Abstract
Purpose
The benefit of sodium-glucose cotransporter 2 inhibitors (SGLT2i) in patients with heart failure (HF) with reduced ejection fraction (HFrEF) and type 2 diabetes mellitus (T2DM) has been unequivocally proven in randomized, controlled trials. However, real-world evidence assessing the implementation of SGLT2i in clinical practice and their benefit in HF outside of highly selected study populations is limited.
Methods
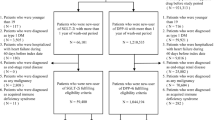
Patients with HF and T2DM admitted to the cardiology ward of the Medical University of Vienna between 01/2014 and 04/2020 were included in the present analysis. All first-time prescriptions of SGLT2i were identified. The outcome of interest was cardiovascular mortality. The median follow-up time was 2.3 years.
Results
Out of 812 patients with T2DM and HF (median age 70.4 [IQR 62.4–76.9] years; 70.3% males), 17.3% received an SGLT2i. The frequency of SGLT2i prescriptions significantly increased over the past 6 years (+ 36.6%, p < 0.001). In propensity score–adjusted pairwise analyses, SGLT2i treatment was inversely associated with long-term cardiovascular mortality in patients with HFrEF presenting with an adjusted HR of 0.33 (95%CI: 0.13–0.86; p = 0.024).
Conclusion
Despite large outcome trials showing a cardiovascular benefit, SGLT2i remain underutilized in clinical practice in patients with T2DM and HF. National and European Medical Agency remuneration regulations would allow more patients at high risk to receive these cardiovascular protective drugs. Most importantly, an SGLT2i therapy was associated with a survival benefit in patients with HFrEF.



Similar content being viewed by others
Data Availability
Data will be provided upon request.
References
Saeedi P, Petersohn I, Salpea P, Malanda B, Karuranga S, Unwin N, et al. Global and regional diabetes prevalence estimates for 2019 and projections for 2030 and 2045: results from the International Diabetes Federation Diabetes Atlas, 9(th) edition. Diabetes Res Clin Pract Ireland. 2019;157:107843.
de Matheus ASM, Tannus LRM, Cobas RA, Palma CCS, Negrato CA, de Gomes MB. Impact of diabetes on cardiovascular disease: an update. Int J Hypertens. 2013;2013:653789.
Shah AD, Langenberg C, Rapsomaniki E, Denaxas S, Pujades-Rodriguez M, Gale CP, et al. Type 2 diabetes and incidence of cardiovascular diseases: a cohort study in 1·9 million people. Lancet Diabetes Endocrinol Elsevier. 2015;3:105–13.
Zelniker TA, Wiviott SD, Raz I, Im K, Goodrich EL, Bonaca MP, et al. SGLT2 inhibitors for primary and secondary prevention of cardiovascular and renal outcomes in type 2 diabetes: a systematic review and meta-analysis of cardiovascular outcome trials. Lancet Lond Engl. 2019;393:31–9.
Marso SP, Daniels GH, Brown-Frandsen K, Kristensen P, Mann JFE, Nauck MA, et al. Liraglutide and cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2016;375:311–22.
Marso SP, Bain SC, Consoli A, Eliaschewitz FG, Jódar E, Leiter LA, et al. Semaglutide and cardiovascular outcomes in patients with type 2 diabetes. N Engl J Med Massachusetts Medical Society. 2016;375:1834–44.
Zinman B, Wanner C, Lachin JM, Fitchett D, Bluhmki E, Hantel S, et al. Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med. 2015;373:2117–28.
Wiviott SD, Raz I, Bonaca MP, Mosenzon O, Kato ET, Cahn A, et al. Dapagliflozin and cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2019;380:347–57.
Neal B, Perkovic V, Mahaffey KW, de Zeeuw D, Fulcher G, Erondu N, et al. Canagliflozin and cardiovascular and renal events in type 2 diabetes. N Engl J Med. 2017;377:644–57.
Perkovic V, Jardine MJ, Neal B, Bompoint S, Heerspink HJL, Charytan DM, et al. Canagliflozin and renal outcomes in type 2 diabetes and nephropathy. N Engl J Med. 2019;380:2295–306.
McMurray JJV, Solomon SD, Inzucchi SE, Køber L, Kosiborod MN, Martinez FA, et al. Dapagliflozin in patients with heart failure and reduced ejection fraction. N Engl J Med. 2019;381:1995–2008.
Packer M, Anker SD, Butler J, Filippatos G, Pocock SJ, Carson P, et al. Cardiovascular and renal outcomes with empagliflozin in heart failure. N Engl J Med United States. 2020;383:1413–24.
Chahine N, Al-Kindi S. Under-prescription of SGLT2 inhibitors in patients with diabetes and cardiovascular disease in the united states. J Am Coll Cardiol. 2020;75:1915.
Cosentino F, Grant PJ, Aboyans V, Bailey CJ, Ceriello A, Delgado V, et al. 2019 ESC Guidelines on diabetes, pre-diabetes, and cardiovascular diseases developed in collaboration with the EASD: the Task Force for diabetes, pre-diabetes, and cardiovascular diseases of the European Society of Cardiology (ESC) and the European Association for the Study of Diabetes (EASD). Eur Heart J. 2020;41:255–323.
Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JGF, Coats AJS, et al. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: the Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC)Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur Heart J. 2016;37:2129–200.
Hofer F, Kazem N, Schweitzer R, Hammer A, Jakse F, Koller L, et al. Prescription patterns of sodium-glucose cotransporter 2 inhibitors and glucagon-like peptide-1 receptor agonists in patients with coronary artery disease. Cardiovasc Drugs Ther. United States; 2021.
Heerspink HJL, Stefánsson BV, Correa-Rotter R, Chertow GM, Greene T, Hou F-F, et al. Dapagliflozin in patients with chronic kidney disease. N Engl J Med United States. 2020;383:1436–46.
Author information
Authors and Affiliations
Contributions
AN, PS, and FH contributed to the conception or design of the work. FH, AH, RS, and UP contributed to the acquisition, analysis, or interpretation of data for the work. FH drafted the manuscript. AN, NK, LK, BR, and CH critically revised the manuscript. All gave final approval and agree to be accountable for all aspects of work ensuring integrity and accuracy.
Corresponding author
Ethics declarations
Ethics Approval
This article does not contain any studies with human participants performed by any of the authors.
Due to the observational character of the study, patient informed consent was not required.
The study protocol complies with the Declaration of Helsinki and was approved by the local ethics committee of the Medical University of Vienna (EK 2267/2019).
Conflict of Interest
Felix Hofer: none.
Niema Kazem: none.
Bernhard Richter: none.
Ulrike Pailer: none.
Ronny Schweitzer: none.
Andreas Hammer: none.
Lorenz Koller: none.
Christian Hengstenberg: none.
Patrick Sulzgruber: grants from Daiichi Sankyo, grants from AstraZeneca, and grants from Boehringer Ingelheim outside the submitted work.
Alexander Niessner: personal fees from Bayer, personal fees from BMS, grants and personal fees from Boehringer Ingelheim, grants and personal fees from Daiichi Sankyo, and personal fees from Pfizer outside the submitted work.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hofer, F., Kazem, N., Richter, B. et al. Prescription Patterns of Sodium-Glucose Cotransporter 2 Inhibitors and Cardiovascular Outcomes in Patients with Diabetes Mellitus and Heart Failure. Cardiovasc Drugs Ther 36, 497–504 (2022). https://doi.org/10.1007/s10557-021-07234-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-021-07234-7