Abstract
Objective
To define risk factors for meningioma-related seizures and predictors of successful weaning of antiseizure medications following meningioma resection.
Methods
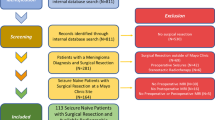
This is a retrospective study of 95 patients who underwent meningioma resection at a single institution. Primary outcome analyzed was ability to achieve seizure freedom without the use of anti-seizure medication at 6-months, 1-year, and last known follow up. Secondary outcome was postoperative seizure freedom.
Results
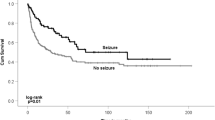
Preoperative seizures (OR: 11.63, 95% CI [3.64, 37.17], p < 0.0001), non-skull base tumor location (OR: 3.01, 95% CI [1.29, 7.02], p = 0.0128), and modified STAMPE score of 3–5 (OR: 5.42, 95% CI [2.18, 13.52], p = 0.0003) were associated with greater likelihood of remaining on antiseizure medication at 6-month follow up. Preoperative seizures (OR: 4.93, 95% CI: [2.00, 12.16 ], p = 0.0008), intratumoral calcifications (OR: 4.19, 95% CI: [1.61, 14.46], p = 0.0055), modified STAMPE score of 3–5 (OR: 5.42, CI [2.18, 13.52], p = 0.0003), and Ki67 greater than 7% (OR: 5.68, CI [1.61, 20.10], p = 0.0060) were significant risk factors for inability to discontinue ASMs by last follow up. Preoperative seizures (OR: 4.33, 95% CI [1.59, 11.85], p = 0.0050) and modified STAMPE score of 3–5 (OR: 6.09, 95% CI [2.16, 17.20], p = 0.0007) were significant risk factors for postoperative seizures.
Conclusions
Preoperative seizures, modified STAMPE2 score of 3–5, non-skull base tumor location, intratumoral calcifications, and Ki67 > 7% were significant risk factors for inability to achieve seizure freedom without ASMs. In addition, the modified STAMPE2 score successfully predicted increased seizure risk following meningioma resection for patients with a score of 3 or higher.
Similar content being viewed by others
References
Buerki RA, Horbinski CM, Kruser T, Horowitz PM, James CD, Lukas RV (2018) An overview of meningiomas. Future Oncol 14(21):2161–2177. https://doi.org/10.2217/fon-2018-0006
Tykocki T, Eltayeb M (2018) Ten-year survival in glioblastoma: A systematic review. J Clin Neurosci 54:7–13. https://doi.org/10.1016/j.jocn.2018.05.002
Englot DJ, Magill ST, Han SJ, Chang EF, Berger MS, McDermott MW (2016) Seizures in supratentorial meningioma: a systematic review and meta-analysis. J Neurosurg 124(6):1552–1561. https://doi.org/10.3171/2015.4.Jns142742
Klein M et al (2003) Epilepsy in low-grade gliomas: the impact on cognitive function and quality of life. Ann Neurol 54(4):514–20. https://doi.org/10.1002/ana.10712
Rahman Z et al (2015) Epilepsy in patients with primary brain tumors: the impact on mood, cognition, and HRQOL. Epilepsy Behav 48:88–95. https://doi.org/10.1016/j.yebeh.2015.03.016.
