Abstract
A novel coronavirus, later named SARS-CoV-2, was first reported in China in December 2019 and subsequently widely identified in the United States, Japan, South Korea, France, India, and other countries. The disease caused by SARS-CoV-2 infection was called COVID-19. The high fatality and morbidity rates of COVID-19 make it the third largest global epidemic in this century. However, there are currently no approved antiviral drugs for the COVID-19 treatment. Recently, two old antimalarial drugs, hydroxychloroquine and chloroquine, have been found to exert anti-SARS-CoV-2 effects both in vitro and in vivo. Preliminary clinical evidence suggests these drugs may have an effect on the treatment of COVID-19. Herein, we review the pharmacokinetics characteristics and antiviral effects of these drugs, in addition to their side effects and clinical evidence of their use for the COVID-19 treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
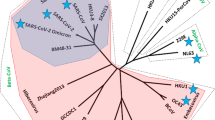
In December 2019, unexplained pneumonia cases were reported in Wuhan, China, which was later confirmed to be caused by a novel coronavirus identified as SARS-CoV-2. The clinical symptoms caused by this novel coronavirus were named as coronavirus disease 2019 (COVID-19) by World Health Organization (WHO). SARS-CoV-2 is a β-coronavirus and its genomic sequence is 96.2% identical to that of Bat-SARSs-CoV RaTG13 and 79.5% identical to that of SARS-CoV. Based on the sequencing results and evolutionary analysis of the viral genome, bats are suspected to be the natural hosts of SARS-CoV-2, while the intermediate host is unknown. Previous studies have shown that SARS-CoV-2, like SARS-CoV, can infect human cells that express angiotensin-converting enzyme 2 (ACE2) (Guo et al. 2020).
The most common symptoms of COVID-19 patients include fever, cough, fatigue, and myalgia. However, the disease can evolve in some cases and patients begin to experience dyspnea, shock, multiple organ damage and may even die (Huang et al. 2020). Studies estimate that the basic reproduction number (R0) of SARS-CoV-2 is about 2.2, but it can vary from 1.4 to 6.5 (Adhikari et al. 2020; Guo et al. 2020; Imai et al. 2020; Shen et al. 2015; Srinivasa et al. 2017).
On the other hand, patients who took these drugs for long periods experienced toxic effects, such as retinopathy, circular defects (or bull’s eye maculopathy), and retinal diameter defects, which are generally irreversible, mainly due to drug accumulation in the eye (Schrezenmeier and Dörner 2020). Among toxic effects, retinopathy is the more serious clinical problem that can cause irreversible damage to vision, and even blindness. The American Academy of Ophthalmology determined the risk factors for retinopathy due to HCQ use, which include a time of use greater than 5 years, a high daily drug dosage (HCQ > 5.0 mg/kg lean body mass; CQ > 2.3 mg/kg lean body mass), renal or liver disease patient, high body fat levels, use of concomitant drugs similar to tamoxifen, macular disease and age over 60 years (Marmor et al. 2016). Remarkably, the daily dose and duration of use are the main risk factors. When the HCQ daily dose exceeds 20 mg/kg, the incidence of retinopathy is a 25 to 40% within 1 to 2 years (Marmor et al. 2016). Although the use duration of HCQ and CQ in COVID-19 patients is generally very short, it is still necessary to be aware of their retinal toxicity. Retinal degeneration caused by HCQ and CQ can continue to develop even after treatment is stopped.
The CQ and HCQ side effects in the heart are mainly conduction disorders and cardiomyopathy, which are usually irreversible and fatal (Frisk-Holmberg et al. 1983; Tönnesmann et al. 2013). The cardiotoxicity of these drugs may be related to the their long-term use, which causes acquired lysosomal accumulation disorder. This eventually leads to drug-induced cardiomyopathy, or in the case of excessive doses ingestion, acute poisoning (Yogasundaram et al. 2014). There is a case report of an elderly woman with lupus patient who used HCQ for a long time was diagnosed with refractory ventricular arrhythmia due to a prolonged QT interval. After excluding other causes, she was diagnosed with cardiac conduction abnormalities caused by chronic HCQ poisoning (Chen et al. 2006).
