Abstract
Introduction
Evidence-based medicine guidelines are increasingly published and sanctioned by organized neurosurgery. However, implementation, interpretation, and use of clinical guidelines may vary substantially on a regional, national and international basis. Survey research can help bridge the gap by providing a snapshot of neurosurgeon attitudes, knowledge, and practices. The American Association of Neurological Surgeons/Congress of Neurological Surgeons (AANS/CNS) Section on Tumors formed a Survey Committee to formalize the process by which surveys are submitted and reviewed before distribution to our membership. The goal of this committee is to provide peer-review so that collected information will be scientifically robust and useful to the neurosurgical community.
Methods
Surveys submitted to the AANS/CNS tumor section between 2015 and 2019 were reviewed and metrics such as response rate and publication status assessed.
Results
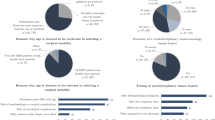
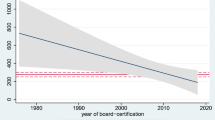
Six surveys were submitted to the Survey Committee of the AANS/CNS section on tumors between 2015 and 2019. Four have been circulated to section members, of which three have been published. Response rate has averaged 19% (range 16–23%), a majority of respondents (mean 70%) practice in academic settings.
Conclusions
The AANS/CNS Section on Tumors Survey Committee has and continues to help promote and improve the practice of surveying our community to answer important questions that can advance future training, research, and practice. There remains significant room for improvement in response rates, but ongoing tumor section efforts to increase member engagement will likely improve these numbers.
Similar content being viewed by others
References
Vachhrajani S, Kulkarni AV, Kestle JRW (2009) Clinical practice guidelines. J Neurosurg Pediatr 3:249–256. https://doi.org/10.3171/2008.12.PEDS08278
Ducis K, Florman JE, Rughani AI (2016) Appraisal of the quality of neurosurgery clinical practice guidelines. World Neurosurg 90:322–339. https://doi.org/10.1016/j.wneu.2016.02.044
Pannullo SC, Ramakrishna R (2016) Neurosurgical guidelines in a medicolegal minefield. World Neurosurg 96:602–603. https://doi.org/10.1016/j.wneu.2016.05.026
Kelley K, Clark B, Brown V, Sitzia J (2003) Good practice in the conduct and reporting of survey research. Int J Qual Health Care 15:261–266. https://doi.org/10.1093/intqhc/mzg031
Cunningham CT, Quan H, Hemmelgarn B et al (2015) Exploring physician specialist response rates to web-based surveys. BMC Med Res Methodol 15:32. https://doi.org/10.1186/s12874-015-0016-z
Braithwaite D, Emery J, De Lusignan S, Sutton S (2003) Using the Internet to conduct surveys of health professionals: a valid alternative? Fam Pract 20:545–551. https://doi.org/10.1093/fampra/cmg509
Burns KEA, Duffett M, Kho ME et al (2008) A guide for the design and conduct of self-administered surveys of clinicians. CMAJ 179:245–252. https://doi.org/10.1503/cmaj.080372
Ponto J (2015) Understanding and evaluating survey research. J Adv Pract Oncol 6:168–171
Dewan MC, Thompson RC, Kalkanis SN et al (2017) Prophylactic antiepileptic drug administration following brain tumor resection: results of a recent AANS/CNS section on tumors survey. J Neurosurg 126:1772–1778. https://doi.org/10.3171/2016.4.JNS16245
Wu AS, Trinh VT, Suki D et al (2013) A prospective randomized trial of peri-operative seizure prophylaxis in patients with intraparenchymal brain tumors. J Neurosurg 118:873–883. https://doi.org/10.3171/2012.12.JNS111970
Chen CC, Rennert RC, Olson JJ (2019) Congress of neurological surgeons systematic review and evidence-based guidelines on the role of prophylactic anticonvulsants in the treatment of adults with metastatic brain tumors. Neurosurgery 84:E195–E197. https://doi.org/10.1093/neuros/nyy545
Siomin V, Angelov L, Li L, Vogelbaum MA (2005) Results of a survey of neurosurgical practice patterns regarding the prophylactic use of anti-epilepsy drugs in patients with brain tumors. J Neurooncol 74:211–215. https://doi.org/10.1007/s11060-004-6912-4
Lunsford LD, Chiang V, Adler JR et al (2012) A recommendation for training in stereotactic radiosurgery for US neurosurgery residents. J Neurosurg 117(Suppl):2–4. https://doi.org/10.3171/2012.6.GKS12838
Yang I, Udawatta M, Prashant GN et al (2019) Commentary: stereotactic radiosurgery training for neurosurgery residents: results of a survey of residents, attendings, and program directors by the American Association of Neurological Surgeons/Congress of Neurological Surgeons Section on Tumors. Neurosurgery 84:E86–E91. https://doi.org/10.1093/neuros/nyy514
