Abstract
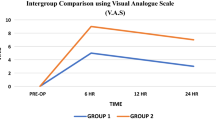
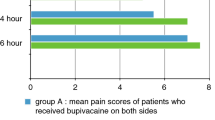
Tonsillectomy is one of the most common surgical procedures practiced in Otorhinolaryngology. A significant obstacle for the speedy and smooth recovery is early post- operative pain. Pain leads to negative outcomes such as poor intake, tachycardia, anxiety, delayed wound healing and insomnia. Aim to assess and compare the effect of post-incisional infiltration of 0.75% Ropivacaine v/s 0.5% Bupivacaine on post tonsillectomy pain, the on start of oral intake and stay in hospital and to investigate any complications that can arise due to infiltration of the said drugs. 60 Patients above the age of 5 years were posted for tonsillectomy or adenotonsillectomy under general anesthesia. Patients were blinded about the group in which they will be enrolled. Group A received Inj. ropivacaine (0.75%) 2 ml and Group B: received Inj. Bupivacaine (0.50%) 2 ml in each fossa. After surgery, no analgesics were given & patients were observed for the intensity of post-operative pain in the immediate post-operative period, at 2, 4, 6, 12, 24, 48 h and further if not discharged using VISUAL ANALOGUE SCORE (VAS) and VERBAL RATING SCALE(VRS). Post-operative pain assessment was done using VAS and VRS at 2nd, 4th, 6th, 12th, 24th and 48th hour which was found to be lower in Group ‘A’. Patients in Group ‘A’ also started their oral intake sooner, had lesser hospitalization days than group ‘B’ patients. Longer time for Rescue analgesic and reduced total dose of analgesic required was seen in Group A compared to Group B. This comparative study on Post-incisional infiltration of 2 ml 0.75% Ropivacaine v/s 2 ml 0.5% Bupivacaine has shown that Ropivacaine is a more effective drug in reducing post-operative pain in comparison to Bupivacaine, proven statistically.







Similar content being viewed by others
References
Mehta DM (2019) A Randomised double blind clinical trial to compare the effects of preincisional infiltration of ropivacaine v/s bupivacaine on post tonsillectomy pain relief. J Med Sci Clin Res [Internet]. 7(5). https://www.researchgate.net/publication/333223115_A_Randomised_double_blind_clinical_trial_to_compare_the_effects_of_preincisional_infiltration_of_ropivacaine_vs_bupivacaine_on_post_tonsillectomy_pain_relief
Robinson SR, Purdie GL (2000) Reducing post-tonsillectomy pain with cryoanalgesia: a randomized controlled trial. Laryngoscope 110(7):1128–1131
Taylor A, McLeod G (2020) Corrigendum to ‘Basic pharmacology of local anaesthetics’[BJA Education 20 (2020) 34–41]. BJA Ed 20(4):140
Giannoni C, White S, Enneking FK, Morey T (2001) Ropivacaine with or without clonidine improves pediatric tonsillectomy pain. Archiv Otolaryngol-Head Neck Surg 127(10):1265–1270
Katz J, Kavanagh BP, Sandler AN, Nierenberg H, Boylan JF, Friedlander M, Shaw BF (1992) Preemptive analgesia. Clinical evidence of neuroplasticity contributing to postoperative pain. https://pubmed.ncbi.nlm.nih.gov/1519781/
JF B, GR S. (1990) Molecular mechanisms of local anesthesia: a review. Anesthesiology [Internet]. 72(4):711–34. https://pubmed.ncbi.nlm.nih.gov/2157353/
Jx M, Bj D (2004) Pharmacokinetics of local anaesthetics in infants and children. Clin Pharmacokinet [Internet]. 43(1):17–32. https://pubmed.ncbi.nlm.nih.gov/14715049/
Akoglu E, Akkurt BCO, Inanoglu K, Okuyucu S, Daglı S (2006) Ropivacaine compared to bupivacaine for post-tonsillectomy pain relief in children: a randomized controlled study. Int J Pediatric Otorhinolaryngol 70(7):1169–1173
Unal Y, Pampal K, Korkmaz S, Arslan M, Zengin A, Kurtipek O (2007) Comparison of bupivacaine and ropivacaine on postoperative pain after tonsillectomy in paediatric patients. Int J Pediatric Otorhinolaryngol 71(1):83–87
Tajima K, Sato S, Miyabe M (1997) A case of acute pulmonary edema and bulbar paralysis after local epinephrine infiltration. J Clin Anesth 9(3):236–238
Park AH, Pappas AL, Fluder E, Creech S, Lugo RA, Hotaling A (2004) Effect of perioperative administration of ropivacaine with epinephrine on postoperative pediatric adenotonsillectomy recovery. Archiv Otolaryngol-Head Neck Surg 130(4):459–464
Arikan OK, Ozcan S, Kazkayasi M, Akpinar S, Koc C (2006) Preincisional infiltration of tonsils with ropivacaine in post-tonsillectomy pain relief: double-blind, randomized, placebo-controlled intraindividual study. J Otolaryngol 35(3):167–172
Arikan OK, Sahin S, Kazkayasi M, Muluk NB, Akpinar S, Kilic R (2008) High-dose ropivacaine versus bupivacaine for posttonsillectomy pain relief in adults. J Otolaryngol Head Neck Surg 37(6):836–843
Kasapoglu F, Kaya FN, Tuzemen G, Ozmen OA, Kaya A, Onart S (2011) Comparison of peritonsillar levobupivacaine and bupivacaine infiltration for post-tonsillectomy pain relief in children: placebo-controlled clinical study. Int J Pediatric Otorhinolaryngol 75(3):322–326
Grubb T, Lobprise H (2020) Local and regional anaesthesia in dogs and cats: Overview of concepts and drugs (Part 1). Veterinary Med Sci 6(2):209–217
Özkiriş M, Kapusuz Z, Saydam L (2012) Comparison of ropivacaine, bupivacaine and lidocaine in the management of post-tonsillectomy pain. Int J Pediatric Otorhinolaryngol 76(12):1831–1834
Baugh RF, Archer SM, Mitchell RB, Rosenfeld RM, Amin R, Burns JJ, Patel MM (2011) Clinical practice guideline: tonsillectomy in children. Otolaryngol Head Neck Surg 144:S1–S30
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethics Approval
Institutional Ethical Committee Approval taken before the study.
Informed Consent
Informed Written Consent about the study taken before every surgery in the patient’s own vernacular language.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nitin, B., Gupta, M. To Compare the Effects of Post-tonsillectomy Intra-operative Infiltration of Ropivacaine Versus Bupivacaine in Tonsillar Fossa. Indian J Otolaryngol Head Neck Surg 76, 1805–1818 (2024). https://doi.org/10.1007/s12070-023-04417-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-023-04417-6