Abstract
Objective
Glucomannan is a dietary fiber that slows the absorption of carbohydrates and suppresses appetite, thereby reducing blood glucose. This meta-analysis sought to examine the effect of glucomannan supplementation on Fasting Blood Glucose (FBG) and Postprandial Glucose (PPG) in adults.
Method
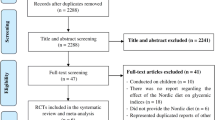
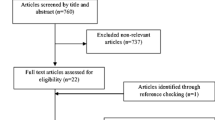
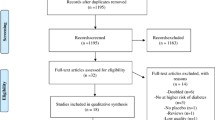
We searched PubMed, and SCOPUS databases, and Google Scholar from inception to May 2020, using relevant keywords. All randomized controlled clinical trials (RCTs) that examined the effect of glucomannan supplementation on FBG and PPG in adults were included. Weighted mean differences (WMD) and their 95% confidence interval (CI) were calculated using Stata. Subgroup analysis was used to discern possible sources of heterogeneity.
Results
Overall, 6 trials were included, consisting of 124 participants. We found that glucomannan supplementation significantly reduced FBG (WMD): -0.60 mmol/L, 95% CI: -1.16, -0.05; P=0.03, but not PPG (WMD: -2.07mmol/L ; 95% CI: -5.09, 0.95; P=0.18), compared with controls group. We conducted subgroup analysis based on dosage and duration of intervention and health status of the population. Findings from subgroup analysis revealed a significant effect of glucomannan supplementation on FBG in diabetic patients (WMD: -1.28 mmol/L, 95% CI: -2.54, -0.02; P=0.04).
Conclusion
Glucomannan supplementation can elicit significant reductions in FBG, but has no significant impact on PPG, in adults. More RCTs may find the exact effect of glucomannan on FBG and PPG.



Similar content being viewed by others
Data availability
Not applicable.
Abbreviations
- CI:
-
Confidence Intervals
- DM:
-
Diabetes mellitus
- FBG:
-
Fasting Blood Glucose
- IDF:
-
International Diabetes Federation
- IR:
-
Insulin Resistance
- KGM:
-
konjac Glucomannan
- KM:
-
Konjac-Mannan
- LDL-C:
-
Low-Density Lipoprotein Cholesterol
- LEA:
-
Lower-Extremity Amputations
- MeSH:
-
Medical Subject Headings
- MNT:
-
Medical Nutrition Therapy
- PPG:
-
Postprandial Glucose
- PRISMA-P:
-
Preferred Reporting Items for Systematic Review and Meta-Analysis Protocols
- RCTs:
-
Randomized Controlled Trials
- SEM:
-
Standard Error of the Mean
- TC:
-
Total Cholesterol
- T2DM:
-
Type 2 Diabetes Mellitus
- WMD:
-
Weighted Mean Differences
References
Hassanein M, Amod A, Khunti K, Lee MK, Mohan V. Introduction: Real-world evidence in type 2 diabetes. Diabetes Ther. 2020;11(2):29–32.
Zahed K, Sasangohar F, Mehta R, Erraguntla M, Qaraqe K: Diabetes management experience and the state of hypoglycemia: A national online survey. J MIR Diabetes 2020.
Khazrai YM, Defeudis G, Pozzilli P. Effect of diet on type 2 diabetes mellitus: a review. Diabetes Metab Res Rev. 2014;30(Suppl 1):24–33.
Kaura Parbhakar K, Rosella LC, Singhal S, Quinonez CR. Acute and chronic diabetes complications associated with self-reported oral health: a retrospective cohort study. BMC Oral Health. 2020;20:66.
Ly F, Dan W, Wei C, Wu A. Vascular cognitive impairment and dementia in type 2 diabetes mellitus: An overview. Life Sci. 2020;254:117771.
Moscovici K, Wainstock T, Sheiner E, Pariente G. The association between family history of diabetes mellitus and offspring long-term neurological hospitalisation. Acta Paediatr. 2020;109:1236–42.
