Abstract
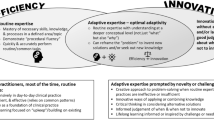
Adaptive expertise represents the combination of both efficient problem-solving for clinical encounters with known solutions, as well as the ability to learn and innovate when faced with a novel challenge. Fostering adaptive expertise requires careful approaches to instructional design to emphasize deeper, more effortful learning. These teaching strategies are time-intensive, effortful, and challenging to implement in health professions education curricula. The authors are educators whose missions encompass the medical education continuum, from undergraduate through to organizational learning. Each has grappled with how to promote adaptive expertise development in their context. They describe themes drawn from educational experiences at these various learner levels to illustrate strategies that may be used to cultivate adaptive expertise.
At Vanderbilt University School of Medicine, a restructuring of the medical school curriculum provided multiple opportunities to use specific curricular strategies to foster adaptive expertise development. The advantage for students in terms of future learning had to be rationalized against assessments that are more short-term in nature. In a consortium of emergency medicine residency programs, a diversity of instructional approaches was deployed to foster adaptive expertise within complex clinical learning environments. Here the value of adaptive expertise approaches must be balanced with the efficiency imperative in clinical care. At Mayo Clinic, an existing continuous professional development program was used to orient the entire organization towards an adaptive expertise mindset, with each individual making a contribution to the shift.
The different contexts illustrate both the flexibility of the adaptive expertise conceptualization and the need to customize the educational approach to the developmental stage of the learner. In particular, an important benefit of teaching to adaptive expertise is the opportunity to influence individual professional identity formation to ensure that clinicians of the future value deeper, more effortful learning strategies throughout their careers.


Similar content being viewed by others
References
Auerbach, L., Santen, S. A., Cutrer, W. B., Daniel, M., Wilson-Delfosse, A. L., & Roberts, N. K. (2020). The educators’ experience: Learning environments that support the master adaptive learner. Medical Teacher, 42(11), 1270–1274.
Betinol, E., Murphy, S., & Regehr, G. (2022). Exploring the development of adaptive expertise through the lens of threshold concepts. Medical Education. https://doi.org/10.1111/medu.14887
Billings, H., Malin, T., Allen, J., Bergene, A., Cornelius, K., Craft, S., Hartzheim, L., Johnson, S. A., Kallay, J., Kreuter, J., & Raths, M. (2022). Reimagining learning spaces of the future: An interprofessional, virtual workshop utilizing rapid idea generation and lean startup methodologies. MedEdPORTAL, 18, 11217.
Bird, E. C., Osheroff, N., Pettepher, C. C., Cutrer, W. B., & Carnahan, R. H. (2017). Using small case-based learning groups as a setting for teaching medical students how to provide and receive peer feedback. Medical Science Educator, 27(4), 759–765.
Bjork, E. L., & Bjork, R. A. (2011). Making things hard on yourself, but in a good way: Creating desirable difficulties to enhance learning. In M. A. Gernsbacher, R. W. Pew, L. M. Hough, & J. R. Pomerantz (Eds.), Psychology and the real world: Essays illustrating fundamental contributions to society (pp. 56–64). Worth Publisher.
Bjork, R. A., & Bjork, E. L. (2020). Desirable difficulties in theory and practice. Journal of Applied Research in Memory and Cognition, 9(4), 475–479.
Bransford, J. D., & Schwartz, D. L. (1999). Rethinking transfer: A simple proposal with multiple implications. Review of Research in Education, 24(1), 61–100.
Branzetti, J., Commissaris, C., Croteau, C., Ehmann, M. R., Gisondi, M. A., Hopson, L. R., Lai, K. Y., & Regan, L. (2022). The best laid plans? A qualitative investigation of how resident physicians plan their learning. Academic Medicine : Journal of the Association of American Medical Colleges, Advance Online Publication. https://doi.org/10.1097/ACM.0000000000004751
Carbonell, K. B., Stalmeijer, R. E., Könings, K. D., Segers, M., & van Merriënboer, J. J. (2014). How experts deal with novel situations: A review of adaptive expertise. Educational Research Review, 12, 14–29.
Charlin, B., Tardif, J., & Boshuizen, H. P. (2000). Scripts and medical diagnostic knowledge: Theory and applications for clinical reasoning instruction and research. Academic Medicine, 75(2), 182–190.
Cutrer, W. B., & Brady, D. (2020). Vanderbilt university school of medicine. Academic Medicine, 95(9S), S474–S477.
Cutrer, W. B., Sullivan, W. M., & Fleming, A. E. (2013). Educational strategies for improving clinical reasoning. Current Problems in Pediatric and Adolescent Health Care, 43(9), 248–257.
