Abstract
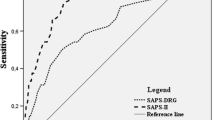
Early prediction of in-hospital mortality in aneurysmal subarachnoid hemorrhage (aSAH) is essential for the optimal management of these patients. Recently, a retrospective cohort observation has reported that the rate-pressure product (RPP, the product of systolic blood pressure and heart rate), an objective and easily calculated bedside index of cardiac hemodynamics, was predictively associated with in-hospital mortality following traumatic brain injury. We thus wondered whether this finding could also be generalized to aSAH patients. The current study aimed to examine the association of RPP at the time of emergency room (ER) admission with in-hospital mortality and its predictive performance among aSAH patients. We retrospectively included 515 aSAH patients who had been admitted to our ER between 2016 and 2020. Their baseline heart rate and systolic blood pressure at ER presentation were extracted for the calculation of the admission RPP. Meanwhile, we collected relevant clinical, laboratory, and neuroimaging data. Then, these data including the admission RPP were examined by univariate and multivariate analyses to identify independent predictors of hospital mortality. Eventually, continuous and ordinal variables were selected from those independent predictors, and the performance of these selected predictors was further evaluated and compared based on receiver operating characteristic (ROC) curve analyzes. We identified both low (< 10,000; adjusted odds ratio (OR) 3.49, 95% CI 1.93–6.29, p < 0.001) and high (> 15,000; adjusted OR 8.42, 95% CI 4.16–17.06, p < 0.001) RPP on ER admission to be independently associated with in-hospital mortality after aSAH. Furthermore, after centering the admission RPP by its median, the area under its ROC curve (0.761, 95% CI 0.722–0.798, p < 0.001) was found to be statistically superior to any of the other independent predictors included in the ROC analyzes (all p < 0.01). In light of the predictive superiority of the admission RPP, as well as its objectivity and easy accessibility, it is indeed a potentially more applicable predictor for in-hospital death in aSAH patients.




Similar content being viewed by others
Data availability
Data supporting the study is available from the corresponding author on reasonable demand.
Code availability
Not applicable.
References
Nieuwkamp DJ, Vaartjes I, Algra A, Bots ML, Rinkel GJ (2013) Age- and gender-specific time trend in risk of death of patients admitted with aneurysmal subarachnoid hemorrhage in the Netherlands. Int J Stroke 8:90–94. https://doi.org/10.1111/ijs.12006
Nieuwkamp DJ, Setz LE, Algra A, Linn FH, de Rooij NK, Rinkel GJ (2009) Changes in case fatality of aneurysmal subarachnoid haemorrhage over time, according to age, sex, and region: a meta-analysis. Lancet Neurol 8:635–642. https://doi.org/10.1016/S1474-4422(09)70126-7
Øie LR, Solheim O, Majewska P, Nordseth T, Müller TB, Carlsen SM, Jensberg H, Salvesen Ø, Gulati S (2020) Incidence and case fatality of aneurysmal subarachnoid hemorrhage admitted to hospital between 2008 and 2014 in Norway. Acta Neurochir Wien 162:2251–2259. https://doi.org/10.1007/s00701-020-04463-x
Abulhasan YB, Alabdulraheem N, Simoneau G, Angle MR, Teitelbaum J (2018) Mortality after spontaneous subarachnoid hemorrhage: causality and validation of a prediction model. World Neurosurg 112:e799–e811. https://doi.org/10.1016/j.wneu.2018.01.160
Ding CY, Cai HP, Ge HL, Yu LH, Lin YX, Kang DZ (2020) Is admission lipoprotein-associated phospholipase A2 a novel predictor of vasospasm and outcome in patients with aneurysmal subarachnoid hemorrhage? Neurosurgery 86:122–131. https://doi.org/10.1093/neuros/nyz041
Jabbarli R, Reinhard M, Niesen WD, Roelz R, Shah M, Kaier K, Hippchen B, Taschner C, Van Velthoven V (2015) Predictors and impact of early cerebral infarction after aneurysmal subarachnoid hemorrhage. Eur J Neurol 22:941–947. https://doi.org/10.1111/ene.12686
Mourelo-Fariña M, Pértega S, Galeiras R (2021) A model for prediction of in-hospital mortality in patients with subarachnoid hemorrhage. Neurocrit Care 34:508–518. https://doi.org/10.1007/s12028-020-01041-y
