Abstract
Background
Accurate etiology diagnosis is crucial for central nervous system infections (CNS infections). The diagnostic value of metagenomic next-generation sequencing (mNGS), an emerging powerful platform, remains to be studied in CNS infections.
Methods
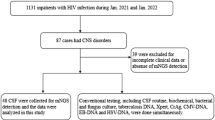
We conducted a single-center prospective cohort study to compare mNGS with conventional methods including culture, smear and etc. 248 suspected CNS infectious patients were enrolled and clinical data were recorded.
Results
mNGS reported a 90.00% (9/10) sensitivity in culture-positive patients without empirical treatment and 66.67% (6/9) in empirically-treated patients. Detected an extra of 48 bacteria and fungi in culture-negative patients, mNGS provided a higher detection rate compared to culture in patients with (34.45% vs. 7.56%, McNemar test, p < 0.0083) or without empirical therapy (50.00% vs. 25.00%, McNemar test, p > 0.0083). Compared to conventional methods, positive percent agreement and negative percent agreement was 75.00% and 69.11% separately. mNGS detection rate was significantly higher in patients with cerebrospinal fluid (CSF) WBC > 300 * 106/L, CSF protein > 500 mg/L or glucose ratio ≤ 0.3. mNGS sequencing read is correlated with CSF WBC, glucose ratio levels and clinical disease progression.
Conclusion
mNGS showed a satisfying diagnostic performance in CNS infections and had an overall superior detection rate to culture. mNGS may held diagnostic advantages especially in empirically treated patients. CSF laboratory results were statistically relevant to mNGS detection rate, and mNGS could dynamically monitor disease progression.
Similar content being viewed by others
Background
Central nervous system infections (CNS infections) refers to inflammations of brain and spinal cord caused by various pathogenic microbes, including meningitis, encephalitis, abscess and etc. Despite continuously improving diagnostic and treatment skills, CNS infections still compose a considerable portion of human morbidity and mortality, and it is estimated that nearly 320,000 people died from meningitis in 2016 [1]. Timely identification of causative agents is critical for the administration of effective treatment and difficulties in this area still exist. Traditional cerebrospinal fluid (CSF) culture can identify approximately 30–40% CNS infections (including meningitis and encephalitis) [2], and some study even reported 80–90% detection rate in acute community-acquired bacterial meningitis patients [3]. However, in develo** countries like China, the detection rate of CSF culture in meningitis ranges 5.4–24.3% from updated surveys [4,31, 32]. What’s more, RNA library preparations were conducted in a limited number of patients, which might neglect some neuroinvasive RNA viruses. Further, as the mNGS results may be easily influenced by many factors, the standards in our single center cross-section study should be thoroughly modified and tested before applying to other centers.
Conclusion
This single center study demonstrated that in CNS infected patients, mNGS had an overall superior detection rates of potential pathogens to conventional methods, and the complementation of mNGS and conventional methods would significantly improve the etiology diagnosis. For patients who had received empirical antibiotics treatment, mNGS would hold significant diagnostic advantages over conventional methods, however, the detection rate of mNGS would continuously decrease with the increasing effective treatment lengths. Our findings also discovered that elevated CSF WBC and protein level or decreased glucose ratio is correlated with higher mNGS positivity in CNS infections. Furthermore, mNGS could dynamically surveil pathogen loads and disease progression using semi-quantitative value analysis. Although mNGS has showed the ability to diagnosis clinical infections, it alone still could not replace the necessity of culture. In future, multi-center studies will be needed to explore universal criteria or guidelines of mNGS in CNS infections.
Data availability
We have deposited non-human sequences to China National GeneBank Database (CNGBdb) (Project accession: CNP0000610).
References
The global burden of meningitis. 2018. https://www.meningitis.org/meningitis/the-global-burden-of-meningitis.
Leber AL, Everhart K, Balada-Llasat JM, Cullison J, Daly J, Holt S, Lephart P, Salimnia H, Schreckenberger PC, DesJarlais S, et al. Multicenter evaluation of BioFire FilmArray meningitis/encephalitis panel for detection of bacteria, viruses, and yeast in cerebrospinal fluid specimens. J Clin Microbiol. 2016;54:2251–61.
Brouwer MC, Thwaites GE, Tunkel AR, van de Beek D. Dilemmas in the diagnosis of acute community-acquired bacterial meningitis. Lancet. 2012;380:1684–92.
Li Y, Yin Z, Shao Z, Li M, Liang X, Sandhu HS, Hadler SC, Li J, Sun Y, Li J, et al. Population-based surveillance for bacterial meningitis in China, September 2006–December 2009. Emerg Infect Dis. 2014;20:61–9.
Forrester N, **e Y, Tan Y, Chongsuvivatwong V, Wu X, Bi F, Hadler SC, Jiraphongsa C, Sornsrivichai V, Lin M, Quan Y. A population-based acute meningitis and encephalitis syndromes surveillance in Guangxi, China, May 2007–June 2012. PLoS ONE. 2015;10:e0144366.
