KL, Tjia J, Baek J, Liu SH, Ulbricht CM. Physical frailty and cognitive impairment in older nursing home residents: a latent class analysis. BMC Geriatrics. 2021;21(1). doi:https://doi.org/10.1186/s12877-021-02433-1
Boyle PA, Buchman AS, Wilson RS, Leurgans SE, Bennett DA. Physical frailty is associated with incident mild cognitive impairment in community-based older persons. J Am Geriatr Soc. 2010;58(2):248–255. doi:https://doi.org/10.1111/j.1532-5415.2009.02671.x
Buchman AS, Boyle P, Wilson RS, Tang Y, Bennett DA. Frailty is associated with incident Alzheimer’s disease and cognitive decline in the elderly. Psychosomatic Medicine. 2007;69:483–489.
Samper-Ternent R, al Snih S, Raji MA, Markides KS, Ottenbacher KJ. Relationship between frailty and cognitive decline in older Mexican Americans. J Am Geriatr Soc. 2008;56(10):1845–1852. doi:https://doi.org/10.1111/j.1532-5415.2008.01947.x
Drame M, NovéLLa J, Jolly D, et al. Rapid cognitive decline, one-year institutional admission and one-year mortality: Analysis of the ability to predict and inter-tool agreement of four validated clinical frailty indexes in the safes cohort. J Nutr Health Aging. 2010;15(8):699–705. doi:doi:https://doi.org/10.1007/s12603-011-0164-8
Bunce D, Batterham PJ, MacKinnon AJ. Long-term Associations between Physical Frailty and Performance in Specific Cognitive Domains. Journals of Gerontology — Series B Psychological Sciences and Social Sciences. 2019;74(6):919–926. doi:https://doi.org/10.1093/geronb/gbx177
Langlois F, Vu TTM, Kergoat MJ, Chassé K, Dupuis G, Bherer L. The multiple dimensions of frailty: Physical capacity, cognition, and quality of life. International Psychogeriatrics. 2012;24(9):1429–1436. doi:https://doi.org/10.1017/S1041610212000634
Macuco CRM, Batistoni SST, Lopes A, et al. Mini-Mental State Examination performance in frail, pre-frail, and non-frail community dwelling older adults in Ermelino Matarazzo, So Paulo, Brazil. International Psychogeriatrics. 2012;24(11):1725–1731. doi:https://doi.org/10.1017/S1041610212000907
Gray SL, Anderson ML, Hubbard RA, et al. Frailty and incident dementia. Journals of Gerontology — Series A Biological Sciences and Medical Sciences. 2013;68(9):1083–1090. doi:https://doi.org/10.1093/gerona/glt013
Kojima G, Taniguchi Y, Iliffe S, Walters K. Frailty as a Predictor of Alzheimer Disease, Vascular Dementia, and All Dementia Among Community-Dwelling Older People: A Systematic Review and Meta-Analysis. J Am Med Dir Assoc. 2016;17(10):881–888. doi:https://doi.org/10.1016/j.jamda.2016.05.013
Zhao X, Li D, Zhang Q, Liu H. Spousal concordance in frailty predicting mental and functional health decline: A four-year follow-up study of older couples in urban and rural China. Journal of Clinical Nursing. Published online 2021. doi:https://doi.org/10.1111/jocn.15927
Kojima G. Frailty as a predictor of disabilities among community-dwelling older people: a systematic review and meta-analysis. Disability and Rehabilitation. 2017;39(19):1897–1908. doi:https://doi.org/10.1080/09638288.2016.1212282
Vermeulen J, Neyens JC, van Rossum E, Spreeuwenberg MD, de Witte LP. Predicting ADL disability in community-dwelling elderly people using physical frailty indicators: A systematic review. BMC Geriatrics. 2011;11. doi:https://doi.org/10.1186/1471-2318-11-33