Because CQ and HCQ affect the cardiac conduction system, their use should be avoided in combination with other drugs that block cardiac conduction to prevent fatal arrhythmia. Among them, digitalis drugs (digoxin, desacetylgoxin, digitoxin, and trichoside K), antiarrhythmic drugs class Ia (quinidine and procainamide), antiarrhythmic drugs class III (amiodarone, sotalol, ibutilide, and dronedarone), benpredil, hydrochlorothiazide, and indapamide. In addition, the CQ/HCQ combination with antibiotics, such as quinolones and macrolides, should be prohibited to avoid the risk of promoting the QT interval prolongation and leading to tip torsion. In addition, it is worth mentioning that the interval between the therapeutic and toxic doses of CQ and HCQ is narrow, and acute CQ poisoning is associated with a potential life-threatening cardiovascular disease (Touret and de Lamballerie 2020).
Regarding the nervous system, currently there is no experimental evidence that CQ, HCQ and their metabolites can affect its conduction properties. It is only known that quinine is neurotoxic to dopaminergic neurons in the limbic system (Zou et al. 2018). Further studies are needed to investigate the CQ and HCQ effects on the central and peripheral nervous systems. Therefore, the CQ and HCQ use should follow strict rules and self-medication is not recommended. Moreover, for patients using these drugs, ECG and echocardiographic monitoring should be performed regularly to early detect potential cardiac toxicity early (Yogasundaram et al. 2014).
Over the years, researchers have measured the correlation between CQ/HCQ and toxicity. Their toxicological properties are concentration-dependent. The concentration that causes mild side effects, such as dizziness, diplopia, and fatigue, is about 0.5 to 1.2 × 10–6 mol/L. According to previous reports, about 80% of patients with side effects have CQ/HCQ plasma concentration higher than 2.5 × 10–6 mol/L. On the other hand, no toxic reaction has been reported when their plasma concentration is below 1.25 × 10–6 mol/L. Finally, the critical plasma concentration of cardiovascular toxicity caused by CQ is about 1000 μg/L (3 × 10−6 mol/L) (Ducharme and Farinotti 1996).
Conclusion and suggestions
In summary, HCQ and CQ were found to have exert anti-SARS-CoV-2 effects both in vitro and in vivo, and represent potential treatment options for COVID-19 (Fig. 1). However, the clinical evidence of their effects is from some single-center clinical trials. Evidence from multi-center clinical trials is still lacking. In accordance with the pharmacological and toxicological effects of CQ and HCQ discussed here, the authors of this review recommend the following: (1) Multicenter randomized controlled clinical trials are needed to clarify the CQ and HCQ efficiency and safety in the COVID-19 treatment; (2) Considering their ocular, cardiac and neuro toxicities, CQ and HCQ should not be recommended as preventive drugs for the COVID-19 pandemic; (3) Follow-up of patients who received CQ or HCQ treatment is necessary to access their long-term effects and side effects; (4) The CQ and HCQ dosage and their combination regimen with other drugs in clinical trials should be appropriately adjusted.
