Abstract
Colorectal cancer (CRC) is the third most prevalent cancer and the third highest cancer-related mortality in the United States. Bigelovin, a sesquiterpene lactone isolated from Inula helianthus aquatica, has been proven to induce apoptosis and exhibit anti-inflammatory and anti-angiogenic activities. However, the effects of bigelovin on CRC and underlying mechanisms have not been explored. The present study demonstrated that bigelovin exhibited potent anti-tumor activities against CRC in vitro and in vivo. Bigelovin suppressed cell proliferation and colony formation and induced apoptosis in human colorectal cancer HT-29 and HCT 116 cells in vitro. Results also revealed that bigelovin activated caspases, caused the G2/M cell cycle arrest and induced DNA damage through up-regulation of death receptor (DR) 5 and increase of ROS. In HCT 116 xenograft model, bigelovin treatment resulted in suppression of tumor growth. Bigelovin at 20 mg/kg showed more significant tumor suppression and less side effects than conventional FOLFOX (containing folinic acid, 5-fluorouracil and oxaliplatin) treatment. In addition, in vivo data confirmed that anti-tumor activity of bigelovin in CRC was through induction of apoptosis by up-regulating DR5 and increasing ROS. In conclusion, these results strongly suggested that bigelovin has potential to be developed as therapeutic agent for CRC patients.
Similar content being viewed by others
Introduction
Colorectal cancer is one of the top three most common cancer and the third leading cause of cancer-related death in the United States1. In 2016, American Cancer Society (ACS) estimates that 134,490 persons will be diagnosed having colorectal cancer (CRC), and more than one-third will die from this cancer2. Although the incidence and mortality rate of CRC in developed countries declined during the last decade mainly due to the early screen in asymptomatic and average risk people2,3, incidence and mortality rate are still growing in develo** world with increasing westernized lifestyle and aging population3. Surgery is the primary treatment for most of the CRC patients4. For patients in higher level of metastatic stage, radiation and chemotherapy often accompany with surgery. Currently, fluorouracil (5-Fu) is often used alone or combined with folinic acid and oxaliplatin as FOLFOX to treat primary colon cancer. For advanced or metastatic CRC, FOLFOX and FOLFIRI (5-Fu, folinic acid and irinotecan) are the most commonly used chemotherapy combinations. Despite the effectiveness of the chemotherapy and radioactive therapy, the high incidence (up to 98%) of side effects, including hair loss, nausea, vomiting, neurotoxicity, increasing the chance of infection and immune system suppression often affect the quality of life5,6. Targeted therapy to vascular endothelial growth factor (e.g. bevacizumab) or epidermal growth factor receptor (e.g. cetuximab) are common adjuvant/alternative treatments for CRC7. Although they are reported to increase survival rates for cancer patients, the costs for these treatments are high8. Hence, the searching of new compounds from natural source with high efficacy, low toxicity and low cost for CRC remains highly desirable.
Traditional Chinese medicines (TCM) have been used for thousands of years for treating various diseases, however, the active components and mechanisms are still often unanswered. In the past, natural compounds have been proven as rich sources of anticancer drugs, such as paclitaxel, camptothecin9,10. Bigelovin, a sesquiterpene lactone isolated from Inula helianthus-aquatica, was identified as a selective retinoid X receptor α agonist11, possessed anti-emetic12 activities, anti-angiogenic activities13, and down-regulated the gene expressions of inflammatory-related cell adhesion molecules and monocyte adhesion14. Previous studies demonstrated that bigelovin could induce apoptosis on a panel of cancer cell lines including leukemia, lung, liver, glioma, kidney, gastric, cervix and breast in vitro15,16. However, the anti-CRC effect and the underlying mechanisms of bigelovin have not been investigated.
