Abstract
Purpose
The aim of this study was to estimate preferences related to quality of life attributes in people with multiple sclerosis, by kee** heterogeneity of patient preference in mind, using the latent class approach.
Methods
A discrete choice experiment survey was developed using the following attributes: activities of daily living, instrumental activities of daily living, pain/fatigue, anxiety/depression and attention/concentration. Choice sets were presented as pairs of hypothetical health status, based upon a fractional factorial design.
Results
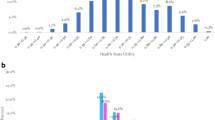
The latent class logit model estimated on 152 patients identified three subpopulations, which, respectively, attached more importance to: (1) the physical dimension; (2) pain/fatigue and anxiety/depression; and (3) instrumental activities of daily living impairments, anxiety/depression and attention/concentration. A posterior analysis suggests that the latent class membership may be related to an individual’s age to some extent, or to diagnosis and treatment, while apart from energy dimension, no significant difference exists between latent groups, with regard to Multiple Sclerosis Quality of Life-54 scales.
Conclusions
A quality of life preference-based utility measure for people with multiple sclerosis was developed. These utility values allow identification of a hierarchic priority among different aspects of quality of life and may allow physicians to develop a care programme tailored to patient needs.

Similar content being viewed by others
References
Revicki, D. A., Osoba, D., Fairclough, D., Barofsky, I., Berzon, R., Leidy, N. K., et al. (2000). Recommendations on health-related quality of life research to support labeling and promotional claims in the United States. Quality of Life Research, 9(8), 887–900.
Trask, P. C., Hsu, M. A., & McQuellon, R. (2009). Other paradigms: Health-related quality of life as a measure in cancer treatment: its importance and relevance. Cancer Journal, 15(5), 435–440.
Miller, D. K. R. (2008). Health-related quality of life assessment in multiple sclerosis. Reviews in Neurological Diseases, 5(2), 56–64.
Montazeri, A. (2009). Quality of life data as prognostic indicators of survival in cancer patients: An overview of the literature from 1982 to 2008. Health and Quality of Life Outcomes, 7, 102.
Miller, D. M., & Allen, R. (2010). Quality of life in multiple sclerosis: Determinants, measurement, and use in clinical practice. Current Neurology and Neuroscience Reports, 10(5), 397–406.
Opara, J. A., Jaracz, K., & Brola, W. (2010). Quality of life in multiple sclerosis. Journal of Medicine and Life, 3(4), 352–358.
Camfield, L., & Skevington, S. M. (2008). On subjective well-being and quality of life. Journal of Health Psychology, 13(6), 764–775.
Guyatt, G. H., Feeny, D. H., & Patrick, D. L. (1993). Measuring health-related quality of life. Annals of Internal Medicine, 118(8), 622–629.
Mayo, N. E., Hum, S., & Kuspinar, A. (2012). Methods and measures: What’s new for MS? Mult Scler (Houndmills, Basingstoke, England), 19(6), 709–713.
Hensher, D. A., Rose, J. M., & Greene, W. H. (2005). Applied choice analysis: A primer. Cambridge: Cambridge University Press.
Ryan, M., Major, K., & Skatun, D. (2005). Using discrete choice experiments to go beyond clinical outcomes when evaluating clinical practice. Journal of Evaluation in Clinical Practice, 11(4), 328–338.
Ryan, M. (2004). Discrete choice experiments in health care. BMJ, 328(7436), 360–361.
Sung, L., Alibhai, S. M., Ethier, M. C., Teuffel, O., Cheng, S., Fisman, D., et al. (2012). Discrete choice experiment produced estimates of acceptable risks of therapeutic options in cancer patients with febrile neutropenia. Journal of Clinical Epidemiology, 65, 627–634.
Flynn, T. N., Louviere, J. J., Peters, T. J., & Coast, J. (2010). Using discrete choice experiments to understand preferences for quality of life. Variance-scale heterogeneity matters. Social Science and Medicine, 70(12), 1957–1965.
Ryan, M., Bate, A., Eastmond, C. J., & Ludbrook, A. (2001). Use of discrete choice experiments to elicit preferences. Quality Health Care, 10(Suppl 1), i55–i60.
Ryan, M., & Gerard, K. (2003). Using discrete choice experiments to value health care programmes: Current practice and future research reflections. Applied Health Economics and Health Policy, 2(1), 55–64.
Ryan, M., Netten, A., Skatun, D., & Smith, P. (2006). Using discrete choice experiments to estimate a preference-based measure of outcome—An application to social care for older people. Journal of Health Economics, 25(5), 927–944.
