Abstract
Context
ACL injury continues to be the largest single problem in orthopedic sports medicine. MRI has become the prime diagnostic tool of the various knee pathological and anatomical variability conditions.
Aim
To test the integrity of the new combined method for assessment of tibial plateau anatomic variables using conventional MRI.
Settings and design
Retrospective control study.
Methods
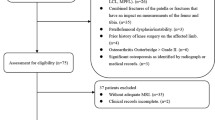
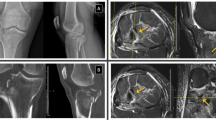
We evaluated the medial tibial plateau slope (MTPS), lateral tibial plateau slope (LTPS), and medial tibial plateau depth (MTPD) in ACL-injured group of patients (156) and non-ACL-injured control group (93) using MRI scan. Inclusion criteria for ACL-injured group—as surgically confirmed—were isolated ACL injury, while inclusion criteria for non-ACL-injured group were minor trauma, bruises, etc.
Statistical analysis used
Student’s t test and ICC were used. A p value of <0.05 was assigned as significant.
Results
Both male and female patients in the ACL-injured group showed increased LTPS in comparison to control group (p = 0.0197), whereas no significant difference in MTPS and MTPD was detected (p = 0.75 and 0.9, respectively). Steeper LTPS was detected in males of the patient group than in control group (p = 0.0001). Control group males had less steep MTPS (p = 0.002) and LTPS (p = 0.035) and deeper MTPD (p = 0.004) than control group females.
Conclusion
We conclude that the combined method conducted by Khan et al. (Int Orthop (SICOT) 2011 35(8):1251–1256) using conventional MRI for measurement of MTPS, LTPS, and MTPD as risk factors for ACL injury is solid and reproducible.
Level of evidence: III. Diagnostic study









Similar content being viewed by others
References
Barry P, Boden M, Letha Y et al (2000) Etiology and Prevention of Noncontact ACL Injury. Phys Sportsmed 28(4):53–60
Griffin L, Albohm M, Arendt E et al (2006) Understanding and preventing noncontact anterior cruciate ligament injuries: A review of the Hunt Valley II meeting. Am J Sports Med 34(9):1512–1532
Renstrom P, Ljungqvist A, Arendt E et al (2008) Non-contact ACL injuries in female athletes: An International Olympic Committee current concepts statement. Br J Sports Med 42(6):394–412
Toth A, Cordasco F (2001) Anterior cruciate ligament injuries in the female athlete. J Gend Specif Med 4:25–34
Neuman P, Englund M, Kostogiannis I et al (2008) Prevalence of tibiofemoral osteoarthritis 15 years after nonoperative treatment of anterior cruciate ligament injury: A prospective cohort study. Am J Sports Med 36(9):1717–1725
McLean SG, Mélanie L (2010) Complex Integrative Morphological and Mechanical Contributions to ACL Injury Risk. Exerc Sport Sci Rev Am Coll Sports Med 38(4):192–200
Khan MS, Seon JK, Song EK (2011) Risk factors for anterior cruciate ligament injury: Assessment of tibial plateau anatomic variables on conventional MRI using a new combined method. Int Orthop (SICOT) 35(8):1251–1256. doi:10.1007/s00264-011-1217-7
Hashemi J, Naveen C, Brian G et al (2008) The geometry of the tibial plateau and its influence on the biomechanics of the tibiofemoral joint. J Bone Joint Surg Am 90:2724–2734
Souryal T, Moore H, Evans J (1988) Bilaterality in anterior cruciate ligament injuries: Associated intercondylar notch stenosis. Am J Sports Med 16:449–454
Shelbourne K, Facibene W, Hunt J (1997) Radiographic and intraoperative intercondylar notch width measurements in men and women with unilateral and bilateral anterior cruciate ligament tears. Knee Surg Sports Traumatol Arthrosc 5:229–233
Domzaliski M, Grzelak P, Gabos P (2010) Risk factors for anterior cruciate ligament injury in skeletally immature patients: Analysis of intercondylar notch width using magnetic resonance imaging. Int Orthop 34(5):703–707
Hashemi J, Naveen C, Hossein M et al (2010) Shallow medial tibial plateau and steep medial and lateral tibial slopes: New risk factors for anterior cruciate ligament injuries. Am J Sports Med 38(1):54–62
Stulberg S (2003) How accurate is current TKR instrumentation? Clin Orthop Relat Res 416:177–184
Bai B, Kummer F, Sala DA et al (2001) Effect of articular step-off and meniscectomy on joint alignment and contact pressures for fractures of the lateral tibial plateau. J Orthop Trauma 15:101–106
Waelchli B, Romero J (2001) Dislocation of the polyethylene inlay due to anterior tibial slope in revision total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 9:296–298
Hudek R, Silvia S, Felix R et al (2009) Novel measurement technique of the medial tibial slope on conventional MRI. Clin Orthop Relat Res 467(8):2066–2072
Griffin L, Albohm M, Arendt E et al (2006) Update on ACL prevention: Theoretical and practical guidelines. Am J Sports Med 34:1512–1532
Stijak L, Herzog R, Schai P (2008) Is there an influence of the tibial slope of the lateral condyle on the ACL lesion? A case–control study. Knee Surg Sports Traumatol Arthrosc 6:112–117
Simon R, Everhart J, Nagaraja H et al (2010) A case–control study of anterior cruciate ligament volume, tibial plateau slopes and intercondylar notch dimensions in ACL-injured knees. J Biomech 43(9):1702–1707
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors declared no conflict of interest.
Rights and permissions
About this article
Cite this article
Ghandour, T.M., Abdelrahman, A.A., Talaat, A. et al. Can Khan’s new method using MRI integrable to detect tibial plateau slope and depth as risk factors for anterior cruciate tear?. Eur Orthop Traumatol 6, 439–444 (2015). https://doi.org/10.1007/s12570-015-0337-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12570-015-0337-8