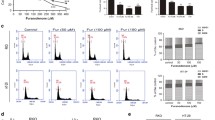
Death receptor 5 (DR5) is a TNF-related apoptosis inducing ligand (TRAIL) receptor, which has been identified as a novel target with better selectivity for cancer therapy as shown to induce apoptosis in a diversity of cell types17. Engagement of DR 5 results in the activation of caspase 8, which in turn activates downstream effector caspases in the extrinsic apoptosis pathway. While reactive oxygen species (ROS) are known to be regulator of TRAIL receptor induction18. Furthermore, emerging evidences illustrated that other terpenoids such as eriocalyxin B19, celastrol20, tagalsins21 and zerumbone22 can cause ROS-mediated apoptosis due to their structure of α, β-unsaturated ketone moieties19. Bigelovin also has two α, β-unsaturated ketone moieties (Fig. 1a), thus we hypothesized that bigelovin-induced apoptosis may be mediated by ROS.
(a) Chemical structure of bigelovin with two α, β-unsaturated ketone moieties. (b) Bigelovin was selectively toxic to colorectal cancer cells comparing to primary normal colon cells. IC50 values from 48 h incubation in HT-29 and HCT 116 cell lines and primary normal colon cells by MTT assay. (Mean ± SD; ***p < 0.001, vs primary normal colon cells; n = 4). (c) Cell proliferation assay of two cell lines treated with bigelovin for indicated dose and time points (**p < 0.01, ***,###,&&&p < 0.001 vs. medium control at the corresponding time point; n = 3–4). HT-29 (d) and HCT 116 (e) were seeded in 100 mm dish, and after 48 h bigelovin treatment, they were reseeded and maintained for 8 or 11 days to form colonies (**p < 0.01, ***p < 0.001 vs. medium control; n = 4–5).
The present study aimed to investigate the inhibitory effect of bigelovin on CRC through evaluating its anti-tumor effect in vivo and elucidating the underlying mechanisms of actions in vitro.
Results
Bigelovin inhibited growth and colony formation of human colon cells
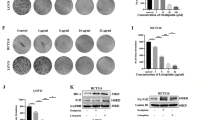
Cell viability was assessed by MTT assay on HT-29 and HCT 116 cells. Cells were treated with bigelovin (0.037 to 9 μM) or 5-Fu/cisplatin (0.11 to 27 μM) for 24, 48 and 72 h. As shown in the Supplementary Table S1, colon cancer cell lines were more sensitive to bigelovin treatment rather than 5-Fu or cisplatin. Bigelovin induced cytotoxicity in these two cancer cell lines in time-dependent and dose-dependent manners. To test the selectivity of bigelovin, primary human colon cells were used (mixture of fibroblast and epithelial cells, data not shown). From IC50 values, primary colon cells were less sensitive to bigelovin treatment (8.55 μM for 48 h treatment) comparing to colon cancer cell lines (0.8 and 1.2 μM for 48 h treatment, Fig. 1b and Table S1). To test the effects of bigelovin on cell proliferation, HT-29 and HCT 116 cells were treated with bigelovin at 1.4–5.4 μM (1 to 3 folds of 24 h IC50 values for each cell line) for 24, 48 and 72 h. As shown in Fig. 1c, bigelovin significantly reduced cell proliferation of both cell lines in a time- and dose- dependent manners. Further more, to determine cell lethal- and sub-lethal damage repair after bigelovin treatment, HT-29 and HCT 116 cells were reseeded and maintained for 8 or 11 days to allow colony formation. Cells which were treated by bigelovin showed significantly decreased colony formation ability as compared with vehicle control (Fig. 1d,e). The decreasing of colony formation ability indicated that bigelovin could decrease damage repair ability of colon cancer cell lines. Taken together, our results showed that bigelovin suppressed the growth of colorectal cancer cells.