Mader MM, Piffko A, Dengler NF, Ricklefs FL, Dührsen L, Schmidt NO, Regelsberge-r J, Westphal M, Wolf S, Czorlich P (2020) Initial pupil status is a strong predictor for in-hospital mortality after aneurysmal subarachnoid hemorrhage. Sci Rep 10:4764. https://doi.org/10.1038/s41598-020-61513-1
Risselada R, Lingsma HF, Bauer-Mehren A, Friedrich CM, Molyneux AJ, Kerr RS, Yarnold J, Sneade M, Steyerberg EW, Sturkenboom MC (2010) Prediction of 60 day case-fatality after aneurysmal subarachnoid haemorrhage: results from the International Subarachnoid Aneurysm Trial (ISAT). Eur J Epidemiol 25:261–266. https://doi.org/10.1007/s10654-010-9432-x
Slettebø H, Karic T, Sorteberg A (2020) Impact of smoking on course and outcome of aneurysmal subarachnoid hemorrhage. Acta Neurochir Wien 162:3117–3128. https://doi.org/10.1007/s00701-020-04506-3
Degen LA, Dorhout Mees SM, Algra A, Rinkel GJ (2011) Interobserver variability of gra-ding scales for aneurysmal subarachnoid hemorrhage. Stroke 42:1546–1549. https://doi.org/10.1161/STROKEAHA.110.601211
Frontera JA, Claassen J, Schmidt JM, Wartenberg KE, Temes R, Connolly ES Jr, MacDon-ald RL, Mayer SA (2006) Prediction of symptomatic vasospasm after subarachnoid hemorrhage: the modified fisher scale. Neurosurgery 59:21–27. https://doi.org/10.1227/01.NEU.0000218821.34014.1B
Smith ML, Abrahams JM, Chandela S, Smith MJ, Hurst RW, Le Roux PD (2005) Subarachnoid hemorrhage on computed tomography scanning and the development of cerebral vasospasm: the Fisher grade revisited. Surg Neurol 63:229–235. https://doi.org/10.1016/j.surneu.2004.06.017
Stienen MN, Germans M, Burkhardt JK, Neidert MC, Fung C, Bervini D, Zumofen D, R-öthlisberger M, Marbacher S, Maduri R, Robert T, Seule MA, Bijlenga P, Schaller K, Fa-ndino J, Smoll NR, Maldaner N, Finkenstädt S, Esposito G, Schatlo B, Keller E, Bozino-v O, Regli L, Swiss SOS Study Group (2018) Predictors of in-hospital death after aneurysmal subarachnoid hemorrhage: analysis of a nationwide database (Swiss SOS [Swiss Study on Aneurysmal Subarachnoid Hemorrhage]). Stroke 49:333–340. https://doi.org/10.1161/STROKEAHA.117.019328
Hagel JA, Sperotto F, Laussen PC, Salvin JW, Bachu A, Kheir JN (2021) Shock Index, coronary perfusion pressure, and rate pressure product as predictors of adverse outcome after pediatric cardiac surgery. Pediatr Crit Care Med 22:e67–e78. https://doi.org/10.1097/PCC.0000000000002524
Kiviniemi AM, Kenttä TV, Lepojärvi S, Perkiömäki JS, Piira OP, Ukkola O, Huikuri HV, Junttila MJ, Tulppo MP (2019) Recovery of rate-pressure product and cardiac mortality in coronary artery disease patients with type 2 diabetes. Diabetes Res Clin Pract 150:150–157. https://doi.org/10.1016/j.diabres.2019.03.007
Verma AK, Sun JL, Hernandez A, Teerlink JR, Schulte PJ, Ezekowitz J, Voors A, St-arling R, Armstrong P, O’Conner CM, Mentz RJ (2018) Rate pressure product and the components of heart rate and systolic blood pressure in hospitalized heart failure patients with preserved ejection fraction: Insights from ASCEND-HF. Clin Cardiol 41:945–952. https://doi.org/10.1002/clc.22981
Krishnamoorthy V, Vavilala MS, Chaikittisilpa N, Rivara FP, Temkin NR, Lele AV, Gibbons EF, Rowhani-Rahbar A (2018) Association of early myocardial workload and mortality following severe traumatic brain Injury. Crit Care Med 46:965–971. https://doi.org/10.1097/CCM.0000000000003052
Izzy S, Muehlschlegel S (2014) Cerebral vasospasm after aneurysmal subarachnoid hemorrhage and traumatic brain injury. Curr Treat Options Neurol 16:278. https://doi.org/10.1007/s11940-013-0278-x
Rzheutskaya RE (2012) Characteristics of hemodynamic disorders in patients with severe traumatic brain injury. Crit Care Res Pract 2012:606179. https://doi.org/10.1155/2012/606179
Treggiari MM (2011) Participants in the international multi-disciplinary consensus conference on the critical care management of subarachnoid hemorrhage. Hemodynamic management of subarachnoid hemorrhage. Neurocrit Care 15:329–335. https://doi.org/10.1007/s12028-011-9589-5
Ho KM (2017) Effect of non-linearity of a predictor on the shape and magnitude of its receiver-operating-characteristic curve in predicting a binary outcome. Sci Rep 7:10155. https://doi.org/10.1038/s41598-017-10408-9