Anti-SARS-CoV-2 effects of HCQ and CQ exert both in vitro and in vivo. Descriptive graphic shown the process of SARS-CoV-2 infection and replication, and the anti-SARS-CoV-2 effects of HCQ and CQ in it. (1) CQ and HCQ can glycosylate SARS-CoV-2 itself and its receptor. (2) CQ and HCQ can inhibit cell autophagy, which was involve in virus infection process. (3) CQ and HCQ can directly inhibit the replication of RNA viruses. (4) CQ and HCQ can directly inhibit the expression of SARS-CoV viral gene. (5) After CQ and HCQ directly enter the cell body, the intracellular pH rises and inhibits a series of viral replication and recombination processes
References
Adhikari SP, Meng S, Wu YJ, Mao YP, Ye RX, Wang QZ, Sun C, Sylvia S, Rozelle S, Raat H, Zhou H (2020) Epidemiology, causes, clinical manifestation and diagnosis, prevention and control of coronavirus disease (COVID-19) during the early outbreak period: a sco** review. Infect Dis Poverty 9:29. https://doi.org/10.1186/s40249-020-00646-x
Al-Bari MA (2015) Chloroquine analogues in drug discovery: new directions of uses, mechanisms of actions and toxic manifestations from malaria to multifarious diseases. J Antimicrob Chemother 70:1608–1621. https://doi.org/10.1093/jac/dkv018
Bishop NE (1998) Examination of potential inhibitors of hepatitis A virus uncoating. Intervirology 41:261–271. https://doi.org/10.1159/000024948
Chatre C, Roubille F, Vernhet H, Jorgensen C, Pers YM (2018) Cardiac complications attributed to chloroquine and hydroxychloroquine: a systematic review of the literature. Drug Saf 41:919–931. https://doi.org/10.1007/s40264-018-0689-4
Chen CY, Wang FL, Lin CC (2006) Chronic hydroxychloroquine use associated with QT prolongation and refractory ventricular arrhythmia. Clin Toxicol (Phila) 44:173–175. https://doi.org/10.1080/15563650500514558
Chen J, Liu D, Liu L, Liu P, Xu Q, **a L, Ling Y, Huang D, Song S, Zhang D (2020a) A pilot study of hydroxychloroquine in treatment of patients with moderate COVID-19. Zhejiang Da Xue Xue Bao Yi Xue Ban 49:215–219
Chen Z, Hu J, Zhang Z, Jiang S, Han S, Yan D, Zhuang R, Hu B, Zhang Z (2020b) Efficacy of hydroxychloroquine in patients with COVID-19: results of a randomized clinical trial. MedRxiv. https://doi.org/10.1101/2020.03.22.2004075
Cortegiani A, Ingoglia G, Ippolito M, Giarratano A, Einav S (2020) A systematic review on the efficacy and safety of chloroquine for the treatment of COVID-19. J Crit Care 57:279–283. https://doi.org/10.1016/j.jcrc.2020.03.005
Ducharme J, Farinotti R (1996) Clinical pharmacokinetics and metabolism of chloroquine. Focus on recent advancements. Clin Pharmacokinet 31:257–274. https://doi.org/10.2165/00003088-199631040-00003
EMA(European Medicines Agency) (2020) COVID-19: chloroquine and hydroxychloroquine only be used in clinical trials or emergency use programmes. Available at European Medicines Agency document Website https://www.ema.europa.eu/en/documents/press-release/covid-19-chloroquine-hydroxychloroquine-only-be-used-clinical-trials-emergency-use-programmes_en.pdf. Accessed 1 Apr 2020
FDA(US Food & Drug Administration) (2020) Re: Request for Emergency Use Authorization For Use of Chloroquine Phoslhate or Hydroxychloroquine Sulfate Supplied From the Strategic National Stockpile for Treatment of 2019 Covrnavirus Disease. US Food & Drug Administration official Website. Available at https://www.fda.gov/media/136534/download. Accessed 29 Mar 2020
Frisk-Holmberg M, Bergqvist Y, Englund U (1983) Chloroquine intoxication. Br J Clin Pharmacol 15:502–503. https://doi.org/10.1111/j.1365-2125.1983.tb01540.x
Furst DE (1996) Pharmacokinetics of hydroxychloroquine and chloroquine during treatment of rheumatic diseases. Lupus 5:S11–S15
