Abstract
Purposes
Evaluate the effect of a 4-h prosection-based surgical anatomy training session on medical student anatomical knowledge and confidence. Compare the effect of the training between two student cohorts.
Methods
Two cohorts participated in the study. “Legacy” students received a 91-h dissection-based anatomy course in their pre-clinical curriculum. “NextGen” students received 14 h of pre-clinical anatomy training without dissection. Both cohorts participated in the surgical anatomy training session during their surgery clerkship. The session consisting of six stations: anterior abdominal wall, hepatobiliary, stomach/small intestine, colon/rectum, neck/breast, and cardiothoracic. Pre- and post-session tests assessed student confidence in and knowledge of surgical anatomy.
Results
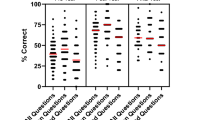
Two hundred and ninety four medical students completed the anatomy training. Overall scores increased 21% from pre-test (50 ± 19%) to post-test (71 ± 17%, p < 0.001). NextGen students scored lower than Legacy medical students on both the pre-test (44 ± 17% vs. 58 ± 20%, p < 0.001) and post-test (65 ± 16% vs. 81 ± 15%, p < 0.001). Student’s confidence in their understanding of general surgical anatomy improved from a Likert score of 2 [1–3] pre-session to 3 [2–4] post-session, p < 0.001. Compared to Legacy Students, NextGen students reported lower confidence pre-session (1 [1–2] vs. 3 [2–4], p < 0.001) and post-session (3 [2–4] vs. 4 [4–4], p < 0.001).
Conclusions
This innovative prosection-based surgical anatomy teaching model demonstrates an effective method to improve medical student knowledge of, and confidence in, surgical anatomy. However, the difference in performance between the two student cohorts demonstrates that prosection-based teaching cannot replace or fully compensate for a pre-clinical, dissection-based anatomy curriculum.





Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Drake RL, McBride JM, Pawlina W. An update on the status of anatomical sciences education in United States medical schools. Anat Sci Educ. 2014. https://doi.org/10.1002/ase.1468.
McBride JM, Drake RL. National survey on anatomical sciences in medical education. Anat Sci Educ. 2018. https://doi.org/10.1002/ase.1760.
Brooks WS, et al. Integration of gross anatomy in an organ system-based medical curriculum: strategies and challenges. Anat Sci Educ. 2015. https://doi.org/10.1002/ase.1483.
Estai M, Bunt S. Best teaching practices in anatomy education: a critical review. Ann Anat. 2016. https://doi.org/10.1016/j.aanat.2016.02.010.
Hu M, Wattchow D, de Fontgalland D. From ancient to avant-garde: a review of traditional and modern multimodal approaches to surgical anatomy education. ANZ J Surg. 2018. https://doi.org/10.1111/ans.14189.
Mitchell R, Batty L. Undergraduate perspectives on the teaching and learning of anatomy. ANZ J Surg. 2009. https://doi.org/10.1111/j.1445-2197.2008.04826.x.
Insull PJ, Kejriwal R, Blyth P. Surgical inclination and anatomy teaching at the University of Auckland. ANZ J Surg. 2006. https://doi.org/10.1111/j.1445-2197.2006.03942.x.
Ahmad K, et al. Addressing the failures of undergraduate anatomy education: dissecting the issue and innovating a solution. Ann Med Surg (Lond). 2021. https://doi.org/10.1016/j.amsu.2020.12.024.
Fillmore EP, et al. Understanding the current anatomical competence landscape: comparing perceptions of program directors, residents, and fourth-year medical students. Anat Sci Educ. 2016. https://doi.org/10.1002/ase.1578.
Sheikh AH, et al. Cadaveric anatomy in the future of medical education: what is the surgeons view? Anat Sci Educ. 2016. https://doi.org/10.1002/ase.1560.
Mechaber AJ, et al. University of Miami Leonard M. Miller School of Medicine. Acad Med. 2020. https://doi.org/10.1097/ACM.0000000000003459.
Harris PA, et al. Research electronic data capture (REDCap)—a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009. https://doi.org/10.1016/j.jbi.2008.08.010.
Stroumsa D, et al. The power and limits of classification—a 32-year-old man with abdominal pain. N Engl J Med. 2019. https://doi.org/10.1056/NEJMp1811491.
Flack N, Nicholson HD. What do medical students learn from dissection? Anat Sci Educ. 2018. https://doi.org/10.1002/ase.1758.
Ghosh SK. Cadaveric dissection as an educational tool for anatomical sciences in the 21st century. Anat Sci Educ. 2017. https://doi.org/10.1002/ase.1649.
McLachlan JC, Patten D. Anatomy teaching: ghosts of the past, present and future. Med Educ. 2006. https://doi.org/10.1111/j.1365-2929.2006.02401.x.
Bockers A, et al. The gross anatomy course: an analysis of its importance. Anat Sci Educ. 2010. https://doi.org/10.1002/ase.124.
Are C, et al. An experience in surgical anatomy to provide first-year medical students with an early exposure to general surgery: a pilot study. J Surg Educ. 2009. https://doi.org/10.1016/j.jsurg.2009.04.005.
Ferlauto HR, et al. A novel model for a student-led surgical anatomy seminar. J Surg Educ. 2021. https://doi.org/10.1016/j.jsurg.2020.07.029.
