Abstract
Purpose
We sought to detect left ventricular (LV) adverse alterations in structure and function in type 2 diabetes mellitus (T2DM) patients with or without mild renal dysfunction (MRD) using comprehensive echocardiography techniques and to explore the independent risk factors for LV remodeling (LVR) and dysfunction in these patients.
Methods
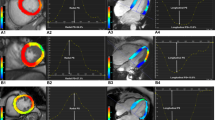
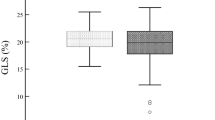
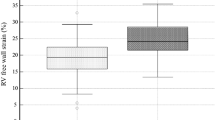
The study included 82 T2DM patients with normal LV ejection fraction (presence (n = 42)/absence (n = 40) of MRD). Age- and gender-matched controls (n = 40) were also recruited. LV structure and function were evaluated using conventional echocardiography and three-dimensional speckle tracking echocardiography (3DSTE). Global longitudinal strain (GLS), global circumferential strain (GCS), global area strain (GAS), and global radial strain (GRS) were all measured using 3DSTE.
Results
Compared with the controls with absolute advantage of LV normal geometry, LVR was more frequently present in the two T2DM groups, with the largest proportion in those with T2DM and MRD (P < 0.001). Fasting plasma glucose (FPG) and MRD were both significant risk factors for LVR in T2DM patients.
The detection rates of LV diastolic dysfunction and subclinical systolic dysfunction were significantly higher in the T2DM groups than in the controls (P = 0.000). Moreover, the two case groups also showed significantly lower strain values in multiple directions than the controls (all P < 0.05). FPG was significantly associated with LV diastolic dysfunction, whereas FPG and MRD were both significantly associated with subclinical LV systolic dysfunction in T2DM patients.
Conclusions
The combined use of conventional echocardiography and 3DSTE allowed the timely detection of early cardiac damage in T2DM patients with or without MRD.

Similar content being viewed by others
References
Ahn HS, Kim JH, Jeong H, et al. Differential urinary proteome analysis for predicting prognosis in type 2 diabetes patients with and without renal dysfunction. Int J Mol Sci. 2020;21:4236. https://doi.org/10.3390/ijms21124236.
Duran M, Elcik D, Inanc MT, et al. Relationship between mild renal dysfunction and coronary artery disease in young patients with stable angina pectoris. Biomark Med. 2020;14:433–40.
Li Y, Teng D, Shi X, et al. Prevalence of diabetes recorded in mainland China using 2018 diagnostic criteria from the American Diabetes Association: national cross sectional study. BMJ. 2020;369: m997.
Matthews DR, Hosker JP, Rudenski AS, et al. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985;28:412–9.
Ma YC, Zuo L, Chen JH, et al. Modified glomerular filtration rate estimating equation for Chinese patients with chronic kidney disease. J Am Soc Nephrol. 2006;17:2937–44.
Cao C, Hu JX, Dong YF, et al. Association of endothelial and mild renal dysfunction with the severity of left ventricular hypertrophy in hypertensive patients. Am J Hypertens. 2016;29:501–8.
Lang RM, Badano LP, Mor-Avi V, et al. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American society of echocardiography and the European association of cardiovascular imaging. J Am Soc Echocardiogr. 2015;28:1–39.
Oktay AA, Lavie CJ, Milani RV, et al. Current perspectives on left ventricular geometry in systemic hypertension. Prog Cardiovasc Dis. 2016;59:235–46.
Yildiz M, Oktay AA, Stewart MH, et al. Left ventricular hypertrophy and hypertension. Prog Cardiovasc Dis. 2020;63:10–21.
Toya T, Fukushima S, Shimahara Y, et al. Reverse left ventricular remodeling after aortic valve replacement for severe aortic insufficiency. Interact Cardiovasc Thorac Surg. 2021;32:846–54.
van Blisen M, Smeets PJ, Gilde AJ, et al. Metabolic remodeling of the failing heart: the cardiac burn-out syndrome? Cradovasc Res. 2004;61:218–26.
Cioffi G, Giorda CB, Lucci D, et al. Effects of linagliptin on left ventricular DYsfunction in patients with type 2 DiAbetes and concentric left ventricular geometry: results of the DYDA 2 trial. Eur J Prev Cardiol. 2021;23:8–17.
Antakly-Hanon Y, Ben Hamou A, Garçon P, et al. Asymptomatic left ventricular dysfunction in patients with type 2 diabetes free of cardiovascular disease and its relationship with clinical characteristics: The DIACAR cohort study. Diabetes Obes Metab. 2021;23:434–43.
Rutter MK, Parise H, Benjamin EJ, et, al. Impact of glucose intolerance and insulin resistance on cardiac structure and function: sex-related differences in the Framingham heart study. Circulation. 2003;107:448–54.
Kato Y, Hayashi M, Ohno Y, et al. Mild renal dysfunction is associated with insulin resistance in chronic glomerulonephritis. Clin Nephrol. 2000;54:366–73.
Leoncini G, Viazzi F, Parodi D, et al. Mild renal dysfunction and subclinical cardiovascular damage in primary hypertension. Hypertension. 2003;42:14–8.
Smilde TD, Asselbergs FW, Hillege HL, et al. Mild renal dysfunction is associated with electrocardiographic left ventricular hypertrophy. Am J Hypertens. 2005;18:342–7.