Cutrer, W. B., Miller, B., Pusic, M. V., Mejicano, G., Mangrulkar, R. S., Gruppen, L. D., Hawkins, R. E., Skochelak, S. E., & Moore, D. E., Jr. (2017). Fostering the development of master adaptive learners: a conceptual model to guide skill acquisition in medical education. Academic Medicine, 92(1), 70–75.
Cutrer, W. B., Atkinson, H. G., Friedman, E., Deiorio, N., Gruppen, L. D., Dekhtyar, M., & Pusic, M. (2018). Exploring the characteristics and context that allow master adaptive learners to thrive. Medical Teacher, 40(8), 791–796.
Cutrer, W. B., Spickard, W. A., III., Triola, M. M., Allen, B. L., Spell, N., III., Herrine, S. K., Dalrymple, J. L., Gorman, P. N., & Lomis, K. D. (2021). Exploiting the power of information in medical education. Medical Teacher, 43(2), S17–S24.
Dahlman, K. B., Weinger, M. B., Lomis, K. D., Nanney, L., Osheroff, N., Moore, D. E., Estrada, L., & Cutrer, W. B. (2018). Integrating foundational sciences in a clinical context in the post-clerkship curriculum. Medical Science Educator, 28(1), 145–154.
Fleming, A., Cutrer, W., Reimschisel, T., & Gigante, J. (2012). You too can teach clinical reasoning! Pediatrics, 130(5), 795–797.
Fleming, A., Cutrer, W., Moutsios, S., Heavrin, B., Pilla, M., Eichbaum, Q., & Rodgers, S. (2013). Building learning communities: Evolution of the colleges at Vanderbilt University school of medicine. Academic Medicine, 88(9), 1246–1251.
Garrison, D. R. (2007). Online community of inquiry review: Social, cognitive, and teaching presence issues. Journal of Asynchronous Learning Networks, 11(1), 61–72.
Garvin, D. A. (1993). Building a learning organization. Harvard Business Review, 71(4), 78–91. PMID:1012704.
Gephart, M. A., Marsick, V. J., Van Buren, M. E., Spiro, M. S., & Senge, P. (1996). Learning organizations come alive. Training & Development, 50(12), 34–46.
Gonzalo, J. D., Haidet, P., Papp, K. K., Wolpaw, D. R., Moser, E., Wittenstein, R. D., & Wolpaw, T. (2017). Educating for the 21st-century health care system. Academic Medicine, 92(1), 35–39.
Grotzer, T.A., Forshaw, T., & Gonzalez, E. (2021). Develo** adaptive expertise for navigating new terrain: An essential element of success in learning and the workplace. The Next Level Lab at the Harvard Graduate School of Education. President and Fellows of Harvard College: Cambridge, MA.
Gunnerson, K. J., Bassin, B. S., Havey, R. A., Haas, N. L., Sozener, C. B., Medlin, R. P., Gegenheimer-Holmes, J. A., Laurinec, S. L., Boyd, C., Cranford, J. A., & Whitmore, S. P. (2019). Association of an emergency department–based intensive care unit with survival and inpatient intensive care unit admissions. JAMA Network Open, 2(7), e197584–e197584.
Jolly, B. (2014). Faculty development for organizational change. In Faculty Development in the Health Professions (pp. 119–137). Springer, Dordrecht.
Kegan, R., Lahey, L., Fleming, A., & Miller, M. (2014). Making business personal. Harvard Business Review, 92(4), 44–52.
Kua, J., Lim, W. S., Teo, W., & Edwards, R. A. (2021). A sco** review of adaptive expertise in education. Medical Teacher, 43(3), 347–355.
Kulasegaram, K. M., Martimianakis, M. A., Mylopoulos, M., Whitehead, C. R., & Woods, N. N. (2013). Cognition before curriculum: Rethinking the integration of basic science and clinical learning. Academic Medicine, 88(10), 1578–1585.
Lomis, K. D., Mejicano, G. C., Caverzagie, K. J., Monrad, S. U., Pusic, M., & Hauer, K. E. (2021a). The critical role of infrastructure and organizational culture in implementing competency-based education and individualized pathways in undergraduate medical education. Medical Teacher, 43(sup2), S7–S16.
Lomis, K. D., Santen, S. A., Dekhtyar, M., Elliott, V. S., Richardson, J., Hammoud, M. M., Hawkins, R., & Skochelak, S. E. (2021b). The accelerating change in medical education consortium: key drivers of transformative change. Academic Medicine, 96(7), 979–988.
Mayo Clinic College of Medicine and Science. (2021, March). Our Voices, Our Ideas: Students at the Education and Technology Forum. Accessed at https://college.mayo.edu/about/news/news-archive/our-voices-our-ideas-students-at-the-education-and-technology-forum
Merritt, C., Santen, S. A., Cico, S. J., Wolff, M., & Pusic, M. (2022). Punctuated equilibrium: COVID and the duty to teach for adaptive expertise. Western Journal of Emergency Medicine, 23(1), 56.