Hammer N, et al. Teaching surgical exposures to undergraduate medical students: an integration concept for anatomical and surgical education. Arch Orthop Trauma Surg. 2015. https://doi.org/10.1007/s00402-015-2217-7.
Bockers A, et al. Ready for the OR?—Clinical anatomy and basic surgical skills for students in their preclinical education. GMS Z Med Ausbild. 2011. https://doi.org/10.3205/zma000757.
Haubert LM, Jones K, Moffatt-Bruce SD. Surgical clinical correlates in anatomy: design and implementation of a first-year medical school program. Anat Sci Educ. 2009. https://doi.org/10.1002/ase.108.
Ozcan S, et al. Impact of cadaveric surgical anatomy training on urology residents knowledge: a preliminary study. Turk J Urol. 2015. https://doi.org/10.5152/tud.2015.87422.
Sharma G, et al. A cadaveric procedural anatomy course enhances operative competence. J Surg Res. 2016. https://doi.org/10.1016/j.jss.2015.09.037.
Farey JE, et al. Predictors of confidence in anatomy knowledge for work as a junior doctor: a national survey of Australian medical students. BMC Med Educ. 2018. https://doi.org/10.1186/s12909-018-1280-5.
Orsbon CP, Kaiser RS, Ross CF. Physician opinions about an anatomy core curriculum: a case for medical imaging and vertical integration. Anat Sci Educ. 2014. https://doi.org/10.1002/ase.1401.
Bergman EM, van der Vleuten CP, Scherpbier AJ. Why don’t they know enough about anatomy? A narrative review. Med Teach. 2011. https://doi.org/10.3109/0142159X.2010.536276.
Hagan EA, Jaffe BM. Effect of curriculum changes on student performance during general surgical clerkship. J Surg Educ. 2018. https://doi.org/10.1016/j.jsurg.2017.08.020.
Bockers A, Mayer C, Bockers TM. Does learning in clinical context in anatomical sciences improve examination results, learning motivation, or learning orientation? Anat Sci Educ. 2014. https://doi.org/10.1002/ase.1375.
Carmichael H, et al. “Bedside Anatomy”: a tool to contextualize learning and introduce surgical careers. J Surg Res. 2020. https://doi.org/10.1016/j.jss.2019.12.015.
Nutt J, et al. Cadaveric surgery: a novel approach to teaching clinical anatomy. Clin Teach. 2012. https://doi.org/10.1111/j.1743-498X.2012.00536.x.
Acker R, et al. Eyes of the beholders: first-year medical students’ perceptions of surgeons and the field of surgery. Am J Surg. 2021. https://doi.org/10.1016/j.amjsurg.2021.10.019.
McKinley SK, et al. Medical students’ perceptions and motivations prior to their surgery clerkship. Am J Surg. 2019. https://doi.org/10.1016/j.amjsurg.2019.01.010.
McKinley SK, et al. Enhancing the formal preclinical curriculum to improve medical student perception of surgery. J Surg Educ. 2020. https://doi.org/10.1016/j.jsurg.2020.02.009.
Naylor RA, Reisch JS, Valentine RJ. Do student perceptions of surgeons change during medical school? A longitudinal analysis during a 4-year curriculum. J Am Coll Surg. 2010. https://doi.org/10.1016/j.jamcollsurg.2009.12.016.
Hill EJR, et al. Can I cut it? Medical students’ perceptions of surgeons and surgical careers. Am J Surg. 2014. https://doi.org/10.1016/j.amjsurg.2014.04.016.
Kozar RA, et al. Brief intervention by surgeons can influence students toward a career in surgery. J Surg Res. 2003. https://doi.org/10.1016/s0022-4804(03)00104-5.
Kozar RA, et al. Preclinical students: who are surgeons? J Surg Res. 2004. https://doi.org/10.1016/j.jss.2004.03.024.
Are C, et al. The influence of surgical demonstrations during an anatomy course on the perceptions of first-year medical students toward surgeons and a surgical career. J Surg Educ. 2010. https://doi.org/10.1016/j.jsurg.2010.07.016.
Acknowledgements
Thank you to Brandon Rose, MD, MPH (TheCodingDocs.com) for his help in using RStudio to create the figures for this project. This project would not have been possible without the support of the anatomy faculty at the University of Miami Miller School of Medicine. A special thank you to Shawn Hunt PhD., Bryon Smith DPT., and the many student volunteers that helped to prosect for and teach during each of the anatomy training sessions. The authors are grateful to those altruistic individuals who donated their bodies to the State of Florida Anatomical Board at the University of Miami Miller School of Medicine (sofab.med.miami.edu). These individuals have helped to educate over 400 medical students in the intricacies of human anatomy and the professional practice of medicine, and without their selfless donation, this research would not have been possible.
Funding
No funding was received to assist with the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Material preparation, data collection, and analysis were performed by AJD, RAS, and CTH. Anatomical illustrations were drawn by EDR. The manuscript was written by AJD. All the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all the authors, the corresponding author states that there is no conflict of interest.
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. This study was reviewed and deemed exempt by the University of Miami Institutional Review Board as the research was conducted in an established educational setting that involved normal educational practices that are not likely to adversely impact students’ opportunity to learn required educational content.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Draper, A.J., Saberi, R.A., Huerta, C.T. et al. A prosection-based surgical anatomy training session that improves medical student anatomical knowledge and confidence on the surgery clerkship. Global Surg Educ 1, 68 (2022). https://doi.org/10.1007/s44186-022-00074-5
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s44186-022-00074-5