Ye M, Liu Y, Wang H, et al. Serum apolipoprotein B is inversely associated with eccentric left ventricular hypertrophy in peritoneal dialysis patients. Int Urol Nephrol. 2018;50:155–65.
Patel N, Yaqoob MM, Aksentijevic D. Cardiac metabolic remodelling in chronic kidney disease. Nat Rev Nephrol. 2022;18:524–37.
Nicoara A, Jones-Haywood M. Diastolic heart failure: diagnosis and therapy. Curr Opin Anesthesiol. 2016;29:61–7.
Mocan M, Anton F, Suciu Ș, et al. Multi-marker assessment of diastolic dysfunction in metabolic syndrome patients. Metab Syndr Relatd. 2017;15:507–14.
Lorell BH. Left ventricular hypertrophy and diastolic dysfunction. Hosp Pract. 1992;27:189–94.
Toba A, Kariya T, Aoyama R, et al. Impact of age on left ventricular geometry and diastolic function in elderly patients with treated hypertension. Blood Press. 2017;26:264–71.
Lee H, Kong YH, Kim KH, et al. Left ventricular hypertrophy and diastolic function in children and adolescents with essential hypertension. Clin Hypertens. 2015;21:21.
Akdeniz B, Gedik A, Turan O. Evaluation of left ventricular diastolic function according to new criteria and determinants in acromegaly. NT Heart J. 2012;53:299–305.
Tran AH, Flynn JT, Becker RC, et al. Subclinical systolic and diastolic dysfunction is evident in youth with elevated blood pressure. Hypertension. 2020;75:1551–6.
Oneglia AP, Szczepaniak LS, Cipher DJ, et al. Myocardial steatosis impairs left ventricular diastolic-systolic coupling in healthy humans. J Physiol-London. 2023;60:1371–82.
Sampaio F, Pimenta J, Bettencourt N, et al. Systolic and diastolic dysfunction in cirrhosis: a tissue-Doppler and speckle tracking echocardiography study. Liver Int. 2013;33:1158–65.
Hernandez-Suarez DF, Lopez-Menendez F, Roche-Lima A, et al. Assessment of mitral annular plane systolic excursion in patients with left ventricular diastolic dysfunction. Cardiol Res. 2019;10:83–8.
Gu H, Liu Y, Mei S, et al. Left ventricular diastolic dysfunction in nonhuman primate model of dys-metabolism and diabetes. BMC Cardiovasc Disord. 2015;15:141.
Parsaee H, Nabati M, Azizi S, et al. Correlation between albuminuria and tissue Doppler-derived left ventricular myocardial performance index in patients with type 2 diabetes. J Clin Ultrasound. 2021;49:472–8.
Morais H, Feijão A, De Victória PS. Values of left ventricular diastolic function assessed by left atrial volumes and Doppler echocardiography in healthy Angolans: effect of age and gender: a pilot study. J Clin Ultrasound. 2021;49:791–8.
Miyoshi T, Addetia K, Citro R, et al. Left ventricular diastolic function in healthy adult individuals: results of the world alliance societies of echocardiography normal values study. J Am Soc Echocardiog. 2020;33:1223–33.
Cardio-Renal Connections in Heart Failure and Cardiovascular Disease | National Heart, Lung, and Blood Institute (NHLBI). https://www.nhlbi.nih. gov/events/2004/cardio-renal-connections-heartfailure-and-cardiovasculardisease (Accessed March 25, 2022).
Ricci Z, Romagnoli S, Ronco C. Cardiorenal Syndrome. Crit Care Clin. 2021;37:335–47.
Oyedeji AT, Balogun MO, Akintomide AA, et al. The significance of mild renal dysfunction in chronic heart failure. Afr J Med. 2011;30:442–6.
Lekakis JP, Papamichael CM, Vemmos CN, et al. Peripheral vascular endothelial dysfunction in patients with angina pectoris and normal coronary arteriograms. J Am Coll Cardiol. 1998;31:541–6.
Wong TY, Klein R, Sharrett AR, et al. Retinal arteriolar narrowing and risk of coronary heart disease in men and women the atherosclerosis risk in communities study. JAMA. 2002;287:1153–9.
Schwartzkopff B, Motz W, Frenzel H, et al. Structural and functional alterations of the intra-myocardial coronary arterioles in patients with arterial hypertension. Circulation. 1993;88:993–1003.
Chade AR, Brosh D, Higano ST, et al. Mild renal insufficiency is associated with reduced coronary flow in patients with non-obstructive coronary artery disease. Kidney Intern. 2006;69:266–71.
Martin FL, McKie PM, Cataliotti A, et al. Experimental mild renal insufficiency mediates early cardiac apoptosis, fibrosis, and diastolic dysfunction: a kidney-heart connection. Am J Physiol Regul Integr Comp Physiol. 2012;302:R292-9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Qingqing Wang and **a Tao declare that there are no conflicts of interest.
Ethical approval
The study was approved by the local ethics committee and the institutional review board (IRB) of our hospital in accordance with the Declaration of Helsinki. All study subjects or their guardians signed written informed consent prior to enrollment.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Wang, Q., Tao, X. Mild renal dysfunction causes aggravated cardiac damage in type 2 diabetic patients: a comprehensive echocardiography study. J Med Ultrasonics (2024). https://doi.org/10.1007/s10396-024-01456-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10396-024-01456-6