Abstract
Purpose
The purpose of this study was to determine the effect of sulforaphane (SFN) on hepatic ischemia reperfusion injury (HIRI) and to explore the underlying mechanisms.
Methods
The rat model of HIRI was established. Thirty-two rats were randomly divided into sham (A), SFN (B), HIRI (C), and SFN + HIRI (D) groups. Animals in the HIRI and Sham groups were treated with equal volumes of the vehicle of SPF. Liver functions were evaluated by serum alanine aminotransferase (ALT) and aspartate aminotransferase (AST). Liver samples were collected for histological examination and determination of malondialdehyde (MDA), superoxide dismutase (SOD), glutathione (GSH), and glutathione peroxidase (GSH-Px) levels. Mitochondrial Na+–K+-ATPase and Ca2+-ATPase were measured by colorimetry. Expression levels of NQO1, Nrf2, and HO-1 in liver tissue were detected by western blot analysis. Additionally, oncosis and apoptosis were detected by Annexin V-FITC/PI immunofluorescent flow cytometry analysis.
Results
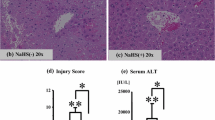
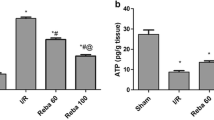
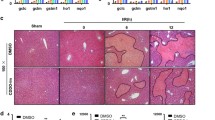
The HIRI group showed a significant increase in serum levels of liver enzymes (ALT, AST) associated with histopathological damage in the liver. Pre-treatment with SFN could reduce the levels of MDA and MPO in liver tissue and improve the activities of SOD, GSH, GSH-Px, and mitochondrial Na+–K+-ATPase and Ca2+-ATPase in liver tissue. Moreover, SFN could still increase the expression of NQO1, Nrf2, and HO-1 in liver tissue and decrease the oncosis and apoptosis of liver cells.
Conclusions
Pre-treatment with SFN could attenuate HIRI via the activation of Nrf2/ARE signaling pathways, ameliorate oxidative stress, and maintain the normal activities of Na+–K+-ATPase and Ca2+-ATPase, thus reducing the occurrence of cell oncosis and apoptosis. Therefore, SFN can be considered a potential candidate as an anti-ischemic medication to minimize HIRI.





Similar content being viewed by others
References
Serracino-Inglott F, Habib NA, Mathie RT. Hepatic ischemia–reperfusion injury. Am J Surg 2001;181(2):160–166
Galaris D, Barbouti A, Korantzopoulos P. Oxidative stress in hepatic ischemia–reperfusion injury: the role of antioxidants and iron chelating compounds. Curr Pharm Des 2006;12(23):2875–2890
Jaeschke H. Reactive oxygen and mechanisms of inflammatory liver injury: present concepts. J Gastroenterol Hepatol 2011;26(Suppl 1):173–179
Jaeschke H, Woolbright BL. Current strategies to minimize hepatic ischemia–reperfusion injury by targeting reactive oxygen species. Transplant Rev (Orlando) 2012;26(2):103–114
van Golen RF, van Gulik TM, Heger M. Mechanistic overview of reactive species-induced degradation of the endothelial glycocalyx during hepatic ischemia/reperfusion injury. Free Radic Biol Med 2012;52(8):1382–1402
Bir SC, Kolluru GK, Fang K, Kevil CG. Redox balance dynamically regulates vascular growth and remodeling. Semin Cell Dev Biol 2012;23(7):745–757
Ohnuma T, Nakayama S, Anan E, Nishiyama T, Ogura K, Hiratsuka A. Activation of the Nrf2/ARE pathway via S-alkylation of cysteine 151 in the chemopreventive agent-sensor Keap1 protein by falcarindiol, a conjugated diacetylene compound. Toxicol Appl Pharmacol 2010;244(1):27–36
Yan D, Dong J, Sulik KK, Chen SY. Induction of the Nrf2-driven antioxidant response by tert-butylhydroquinone prevents ethanol-induced apoptosis in cranial neural crest cells. Biochem Pharmacol 2010;80(1):144–149
Yoon HY, Kang NI, Lee HK, Jang KY, Park JW, Park BH. Sulforaphane protects kidneys against ischemia–reperfusion injury through induction of the Nrf2-dependent phase 2 enzyme. Biochem Pharmacol 2008;75(11):2214–2223
Wang B, Zhu X, Kim Y, Li J, Huang S, Saleem S, et al. Histone deacetylase inhibition activates transcription factor Nrf2 and protects against cerebral ischemic damage. Free Radic Biol Med 2012;52(5):928–936
Kuo PC, Drachenberg CI, de la Torre A, Bartlett ST, Lim JW, Plotkin JS, et al. Apoptosis and hepatic allograft reperfusion injury. Clin Transplant 1998;12(3):219–223
Leppo J. Imaging cell injury and death. Curr Cardiol Rep 2003;5(1):40–44