Lacroix M, Abi-Said D, Fourney DR et al (2001) A multivariate analysis of 416 patients with glioblastoma multiforme: prognosis, extent of resection, and survival. J Neurosurg 95:190–198. https://doi.org/10.3171/jns.2001.95.2.0190
Li YM, Suki D, Hess K, Sawaya R (2016) The influence of maximum safe resection of glioblastoma on survival in 1229 patients: can we do better than gross-total resection? J Neurosurg 124:977–988. https://doi.org/10.3171/2015.5.JNS142087
Sanai N, Polley M-Y, McDermott MW et al (2011) An extent of resection threshold for newly diagnosed glioblastomas. J Neurosurg 115:3–8. https://doi.org/10.3171/2011.2.JNS10998
Keles GE, Lundin DA, Lamborn KR et al (2004) Intraoperative subcortical stimulation map** for hemispherical perirolandic gliomas located within or adjacent to the descending motor pathways: evaluation of morbidity and assessment of functional outcome in 294 patients. J Neurosurg 100:369–375. https://doi.org/10.3171/jns.2004.100.3.0369
Oppenlander ME, Wolf AB, Snyder LA et al (2014) An extent of resection threshold for recurrent glioblastoma and its risk for neurological morbidity. J Neurosurg 120:846–853. https://doi.org/10.3171/2013.12.JNS13184
Stummer W, Reulen H-J, Meinel T et al (2008) Extent of resection and survival in glioblastoma multiforme: identification of and adjustment for bias. Neurosurgery 62:564–576. https://doi.org/10.1227/01.neu.0000317304.31579.17(Discussion 564–576)
Baron RB, Kessler RA, Hadjipanayis CG (2019) Initial biopsy and early re-resection practices in the treatment of glioblastoma among AANS/CNS tumor section surgeons. J Neurooncol 144:529–534. https://doi.org/10.1007/s11060-019-03253-5
Sanai N, Mirzadeh Z, Berger MS (2008) Functional outcome after language map** for glioma resection. N Engl J Med 358:18–27. https://doi.org/10.1056/NEJMoa067819
Kombos T, Suess O, Kern BC et al (1999) Comparison between monopolar and bipolar electrical stimulation of the motor cortex. Acta Neurochir 141:1295–1301
Solomon DA, Wood MD, Tihan T et al (2016) Diffuse midline gliomas with histone H3–K27M mutation: a series of 47 cases assessing the spectrum of morphologic variation and associated genetic alterations. Brain Pathol 26:569–580. https://doi.org/10.1111/bpa.12336
Lee J, Solomon DA, Tihan T (2017) The role of histone modifications and telomere alterations in the pathogenesis of diffuse gliomas in adults and children. J Neurooncol 132:1–11. https://doi.org/10.1007/s11060-016-2349-9
Gupta N, Goumnerova LC, Manley P et al (2018) Prospective feasibility and safety assessment of surgical biopsy for patients with newly diagnosed diffuse intrinsic pontine glioma. Neuro Oncol 20:1547–1555. https://doi.org/10.1093/neuonc/noy070
Catt S, Chalmers A, Fallowfield L (2008) Psychosocial and supportive-care needs in high-grade glioma. Lancet Oncol 9:884–891. https://doi.org/10.1016/S1470-2045(08)70230-4
Ford E, Catt S, Chalmers A, Fallowfield L (2012) Systematic review of supportive care needs in patients with primary malignant brain tumors. Neuro Oncol 14:392–404. https://doi.org/10.1093/neuonc/nor229
Pompili A, Telera S, Villani V, Pace A (2014) Home palliative care and end of life issues in glioblastoma multiforme: results and comments from a homogeneous cohort of patients. Neurosurg Focus 37:E5. https://doi.org/10.3171/2014.9.FOCUS14493
Flanigan TS (2008) Conducting survey research among physicians and other medical professionals: a review of current literature. Proc Surv Res Methods Sect 12:4136–4147
VanGeest JB, Johnson TP, Welch VL (2007) Methodologies for improving response rates in surveys of physicians: a systematic review. Eval Health Prof 30:303–321. https://doi.org/10.1177/0163278707307899
Stern MJ, Bilgen I, Dillman DA (2014) The state of survey methodology: challenges, dilemmas, and new frontiers in the era of the tailored design. Field Methods 26:284–301. https://doi.org/10.1177/1525822X13519561
Attenello FJ, Buchanan IA, Wen T et al (2018) Factors associated with burnout among US neurosurgery residents: a nationwide survey. J Neurosurg 129:1349–1363. https://doi.org/10.3171/2017.9.JNS17996
O’Neill BR, Velez DA, Braxton EE et al (2008) A survey of ventriculostomy and intracranial pressure monitor placement practices. Surg Neurol 70:268–273. https://doi.org/10.1016/j.surneu.2007.05.007
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Chetan Bettegowda is a consultant for Depuy-Synthes. Evan D. Bander, Jonathan H. Sherman, Manish K. Aghi, Jason Sheehan, and Rohan Ramakrishna have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bander, E.D., Sherman, J.H., Bettegowda, C. et al. Beyond guidelines: analysis of current practice patterns of AANS/CNS tumor neurosurgeons. J Neurooncol 151, 361–366 (2021). https://doi.org/10.1007/s11060-020-03389-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-020-03389-9