Buigues C, Padilla-Sánchez C, Fernández Garrido J, Navarro-Martínez R, Ruiz-Ros V, Cauli O. The relationship between depression and frailty syndrome: A systematic review. Aging and Mental Health. 2015;19(9):762–772. doi:https://doi.org/10.1080/13607863.2014.967174
Soysal P, Veronese N, Thompson T, et al. Relationship between depression and frailty in older adults: A systematic review and meta-analysis. Ageing Research Reviews. 2017;36:78–87. doi:https://doi.org/10.1016/j.arr.2017.03.005
Collard RM, Comijs HC, Naarding P, et al. Frailty as a Predictor of the Incidence and Course of Depressed Mood. J Am Med Dir Assoc. 2015;16(6):509–514. doi:https://doi.org/10.1016/j.jamda.2015.01.088
Feng L, Nyunt MSZ, Feng L, Yap KB, Ng TP. Frailty predicts new and persistent depressive symptoms among community-dwelling older adults: Findings from singapore longitudinal aging study. J Am Med Dir Assoc. 2014;15(1):76.e7-76.e12. doi:https://doi.org/10.1016/j.jamda.2013.10.001
Liu H, Li D, Zhao X, Fang B, Zhang Q, Li T. Longitudinal impact of frailty states and sleep duration on subsequent depressive symptoms of older adults. J Am Geriatr Soc. 2021;69(4):1003–1011. doi:https://doi.org/10.1111/jgs.16999
Rajan KB, Hebert LE, Scherr PA, Mendes De Leon CF, Evans DA. Disability in basic and instrumental activities of daily living is associated with faster rate of decline in cognitive function of older adults. Journals of Gerontology — Series A Biological Sciences and Medical Sciences. 2013;68(5):624–630. doi:https://doi.org/10.1093/gerona/gls208
Saenz JL, Garcia MA, Downer B. Late life depressive symptoms and cognitive function among older Mexican adults: the past and the present. Aging and Mental Health. 2020;24(3):413–422. doi:https://doi.org/10.1080/13607863.2018.1544214
Yang X, Pan A, Gong J, et al. Prospective associations between depressive symptoms and cognitive functions in middle-aged and elderly Chinese adults. Journal of Affective Disorders. 2020;263:692–697. doi:https://doi.org/10.1016/j.jad.2019.11.048
van den Kommer TN, Comijs HC, Aartsen MJ, Huisman M, Deeg DJH, Beekman ATF. Depression and cognition: How do they interrelate in old age? American Journal of Geriatric Psychiatry. 2013;21(4):398–410. doi:https://doi.org/10.1016/j.jagp.2012.12.015
Potter GG, McQuoid DR, Whitson HE, Steffens DC. Physical frailty in late-life depression is associated with deficits in speed-dependent executive functions. International Journal of Geriatric Psychiatry. 2016;31(5):466–474. doi:https://doi.org/10.1002/gps.4351
Crimmins EM, Kim JK, Langa KM, Weir DR. Assessment of cognition using surveys and neuropsychological assessment: the Health and Retirement Study and the Aging, Demographics, and Memory Study. J Gerontol B Psychol Sci Soc Sci. 2011;66 Suppl 1. doi:https://doi.org/10.1093/geronb/gbr048
Wu C, Smit E, Xue QL, Odden MC. Prevalence and correlates of frailty among community-dwelling Chinese older adults: The China health and retirement longitudinal study. Journals of Gerontology — Series A Biological Sciences and Medical Sciences. 2018;73(1):102–108. doi:https://doi.org/10.1093/gerona/glx098
Pedersen A, Mikkelsen E, Cronin-Fenton D, et al. Missing data and multiple imputation in clinical epidemiological research. Clinical Epidemiology. 2017;9:157–166.
Buchman A, Schneider J, Leurgans S, Bennett D. Physical frailty in older persons is associated with Alzheimer disease pathology. Neurlogy. 2008;71(7):499–504.