Bitton S, Wainstock T, Sheiner E, Landau D, Avigan L, Pariente G. Is there an association between family history of diabetes mellitus and long-term cardiovascular hospitalizations of offspring? Prim Care Diabetes. 2019;13:529–34.
Wild S, Roglic G, Green A, Sicree R, King H. Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care. 2004;27:1047–53.
Hossain P, Kawar B, El Nahas M. Obesity and diabetes in the develo** world--a growing challenge. N Engl J Med. 2007;356:213–5.
Irene R. Diabetes Mellitus and Stroke - A cross Sectional Study of 2.5 Million Adults in the United States. Maedica (Buchar). 2020;15:24–31.
Hackett RA, Steptoe A. Type 2 diabetes mellitus and psychological stress - a modifiable risk factor. Nat Rev Endocrinol. 2017;13:547–60.
Zheng Y, Ley SH, Hu FB. Global aetiology and epidemiology of type 2 diabetes mellitus and its complications. Nat Rev Endocrinol. 2018;14:88–98.
Harding JL, Pavkov ME, Magliano DJ, Shaw JE, Gregg EW. Global trends in diabetes complications: a review of current evidence. Diabetologia. 2019;62:3–16.
Simpson TC, Weldon JC, Worthington HV, Needleman I, Wild SH, Moles DR, Stevenson B, Furness S, Iheozor-Ejiofor Z: Treatment of periodontal disease for glycaemic control in people with diabetes mellitus. Cochrane Database Syst Rev 2015:Cd004714.
Birkeland E, Gharagozlian S, Birkeland KI, Valeur J, Mage I, Rud I, Aas AM. Prebiotic effect of inulin-type fructans on faecal microbiota and short-chain fatty acids in type 2 diabetes: a randomised controlled trial. Eur J Nutr. 2020;59(7):3325–38.
5. Lifestyle Management. Standards of Medical Care in Diabetes-2019. Diabetes Care. 2019;42:S46–s60.
Suwannaporn P, Tester RF, Al-Ghazzewi FH, Artitdit P. Effect of short term administration of konjac glucomannan hydrolysates on adult blood lipid parameters and glucose concentrations. Nutr Food Sci. 2015;45(4):616–24.
Chearskul S, Sangurai S, Nitiyanant W, Kriengsinyos W, Kooptiwut S, Harindhanavudhi T. Glycemic and lipid responses to glucomannan in Thais with type 2 diabetes mellitus. Med J Med Assoc Thailand. 2007;90:2150.
Martino F, Martino E, Morrone F, Carnevali E, Forcone R, Niglio T. Effect of dietary supplementation with glucomannan on plasma total cholesterol and low density lipoprotein cholesterol in hypercholesterolemic children. Nutr Metab Cardiovasc Dis. 2005;15:174–80.
Yoshida M, Vanstone CA, Parsons WD, Zawistowski J, Jones PJ. Effect of plant sterols and glucomannan on lipids in individuals with and without type II diabetes. Eur J Clin Nutr. 2006;60:529–37.
Chen HL, Sheu WH, Tai TS, Liaw YP, Chen YC. Konjac supplement alleviated hypercholesterolemia and hyperglycemia in type 2 diabetic subjects--a randomized double-blind trial. J Am Coll Nutr. 2003;22:36–42.
Birketvedt GS, Shimshi M, Erling T, Florholmen J. Experiences with three different fiber supplements in weight reduction. Med Sci Monit. 2005;11:Pi5–8.
Vuksan V, Sievenpiper JL, Owen R, Swilley JA, Spadafora P, Jenkins DJ, Vidgen E, Brighenti F, Josse RG, Leiter LA, et al. Beneficial effects of viscous dietary fiber from Konjac-mannan in subjects with the insulin resistance syndrome: results of a controlled metabolic trial. Diabetes Care. 2000;23:9–14.
Jenkins DJ, Jenkins AL, Wolever TM, Vuksan V, Rao AV, Thompson LU, Josse RG. Low glycemic index: lente carbohydrates and physiological effects of altered food frequency. Am J Clin Nutr. 1994;59:706s–9s.
