Abstract
Objective:
The neutrophil ‘left shift’ can be measured via the immature to total (I/T) neutrophil ratio or the absolute bands per μl using a manual differential count. It can also be measured from an automated differential count by the immature granulocyte percentage (IG%) or the absolute IG per μl. In neonates, it is unknown if the manual or automated differential count is superior.
Study Design:
We directly compared complete blood counts (CBCs) with manual and automated differential counts from infants <90 days old, and documented whether or not each neonate was infected. We developed reference intervals for I/T ratio, bands per μl, IG% and IG per μl using values from non-infected neonates.
Results:
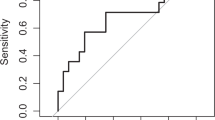
The database had 10 714 CBCs. The upper reference interval for I/T ratio was 0.29 in the first 48 h and 0.31 thereafter; bands per μl was 3710 μl−1 in the first 48 h and 1785 μl−1 thereafter. IG% was 6.2% then 4.2%; IG per μl was 1460 μl−1 then 613 μl−1. Statistical performances of the four methods were equivalent for identifying infection.
Conclusions:
We developed reference intervals for four methods of quantifying a neonate’s ‘left shift’. The information from automated differentials is not inferior to that from manual differentials in identifying infections, but automated differentials have the advantages of a larger sample size, being less expensive, and faster performance times.



Similar content being viewed by others
References
Manroe BL, Rosenfeld CR, Weinberg AG, Browne R . The differential leukocyte count in the assessment and outcome of early-onset neonatal group B streptococcal disease. J Pediatr 1977; 91: 632–637.
Christensen RD, Bradley PP, Rothstein G . The leukocyte left shift in clinical and experimental neonatal sepsis. J Pediatr 1981; 98: 101–105.
Greenberg DN, Yoder BA . Changes in the differential white blood cell count in screening for group B streptococcal sepsis. Pediatr Infect Dis J 1990; 9: 886–889.
Lawrence SM, Eckert J, Makoni M, Pereira HA . Is the use of complete blood counts with manual differentials an antiquated method of determining neutrophil composition in newborns? Ann Clin Lab Sci 2015; 45: 403–413.
Schelonka RL, Yoder BA, Hall RB, Trippett TM, Louder DS, Hickman JR et al. Differentiation of segmented and band neutrophils during the early newborn period. J Pediatr 1995; 127: 298–300.
Newman TB, Draper D, Puopolo KM, Wi S, Escobar GJ . Combining immature and total neutrophil counts to predict early onset sepsis in term and late preterm newborns: use of the I/T2. Pediatr Infect Dis J 2014; 33: 798–802.
Cornbleet PJ . Clinical utility of the band count. Clin Lab Med 2002; 22: 101–136.
Arneth BM, Ragaller M, Hommel K, Tiebel O, Menschikowski M, Siegert G . Novel parameters of extended complete blood cell count under fluorescence flow cytometry in patients with sepsis. J Clin Lab Anal 2014; 28: 130–135.
Becker PH, Fenneteau O, Da Costa L . Performance evaluation of the Sysmex XN-1000 hematology analyzer in assessment of the white blood cell count differential in pediatric specimens. Int J Lab Hematol 2016; 38: 54–63.
Wong EC . Hematology analyzers: special considerations for pediatric patients. Clin Lab Med 2015; 35: 165–181.
Chabot-Richards DS, George TI . White blood cell counts: reference methodology. Clin Lab Med 2015; 35: 11–24.
Kim H, Hur M, Choi SG, Moon HW, Yun YM, Hwang HS et al. Performance evaluation of Sysmex XN hematology analyzer in umbilical cord blood: a comparison study with Sysmex XE-2100. Clin Chem Lab Med 2014; 52: 1771–1779.
Wiland EL, Sandhaus LM, Georgievskaya Z, Hoyen CM, O'Riordan MA, Nock ML . Adult and child automated immature granulocyte norms are inappropriate for evaluating early-onset sepsis in newborns. Acta Paediatr 2014; 103: 494–497.
Nigro KG, O'Riordan M, Molloy EJ, Walsh MC, Sandhaus LM . Performance of an automated immature granulocyte count as a predictor of neonatal sepsis. Am J Clin Pathol 2005; 123: 618–624.
