Abstract
Background
Beta thalassemia major (β-TM) is a common cause of skeletal morbidity and is associated with increased bone fracture risk, particularly in inadequately transfused children. The aim of this study was to investigate some potential biochemical markers as possible early predictors of BMD variations in children with β-TM.
Methods
The study included 38 children with β-TM and 40 sex-age matched controls. All patients were subjected to BMD assessment by dual-energy X-ray absorptiometry (DEXA). Serum beta-crosslaps (beta-CTx), osteoprotegerin (OPG), receptor activator of nuclear factor-kappa B ligand (RANKL), urinary deoxypyridinoline (DPD) and ferritin levels were compared between the groups.
Results
Serum OPG levels were significantly lower in thalassemic children than in controls. The mean ratio of RANKL/OPG was significantly higher in the thalassemic patients than in the control group. Osteoporosis was detected in 10 (3 female and 7 male) of 38 patients (26.3%) according to the femur Z score and in 6 of them (4 male and 2 female) (15.8%) according to the spine Z score.
Conclusions
Serum OPG concentrations can be used as a biochemical marker in screening patients with beta-thalassemia major for the development of osteoporosis.
Similar content being viewed by others
What is already known about this topic?
It is well known that beta-thalassemia major is associated with a number of comorbidities, including osteoporosis. Screening children with beta-thalassemia major for osteoporosis with dual-energy X-ray absorptiometry (DEXA) is necessary for detecting osteoporosis and improving bone health. However, DEXA is a radiological tool with X-ray exposure that is not available in every centre. Therefore, there is a need for biochemical markers.
What does this study add?
This study shows that serum osteoprotegerin concentrations can be used as a biochemical marker in screening patients with beta-thalassemia major for the development of osteoporosis.
Background
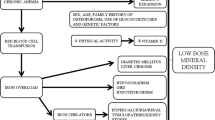
Beta thalassemia major (β-TM) is a common cause of skeletal morbidity and increased bone fracture risk in thalassemic patients [1]. Its pathogenesis is multifactorial and mainly includes bone marrow expansion, endocrine dysfunction and iron overload [20, 21]. In a study conducted on patients with sickle cell anaemia, the mean lumbar spine Z score was significantly lower in prepubertal girls than in boys. However, there was no significant difference in the pubertal group [22]. When the prepubertal thalassemic patients in this study were evaluated according to sex, the mean spine DEXA Z score results were higher in females than males. In contrast, the mean femur Z score was higher in males than females.
Iron accumulation has a negative effect on bone mineralisation. BMD was significantly influenced by noneffective chelation in children with beta-thalassemia major [23]. According to the results of this study, it was confirmed that DEXA Z scores similarly decreased with increasing levels of ferritin.
Limitations
One of the most important limitations of the study is that the participants were not homogeneous in terms of the duration of thalassemia disease. This may affect the degree of osteoporosis in these patients, and thus the correlation between osteoporosis and the potential markers studied. The inability to perform DEXA examination in healthy controls is another important limitation. The possibility of osteoporosis among these patients may confound the comparisons between patients with β-TM and healthy controls. Therefore, there is a need for larger-scale studies comparing the results of a more homogeneous study group in terms of disease duration and a control group that is proven to be free of osteoporosis.
Conclusion
Osteoporosis is a multifactorial disease and may occur early, especially in chronic diseases such as thalassemia. Because of the difficulties in diagnosis and follow-up, screening with DEXA and measuring ferritin level and RANKL/OPG ratios on a regular basis is essential. It should be kept in mind that osteoporosis may develop with advancing age in both sexes.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- β-CTX:
-
Beta-crosslaps
- β-TM:
-
Beta Thalassemia Major
- DPD:
-
Deoxypyridinoline
- DEXA:
-
Dual-Energy X-ray
- RANKL:
-
Activator of nuclear factor-kappa B ligand
- OPG:
-
Osteoprotegerin
- TURKAK:
-
Turkish Accreditation Agency
References
Al Gaudio A, Morabito N, Xourafa A, Macrì I, Meo A, Morgante S, et al. Bisphosphonates in the treatment of thalassemia-associated osteoporosis. J Endocrinol Investig. 2008;31(2):181–4.
Voskaridou E, Christoulas D, **rakia C, Varvagiannis K, Boutsikas G, Bilalis A, et al. Serum Dickkopf-1 is increased and correlates with reduced bone mineral density in patients with thalassemia-induced osteoporosis. Reduction post-zoledronic acid administration. Haematologica. 2009;94(5):725–8.
Voskaridou E, Terpos E. New insights into the pathophysiology and management of osteoporosis in patients with beta thalassaemia. Br J Haematol. 2004;127(2):127–39.
Fung EB, Vichinsky EP, Kwiatkowski JL, Huang J, Bachrach LK, Sawyer AJ, et al. Characterization of low bone mass in young patients with thalassemia by DXA, pQCT and markers of bone turnover. Bone. 2011;48(6):1305–12.
Filosa A, Di Maio S, Vocca S, Saviano A, Esposito G, Pagano L. Longitudinal monitoring of bone mineral density in thalassaemic patients. Genetic structure and osteoporosis. Acta Pediatr. 1997;86:342–6.
Skordis N, Toumba M. Bone disease in thalassaemia major: recent advances in pathogenesis and clinical aspects. Pediatr Endocrinol Rev. 2011;8:300–6.
Toumba M, Skordis N. Osteoporosis syndrome in thalassaemia major: an overview. J Osteoporos. 2010;2010:537673.
Salah H, Atfy M, Fathy A, Atfy M, Mansor H, Saeed J. The clinical significance of OPG/sRANKL ratio in thalassemia patients suffering from osteopenia or osteoporosis in Egyptian patients. Immunol Investig. 2010;39(8):820–32.