Bigelovin induced apoptosis through caspases activation
Suppression of cancer growth arises from inducing of apoptosis, inhibition of cell proliferation, or bothSiRNA transfection For siRNA transfection, HT-29 and HCT 116 cells were plated in 6-well plates/60 mm dish and cultured for 16 h. Thirty pmol siRNAs (s225038 and s16756) /negative control, 9 μL Lipofectamine™ RNAiMAX were mixed with 150 μL Opti-MEM medium separately for 5 min. Lipofectamine was added to siRNAs for 20 min of incubation. Culture medium of HT-29 and HCT 116 cells was changed to Opti-MEM medium and then a mixture of siRNAs were added to cells. After 24 h of incubation, culture medium was changed to fresh, full-culture medium plus bigelovin/ vehicle DMSO at the indicated dose for 24 h. All animal experiments were carried out under institutional guidelines, and experimental procedures were approved by the Animal Experimentation Ethics Committee of The Chinese University of Hong Kong (Ref. No. 14/170/MIS). Male BALB/c nude mice (6–8 weeks of age) were supplied by the Laboratory Animal Services Centre of CUHK. Mice were bred and maintained in pathogen-free conditions (sterile water and food) in specifically designed air-controlled rooms with a 12-h light/dark cycle. HCT 116 cells (5 × 106) were suspended in 100 μL PBS and injected subcutaneously into the back of nude mice. After tumor reaching 50 mm3 in volume, mice were randomized into groups of 5 animals and treated with either vehicle, bigelovin (5 mg/kg, 10 mg/kg, and 20 mg/kg) or FOLFOX (15 mg/kg fluorouracil daily; 5 mg/kg folinic acid daily and 5 mg/kg oxaliplatin once a week) as positive control. Bigelovin or vehicle was administered intraperitoneally every two days for 10 times while FOLFOX was administered intraperitoneally daily for 7 days. Tumors were measured twice per week using calipers and tumor volumes were calculated using the formula length × width × depth/2 (mm3), and at the same time, each mouse was weighed. Bigelovin was dissolved in PBS (with 2% DMSO). At the end of experiment, plasma, tumors, livers, hearts, kidneys and lungs were collected. The plasma enzymes, aspartate aminotransferase (AST), alanine aminotransferase (ALT) and lactate dehydrogenase (LDH) were used to assess tissue damage; creatine kinase (CK) was used to assess muscle damage. They were evaluated according to manufacturer’s instructions (Stanbio Laboratory, USA). Tumor tissue specimens were collected from mice and separated into two halves, one half was fixed in 10% formalin and embedded in paraffin whereas the other half was embedded in Optimal Cutting Temperature compound (OCT) and frozen at −80 °C. Other organs (liver, lung, heart, kidney) were fixed in 10% formalin, embedded in paraffin and sectioned at 5 μm, collected on coated slides for staining. Tumor sections on slides were dewaxed, rehydrated, incubated with Cova Decloater and incubated with primary antibodies (Ki 67, DR5, Factor VIII) overnight at 4 °C as described in other study51. Formalin-fixed paraffin embedded sections were also used in TUNEL assay as per kit’s instruction. Frozen sections of tumors were sectioned at 10 μm using a cryostat (CM 1100, Leica, Germany), and stained with dihydroethidium (DHE, 2.5 μM in Krebs-HEPES buffer) dye for 15 min at 37 °C in the dark50. Fluorescence captured by fluorescence microscope (Olympus IX71, Japan) and intensity of fluorescence was calculated by Image J software (Image J 1.50b). All in vitro experiments were performed at least three times. Quantitative results were analyzed by Student’s t test or one-way ANOVA. Statistical significance was considered when p < 0.05. All statistical analysis was assessed by SPSS 20 software.In vivo xenograft studies
Immunohistochemistry
Statistical analysis
Additional Information
How to cite this article: Li, M. et al. Bigelovin triggered apoptosis in colorectal cancer in vitro and in vivo via upregulating death receptor 5 and reactive oxidative species. Sci. Rep. 7, 42176; doi: 10.1038/srep42176 (2017).
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
El-Shami, K. et al. American Cancer Society Colorectal Cancer Survivorship Care Guidelines. CA: A Cancer Journal for Clinicians 65, 427–455 (2015).
Smith, R. A. et al. Cancer screening in the United States, 2016: A review of current American Cancer Society guidelines and current issues in cancer screening. CA Cancer J Clin 66, 95–114 (2016).
Torre, L. A. et al. Global cancer statistics, 2012. CA: A Cancer Journal for Clinicians 65, 87–108 (2015).