Gautret P, Lagier JC, Parola P, Hoang VT, Meddeb L, Mailhe M, Doudier B, Courjon J, Giordanengo V, Vieira VE, Dupont HT, Honore S, Colson P, Chabriere E, La Scola B, Rolain JM, Brouqui P, Raoult D (2020a) Hydroxychloroquine and azithromycin as a treatment of COVID-19: results of an open-label non-randomized clinical trial. Int J Antimicrob Agents. https://doi.org/10.1016/j.ijantimicag.2020.105949
Gautret P, Lagier JC, Parola P, Hoang VT, Meddeb L, Sevestre J, Mailhe M, Doudier B, Aubry C, Amrane S, Seng P, Hocquart M, Eldin C, Finance J, Vieira VE, Tissot-Dupont HT, Honoré S, Stein A, Million M, Colson P, La Scola B, Veit V, Jacquier A, Deharo JC, Drancourt M, Fournier PE, Rolain JM, Brouqui P, Raoult D (2020b) Clinical and microbiological effect of a combination of hydroxychloroquine and azithromycin in 80 COVID-19 patients with at least a six-day follow up: an observational study. Travel Med Infect Dis 34:101663. https://doi.org/10.1016/j.tmaid.2020.101663
Guo YR, Cao QD, Hong ZS, Tan YY, Chen SD, ** HJ, Tan KS, Wang DY, Yan Y (2020) The origin, transmission and clinical therapies on coronavirus disease 2019 (COVID-19) outbreak–an update on the status. Mil Med Res 7:10–11. https://doi.org/10.1186/s40779-020-00240-0
Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, Zhang L, Fan G, Xu J, Gu X, Cheng Z, Yu T, **a J, Wei Y, Wu W, **e X, Yin W, Li H, Liu M, **ao Y, Gao H, Guo L, **e J, Wang G, Jiang R, Gao Z, ** Q, Wang J, Cao B (2020) Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. The Lancet 395:497–506. https://doi.org/10.1016/S0140-6736(20)30183-5
Imai N, Cori A, Dorigatti I, Baguelin M, Donnelly CA, Riley S, Ferguson NM (2020) Report 3: transmissibility of 2019-nCoV. Feminine-Perspective Magazine Web. Available at https://fpmag.net/wp-content/uploads/2020/01/Imperial-2019-nCoV-transmissibility.pdf. Accessed 29 Mar 2020
Inglot AD (1969) Comparison of the antiviral activity in vitro of some non-steroidal anti-inflammatory drugs. J Gen Virol 4:203–214. https://doi.org/10.1099/0022-1317-4-2-203
Keyaerts E, Vijgen L, Maes P, Neyts J, Van Ranst M (2004) In vitro inhibition of severe acute respiratory syndrome coronavirus by chloroquine. Biochem Biophys Res Commun 323:264–268. https://doi.org/10.1016/j.bbrc.2004.08.085
Keyaerts E, Li S, Vijgen L, Rysman E, Verbeeck J, Van Ranst M, Maes P (2009) Antiviral activity of chloroquine against human coronavirus OC43 infection in newborn mice. Antimicrob Agents Chemother 53:3416–3421. https://doi.org/10.1128/AAC.01509-08
Legssyer R, Josse C, Piette J, Ward RJ, Crichton RR (2003) Changes in function of iron-loaded alveolar macrophages after in vivo administration of desferrioxamine and/or chloroquine. J Inorg Biochem 94:36–42. https://doi.org/10.1016/s0162-0134(02)00633-5
Li C, Zhu X, Ji X, Quanquin N, Deng YQ, Tian M, Aliyari R, Zuo X, Yuan L, Afridi SK, Li XF, Jung JU, Nielsen-Saines K, Qin FX, Qin CF, Xu Z, Cheng G (2017) Chloroquine, a FDA-approved drug, prevents Zika Virus infection and its associated congenital microcephaly in mice. EBioMedicine 24:189–194. https://doi.org/10.1016/j.ebiom.2017.09.034
Liu J, Cao R, Xu M, Wang X, Zhang H, Hu H, Li Y, Hu Z, Zhong W, Wang M (2020) Hydroxychloroquine, a less toxic derivative of chloroquine, is effective in inhibiting SARS-CoV-2 infection in vitro. Cell Discov 6:16. https://doi.org/10.1038/s41421-020-0156-0
Marmor MF, Kellner U, Lai TY, Melles RB, Mieler WF, American Academy of Ophthalmology (2016) Recommendations on screening for chloroquine and hydroxychloroquine etinopathy (2016 Revision). Ophthalmology 123:1386–1394. https://doi.org/10.1016/j.ophtha.2016.01.058
Mediterranee-infection Hospital (2020) Countries and regions where hydroxychloroquine and chloroquine are recommended to fight coronavirus. Available at Mediterranee-infection Hospital Website https://www.mediterranee-infection.com/coronavirus-pays-ou-lhydroxychloroquine-est-recommandee. Accessed 28 Mar 2020
Mitjà O, Clotet B (2020) Use of antiviral drugs to reduce COVID-19 transmission. Lancet Glob Health 8:e639–e640. https://doi.org/10.1016/S2214-109X(20)30114-5