The EuroQoL Group. (1990). EuroQoL-a new facility for the measurement of health-related quality of life. Health Policy, 16, 199–208.
Rand-Hendriksen, K., Augestad, L. A., Kristiansen, I. S., & Stavem, K. (2012). Comparison of hypothetical and experienced EQ-5D valuations: Relative weights of the five dimensions. Quality of Life Research, 21(6), 1005–1012.
Kuspinar, A., & Mayo, N. E. (2013). Do generic utility measures capture what is important to the quality of life of people with multiple sclerosis? Health and Quality of Life Outcomes, 11, 71.
Miller, A., & Dishon, S. (2006). Health-related quality of life in multiple sclerosis: The impact of disability, gender and employment status. Quality of Life Research, 15(2), 259–271.
Buchanan, R. J., Johnson, O., Zuniga, M. A., Carrillo-Zuniga, G., & Chakravorty, B. J. (2012). Health-related quality of life among Latinos with multiple sclerosis. Journal of Social Work in Disability & Rehabilitation, 11(4), 240–257.
Bridges, J. F., Hauber, A. B., Marshall, D., Lloyd, A., Prosser, L. A., Regier, D. A., et al. (2011). Conjoint analysis applications in health—a checklist: A report of the ISPOR good research practices for conjoint analysis task force. Value Health, 14(4), 403–413.
McFadden, D. (1974). The measurement of urban travel demand. Journal of Public Economics, 3, 303–328.
Train, K. E. (2009). Discrete choice methods with simulation. Cambridge University Press.
Hole, A. R. (2008). Modelling heterogeneity in patients’ preferences for the attributes of a general practitioner appointment. Journal of Health Economics, 27(4), 1078–1094.
Shingler, S. L., Swinburn, P., Ali, S., Perard, R., & Lloyd, A. J. (2013). A discrete choice experiment to determine patient preferences for injection devices in multiple sclerosis. Journal of Health Economics, 16(8), 1036–1042.
Vickrey, B. G., Hays, R. D., Harooni, R., Myers, L. W., & Ellison, G. W. (1995). A health-related quality of life measure for multiple sclerosis. Quality of Life Research, 4(3), 187–206.
Kurtzke, J. F. (1983). Rating neurologic impairment in multiple sclerosis: An expanded disability status scale (EDSS). Neurology, 33(11), 1444–1452.
Benedict, R. H., Wahlig, E., Bakshi, R., Fishman, I., Munschauer, F., Zivadinov, R., et al. (2005). Predicting quality of life in multiple sclerosis: Accounting for physical disability, fatigue, cognition, mood disorder, personality, and behavior change. Journal of the Neurological Sciences, 231(1–2), 29–34.
Tarrants, M., Oleen-Burkey, M., Castelli-Haley, J., & Lage, M. J. (2011). The impact of comorbid depression on adherence to therapy for multiple sclerosis. Multiple Sclerosis International, 2011, 271321.
Amato, M. P., Ponziani, G., Rossi, F., Liedl, C. L., Stefanile, C., & Rossi, L. (2001). Quality of life in multiple sclerosis: The impact of depression, fatigue and disability. Multiple Sclerosis, 7(5), 340–344.
Feinstein, A. (2011). Multiple sclerosis and depression. Multiple Sclerosis, 17(11), 1276–1281.
Prakash, R. S., Snook, E. M., Lewis, J. M., Motl, R. W., & Kramer, A. F. (2008). Cognitive impairments in relapsing-remitting multiple sclerosis: A meta-analysis. Multiple Sclerosis, 14(9), 1250–1261.
Cella, D. F., Dineen, K., Arnason, B., et al. (1996). Validation of the functional assessment of multiple sclerosis (FAMS) quality of life instrument. Neurology, 47, 129–139.
Hobart, J. C., Lam**, D. L., Fitzpatrick, R., et al. (2001). The multiple sclerosis impact scale (MSIS-29): A new patient-based outcome measure. Brain, 124, 962–973.
Kuhfeld, W. F. (2005). Marketing research methods in SAS. Experimental design, choice, conjoint, and graphical techniques. Cary, NC: SAS-Institute TS-722.
Orme, B. (1998). Sample size issues for conjoint analysis studies. In S. Software (Ed.), Sawtooth software: Research paper series.
Daly, A. J., & Hess, S. (2010). October). In European transport conference, Glasgow: Simple approaches for random utility modelling with panel data.
Greene, W. H. (2007). NLOGIT version 4.0: Reference guide. Plainview, NY: Econometric Software.
Institute, S. A. S. (1990). The SAS system for windows. Cary, North Carolina: SAS Institute Inc.