Chen C, Zhang B, Yu S, Sun F, Ruan Q, Zhang W, Shao L, Chen S. The incidence and risk factors of meningitis after major craniotomy in China: a retrospective cohort study. PLoS ONE. 2014;9:e101961.
Duan QJ, Shang SQ, Wu YD. Rapid diagnosis of bacterial meningitis in children with fluorescence quantitative polymerase chain reaction amplification in the bacterial 16S rRNA gene. Eur J Pediatr. 2009;168:211–6.
Bahr NC, Nuwagira E, Evans EE, Cresswell FV, Bystrom PV, Byamukama A, Bridge SC, Bangdiwala AS, Meya DB, Denkinger CM, et al. Diagnostic accuracy of Xpert MTB/RIF Ultra for tuberculous meningitis in HIV-infected adults: a prospective cohort study. Lancet Infect Dis. 2018;18:68–75.
Wilson MR, Naccache SN, Samayoa E, Biagtan M, Bashir H, Yu G, Salamat SM, Somasekar S, Federman S, Miller S, et al. Actionable diagnosis of neuroleptospirosis by next-generation sequencing. N Engl J Med. 2014;370:2408–17.
Wilson MR, Shanbhag NM, Reid MJ, Singhal NS, Gelfand JM, Sample HA, Benkli B, O’Donovan BD, Ali IK, Keating MK, et al. Diagnosing Balamuthia mandrillaris encephalitis with metagenomic deep sequencing. Ann Neurol. 2015;78:722–30.
Guan H, Shen A, Lv X, Yang X, Ren H, Zhao Y, Zhang Y, Gong Y, Ni P, Wu H, et al. Detection of virus in CSF from the cases with meningoencephalitis by next-generation sequencing. J Neurovirol. 2016;22:240–5.
Kawada J, Okuno Y, Torii Y, Okada R, Hayano S, Ando S, Kamiya Y, Kojima S, Ito Y. Identification of viruses in cases of pediatric acute encephalitis and encephalopathy using next-generation sequencing. Sci Rep. 2016;6:33452.
Wuthrich D, Boujon CL, Truchet L, Selimovic-Hamza S, Oevermann A, Bouzalas IG, Bruggmann R, Seuberlich T. Exploring the virome of cattle with non-suppurative encephalitis of unknown etiology by metagenomics. Virology. 2016;493:22–30.
Wylie KM, Blanco-Guzman M, Wylie TN, Lawrence SJ, Ghobadi A, DiPersio JF, Storch GA. High-throughput sequencing of cerebrospinal fluid for diagnosis of chronic Propionibacterium acnes meningitis in an allogeneic stem cell transplant recipient. Transpl Infect Dis. 2016;18:227–33.
Chiu CY, Coffey LL, Murkey J, Symmes K, Sample HA, Wilson MR, Naccache SN, Arevalo S, Somasekar S, Federman S, et al. Diagnosis of fatal human case of St. louis encephalitis virus infection by metagenomic sequencing, California, 2016. Emerg Infect Dis. 2017;23:1964–8.
Murkey JA, Chew KW, Carlson M, Shannon CL, Sirohi D, Sample HA, Wilson MR, Vespa P, Humphries RM, Miller S, et al. Hepatitis E virus-associated meningoencephalitis in a lung transplant recipient diagnosed by clinical metagenomic sequencing. Open Forum Infect Dis. 2017;4:ofx121.
Piantadosi A, Mukerji SS, Chitneni P, Cho TA, Cosimi LA, Hung DT, Goldberg MB, Sabeti PC, Kuritzkes DR, Grad YH. Metagenomic sequencing of an echovirus 30 genome from cerebrospinal fluid of a patient with aseptic meningitis and orchitis. Open Forum Infect Dis. 2017;4:ofx138.
Wilson MR, Zimmermann LL, Crawford ED, Sample HA, Soni PR, Baker AN, Khan LM, DeRisi JL. Acute west nile virus meningoencephalitis diagnosed via metagenomic deep sequencing of cerebrospinal fluid in a renal transplant patient. Am J Transplant. 2017;17:803–8.
Wilson MR, O’Donovan BD, Gelfand JM, Sample HA, Chow FC, Betjemann JP, Shah MP, Richie MB, Gorman MP, Hajj-Ali RA, et al. Chronic meningitis investigated via metagenomic next-generation sequencing. JAMA Neurol. 2018;75:947–55.
Wilson MR, Sample HA, Zorn KC, Arevalo S, Yu G, Neuhaus J, Federman S, Stryke D, Briggs B, Langelier C, et al. Clinical metagenomic sequencing for diagnosis of meningitis and encephalitis. N Engl J Med. 2019;380:2327–40.
Stahl JP, Azouvi P, Bruneel F, De Broucker T, Duval X, Fantin B, Girard N, Herrmann JL, Honnorat J, Lecuit M, et al. Guidelines on the management of infectious encephalitis in adults. Médecine et Maladies Infectieuses. 2017;47:179–94.
