Abstract
Purpose
To assess the prevalence, awareness, and quality of life (QOL) impact of symptoms suggestive of underactive bladder (UAB) in the USA.
Methods
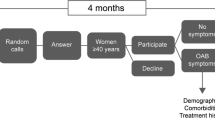
A thirteen-item paper survey was mailed to 25,000 individuals 60 years or older living in the USA. It aimed to collect information relating to demographics, familiarity with UAB, patient urinary symptoms, and QOL concerns.
Results
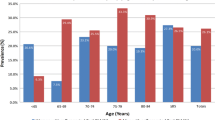
Nine hundred and seventy-seven survey participants were stratified into four groups based on the number of UAB symptoms (straining, retention, and difficulty emptying) present: zero, one, two, and three. As the number of reported UAB symptoms increased, there was an increase prevalence in nocturia, urge, and urinary frequency (p < 0.0001). Increased UAB symptoms were associated with an increased prevalence of concerns related to urgency, urge incontinence, nocturia, and overall urinary status (p < 0.0001). Urology visits were most common in individuals who reported the most UAB symptoms (p < 0.0001); however, there was no difference among groups with regard to UAB awareness. Women were less likely to report any UAB symptoms (p < 0.0001), symptoms of urge (p = 0.001), retention (p = 0.002), difficulty emptying their bladder (p < 0.0001), a history of catheter use for retention (P = 0.002), and urology visits in the past 3 years (p < 0.0001). This study is limited in its inability to differentiate UAB from disorders that may mimic UAB clinically, based on the survey questions asked.
Conclusions
Underactive bladder symptoms are common and can have a significant impact on ones QOL, although awareness is still lacking among potentially affected individuals. More must be done to allow one to better differentiate between UAB and conditions that are clinically similar.



Similar content being viewed by others
Abbreviations
- BOO:
-
Bladder outlet obstruction
- DU:
-
Detrusor underactivity
- ICS:
-
International Continence Society
- LUTS:
-
Lower urinary tract symptoms
- UAB:
-
Underactive bladder
- UAB-q:
-
Underactive bladder questionnaire
- UTI:
-
Urinary tract infection
- QOL:
-
Quality of life
- OAB:
-
Overactive bladder
- PFS:
-
Pressure flow studies
- BPH:
-
Benign prostatic hyperplasia
- UI:
-
Urge incontinence
References
Miyazato M, Yoshimura N, Chancellor MB (2013) The other bladder syndrome: underactive bladder. Rev Urol 15(1):11–22. doi:10.3909/riu0558
Van Koeveringe GA, Vahabi B, Andersson KE et al (2011) Detrusor underactivity: a plea for new approaches to a common bladder dysfunction. Neurourol Urodyn 30:723–728. doi:10.1002/nau.21097
Chapple CR, Osman NI, Birder L et al (2015) The underactive baldder: a new clinical concept? Eur Urol 68(3):351–353. doi:10.1016/j.eururo.2015.02.030
Valente S, DuBeau C, Chancellor D et al (2014) Epidemiology and demographics of the underactive bladder: a cross-sectional survey. Int Urol Nephrol 46(1):S7–S10. doi:10.1007/s11255-014-0811-1
Jeuong SJ, Kim JH, Lee JY et al (2012) Prevalence and clinical features of detrusor underactivity among elderly with lower urinary tract symptoms: a comparison between men and women. Korean J Urol 53(5):342–348. doi:10.4111/kju.2012.53.5.342
Hoag N, Gani J (2015) Underactive bladder: clinical features, urodynamic parameters and treatment. Int Neurourol J 19:185–189. doi:10.5213/inj.2015.19.3.185
Chuang YC, Plata M, Lamb LE, Chancellor MB (2015) Underactive bladder in older adults. Clin Geriatr Med 31(4):523–533. doi:10.1016/j.cger.2015.06.002
Dubeau CE (2006) The aging lower urinary tract. J Urol 175(3):S11–S15. doi:10.1016/S0022-5347(05)00311-3
Ortman JM, Velkoff VA, Hogan H (2016) An aging nation: the older population in the United States. United States Census Bureau Website. http://www.census.gov/library/publications/2014/demo/p25-1140.html. Accessed 14 May 2016
Coyne KS, Wein A, Nicholson S et al (2014) Economic burden of urgency urinary incontinence in the United States: a systematic review. J Manag Care Pharm 20(2):130–140. doi:10.18553/jmcp.2014.20.2.130
Foxman B, Barlow R, D’Arcy H et al (2000) Urinary tract infection: self-reported incidence and associated costs. Ann Epidemiol 10(8):509–515. doi:10.1016/S1047-2797(00)00072-7
Abarbanel J, Marcus EL (2007) Impaired detrusor contractility in community-dwelling elderly presenting with lower urinary tract symptoms. Urology 69(3):436–440. doi:10.1016/j.urology.2006.11.019
Kadow BT, Tyagi P, Chermansky CJ (2015) Neurogenic causes of detrusor underactivity. Curr Bladder Dysfunct Rep 10(4):325–331. doi:10.1007/s11884-015-0331-6
Gammie A, Kaper M, Dorrepaal C et al (2016) Signs and symptoms of detrusor underactivity: an analysis of clinical presentation and urodynamic tests from a large group of patients undergoing pressure flow studies. Eur Urol 69(2):361–369. doi:10.1016/j.eururo.2015.08.014
Liuz Z, Uchiyama T, Sakakibara R et al (2015) Underactive and overactive bladders are related to motor function and quality of life in Parkinson’s disease. Int Urol Nephrol 47(5):751–757. doi:10.1007/s11255-015-0951-y
Griebling TL, DuBeau CE, Kuchel G et al (2014) Defining and advancing education and conservative therapies of underactive bladder. Int Urol Nephrol 46:S29–S34. doi:10.1007/s11255-014-0799-6
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
This project was supported by the Aikens Center for Neurourology Research at Beaumont Health.
Research involving human participants
This study was IRB approved at Beaumont Health System.
Rights and permissions
About this article
Cite this article
Faraj, K., Doo, F., Boura, J. et al. A cross-sectional study in the USA of the epidemiology and quality of life of underactive bladder symptoms. Int Urol Nephrol 48, 1797–1802 (2016). https://doi.org/10.1007/s11255-016-1382-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-016-1382-0