Aspinall, P. A., Johnson, Z. K., Azuara-Blanco, A., Montarzino, A., Brice, R., & Vickers, A. (2008). Evaluation of quality of life and priorities of patients with glaucoma. Investigative Ophthalmology & Visual Science, 49(5), 1907–1915.
Osoba, D., Hsu, M. A., Copley-Merriman, C., Coombs, J., Johnson, F. R., Hauber, B., et al. (2006). Stated preferences of patients with cancer for health-related quality-of-life (HRQoL) domains during treatment. Quality of Life Research, 15(2), 273–283.
Kaplan, R. M., Feeny, D., & Revicki, D. A. (1993). Methods for assessing relative importance in preference based outcome measures. Quality of Life Research, 2(6), 467–475.
Tsevat, J. (2000). What do utilities measure? Medical Care, 38(Suppl 9), II160–164.
Jones, K. H., Ford, D. V., Jones, P. A., John, A., Middleton, R. M., Lockhart-Jones, H., et al. (2013). How people with multiple sclerosis rate their quality of life: An EQ-5D survey via the UK MS register. PLoS One, 8(6), e65640.
Zimbardo, P. G., & Boyd, J. N. (1999). Putting time in perspective: A valid, reliable individual-differences metric. Journal of Personality and Social Psychology, 77(6), 1271.
Boniwell, I., & Zimbardo, P. G. (2004). Balancing one’s time perspective in pursuit of optimal functioning. In P. A. Linley & S. Joseph (Eds.), Positive Psychology in Practice (pp. 165–178). Hoboken, NJ: Wiley.
Revicki, D. A., & Kaplan, R. M. (1993). Relationship between psychometric and utility-based approaches to the measurement of health-related quality of life. Quality of Life Research, 2(6), 477–487.
Brown, M. M., Brown, G. C., Sharma, S., & Shah, G. (1999). Utility values and diabetic retinopathy. American Journal of Ophthalmology, 128(3), 324–330.
Sayao, A. L., Bueno, A. M., Devonshire, V., & Tremlett, H. (2011). The psychosocial and cognitive impact of longstanding ‘benign’ multiple sclerosis. Multiple Sclerosis, 17(11), 1375–1383.
Ryan, M., & Skatun, D. (2004). Modelling non-demanders in choice experiments. Health Economics, 13(4), 397–402.
Acknowledgments
This study was supported by the Piedmont Region–Regional Health Authority and Fondazione Ricerca Biomedica Onlus.
Author information
Authors and Affiliations
Corresponding author
Appendix 1
Appendix 1
Latent class model (finite mixture logit model) in discrete choice experiments.
Following the random utility framework, the utility that individual n assign to alternative j can be written as U jn = V jn + ɛ jn , where \(V_{jn} = \sum_{K = 1}^{K} \beta_{k} x_{jkn}\) is the deterministic part of utility (in which K is the number of attributes used in the experiment, k = 1,2,…,K, x nk is an observed variable related to attribute k and β k is the attribute coefficient, homogeneous across the population), while ɛ jn is the stochastic part, also capturing the unobserved heterogeneity Given two alternatives i and j, an individual will choose alternative j if U jn > U in .
Let P nt (j|β) give the probability of respondent n choosing alternative j on an occasion (called here scenario) t, conditional on a vector of attributes coefficients (β), in a fixed logit model we have:
Preference variation among individuals that is unaccounted for in modelling can result in a biased estimate. Two types of approaches allow to take into account differences in preferences: the random coefficient and the latent class models.
In the random utility model (continuous mixture model), the vector β follows a random distribution with parameters Ω and the choice probabilities are given by:
where P nt (j|β) is the logit choice probability and f(β|Ω) is the density function for the vector of attributes coefficients β.
In a latent class model (finite mixture model), preference variation is accommodated by identifying C groups of respondents with different values for the vector of attributes coefficients (β c). In this model, f(β) is a discrete distribution and the choice probability is the weighted sum of the choice probabilities across the C classes, with the class allocation probability π nc has been used as weight:
This specification is useful if there are C segments in the population, each of which has its own choice preferences. The share of population in class c is π nc (\(\sum\nolimits_{c = 1}^{C} { \, \pi_{nc} = 1}\)), and it is estimated along with the βs for each segment.
Rights and permissions
About this article
Cite this article
Rosato, R., Testa, S., Oggero, A. et al. Quality of life and patient preferences: identification of subgroups of multiple sclerosis patients. Qual Life Res 24, 2173–2182 (2015). https://doi.org/10.1007/s11136-015-0952-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-015-0952-4