Harward SC, Rolston JD, Englot DJ (2020) Seizures in meningioma. Handb Clin Neurol 170:187–200. https://doi.org/10.1016/b978-0-12-822198-3.00053-7
Chen WC et al (2017) “Factors Associated With Pre- and Postoperative Seizures in 1033 Patients Undergoing Supratentorial Meningioma Resection,“ (in eng), Neurosurgery, vol. 81, no. 2, pp. 297–306, Aug 1 https://doi.org/10.1093/neuros/nyx001
Lu VM, Wahood W, Akinduro OO, Parney IF, Quinones-Hinojosa A, Chaichana KL (2019) Four Independent Predictors of Postoperative Seizures After Meningioma Surgery: A Meta-Analysis. World Neurosurg 130:537–545.e3. https://doi.org/10.1016/j.wneu.2019.06.063
Oya S et al (2021) Nation-wide brain tumor registry-based study of intracranial meningioma in Japan: analysis of surgery-related risks. Neurol Med Chir (Tokyo) 61(2):98–106. https://doi.org/10.2176/nmc.oa.2020-0304
Yang M et al (2020) Prophylactic AEDs treatment for patients with supratentorial meningioma does not reduce the rate of perioperative seizures: a retrospective single-Center cohort study. Front Oncol 10:568369. https://doi.org/10.3389/fonc.2020.568369
Brokinkel B et al (2021) Predicting postoperative seizure development in meningiomas - analyses of clinical, histological and radiological risk factors. Clin Neurol Neurosurg 200:106315. https://doi.org/10.1016/j.clineuro.2020.106315
Islim AI et al (Oct 2018) Postoperative seizures in meningioma patients: improving patient selection for antiepileptic drug therapy, (in eng). J Neurooncol 140(1):123–134. https://doi.org/10.1007/s11060-018-2941-2
Baumgarten P et al (2021) Early and late postoperative seizures in meningioma patients and prediction by a recent scoring system. Cancers (Basel) 13(3). https://doi.org/10.3390/cancers13030450
Wirsching HG et al (2016) Predicting outcome of epilepsy after meningioma resection. Neuro Oncol 18(7):1002–10. https://doi.org/10.1093/neuonc/nov303
Gupte TP et al (2020) Clinical and genomic factors associated with seizures in meningiomas. J Neurosurg 1–10. https://doi.org/10.3171/2020.7.Jns201042
Schneider M et al (2019) Preoperative tumor-associated epilepsy in patients with supratentorial meningioma: factors influencing seizure outcome after meningioma surgery. J Neurosurg 1–7. https://doi.org/10.3171/2019.7.Jns19455
Li X et al (2020) Risk factors and control of seizures in 778 Chinese patients undergoing initial resection of supratentorial meningiomas. Neurosurg Rev 43(2):597–608. https://doi.org/10.1007/s10143-019-01085-5
Zhang P et al (2020) Risk factors analysis and a nomogram model establishment for late postoperative seizures in patients with meningioma. J Clin Neurosci 80:310–317. https://doi.org/10.1016/j.jocn.2020.06.005
Skardelly M et al (2017) Risk Factors of Preoperative and Early Postoperative Seizures in Patients with Meningioma: A Retrospective Single-Center Cohort Study. World Neurosurg 97:538–546. https://doi.org/10.1016/j.wneu.2016.10.062
Weston J, Greenhalgh J, Marson AG (2015) Antiepileptic Drugs as prophylaxis for post-craniotomy seizures. Cochrane Database Syst Rev no 3. https://doi.org/10.1002/14651858.CD007286.pub3
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
E.E., J.T., and M.T. contributed to project development and design. E.E., J.H., S.R., participated in data collection. M.D. and E.E. conducted the data analysis. E.E. wrote the main manuscript text. M.D. and E.E. prepared Tables 1, 2, 3, 4 and 5. J.T. and S.M. provided editorial guidance and analytical support. All authors reviewed the manuscript and contributed suggestions for improvement.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Disclosures
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval
This study was approved by an institutional review board and conducted in line with the principles outlined by their ethical standards and criteria.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Previous presentations:
An abstract for this project was previously presented as an E-poster at the American Association of Neurological Surgeons annual meeting in Philadelphia, Pennsylvania, April 29 2022.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ellis, E.M., Drumm, M.R., Rai, S.M. et al. Long-term antiseizure medication use in patients after meningioma resection: identifying predictors for successful weaning and failures. J Neurooncol 165, 201–207 (2023). https://doi.org/10.1007/s11060-023-04481-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-023-04481-6