Molina JM, Delaugerre C, Le Goff J, Mela-Lima B, Ponscarme D, Goldwirt L, de Castro N (2020) No evidence of rapid antiviral clearance or clinical benefit with the combination of hydroxychloroquine and azithromycin in patients with severe COVID-19 infection. Med Mal Infect 50:384. https://doi.org/10.1016/j.medmal.2020.03.006
Motarjemizadeh Q, Aidenloo NS, Abbaszadeh M (2015) Detection of hydroxychloroquine retinal toxicity by automated perimetry in 60 rheumatoid arthritis patients with normal fundoscopic findings. Glob J Health Sci 8:59–64. https://doi.org/10.5539/gjhs.v8n3p59
Naarding MA, Baan E, Pollakis G, Paxton WA (2007) Effect of chloroquine on reducing HIV-1 replication in vitro and the DC-SIGN mediated transfer of virus to CD4+ T-lymphocytes. Retrovirology 4:6. https://doi.org/10.1186/1742-4690-4-6
Piller C (2020) Former FDA leaders decry emergency authorization of malaria drugs for coronavirus. Science Magazine NewWeb. Available at https://www.sciencemag.org/news/2020/04/former-fda-leaders-decry-emergency-authorization-malaria-drugs-coronavirus. Accessed 7 Apr 2020
Plantone D, Koudriavtseva T (2018) Current and future use of chloroquine and hydroxychloroquine in infectious, immune, neoplastic, and neurological diseases: a mini-review. Clin Drug Investig 38:653–671. https://doi.org/10.1007/s40261-018-0656-y
Randolph VB, Winkler G, Stollar V (1990) Acidotropic amines inhibit proteolytic processing of flavivirus prM protein. Virology 174:450–458. https://doi.org/10.1016/0042-6822(90)90099-d
Schrezenmeier E, Dörner T (2020) Mechanisms of action of hydroxychloroquine and chloroquine: implications for rheumatology. Nat Rev Rheumatol 16:155–166. https://doi.org/10.1038/s41584-020-0372-x
Sermo.Com (2020) Breaking Results: Sermo’s COVID-19 Real Time Barometer Study. Available at Sermo’s COVID-19-Barometer Web https://public-cdn.sermo.com/covid19/c8/be4e/4edbd4/dbd4ba4ac5a3b3d9a479f99cc5/wave-i-sermo-covid-19-global-analysis-final.pdf. Accessed 27 Mar 2020.
Shen M, Peng Z, **ao Y, Zhang L (2020) Modelling the epidemic trend of the 2019 novel coronavirus outbreak in China. Biorxiv. https://doi.org/10.1101/2020.01.23.916726
Shibata M, Aoki H, Tsurumi T, Sugiura Y, Nishiyama Y, Suzuki S, Maeno K (1983) Mechanism of uncoating of influenza B virus in MDCK cells: action of chloroquine. J Gen Virol 64:1149–1156. https://doi.org/10.1099/0022-1317-64-5-1149
Srinivasa A, Tosounidou S, Gordon C (2017) Increased Incidence of Gastrointestinal Side Effects in Patients Taking Hydroxychloroquine: A Brand-related Issue? J Rheumatol 44:398. https://doi.org/10.3899/jrheum.161063
Tan YW, Yam WK, Sun J, Chu JJH (2018) An evaluation of Chloroquine as a broad-acting antiviral against Hand, Foot and Mouth Disease. Antiviral Res 149:143–149. https://doi.org/10.1016/j.antiviral.2017.11.017
Tasanor O, Noedl H, Na-Bangchang K, Congpuong K, Sirichaisinthop J, Wernsdorfer WH (2002) An in vitro system for assessing the sensitivity of Plasmodium vivax to chloroquine. Acta Trop 83:49–61. https://doi.org/10.1016/s0001-706x(02)00056-6
Tönnesmann E, Kandolf R, Lewalter T (2013) Chloroquine cardiomyopathy—a review of the literature. Immunopharmacol Immunotoxicol 35:434–442. https://doi.org/10.3109/08923973.2013.780078
Touret F, de Lamballerie X (2020) Of chloroquine and COVID-19. Antiviral Res 177:104762. https://doi.org/10.1016/j.antiviral.2020.104762
Vincent MJ, Bergeron E, Benjannet S, Erickson BR, Rollin PE, Ksiazek TG, Seidah NG, Nichol ST (2005) Chloroquine is a potent inhibitor of SARS coronavirus infection and spread. Virol J 2:69. https://doi.org/10.1186/1743-422X-2-69
Voss A (2020) Official Statement from International Society of Antimicrobial Chemotherapy (ISAC). Available at International Society of Antimicrobial Chemotherapy PublicationWeb https://www.isac.world/news-and-publications/official-isac-statement. Accessed 3 Apr 2020.