Compton, C. C. Colorectal carcinoma: diagnostic, prognostic, and molecular features. Modern Pathology 16, 376–388 (2003).
Schuell, B. et al. Side effects during chemotherapy predict tumour response in advanced colorectal cancer. Br J Cancer 93, 744–748 (2005).
Wiela-Hojenska, A., Kowalska, T., Filipczyk-Cisarz, E., Lapinski, L. & Nartowski, K. Evaluation of the toxicity of anticancer chemotherapy in patients with colon cancer. Adv Clin Exp Med 24, 103–111 (2015).
Gupta, S. C. et al. Nimbolide, a limonoid triterpene, inhibits growth of human colorectal cancer xenografts by suppressing the proinflammatory microenvironment. Clin Cancer Res 19, 4465–4476 (2013).
Valachis, A., Polyzos, N. P., Nearchou, A., Lind, P. & Mauri, D. Financial relationships in economic analyses of targeted therapies in oncology. Journal of Clinical Oncology 30, 1316–1320 (2012).
Lee, K. W., Bode, A. M. & Dong, Z. Molecular targets of phytochemicals for cancer prevention. Nature Reviews Cancer 11, 211–218 (2011).
Dancey, J. & Eisenhauer, E. A. Current perspectives on camptothecins in cancer treatment. Br J Cancer 74, 327–338 (1996).
Zhang, H. et al. Structure basis of bigelovin as a selective RXR agonist with a distinct binding mode. J Mol Biol 407, 13–20 (2011).
Kinoshita, K. et al. Anti-emetic principles of Inula linariaefolia flowers and Forsythia suspensa fruits. Phytomedicine 3, 51–58 (1996).
Yue, G. G. L. et al. Anti-angiogenesis and immunomodulatory activities of an anti-tumor sesquiterpene bigelovin isolated from Inula helianthus-aquatica . European Journal of Medicinal Chemistry 59, 243–252 (2013).
Nam, K. W. et al. Nuclear factor kappaB-mediated down-regulation of adhesion molecules: possible mechanism for inhibitory activity of bigelovin against inflammatory monocytes adhesion to endothelial cells. J Ethnopharmacol 123, 250–256 (2009).
Liu, J. L. et al. Small compound bigelovin exerts inhibitory effects and triggers proteolysis of E2F1 in multiple myeloma cells. Cancer Sci 104, 1697–1704 (2013).
Zhang, H. H. et al. Bigelovin inhibits STAT3 signaling by inactivating JAK2 and induces apoptosis in human cancer cells. Acta Pharmacol Sin 36, 507–516 (2015).
Wajant, H., Gerspach, J. & Pfizenmaier, K. Engineering death receptor ligands for cancer therapy. Cancer Lett 332, 163–174 (2013).
Prasad, S., Ravindran, J., Sung, B., Pandey, M. K. & Aggarwal, B. B. Garcinol potentiates TRAIL-induced apoptosis through modulation of death receptors and antiapoptotic proteins. Molecular Cancer Therapeutics 9, 856–868 (2010).
Li, L. et al. Eriocalyxin B-induced apoptosis in pancreatic adenocarcinoma cells through thiol-containing antioxidant systems and downstream signalling pathways. Curr Mol Med 14, 673–689 (2014).
Li, H. Y. et al. Celastrol induces apoptosis and autophagy via the ROS/JNK signaling pathway in human osteosarcoma cells: an in vitro and in vivo study. Cell Death Dis 6, e1604 (2015).
Neumann, J. et al. Mangrove dolabrane-type of diterpenes tagalsins suppresses tumor growth via ROS-mediated apoptosis and ATM/ATR-Chk1/Chk2- regulated cell cycle arrest. Int J Cancer 137, 2739–2748 (2015).
Yodkeeree, S., Sung, B., Limtrakul, P. & Aggarwal, B. B. Zerumbone enhances TRAIL-induced apoptosis through the induction of death receptors in human colon cancer cells: Evidence for an essential role of reactive oxygen species. Cancer Research 69, 6581–6589 (2009).