Coghlan LA, Hindman BJ, Bayman EO, Banki NM, Gelb AW, Todd MM, Zaroff JG, Investigators IHAST (2009) Independent associations between electrocardiographic abnormalities and outcomes in patients with aneurysmal subarachnoid hemorrhage: findings from the intra-operative hypothermia aneurysm surgery trial. Stroke 40:412–418. https://doi.org/10.1161/STROKEAHA.108.528778
Frontera JA, Parra A, Shimbo D, Fernandez A, Schmidt JM, Peter P, Claassen J, Wartenberg KE, Rincon F, Badjatia N, Naidech A, Connolly ES, Mayer SA (2008) Cardiac arrhythmias after subarachnoid hemorrhage: risk factors and impact on outcome. Cerebrovasc Dis 26:71–78. https://doi.org/10.1159/000135711
Kerro A, Woods T, Chang JJ (2017) Neurogenic stunned myocardium in subarachnoid hemorrhage. J Crit Care 38:27–34. https://doi.org/10.1016/j.jcrc.2016.10.010
Krishnamoorthy V, Mackensen GB, Gibbons EF, Vavilala MS (2016) Cardiac dysfunction after neurologic injury: what do we know and where are we going? Chest 149:1325–1331. https://doi.org/10.1016/j.chest.2015.12.014
Murthy SB Shah S Rao CP Bershad EM Suarez JI (2015) Neurogenic stunned myocardium following acute subarachnoid hemorrhage: pathophysiology and practical considerations. J Intensive Care Med 30: 318–325. 10.1177%2F0885066613511054
Kuwabara K, Fushimi K, Matsuda S, Ishikawa KB, Horiguchi H, Fujimori K (2013) Association of early post-procedure hemodynamic management with the outcomes of subarachnoid hemorrhage patients. J Neurol 260:820–831. https://doi.org/10.1007/s00415-012-6710-4
Nguyen H, Zaroff JG (2009) Neurogenic stunned myocardium. Curr Neurol Neurosci Rep 9:486–491. https://doi.org/10.1007/s11910-009-0071-0
La Fountaine MF (2018) An anatomical and physiological basis for the cardiovascular autonomic nervous system consequences of sport-related brain injury. Int J Psychophysiol 132:155–166. https://doi.org/10.1016/j.ijpsycho.2017.11.016
Ozdemir B, Kanat A, Ozdemir V, Batcik OE, Yazar U, Guvercin AR (2019) The effect of neuroscientists on the studies of autonomic nervous system dysfunction following experimental subarachnoid hemorrhage. J Craniofac Surg 30:2184–2188. https://doi.org/10.1097/SCS.0000000000005763
Biswas AK, Scott WA, Sommerauer JF, Luckett PM (2000) Heart rate variability after acute traumatic brain injury in children. Crit Care Med 28:3907–3912. https://doi.org/10.1097/00003246-200012000-00030
Kawahara E, Ikeda S, Miyahara Y, Kohno S (2003) Role of autonomic nervous dysfunction in electrocardio-graphic abnormalities and cardiac injury in patients with acute subarachnoid hemorrhage. Circ J 67:753–756. https://doi.org/10.1253/circj.67.753
Winchell RJ, Hoyt DB (1997) Analysis of heart-rate variability: a noninvasive predictor of death and poor outcome in patients with severe head injury. J Trauma 43:927–933. https://doi.org/10.1097/00005373-199712000-00010
Funding
This work was supported by the Yangfan Project for Key Medical Programs from the Hospital Authority of Bei**g (Grant number ZYLX202109, Grant recipient: Shi G) and the Major Projects from Bei**g Municipal Science and Technology Commission (Grant number Z201100005520039, Grant recipient: Shi G). Neither of the funders play any role in the study design, data collection and analysis, decision to publish, or write-up of the manuscript.
Author information
Authors and Affiliations
Contributions
Conceptualization and study design: Zhao J., Shi G., and Zhou J.; funding acquisition: Shi G.; study supervision: Shi G.; data acquisition and curation: Zhang S. and Ma J.; formal analysis: Zhao J.: writing—original draft: Zhao J.; all authors have reviewed, critically revised, and approved the final manuscript submitted.
Corresponding author
Ethics declarations
Ethics approval
This study was performed in accordance with the principles of the Declaration of Helsinki and was approved by the Institutional Review Board of Be**g Tiantan Hospital (approval number: KY-2021–025-003).
Consent to participate
Because of the retrospective and observational design of the study, informed written consent was not required according to the regulations of the local ethics committee.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhao, J., Zhang, S., Ma, J. et al. Admission rate-pressure product as an early predictor for in-hospital mortality after aneurysmal subarachnoid hemorrhage. Neurosurg Rev 45, 2811–2822 (2022). https://doi.org/10.1007/s10143-022-01795-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-022-01795-3