Abstract
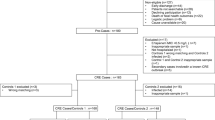
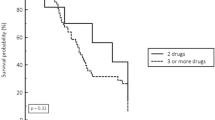
This study was aimed to determine the risk factors of Carbapenem-resistant Enterobacteriaceae (CRE) nosocomial infections and assess the clinical outcomes. A case-case–control design was used to compare two groups of case patients with control patients from March 2010 to November 2014 in China. Risk factors for the acquisition of CRE infections and clinical outcomes were analyzed by univariable and multivariable analysis. A total of 94 patients with CRE infections, 93 patients with Carbapenem-susceptible Enterobacteriaceae (CSE) infections, and 93 patients with organisms other than Enterobacteriaceae infections were enrolled in this study. Fifty-five isolates were detected as the carbapenemase gene. KPC-2 was the most common carbapenemase (65.5 %, 36/55), followed by NDM-1 (16.4 %, 9/55), IMP-4 (14.5 %, 8/55), NDM-5 (1.8 %, 1/55), and NDM-7 (1.8 %, 1/55). Multivariable analysis implicated previous use of third or fourth generation cephalosporins (odds ratio [OR], 4.557; 95 % confidence interval [CI], 1.971–10.539; P < 0.001) and carbapenems (OR, 4.058; 95 % CI, 1.753-9.397; P = 0.001) as independent risk factors associated with CRE infection. The in-hospital mortality of the CRE group was 57.4 %. In the population of CRE infection, presence of central venous catheters (OR, 4.464; 95 % CI, 1.332–14.925; P = 0.015) and receipt of immunosuppressors (OR, 7.246; 95 % CI, 1.217–43.478; P = 0.030) were independent risk factors for mortality. Appropriate definitive treatment (OR, 0.339; 95 % CI, 0.120–0.954; P = 0.040) was a protective factor for in-hospital death of CRE infection. Kaplan–Meier curves of the CRE group had the shortest survival time compared with the other two groups. Survival time of patients infected with Enterobacteriaceae with a high meropenem MIC (≥8 mg/L) was shorter than that of patients with a low meropenem MIC (2,4, and ≤ 1 mg/L). In conclusion, CRE nosocomial infections are associated with prior exposure to third or fourth generation cephalosporins and carbapenems. Patients infected with CRE had poor outcome and high mortality, especially high meropenem MIC (≥8 mg/L). Appropriate definitive treatment to CRE infections in the patient is essential.


Similar content being viewed by others
References
Temkin E, Adler A, Lerner A, Carmeli Y (2014) Carbapenem-resistant Enterobacteriaceae: biology, epidemiology, and management. Ann NY Acad Sci 1323:22–42
Queenan AM, Bush K (2007) Carbapenemases: the versatile beta-lactamases. Clin Microbiol Rev 20:440–458, Table of contents
Nordmann P, Cuzon G, Naas T (2009) The real threat of Klebsiella pneumoniae carbapenemase-producing bacteria. Lancet Infect Dis 9:228–236
Doumith M, Ellington MJ, Livermore DM, Woodford N (2009) Molecular mechanisms disrupting porin expression in ertapenem-resistant Klebsiella and Enterobacter spp. clinical isolates from the UK. J Antimicrob Chemother 63:659–667
Falagas ME, Tansarli GS, Karageorgopoulos DE, Vardakas KZ (2014) Deaths attributable to carbapenem-resistant Enterobacteriaceae infections. Emerg Infect Dis 20:1170–1175
Gupta N, Limbago BM, Patel JB, Kallen AJ (2011) Carbapenem-resistant Enterobacteriaceae: epidemiology and prevention. Clin Infect Dis 53:60–67
Patel G, Huprikar S, Factor SH, Jenkins SG, Calfee DP (2008) Outcomes of carbapenem-resistant Klebsiella pneumoniae infection and the impact of antimicrobial and adjunctive therapies. Infect Control Hosp Epidemiol 29:1099–1106
Chen S, Feng W, Chen J et al (2014) Spread of carbapenemase-producing enterobacteria in a southwest hospital in China. Ann Clin Microbiol Antimicrob 13:42
Kumarasamy KK, Toleman MA, Walsh TR et al (2010) Emergence of a new antibiotic resistance mechanism in India, Pakistan, and the UK: a molecular, biological, and epidemiological study. Lancet Infect Dis 10:597–602
Bogan C, Kaye KS, Chopra T et al (2014) Outcomes of carbapenem-resistant Enterobacteriaceae isolation: matched analysis. Am J Infect Control 42:612–620
Kofteridis DP, Valachis A, Dimopoulou D et al (2014) Risk factors for carbapenem-resistant Klebsiella pneumoniae infection/colonization: a case-case–control study. J Infect Chemother 20:293–297
Schwaber MJ, Klarfeld-Lidji S, Navon-Venezia S, Schwartz D, Leavitt A, Carmeli Y (2008) Predictors of carbapenem-resistant Klebsiella pneumoniae acquisition among hospitalized adults and effect of acquisition on mortality. Antimicrob Agents Chemother 52:1028–1033
Vardakas KZ, Matthaiou DK, Falagas ME, Antypa E, Koteli A, Antoniadou E (2015) Characteristics, risk factors and outcomes of carbapenem-resistant Klebsiella pneumoniae infections in the intensive care unit. J Infect 70:592–599
Correa L, Martino MD, Siqueira I et al (2013) A hospital-based matched case–control study to identify clinical outcome and risk factors associated with carbapenem-resistant Klebsiella pneumoniae infection. BMC Infect Dis 13:80