Boggs DR, Marsh JC, Chervenick PA, Cartwright GE, Wintrobe MM . Neutrophil releasing activity in plasma of normal human subjects injected with endotoxin. Proc Soc Exp Biol Med 1968; 127: 689–693.
Christensen RD, Shigeoka AO, Hill HR, Rothstein G . Circulating and storage neutrophil changes in experimental type II group B streptococcal sepsis. Pediatr Res 1980; 14: 806–808.
Novak RW . The beleaguered band count. Clin Lab Med 1993; 13: 895–903.
Gagon TE, Athens JW, Boggs DR, Cartwright GE . An evaluation of the variance of leukocyte counts as performed with the hemocytometer, Coulter, and Fisher intruments. Tech Bull Regist Med Technol 1966; 36: 274–281.
Bernstein LH, Rucinski J . Measurement of granulocyte maturation may improve the early diagnosis of the septic state. Clin Chem Lab Med 2011; 49: 2089–2095.
Fernandes B, Hamaguchi Y . Automated enumeration of immature granulocytes. Am J Clin Pathol 2007; 128: 454–463.
Ha SO, Park SH, Park SH, Park JS, Huh JW, Lim CM et al. Fraction of immature granulocytes reflects severity but not mortality in sepsis. Scand J Clin Lab Invest 2015; 75: 36–43.
Walker RI, Willemze R . Neutrophil kinetics and the regulation of granulopoiesis. Rev Infect Dis 1980; 2: 282–292.
Skubitz KM . Neutrophilic leukocytes. In: Greer JP, Arber DA, List AF, Glader B, Means RT, Paraskevas F et al. Wintrobe's Clinical Hematology. Lippincott, Williams & Wilkins: Philadelphia, 2014; 2003: p137.
Marsh JC, Boggs DR, Cartwright GE, Wintrobe MM . Neutrophil kinetics in acute infection. J Clin Invest 1967; 46: 1943–1953.
Engle WA, McGuire WA, Schreiner RL, Yu PL . Neutrophil storage pool depletion in neonates with sepsis and neutropenia. J Pediatr 1988; 113: 747–749.
Cairo MS . Neutrophil storage pool depletion in neonates with sepsis. J Pediatr 1989; 114: 1064–1065.
Henry E, Walker D, Wiedmeier SE, Christensen RD . Hematological abnormalities during the first week of life among neonates with Down syndrome: data from a multihospital healthcare system. Am J Med Genet A 2007; 143A: 42–50.
Wheeler JG, Chauvenet AR, Johnson CA, Dillard R, Block SM, Boyle R et al. Neutrophil storage pool depletion in septic, neutropenic neonates. Pediatr Infect Dis 1984; 3: 407–409.
Acknowledgements
We thank Theodore J. Pysher, Professor of Pathology, University of Utah and Director Of Clinical Pathology Primary Children’s Hospital, and Christopher M. Lehman, Professor of Pathology University of Utah and Medical Director Of Clinical Pathology, University of Utah Hospital for helpful discussions and for reviewing the manuscript. We also thank Dr. Jolanta Kunicka and Lance Kocherhans of Sysmex America Inc. for helpful discussions. We also thank the following members of the Intermountain Healthcare Clinical Laboratory staff for extracting data from the hematology analyzers; Robert Childs, Dereck Daniels, Robert Dallin, Rachael Ethington, Dave Garner, Laurie Jeffs, Jennessa Jessop, Heather Kuusela, Chris Partington, Tim Patten, Brooke Qi, Lauralyn Ragin, Tara Regginello, Aba Saunders, Alicia Simon, Jennifer Sorensen, Thomas Taylor, Ashley Windsor and Ryan Wilcox. The study was supported by a research grant (to RDC) from the Intermountain Research and Medical Foundation, Murray, UT, USA.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
MacQueen, B., Christensen, R., Yoder, B. et al. Comparing automated vs manual leukocyte differential counts for quantifying the ‘left shift’ in the blood of neonates. J Perinatol 36, 843–848 (2016). https://doi.org/10.1038/jp.2016.92
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2016.92
- Springer Nature America, Inc.
This article is cited by
-
Reconciling markedly discordant values of serum ferritin versus reticulocyte hemoglobin content
Journal of Perinatology (2021)
-
Neonates with suspected microangiopathic disorders: performance of standard manual schistocyte enumeration vs. the automated fragmented red cell count
Journal of Perinatology (2019)