Mylopoulos, M., & Woods, N. N. (2009). Having our cake and eating it too: Seeking the best of both worlds in expertise research. Medical Education, 43(5), 406–413.
Mylopoulos, M., Brydges, R., Woods, N. N., Manzone, J., & Schwartz, D. L. (2016). Preparation for future learning: A missing competency in health professions education? Medical Education, 50(1), 115–123.
Mylopoulos, M., Steenhof, N., Kaushal, A., & Woods, N. N. (2018a). Twelve tips for designing curricula that support the development of adaptive expertise. Medical Teacher, 40(8), 850–854. https://doi.org/10.1080/0142159X.2018.1484082
Mylopoulos, M., Kulasegaram, K., & Woods, N. N. (2018b). Develo** the experts we need: Fostering adaptive expertise through education. Journal of Evaluation in Clinical Practice, 24(3), 674–677.
Neubauer, B. E., Witkop, C. T., & Varpaio, L. (2019). How phenomenology can help us learn from the experiences of others. Perspectives on Medical Education, 8(2), 90–97.
Pusic, M. V., Santen, S. A., Dekhtyar, M., Poncelet, A. N., Roberts, N. K., Wilson-Delfosse, A. L., & Cutrer, W. B. (2018). Learning to balance efficiency and innovation for optimal adaptive expertise. Medical Teacher, 40(8), 820–827.
Pusic, M., Cutrer, W., & Santen, S. A. (2019a). How does Master Adaptive Learning advance expertise development? Chapter 2. In W. Cutrer & M. V. Pusic (Eds.), The Master Adaptive Learner (pp. 10–17). NL. Elsevier Publishing Group.
Pusic, M., Boutis, K., Cutrer, W., & Santen, S. A. (2019b). How does master adaptive learning ensure optimal pathways to clinical expertise? Chapter 16. In W. Cutrer & M. V. Pusic (Eds.), The Master Adaptive Learner (pp. 174–192). NL. Elsevier Publishing Group.
Regan, L., Hopson, L. R., Gisondi, M. A., & Branzetti, J. (2019). Learning to learn: A qualitative study to uncover strategies used by master adaptive learners in the planning of learning. Medical Teacher, 41(11), 1252–1262.
Schumacher, D. J., Englander, R., & Carraccio, C. (2013). Develo** the master learner: Applying learning theory to the learner, the teacher, and the learning environment. Academic Medicine, 88(11), 1635–1645.
Senge, P. (1990). The Fifth Discipline: The Art and Practice of the Learning Organization. New York.
Steenhof, N. (2020). Adaptive expertise in continuing pharmacy professional development. Pharmacy, 8(1), 21.
Stringer, J. K., Gruppen, L. D., Ryan, M. S., Ginzburg, S. B., Cutrer, W. B., Wolff, M., & Santen, S. A. (2022). Measuring the master adaptive learner: development and internal structure validity evidence for a new instrument. Medical Science Educator, 32(1), 183–193.
ten Cate, O., Snell, L., Mann, K., & Vermunt, J. (2004). Orienting teaching toward the learning process. Academic Medicine : Journal of the Association of American Medical Colleges, 79(3), 219–228. https://doi.org/10.1097/00001888-200403000-00005.
Thistlethwaite, J. E., Davies, D., Ekeocha, S., Kidd, J. M., MacDougall, C., Matthews, P., Purkis, J., & Clay, D. (2012). The effectiveness of case-based learning in health professional education. A BEME systematic review: BEME Guide No 23. Medical teacher, 34(6), e421–e444.
Acknowledgements
HB and EH wish to acknowledge the 2021 and 2022 Mayo Clinic ETF Team, in particular Dr. Amy Seegmiller Renner and Lisa Hartzheim for their development of the personas.
Funding
WBC and MVP wish to acknowledge the grant support of the American Medical Association Reimagining Residency initiative. No funding was received to assist with the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the manuscript conception and design. Material preparation and the first outline of the manuscript was written by MVP and WBC; WBC wrote the first draft of the UME section; LH, LR, MG, JB wrote the first draft of the GME section; HB, EH wrote the first draft of the CPD section; and all authors commented on subsequent versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Research involving human participants
The authors describe their experiences in innovating in their specific education programs where the innovations are considered within the scope of work.
Informed consent
Where we report on research data that was collected, we cite references that report the study details including consent processes and institutional review board approval. No new primary research was carried out for this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pusic, M.V., Hall, E., Billings, H. et al. Educating for adaptive expertise: case examples along the medical education continuum. Adv in Health Sci Educ 27, 1383–1400 (2022). https://doi.org/10.1007/s10459-022-10165-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10459-022-10165-z