Kelaiditi E, Cesari M, Canevelli M, van Kan G, Ousset P, Gillette-Guyonnet S. Cognitive frailty: rational and definition from an (IANA/IAGG) international consensus group. The Journal of Nutrition, Health & Aging. 2013;17(9):726–734.
Chu NM, Bandeen-Roche K, Xue QL, Carlson MC, Sharrett AR, Gross AL. Physical frailty phenotype criteria and their synergistic association on cognitive functioning. Journals of Gerontology — Series A Biological Sciences and Medical Sciences. 2021;76(9):1633–1642. doi:https://doi.org/10.1093/gerona/glaa267
Weir D, Lay M, Langa K. Economic development and gender inequality in cognition: A comparison of China and India, and of SAGE and the HRS sister studies. Journal of the Economics of Ageing. 2014;4:114–125. doi:https://doi.org/10.1016/j.jeoa.2014.08.002
Arts MHL, Collard RM, Comijs HC, et al. Physical Frailty and Cognitive Functioning in Depressed Older Adults: Findings From the NESDO Study. J Am Med Dir Assoc. 2016;17(1):36–43. doi:https://doi.org/10.1016/j.jamda.2015.07.016
Li M, Huang Y, Liu Z, et al. The association between frailty and incidence of dementia in Bei**g: Findings from 10/66 dementia research group population-based cohort study. BMC Geriatrics. 2020;20(1). doi:https://doi.org/10.1186/s12877-020-01539-2
Petermann-Rocha F, Lyall DM, Gray SR, et al. Associations between physical frailty and dementia incidence: a prospective study from UK Biobank. The Lancet Healthy Longevity. 2020;1(2):e58–e68. doi:https://doi.org/10.1016/S2666-7568(20)30007-6
Ávila-Funes JA, Amieva H, Barberger-Gateau P, le Goff M, Raoux N, Ritchie K. Cognitive impairment improves the predictive validity of the phenotype of frailty for adverse health outcomes: The three-city study. J Am Geriatr Soc. 2009;57(3):453–461.
Feng L, Nyunt MSZ, Gao Q, et al. Physical frailty, cognitive impairment, and the risk of neurocognitive disorder in the Singapore longitudinal ageing studies. Journals of Gerontology — Series A Biological Sciences and Medical Sciences. 2017;72(3):369–375. doi:https://doi.org/10.1093/gerona/glw050
Collard RM, Comijs HC, Naarding P, et al. Frailty as a Predictor of the Incidence and Course of Depressed Mood. J Am Med Dir Assoc. 2015;16(6):509–514. doi:https://doi.org/10.1016/j.jamda.2015.01.088
Makizako H, Shimada H, Doi T, et al. Physical frailty predicts incident depressive symptoms in elderly people: Prospective findings from the obu study of health promotion for the elderly. J Am Med Dir Assoc. 2015;16(3):194–199. doi:https://doi.org/10.1016/j.jamda.2014.08.017
Raji MA, Reyes-Ortiz CA, Kuo YF, Markides KS, Ottenbacher KJ. Depressive symptoms and cognitive change in older Mexican Americans. Journal of Geriatric Psychiatry and Neurology. 2007;20(3):145–152. doi:https://doi.org/10.1177/0891988707303604
Sachs-Ericsson N, Joiner T, Ashby Plant E, Blazer DG. The Influence of Depression on Cognitive Decline in Community-Dwelling Elderly Persons. Vol 13.; 2005.
Zhu Y, Li C, **e W, Zhong B, Wu Y, Blumenthal JA. Trajectories of depressive symptoms and subsequent cognitive decline in older adults: a pooled analysis of two longitudinal cohorts. Age and Ageing. Published online 2021.
Fairhall N, Kurrle SE, Sherrington C, Lord SR, Lockwood K, John B. Effectiveness of a multifactorial intervention on preventing development of frailty in pre-frail older people: study protocol for a randomised controlled trial. BMJ Open. 2015;5(2).