Jeong SJ, Yoon SS, Bae IK, Jeong SH, Kim JM, Lee K (2014) Risk factors for mortality in patients with bloodstream infections caused by carbapenem-resistant Pseudomonas aeruginosa: clinical impact of bacterial virulence and strains on outcome. Diagn Microbiol Infect Dis 80:130–135
Kritsotakis EI, Tsioutis C, Roumbelaki M, Christidou A, Gikas A (2011) Antibiotic use and the risk of carbapenem-resistant extended-spectrum-beta-lactamase-producing Klebsiella pneumoniae infection in hospitalized patients: results of a double case–control study. J Antimicrob Chemother 66:1383–1391
Harris AD, Karchmer TB, Carmeli Y, Samore MH (2001) Methodological principles of case–control studies that analyzed risk factors for antibiotic resistance: a systematic review. Clin Infect Dis 32:1055–1061
Kaye KS, Harris AD, Samore M, Carmeli Y (2005) The case-case–control study design: addressing the limitations of risk factor studies for antimicrobial resistance. Infect Control Hosp Epidemiol 26:346–351
Schechner V, Temkin E, Harbarth S, Carmeli Y, Schwaber MJ (2013) Epidemiological interpretation of studies examining the effect of antibiotic usage on resistance. Clin Microbiol Rev 26:289–307
Wacholder S, McLaughlin JK, Silverman DT, Mandel JS (1992) Selection of controls in case–control studies. I. Principles. Am J Epidemiol 135:1019–1028
Wacholder S, Silverman DT, McLaughlin JK, Mandel JS (1992) Selection of controls in case–control studies. II. Types of controls. Am J Epidemiol 135:1029–1041
CLSI. Clinical and Laboratory Standards Institute (2014) Performance standards for antimicrobial testing: twentieth informational supplement, CLSI document. M100-S24. Wayne, PA
Horan TC, Andrus M, Dudeck MA (2008) CDC/NHSN surveillance definition of health care-associated infection and criteria for specific types of infections in the acute care setting. Am J Infect Control 36:309–332
Wang X, Li H, Zhao C et al (2014) Novel NDM-9 metallo-beta-lactamase identified from a ST107 Klebsiella pneumoniae strain isolated in China. Int J Antimicrob Agents 44:90–91
Yang Q, Wang H, Sun H, Chen H, Xu Y, Chen M (2010) Phenotypic and genotypic characterization of Enterobacteriaceae with decreased susceptibility to carbapenems: results from large hospital-based surveillance studies in China. Antimicrob Agents Chemother 54:573–577
Centers for Disease Control and Prevention (CDC) (2013) Vital signs: carbapenem-resistant Enterobacteriaceae. MMWR Morb Mortal Wkly Rep 62:165–70
Hawkey PM, **ong J, Ye H, Li H, M’Zali FH (2001) Occurrence of a new metallo-beta-lactamase IMP-4 carried on a conjugative plasmid in Citrobacter youngae from the People’s Republic of China. FEMS Microbiol Lett 194:53–57
Wei ZQ, Du XX, Yu YS, Shen P, Chen YG, Li LJ (2007) Plasmid-mediated KPC-2 in a Klebsiella pneumoniae isolate from China. Antimicrob Agents Chemother 51:763–765
Yu YS, Du XX, Zhou ZH, Chen YG, Li LJ (2006) First isolation of blaIMI-2 in an Enterobacter cloacae clinical isolate from China. Antimicrob Agents Chemother 50:1610–1611
Zhang X, Lou D, Xu Y et al (2013) First identification of coexistence of blaNDM-1 and blaCMY-42 among Escherichia coli ST167 clinical isolates. BMC Microbiol 13:282
Wang Q, Zhao CJ, Wang H et al (2013) Antimicrobial resistance of gram-negative bacilli isolated from 13 teaching hospitals across China. Zhonghua Yi Xue Za Zhi 93:1388–1396
Ahn JY, Song JE, Kim MH et al (2014) Risk factors for the acquisition of carbapenem-resistant Escherichia coli at a tertiary care center in South Korea: a matched case–control study. Am J Infect Control 42:621–625
Teo J, Cai Y, Tang S et al (2012) Risk factors, molecular epidemiology and outcomes of ertapenem-resistant, carbapenem-susceptible Enterobacteriaceae: a case-case–control study. PLoS One 7:e34254
Qureshi ZA, Paterson DL, Potoski BA et al (2012) Treatment outcome of bacteremia due to KPC-producing Klebsiella pneumoniae: superiority of combination antimicrobial regimens. Antimicrob Agents Chemother 56:2108–2113
Patel TS, Nagel JL (2015) Clinical outcomes of Enterobacteriaceae infections stratified by Carbapenem MICs. J Clin Microbiol 53:201–205
Daikos GL, Markogiannakis A (2011) Carbapenemase-producing Klebsiella pneumoniae: (when) might we still consider treating with carbapenems? Clin Microbiol Infect 17:1135–1141
Axel H, Stephan G (2014) Treatment of infections caused by carbapenem-resistant enterobacteriaceae. Curr Treat Options Infect Dis 4:425–438
Acknowledgments
We thank Professor Fengxue Zhu and Doctor Zengli **ao from Intensive Care Unit of Peking University People’s Hospital for providing APACHE II scores.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by the National Natural Science Foundation (81572036).
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Wang, Q., Zhang, Y., Yao, X. et al. Risk factors and clinical outcomes for carbapenem-resistant Enterobacteriaceae nosocomial infections. Eur J Clin Microbiol Infect Dis 35, 1679–1689 (2016). https://doi.org/10.1007/s10096-016-2710-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-016-2710-0