Abstract
Purpose
This study reports a case of unilateral retinopathy with extinguished full-field ERGs (ffERGs), wherein the visual acuity was 16/16 and the visual field was spared.
Methods
Observational case report.
Results
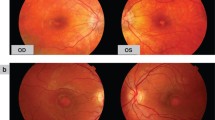
A 39-year-old female had developed nyctalopia in her left eye. Two years later, she visited an ophthalmologist who noted a bilaterally reduced pigmentation of the fundus. Her best-corrected visual acuity was 16/16 in both the eyes. Goldmann perimetry demonstrated that her visual field was bilaterally fully spared. ffERGs measurement was performed in accordance with the ISCEV standard protocol and indicated that her right eye was normal. However, all ERG responses were severely attenuated in her left eye. Multifocal ERG responses were found to be normal in the right eye and extinguished in the left eye except for residual responses that were exclusively located at the center. During the 7 years of the follow-up period, the visual field in the left eye, which was once normal, became shaded, and the development of a ring scotoma was identified. The visual field in the right eye is still full.
Conclusions
The pathogenesis of this patient’s condition still remains unknown, while unilateral retinitis pigmentosa, unilateral pigmentary retinopathy, acute zonal occult outer retinopathy, and autoimmune retinopathy can all be considered as possible explanations. The uniqueness of this case study is that the extinguished ERG responses are predictive of the functional alteration in the affected eye, when the initial visual acuity and the visual field were normal.



Similar content being viewed by others
References
Gauvin M, Chakor H, Koenekoop RK, Little JM, Lina JM, Lachapelle P (2016) Witnessing the first sign of retinitis pigmentosa onset in the allegedly normal eye of a case of unilateral RP: a 30-year follow-up. Doc Ophthalmol 132:213–229
Errera MH, Robson AG, Wong T, Hykin PG, Pal B, Sagoo MS, Pavesio CE, Moore AT, Webster AR, MacLaren RE, Holder GE (2019) Unilateral pigmentary retinopathy: a retrospective case series. Acta Ophthalmol 97:e601–e617
McCulloch DL, Marmor MF, Brigell MG, Hamilton R, Holder GE, Tzekov R, Bach M (2015) ISCEV Standard for full-field clinical electroretinography (2015 update). Doc Ophthalmol 130:1–12
Farrell DF (2009) Unilateral retinitis pigmentosa and cone-rod dystrophy. Clin Ophthalmol 3:263–270
Mukhopadhyay R, Holder GE, Moore AT, Webster AR (2011) Unilateral retinitis pigmentosa occurring in an individual with a germline mutation in the RP1 gene. Arch Ophthalmol 129:954–956
Marsiglia M, Duncker T, Peiretti E, Brodie SE, Tsang SH (2012) Unilateral retinitis pigmentosa: a proposal of genetic pathogenic mechanisms. Eur J Ophthalmol 22:654–660
Sim PY, Jeganathan VSE, Wright AF, Cackett P (2018) Unilateral retinitis pigmentosa occurring in an individual with a mutation in the CLRN1 gene. BMJ Case Rep pii: bcr-2017-222045. https://doi.org/10.1136/bcr-2017-222045
Bawankar P, Deka H, Barman M, Bhattacharjee H, Soibam R (2018) Unilateral retinitis pigmentosa: clinical and electrophysiological diagnosis. Can J Ophthalmol 53:e94–e97
Hood DC, Holopigian K, Greenstein V, Seiple W, Li J, Sutter EE, Carr RE (1999) Assessment of local retinal function in patients with retinitis pigmentosa using the multi-focal ERG technique. Vis Res 38:163–179
Gass JD (2003) Acute zonal occult outer retinopathy: Donders Lecture: The Netherlands Ophthalmological Society, Maastricht, Holland, June 19, 1992. Retina 23(6 Suppl):79–97
Francis PJ, Marinescu A, Fitzke FW, Bird AC, Holder GE (2005) Acute zonal occult outer retinopathy: towards a set of diagnostic criteria. Br J Ophthalmol 89:70–73
Machida S, Kizawa J, Fujiwara T, Murai K, Sugawara E, Imaizumi N (2007) Unilateral cone dysfunction as a manifestation of acute zonal occult outer retinopathy. Retin Cases Brief Rep 1:223–228. https://doi.org/10.1097/01.iae.0000221867.90293.65
Kure K, Obata R, Inoue Y, Iriyama A, Yanagi Y (2011) Acute progression of electrophysiologically affected fellow eye in unilaterally symptomatic acute zonal occult outer retinopathy. Clin Ophthalmol 5:1167–1170
Kido A, Ogino K, Miyake Y, Yanagida K, Kikuchi T, Yoshimura N (2016) Unilateral negative electroretinogram presenting as photophobia. Doc Ophthalmol 133:71–79
Ozawa K, Takahashi S, Mochizuki K, Miyake Y (2019) Two cases of unilateral cone-rod dysfunction with negative electroretinograms. Doc Ophthalmol 139(3):247–256
Robson AG, Richardson EC, Koh AH, Pavesio CE, Hykin PG, Calcagni A, Graham EM, Holder GE (2005) Unilateral electronegative ERG of non-vascular aetiology. Br J Ophthalmol 89:1620–1626
Roels D, Ueno S, Talianu CD, Draganova D, Kondo M, Leroy BP (2017) Unilateral cancer-associated retinopathy: diagnosis, serology and treatment. Doc Ophthalmol 135:233–240
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Statement of human rights
For this type of study, formal consent is not required.
Statement on the welfare of animals
This case report does not contain any studies with animals performed by any of the authors.
Informed consent
The patient has consented to the submission of this case report for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shimada, Y., Horiguchi, M. & Tanikawa, A. Unilaterally extinguished electroretinograms in an eye with normal visual acuity and visual field. Doc Ophthalmol 142, 127–132 (2021). https://doi.org/10.1007/s10633-020-09779-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10633-020-09779-8