Abstract
Objectives
To estimate the interval mammogram rate, i.e. the undertaking of an additional mammography between scheduled screening rounds, and identify factors influencing this phenomenon.
Methods
Data from our screening programme for the year 2014, excluding prevalent rounds, were analysed. Information about the number of women who underwent interval mammograms was obtained reviewing the questionnaires and searching the department database. Data on age, breast density, family history of breast cancer, number of screening rounds, previous recalls, general practitioner, and city of residence (used as a proxy of local socio-economic differences) were evaluated using chi-square test.
Results
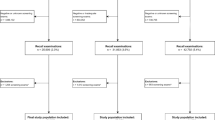
Of 2780 screened women (incident rounds), 2566 had complete data (92%). The interval mammogram rate was 384/2566 (15%, 95% confidence interval 14–17%). Women classified with American College of Radiology c or d breast density categories showed a higher interval mammography probability than those with a and b density (p < 0.001); women in their second round showed a higher probability of interval mammogram compared to women in their fifth, sixth, or seventh round (p ≤ 0.004). No significant differences were found between women with and without an interval mammogram when considering previous recalls for a negative work-up (p = 0.241), positive breast cancer family history (p = 0.538), and city of residence (p = 0.177).
Conclusions
The interval mammogram rate was relatively low (15%). Higher breast density and first of years of adherence to the programme were associated with higher interval mammogram rate.

Similar content being viewed by others
References
Hackshaw A (2003) EUSOMA review of mammography screening. Ann Oncol Off J Eur Soc Med Oncol 14:1193–1195
Ouédraogo S, Dabakuyo-Yonli TS, Amiel P et al (2014) Breast cancer screening programmes: challenging the coexistence with opportunistic mammography. Patient Educ Couns 97:410–417. https://doi.org/10.1016/j.pec.2014.08.016
Chamot E, Charvet A, Perneger TV (2009) Overuse of mammography during the first round of an organized breast cancer screening programme. J Eval Clin Pract 15:620–625. https://doi.org/10.1111/j.1365-2753.2008.01062.x
Bihrmann K, Jensen A, Olsen AH et al (2008) Performance of systematic and non-systematic (‘opportunistic’) screening mammography: a comparative study from Denmark. J Med Screen 15:23–26. https://doi.org/10.1258/jms.2008.007055
de Gelder R, Bulliard JL, de Wolf C et al (2009) Cost-effectiveness of opportunistic versus organised mammography screening in Switzerland. Eur J Cancer 45:127–138. https://doi.org/10.1016/j.ejca.2008.09.015
Carrozzi G, Sampaolo L, Bolognesi L et al (2015) Cancer screening uptake: association with individual characteristics, geographic distribution, and time trends in Italy. Epidemiol Prev 39:9–18
Perry N, Broeders M, de Wolf C et al (2008) European guidelines for quality assurance in breast cancer screening and diagnosis. Fourth edition—Summary document. Ann Oncol 19:614–622
Ciatto S, Ambrogetti D, Bonardi R et al (2005) Second reading of screening mammograms increases cancer detection and recall rates. Results in the Florence screening programme. J Med Screen 12:103–106. https://doi.org/10.1258/0969141053908285
D’Orsi CJ, Sickles EA, Mendelson EB, Morris EA et al (2013) ACR BI-RADS® Atlas. Breast imaging reporting and data system. Reston, VA, American College of Radiology
Bulliard JL, Ducros C, Jemelin C et al (2009) Effectiveness of organised versus opportunistic mammography screening. Ann Oncol 20:1199–1202. https://doi.org/10.1093/annonc/mdn770
Dinnes J, Moss S, Melia J et al (2001) Effectiveness and cost-effectiveness of double reading of mammograms in breast cancer screening: findings of a systematic review. Breast 10:455–463
Posso M, Puig T, Carles M et al (2017) Effectiveness and cost-effectiveness of double reading in digital mammography screening: a systematic review and meta-analysis. Eur J Radiol 96:40–49. https://doi.org/10.1016/j.ejrad.2017.09.013
Vanier A, Leux C, Allioux C et al (2013) Are prognostic factors more favorable for breast cancer detected by organized screening than by opportunistic screening or clinical diagnosis? A study in Loire-Atlantique (France). Cancer Epidemiol 37:683–687. https://doi.org/10.1016/j.canep.2013.07.001
Ciatto S, Bernardi D, Pellegrini M et al (2012) Proportional incidence and radiological review of large (T2 +) breast cancers as surrogate indicators of screening programme performance. Eur Radiol 22:1250–1254. https://doi.org/10.1007/s00330-011-2355-4
Acknowledgements
We thank the precious work of Dr. Roberto Lucchini and of “Servizio di Medicina Preventiva ASL Milano 2”, for organised screening patients’ data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
FS declares to have no competing interests and to have received grants from or to be member of speakers’ bureau/advisory board for Bayer, Bracco, and General Electric. SS declares to have no competing interests and to be member of speakers’ bureau for General Electric. NB declares to have no competing interests and to have received financial support by the Swiss Cancer Research Foundation. All other authors declare that they have no competing interests.
Ethical standards
Local ethics committee approved this retrospective study. The study is in accordance with the Helsinki Declaration of 1975, revised in 2000.
Informed consent
Informed consent was waived by local ethics committee due to the retrospective nature of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Carbonaro, L.A., Rizzo, S.S., Schiaffino, S. et al. Biennial screening mammography: How many women ask for more? Estimate of the interval mammogram rate in an organised population-based screening programme. Radiol med 126, 200–205 (2021). https://doi.org/10.1007/s11547-020-01238-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-020-01238-3