Jørgensen L, Hansen JB, Brox J, Mathiesen E, Vik A, Jacobsen BK. Serum osteoprotegerin levels are related to height loss: the Tromsø study. Eur J Epidemiol. 2011;26(4):305–12.
Morabito N, Gaudio A, Lasco A, et al. Osteoprotegerin and RANKL in the pathogenesis of thalassemia–induced osteoporosis. J Bone Miner Res. 2004;19(5):722–7.
Ozdemir MA, Yilmaz K, Abdulrezzak U, Muhtaroglu S, Patiroglu T, Karakukcu M, et al. The efficacy of vitamin K2 and calcitriol combination on thalassemic osteopathy. J Pediatr Hematol Oncol. 2013;35(8):623–7.
Alfaqih MA, Bashir N, Saadeh R, Khader Y, Barqawi M, Alqudah S. Dysregulation of the RANKL/RANK/OPG axis in thalassemia intermedia patients. BMC Res Notes. 2018;11(1):534. https://doi.org/10.1186/s13104-018-3616-y PMID: 30064480; PMCID: PMC6069879.
Akhtar Ali S, Kang H, Olney R, Ramos-Platt L, Ryabets-Lienhard A, Cheung C, et al. Evaluating RANKL and OPG levels in patients with Duchenne muscular dystrophy. Osteoporos Int. 2019;30(11):2283–8. https://doi.org/10.1007/s00198-019-05077-5 Epub 2019 Aug 7. PMID: 31392399.
Ali R, Hammad A, El-Nahrery E, Hamdy N, Elhawary AK, Eid R. Serum RANKL, osteoprotegerin (OPG) and RANKL/OPG ratio in children with systemic lupus erythematosus. Lupus. 2019;28(10):1233–42. https://doi.org/10.1177/0961203319867129 Epub 2019 Aug 12. PMID: 31403902.
Taylan A, Birlik M, Kenar G, Toprak B, Gundogdu B, Gurler O, et al. Osteoprotegrin interacts with biomarkers and cytokines that have roles in osteoporosis, skin fibrosis, and vasculopathy in systemic sclerosis: a potential multifaceted relationship between OPG/RANKL/TRAIL and Wnt inhibitors. Mod Rheumatol. 2019;29(4):619–24. https://doi.org/10.1080/14397595.2018.1500736 Epub 2018 Sep 25. PMID: 30001654.
Karalazou P, Ntelios D, Chatzopoulou F, Fragou A, Taousani M, Mouzaki K, et al. OPG/RANK/RANKL signaling axis in patients with type I diabetes: associations with parathormone and vitamin D. Ital J Pediatr. 2019;45(1):161. https://doi.org/10.1186/s13052-019-0748-1 PMID: 31823791; PMCID: PMC6902340.
Pietrapertosa AC, Minenna G, Colella SM, Santeramo TM, Renni R, D'Amore M. Osteoprotegerin and RANKL in the pathogenesis of osteoporosis in patients with thalassaemia major. Panminerva Med. 2009;51(1):17–23 PMID: 19352306.
Bagan L, Jiménez Y, Leopoldo M, Rubert A, Bagan J. Serum levels of RANKL and OPG, and the RANKL/OPG ratio in bisphosphonate-related osteonecrosis of the jaw: are they useful biomarkers for the advanced stages of osteonecrosis? Med Oral Patol Oral Cir Bucal. 2017;22(5):e542–7. https://doi.org/10.4317/medoral.22128 PMID: 28809381; PMCID: PMC5694175.
El Amrousy D, El-Afify D, Shabana A. Relationship between bone turnover markers and oxidative stress in children with type 1 diabetes mellitus. Pediatr Res. 2021;89(4):878–81. https://doi.org/10.1038/s41390-020-01197-5 Epub 2020 Oct 10. PMID: 33038875.
Alswat KA. Gender Disparities in Osteoporosis. J Clin Med Res. 2017;9(5):382–7. https://doi.org/10.14740/jocmr2970w.
Kyriakou A, Savva SC, Savvides I, Pangalou E, Ioannou YS, Christou S, et al. Gender differences in the prevalence and severity of bone disease in thalassaemia. Pediatr Endocrinol Rev. 2008;6(Suppl 1):116–22 PMID: 19337164.
Shamshirsaz AA, Bekheirnia MR, Kamgar M, et al. Bone mineral density in Iranian adolescents and young adults with thalassemia major. Pediatr Hematol Oncol. 2007;24(7):469–79.
Büyükşimşek M, Başlamışlı İF. The relationship between Iron accumulation, vitamin D deficiency and bone mineral density in patients with thalassemia major, thalassemia intermedia and sickle cell. Turk J Osteoporos. 2020;26:121–6. https://doi.org/10.4274/tod.galenos.2020.85520.
Acknowledgements
We are grateful to children and their families who gave consent to participate to the study.
Funding
This study was funded by the Department of Scientific Research Projects (no: 1106 M 0107) in Mustafa Kemal University.
Author information
Authors and Affiliations
Contributions
TC and OS conceived the study; TC, SU and AB wrote manuscript draft; TC and SM performed data curation; TC, OS and SU performed patient enrollment; TC, SU and AB revised the manuscript. All the authors read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The protocol was approved by the ethical committee of the University of Mustafa Kemal (Protocol number 2011/12).
All methods were carried out in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Written informed consent was obtained from all participants or if participants are under 16, from a parent and/or legal guardian.
Consent for publication
This manuscript does not contain any individual person’s data.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Çelik, T., Sangün, Ö., Ünal, Ş. et al. Assessment of biochemical bone markers of osteoporosis in children with thalassemia major. Ital J Pediatr 48, 105 (2022). https://doi.org/10.1186/s13052-022-01290-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13052-022-01290-x