**ang, T., Du, L., Pham, P., Zhu, B. & Jiang, S. Nelfinavir, an HIV protease inhibitor, induces apoptosis and cell cycle arrest in human cervical cancer cells via the ROS-dependent mitochondrial pathway. Cancer Letters 364, 79–88 (2015).
Kaufmann, S. H., Desnoyers, S., Ottaviano, Y., Davidson, N. E. & Poirier, G. G. Specific proteolytic cleavage of poly (ADP-ribose) polymerase: an early marker of chemotherapy-induced apoptosis. Cancer Res 53, 3976–3985 (1993).
Evan, G. I. & Vousden, K. H. Proliferation, cell cycle and apoptosis in cancer. Nature 411, 342–348 (2001).
Liu, W.-T. et al. MJ-66 induces malignant glioma cells G2/M phase arrest and mitotic catastrophe through regulation of cyclin B1/Cdk1 complex. Neuropharmacology 86, 219–227 (2014).
Ye, X. S., Fincher, R. R., Tang, A. & Osmani, S. A. The G2/M DNA damage checkpoint inhibits mitosis through Tyr15 phosphorylation of p34cdc2 in Aspergillus nidulans. EMBO J 16, 182–192 (1997).
Park, S., Li, C., Zhao, H., Darzynkiewicz, Z. & Xu, D. Gene 33/Mig6 inhibits hexavalent chromium-induced DNA damage and cell transformation in human lung epithelial cells. Oncotarget 7, 8916–8930 (2016).
Horinaka, M. et al. Luteolin induces apoptosis via death receptor 5 upregulation in human malignant tumor cells. Oncogene 24, 7180–7189 (2005).
Zhang, Z. et al. Increased HMGB1 and cleaved caspase-3 stimulate the proliferation of tumor cells and are correlated with the poor prognosis in colorectal cancer. J Exp Clin Cancer Res 34, 51 (2015).
Lash, G. E. et al. Prednisolone treatment reduces endometrial spiral artery development in women with recurrent miscarriage. Angiogenesis 14, 523–532 (2011).
Zeng, G. Z. et al. Apoptosis inducement of bigelovin from Inula helianthus-aquatica on human leukemia U937 cells. Phytother Res 23, 885–891 (2009).
Suzuki, T. et al. Expression of the E2F family in human gastrointestinal carcinomas. Int J Cancer 81, 535–538 (1999).
Ghobrial, I. M., Witzig, T. E. & Adjei, A. A. Targeting apoptosis pathways in cancer therapy. CA Cancer J Clin 55, 178–194 (2005).
Ahmed, D. et al. Epigenetic and genetic features of 24 colon cancer cell lines. Oncogenesis 2, e71 (2013).
Zhang, S. et al. Small-molecule NSC59984 restores p53 pathway signaling and antitumor effects against colorectal cancer via p73 activation and degradation of mutant p53. Cancer Research 75, 3842–3852 (2015).
Akhtar, N. et al. The pentacyclic triterpenoid, plectranthoic acid, a novel activator of AMPK induces apoptotic death in prostate cancer cells. Oncotarget 7, 3819–3831 (2016).
Nassar, Z. D. et al. Koetjapic acid, a natural triterpenoid, induces apoptosis in colon cancer cells. Oncol Rep 27, 727–733 (2012).
Chen, Z. et al. Triptolide sensitizes pancreatic cancer cells to TRAIL-induced activation of the Death Receptor pathway. Cancer Letters 348, 156–166 (2014).
Murakami, A. et al. Zerumbone, a Southeast Asian ginger sesquiterpene, markedly suppresses free radical generation, proinflammatory protein production, and cancer cell proliferation accompanied by apoptosis: the alpha,beta-unsaturated carbonyl group is a prerequisite. Carcinogenesis 23, 795–802 (2002).
Deorukhkar, A. et al. Zerumbone increases oxidative stress in a thiol-dependent ROS-independent manner to increase DNA damage and sensitize colorectal cancer cells to radiation. Cancer Medicine 4, 278–292 (2015).