Vuksan V, Jenkins DJ, Spadafora P, Sievenpiper JL, Owen R, Vidgen E, Brighenti F, Josse R, Leiter LA, Bruce-Thompson C. Konjac-mannan (glucomannan) improves glycemia and other associated risk factors for coronary heart disease in type 2 diabetes. A randomized controlled metabolic trial. Diabetes Care. 1999;22:913–9.
Sood N, Baker WL, Coleman CI. Effect of glucomannan on plasma lipid and glucose concentrations, body weight, and blood pressure: systematic review and meta-analysis. Am J Clin Nutr. 2008;88:1167–75.
Silva FM, Kramer CK, de Almeida JC, Steemburgo T, Gross JL, Azevedo MJ. Fiber intake and glycemic control in patients with type 2 diabetes mellitus: a systematic review with meta-analysis of randomized controlled trials. Nutr Rev. 2013;71:790–801.
Devaraj RD, Reddy CK, Xu B. Health-promoting effects of konjac glucomannan and its practical applications: A critical review. Int J Biol Macromol. 2019;126:273–81.
Wood RJ, Fernandez ML, Sharman MJ, Silvestre R, Greene CM, Zern TL, Shrestha S, Judelson DA, Gomez AL, Kraemer WJ. Effects of a carbohydrate-restricted diet with and without supplemental soluble fiber on plasma low-density lipoprotein cholesterol and other clinical markers of cardiovascular risk. Metabolism. 2007;56:58–67.
Keithley JK, Swanson B, Mikolaitis SL, DeMeo M, Zeller JM, Fogg L, Adamji J. Safety and efficacy of glucomannan for weight loss in overweight and moderately obese adults. J Obes. 2013;2013:610908.
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev. 2015;4:1.
DerSimonian R, Kacker R. Random-effects model for meta-analysis of clinical trials: an update. Contemp Clin Trials. 2007;28:105–14.
Wan X, Wang W, Liu J, Tong T. Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol. 2014;14:135.
Zhang L, Han Y, Zhao Z, Liu X, Xu Y, Cui G, Zhang X, Zhang R. Beneficial effects of konjac powder on lipid profile in schizophrenia with dyslipidemia: A randomized controlled trial. Asia Pac J Clin Nutr. 2020;29:505–12.
Morgan L, Tredger J, Wright J, Marks V. The effect of soluble-and insoluble-fibre supplementation on post-prandial glucose tolerance, insulin and gastric inhibitory polypeptide secretion in healthy subjects. Br J Nutr. 1990;64:103–10.
Chen H, Nie Q, Hu J, Huang X, Zhang K, Pan S, Nie S. Hypoglycemic and hypolipidemic effects of glucomannan extracted from konjac on type 2 diabetic rats. J Agric Food Chem. 2019;67:5278–88.
Boers HM, MacAulay K, Murray P, Ten Hoorn JS, Hoogenraad A-R, Peters HP, Vente-Spreeuwenberg MA, Mela DJ. Efficacy of different fibres and flour mixes in South-Asian flatbreads for reducing post-prandial glucose responses in healthy adults. Eur J Nutr. 2017;56:2049–60.
Funding
This study was supported by the Department of Community Nutrition, School of Nutritional Sciences and Dietetics, Tehran University of Medical Sciences (TUMS). The funding bodies played no role in the design of the study and collection, analysis, and interpretation of data and in writing the manuscript.
Author information
Authors and Affiliations
Contributions
AM and RZ contributed to the study concept and design; MRA and RZ designed search strategy and screened Papers; SM performed statistical analysis; AM, RZ, NR, SP and FA wrote the first draft of the manuscript; KhM was supervisor of the article; all authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
There is no competing interest in this study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(PDF 82 kb)
Rights and permissions
About this article
Cite this article
Mirzababaei, A., Zandkarimi, R., Moradi, S. et al. The effect of Glucomannan on fasting and postprandial blood glucose in adults: a systematic review and meta-analysis of randomized controlled trials. J Diabetes Metab Disord 21, 1055–1063 (2022). https://doi.org/10.1007/s40200-022-00993-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40200-022-00993-6