Guicciardi ME, Malhi H, Mott JL, Gores GJ. Apoptosis and necrosis in the liver. Compr Physiol 2013;3(2):977–1010
Lin S, Liu K, Wu W, Chen C, Wang Z, Zhang X. Study on pre-treatment of FPS-1 in rats with hepatic ischemia–reperfusion injury. Am J Chin Med 2009;37(2):323–337
Guerrero-Beltrán CE, Calderón-Oliver M, Pedraza-Chaverri J, Chirino YI. Protective effect of sulforaphane against oxidative stress: recent advances. Exp Toxicol Pathol 2012;64(5):503–508
Zhao HD, Zhang F, Shen G, Li YB, Li YH, **g HR, et al. Sulforaphane protects liver injury induced by intestinal ischemia reperfusion through Nrf2–ARE pathway. World J Gastroenterol 2010;16(24):3002–3010
Cekauskas A, Bruns H, Manikas M, Herr I, Gross ML, Zorn M, et al. Sulforaphane decreases kidney injury after transplantation in rats: role of mitochondrial damage. Ann Transplant 2013;18:488–496
Li Z, Galli U, Becker LE, Bruns H, Nickkolgh A, Hoffmann K, et al. Sulforaphane protects hearts from early injury after experimental transplantation. Ann Transplant 2013;18:558–566
** Z, Liu W, Kang Z, Cai J, Wang Q, Cheng N, et al. Sulforaphane protects brains against hypoxic-ischemic injury through induction of Nrf2-dependent phase 2 enzyme. Brain Res 2010;1343:178–185
Borski RJ, Hodson RG. Fish research and the institutional animal care and use committee. ILAR J 2003;44(4):286e94
Suzuki S, Toledo-Pereyra LH, Rodriguez FJ, Cejalvo D. Neutrophil infiltration as an important factor in liver ischemia and reperfusion injury. Modulating effects of FK506 and cyclosporine. Transplantation 1993;55(6):1265–1272
Fahey JW, Talalay P. Antioxidant functions of sulforaphane: a potent inducer of Phase II detoxication enzymes. Food Chem Toxicol 1999;37(9–10):973–979
Hoffmann K, Büchler MW, Schemmer P. Supplementation of amino acids to prevent reperfusion injury after liver surgery and transplantation—where do we stand today? Clin Nutr 2011;30(2):143–147
Glantzounis GK, Salacinski HJ, Yang W, Davidson BR, Seifalian AM. The contemporary role of antioxidant therapy in attenuating liver ischemia–reperfusion injury: a review. Liver Transpl 2005;11(9):1031–1047
Zhai Y, Petrowsky H, Hong JC, Busuttil RW, Kupiec-Weglinski JW. Ischaemia-reperfusion injury in liver transplantation—from bench to bedside. Nat Rev Gastroenterol Hepatol 2013;10(2):79–89
Magesh S, Chen Y, Hu L. Small molecule modulators of Keap1–Nrf2–ARE pathway as potential preventive and therapeutic agents. Med Res Rev 2012;32(4):687–726
Stowe DF, Camara AK. Mitochondrial reactive oxygen species production in excitable cells: modulators of mitochondrial and cell function. Antioxid Redox Signal 2009;11(6):1373–1414
Yorozuya T, Adachi N, Dote K, Nakanishi K, Takasaki Y, Arai T. Enhancement of Na+, K(+)-ATPase and Ca(2+)-ATPase activities in multi-cycle ischemic preconditioning in rabbit hearts. Eur J Cardiothorac Surg 2004;26(5):981–987
Yue R, Hu H, Yiu KH, Luo T, Zhou Z, Xu L, et al. Lycopene protects against hypoxia/reoxygenation-induced apoptosis by preventing mitochondrial dysfunction in primary neonatal mouse cardiomyocytes. PLoS ONE 2012;7(11):e50778
Beal MF. Aging, energy, and oxidative stress in neurodegenerative diseases. Ann Neurol 1995;38(3):357–366
Acknowledgements
The study was supported by the Science and Technology Project Foundation of Guangdong Province, China (No. 2011B031800361).
Compliance with ethical requirements and Conflict of interest
Animal care and surgical procedures were approved by the Institutional Review Board of Sun Yat-sen University under the guidelines of the Chinese Academy of Sciences and carried out in accordance with the provisions of the NIH Guide for the Care and Use of Laboratory Animals. **n** Chi, Rui Zhang, Ning Shen, Yi **, Ayep Alina, Simin Yang and Shiqing Lin declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
**n** Chi and Rui Zhang contributed equally to this study.
Rights and permissions
About this article
Cite this article
Chi, X., Zhang, R., Shen, N. et al. Sulforaphane reduces apoptosis and oncosis along with protecting liver injury-induced ischemic reperfusion by activating the Nrf2/ARE pathway. Hepatol Int 9, 321–329 (2015). https://doi.org/10.1007/s12072-014-9604-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-014-9604-y