Lin, H. H., Shi, M. D., Tseng, H. C. & Chen, J. H. Andrographolide sensitizes the cytotoxicity of human colorectal carcinoma cells toward cisplatin via enhancing apoptosis pathways in vitro and in vivo . Toxicological Sciences 139, 108–120 (2014).
Oliveira, A. R. et al. Triptolide abrogates growth of colon cancer and induces cell cycle arrest by inhibiting transcriptional activation of E2F. Laboratory Investigation 95, 648–659 (2015).
Li, X.-J., Jiang, Z.-Z. & Zhang, L.-y. Triptolide: Progress on research in pharmacodynamics and toxicology. Journal of Ethnopharmacology 155, 67–79 (2014).
Singla, N. & Challana, S. Reproductive toxicity of triptolide in male house rat, Rattus rattus. The Scientific World Journal 2014, 1–6 (2014).
Bokemeyer, C. et al. Fluorouracil, leucovorin, and oxaliplatin with and without cetuximab in the first-line treatment of metastatic colorectal cancer. Journal of Clinical Oncology 27, 663–671 (2008).
Wiezorek, J., Holland, P. & Graves, J. Death receptor agonists as a targeted therapy for cancer. Clinical Cancer Research 16, 1701–1708 (2010).
Mosmann T. Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods 65, 55–63 (1983).
Franken, N. A. P., Rodermond, H. M., Stap, J., Haveman, J. & van Bree, C. Clonogenic assay of cells in vitro . Nature Protocols 1, 2315–2319 (2006).
Li, L. et al. Eriocalyxin B induces apoptosis and cell cycle arrest in pancreatic adenocarcinoma cells through caspase- and p53-dependent pathways. Toxicol Appl Pharmacol 262, 80–90 (2012).
Ruiz de Sabando, A. et al. ML264, a novel small-molecule compound that potently inhibits growth of colorectal cancer. Molecular Cancer Therapeutics 15, 72–83 (2015).
Acknowledgements
This work was supported by the National Basic Research Program of China (2013CB127505), the Foundation of Chinese Academy of Sciences (Hundred Talents Program, XDA09030301-4), the National Natural Science Foundation of China (31470428), and the Natural Science Foundation of Yunnan Provience (2012GA003). The authors would like to thank Miss Ye Cao from the School of Biomedical Sciences and Miss Cherry Wong from Department of Surgery at The Chinese University of Hong Kong for their technical support.
Author information
Authors and Affiliations
Contributions
M.L. carried out the cellular and animal studies, analyzed data and drafted the manuscript. L.S. and L.Z. performed the chemical experiments. G.Y. and C.L. designed the study. J.L., L.L. and X.Z. participated in animal studies. S.T. and K.F. participated in the design of the study. S.N. provided the clinical colon samples. K.F., N.T. and C.L. conceived of the study and contributed essential reagents and tools. All authors reviewed and approved the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Li, M., Song, LH., Yue, GL. et al. Bigelovin triggered apoptosis in colorectal cancer in vitro and in vivo via upregulating death receptor 5 and reactive oxidative species. Sci Rep 7, 42176 (2017). https://doi.org/10.1038/srep42176
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep42176
- Springer Nature Limited
This article is cited by
-
Research progress on antitumor mechanisms and molecular targets of Inula sesquiterpene lactones
Chinese Medicine (2023)
-
Esca** cell death via TRAIL decoy receptors: a systematic review of their roles and expressions in colorectal cancer
Apoptosis (2022)
-
Epistructured catechins, EGCG and EC facilitate apoptosis induction through targeting de novo lipogenesis pathway in HepG2 cells
Cancer Cell International (2018)
-
Bafilomycin C1 induces G0/G1 cell-cycle arrest and mitochondrial-mediated apoptosis in human hepatocellular cancer SMMC7721 cells
The Journal of Antibiotics (2018)
-
Isoalantolactone Inhibits Esophageal Squamous Cell Carcinoma Growth Through Downregulation of MicroRNA-21 and Derepression of PDCD4
Digestive Diseases and Sciences (2018)