Zhou X, Wu H, Ruan Q, Jiang N, Chen X, Shen Y, Zhu YM, Ying Y, Qian YY, Wang X, et al. Clinical evaluation of diagnosis efficacy of active Mycobacterium tuberculosis complex infection via metagenomic next-generation sequencing of direct clinical samples. Front Cell Infect Microbiol. 2019;9:351.
Zhang HC, Ai JW, Cui P, Zhu YM, Hong-Long W, Li YJ, Zhang WH. Incremental value of metagenomic next generation sequencing for the diagnosis of suspected focal infection in adults. J Infect. 2019;79:419–25.
Riddell J, Shuman EK. Epidemiology of central nervous system infection. Neuroimaging Clin N Am. 2012;22:543–56.
Chen PJ, Lin MC, Lai MJ, Lin JC, Lu HH, Tseng VS. Accurate classification of diminutive colorectal polyps using computer-aided analysis. Gastroenterology. 2018;154:568–75.
Brown JR, Bharucha T, Breuer J. Encephalitis diagnosis using metagenomics: application of next generation sequencing for undiagnosed cases. J Infect. 2018;76:225–40.
Fan S, Qiao X, Liu L, Wu H, Zhou J, Sun R, Chen Q, Huang Y, Mao C, Yuan J, et al. Next-generation sequencing of cerebrospinal fluid for the diagnosis of neurocysticercosis. Front Neurol. 2018;9:471.
Bronska E, Kalmusova J, Dzupova O, Maresova V, Kriz P, Benes J. Dynamics of PCR-based diagnosis in patients with invasive meningococcal disease. Clin Microbiol Infect. 2006;12:137–41.
Nigrovic LE, Malley R, Macias CG, Kanegaye JT, Moro-Sutherland DM, Schremmer RD, Schwab SH, Agrawal D, Mansour KM, Bennett JE, et al. Effect of antibiotic pretreatment on cerebrospinal fluid profiles of children with bacterial meningitis. Pediatrics. 2008;122:726–30.
Ai JW, Zhang HC, Cui P, Xu B, Gao Y, Cheng Q, Li T, Wu H, Zhang WH. Dynamic and direct pathogen load surveillance to monitor disease progression and therapeutic efficacy in central nervous system infection using a novel semi-quantitive sequencing platform. J Infect. 2018;76:307–10.
Simner PJ, Miller HB, Breitweiser FP, Pinilla Monsalve G, Pardo CA, Salzberg SL, Sears C, Thomas DL, Eberhart CG, Carroll KC. Development and optimization of metagenomic next-generation sequencing methods for cerebral spinal fluid diagnostics. J Clin Microbiol. 2018;56:e00472-18.
Akcam FZ, Yayli G, Uskun E, Kaya O, Demir C. Evaluation of the Bactec microbial detection system for culturing miscellaneous sterile body fluids. Res Microbiol. 2006;157:433–6.
Acknowledgements
We thank the patients for cooperating with our investigation and acknowledge the professionalism and compassion demonstrated by all the healthcare workers involved in patients’ care.
Funding
This study was supported by the New and Advanced Technology Project of Shanghai Municipal Hospital: Application of next generation sequencing technique in precise diagnosis of infectious diseases (SHDC12017104) and Key Technologies Research and Development Program for Infectious Diseases of China under Grant 2018ZX10305-409-001-003.
Author information
Authors and Affiliations
Contributions
YZ and JA conceived this next-generation sequencing research and wrote the paper, HZ and YMZ collected and analyzed the clinical data; PC, HW, and MY were sub-investigators in the next-generation sequencing research, performed the next-generation sequencing analysis for this study. JA and WZ supervised data collection and analysis, and paper draft. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The study was approved by the Huashan Hospital ethical committee the methods were carried out in accordance with the approved guidelines of the institution.
Consent for publication
Not applicable.
Competing interests
All authors report no potential conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Additional file 1: Table S1.
Commonly reported pathogens in central nervous system (CNS) Infection. Table S2. Criteria of CNS infection. Table S3. Missed or extra identified bacteria and fungi by mNGS when comparing to culture in CNS infections. Table S4. The consistency between mNGS and other conventional methods (PCR, Xpert MTB/RIF, Filmarray, serological antibody test and etc.). Table S5. The comparison of relative abundance of pathogens who were detected at least 5 times between a) culture-positive vs culture-negative and b) with vs without empirical treatment patients. Table S6. The CSF laboratory examinations among different subgroups.
Additional file 2: Data set 1.
Preliminary sequencing threshold of relative abundance.
Additional file 3: Data set 2.
Sequencing details.
Additional file 4: Data set 3.
Sample details of enrolled participants.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Zhang, Y., Cui, P., Zhang, HC. et al. Clinical application and evaluation of metagenomic next-generation sequencing in suspected adult central nervous system infection. J Transl Med 18, 199 (2020). https://doi.org/10.1186/s12967-020-02360-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12967-020-02360-6