Wang D, Hu B, Hu C, Zhu F, Liu X, Zhang J, Wang B, **ang H, Cheng Z, **ong Y, Zhao Y, Li Y, Wang X, Peng Z (2020a) Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA 323:1061–1069. https://doi.org/10.1001/jama.2020.1585
Wang M, Cao R, Zhang L, Yang X, Liu J, Xu M, Shi Z, Hu Z, Zhong W, **ao G (2020b) Remdesivir and chloroquine effectively inhibit the recently emerged novel coronavirus (2019-nCoV) in vitro. Cell Res 30:269–271. https://doi.org/10.1038/s41422-020-0282-0
WHO(World Helth Organization) (2020) Coronavirus disease (COVID-19) Situation Dashboard. Available at World Helth Organization Offical Web https://www.who.int/redirect-pages/page/novel-coronavirus-(covid-19)-situation-dashboard. Accessed 30 Apr 2020
Wu C, Chen X, Cai Y, **a J, Zhou X, Xu S, Huang H, Zhang L, Zhou X, Du C, Zhang Y, Song J, Wang S, Chao Y, Yang Z, Xu J, Zhou X, Chen D, **ong W, Xu L, Zhou F, Jiang J, Bai C, Zheng J, Song Y (2020) Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan, China. JAMA Intern Med 180:1–11. https://doi.org/10.1001/jamainternmed.2020.0994
Yan Y, Zou Z, Sun Y, Li X, Xu KF, Wei Y, ** N, Jiang C (2013) Anti-malaria drug chloroquine is highly effective in treating avian influenza A H5N1 virus infection in an animal model. Cell Res 23:300–302. https://doi.org/10.1038/cr.2012.165
Yogasundaram H, Putko BN, Tien J, Paterson DI, Cujec B, Ringrose J, Oudit GY (2014) Hydroxychloroquine-induced cardiomyopathy: case report, pathophysiology, diagnosis, and treatment. Can J Cardiol 30:1706–1715. https://doi.org/10.1016/j.cjca.2014.08.016
Zhang JJ, Dong X, Cao YY, Yuan YD, Yang YB, Yan YQ, Akdis CA, Gao YD (2020) Clinical characteristics of 140 patients infected with SARS-CoV-2 in Wuhan, China. Allergy 75:1730–1741. https://doi.org/10.1111/all.14238
Zou L, Xue Y, Jones M, Heinbockel T, Ying M, Zhan X (2018) The effects of quinine on neurophysiological properties of dopaminergic neurons. Neurotox Res 34:62–73. https://doi.org/10.1007/s12640-017-9855-1
Acknowledgements
This work was supported by grants from the National Natural Science Foundation of China (Grant Nos. 81822016 and 81771382) to Zhentao Zhang.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zou, L., Dai, L., Zhang, X. et al. Hydroxychloroquine and chloroquine: a potential and controversial treatment for COVID-19. Arch. Pharm. Res. 43, 765–772 (2020). https://doi.org/10.1007/s12272-020-01258-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12272-020-01258-7