Dedeyne L, Deschodt M, Verschueren S, Tournoy J, Gielen E. Effects of multi-domain interventions in (pre)frail elderly on frailty, functional, and cognitive status: A systematic review. Clinical Interventions in Aging. 2017;12:873–896. doi:https://doi.org/10.2147/CIA.S130794
Seino S, Nishi M, Murayama H, et al. Effects of a multifactorial intervention comprising resistance exercise, nutritional and psychosocial programs on frailty and functional health in community-dwelling older adults: A randomized, controlled, cross-over trial. Geriatr Gerontol Int. 2017;17(11):2034–2045.
de Souto Barreto P, Rolland Y, Maltais M, Vellas B. Associations of Multidomain Lifestyle Intervention with Frailty: Secondary Analysis of a Randomized Controlled Trial. American Journal of Medicine. 2018;131(11):1382.e7-1382.e13. doi:https://doi.org/10.1016/j.amjmed.2018.06.002
Meng X, Li G, Zhang G, et al. Effects of dance intervention on frailty among older adults. Archives of Gerontology and Geriatrics. 2020;88. doi:https://doi.org/10.1016/j.archger.2019.104001
Zhang Y, Zhang Y, Du S, Wang Q, **a H, Sun R. Exercise interventions for improving physical function, daily living activities and quality of life in community-dwelling frail older adults: A systematic review and meta-analysis of randomized controlled trials. Geriatric Nursing. 2020;41(3):261–273. doi:https://doi.org/10.1016/j.gerinurse.2019.10.006
Chen YY, Wong GHY, Lum TY, et al. Neighborhood support network, perceived proximity to community facilities and depressive symptoms among low socioeconomic status Chinese elders. Aging and Mental Health. 2016;20(4):423–431. doi:https://doi.org/10.1080/13607863.2015.1018867
Joo JH, Hwang S, Abu H, Gallo JJ. An innovative model of depression care delivery: Peer mentors in collaboration with a mental health professional to relieve depression in older adults. American Journal of Geriatric Psychiatry. 2016;24(5):407–416. doi:https://doi.org/10.1016/j.jagp.2016.02.002
Lai DWL, Li J, Ou X, Li CYP. Effectiveness of a peer-based intervention on loneliness and social isolation of older Chinese immigrants in Canada: A randomized controlled trial. BMC Geriatrics. 2020;20(1). doi:https://doi.org/10.1186/s12877-020-01756-9
**e B, Ma C, Chen Y, Wang J. Prevalence and risk factors of the co-occurrence of physical frailty and cognitive impairment in Chinese community-dwelling older adults. Health and Social Care in the Community. 2021;29(1):294–303. doi:https://doi.org/10.1111/hsc.13092
Xue QL, Buta B, Ma L, Ge M, Carlson M. Integrating frailty and cognitive phenotypes: why, how, now what? Curr Geriatr Rep. 2019;8(2):97–106.
Acknowledgments
This analysis uses data from the Harmonized CHARLS dataset and Codebook, Version D as of June 2021, developed by the Gateway to Global Aging Data. The development of the Harmonized CHARLS was funded by the National Institute on Aging (R01 AG030153, RC2 AG036619, R03 AG043052). For more information, please refer to https://g2aging.org/.
Funding
Funding information: Yiyang Yuan was supported by National Institute on Aging (grant number 5F99AG068591).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical standards: This was a secondary data analysis of existing datasets that did not involve human subjects.
Additional information
Conflict of interest: All authors declare that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Peng, C., Burr, J.A., Yuan, Y. et al. Physical Frailty and Cognitive Function among Older Chinese Adults: The Mediating Roles of Activities of Daily Living Limitations and Depression. J Frailty Aging 12, 156–165 (2023). https://doi.org/10.14283/jfa.2023.1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.14283/jfa.2023.1