Abstract
Purpose
Recently, it has been reported that sarcopenia and nutritional evaluation are associated with the prognosis of patients with cancer; however, there are only a few detailed reports on oral cancer. This single-center retrospective study aimed to analyze the relationship between computed tomography (CT)-assessed sarcopenia (CT-SP), immunocompetence, nutritional status, and the prognosis of patients with oral squamous cell carcinoma (OSCC).
Methods
This retrospective study included patients who underwent radical therapy with surgery for OSCC between January 2014 and January 2021. Skeletal muscle in the third cervical vertebra (C3) was measured using preoperative cervical CT, and the skeletal muscle index (SMI) was calculated. Nutritional status were investigated using blood tests. The correlation between each parameter and prognosis was analyzed. The primary predictor variables were SMI, ECOG performance status, BMI, and nutritional status. The primary outcome variable was the 5-year overall survival rate (OS) and the secondary outcome variable was 5-year disease-specific survival rate (DSS).
Results
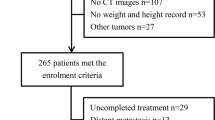
One hundred sixty-three patients were registered retrospectively. The number of patients with CT-SP was 76 (52%). In the univariate analysis, CT-SP, prognostic nutritional index (PNI), and lymphocyte-monocyte ratio (LMR) were associated with poor prognosis, with statistically significant differences in OS and DSS. In the multivariate analysis, only CT-SP was identified as an independent prognostic factor for DSS. CT-SP was significantly correlated with the PNI.
Conclusion
CT-SP was associated with a significant decrease in survival rate in patients with OSCC. Furthermore, CT-SP was correlated with the PNI.


Similar content being viewed by others

Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Sung H et al (2021) Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries, (in eng). CA Cancer J Clin 71(3):209–249. https://doi.org/10.3322/caac.21660
Santilli V, Bernetti A, Mangone M, Paoloni M (2014) Clinical definition of sarcopenia, (in eng). Clin Cases Miner Bone Metab 11(3):177–180
Lin SC et al (2020) Sarcopenia results in poor survival rates in oral cavity cancer patients, (in eng). Clin Otolaryngol 45(3):327–333. https://doi.org/10.1111/coa.13481
Luan CW, Tsai YT, Yang HY, Chen KY, Chen PH, Chou HH (2021) Pretreatment prognostic nutritional index as a prognostic marker in head and neck cancer: a systematic review and meta-analysis, (in eng). Sci Rep 11(1):17117. https://doi.org/10.1038/s41598-021-96598-9
Fang KH et al (2021) Preoperative prognostic nutritional index predicts prognosis of patients with oral cavity cancer, (in eng). Oral Dis. https://doi.org/10.1111/odi.13840
Toiyama Y et al (2016) Clinical burden of C-Reactive protein/albumin ratio before curative surgery for patients with gastric cancer, (in eng). Anticancer Res 36(12):6491–6498. https://doi.org/10.21873/anticanres.11248
Toiyama Y, Miki C, Inoue Y, Tanaka K, Mohri Y, Kusunoki M (2011) "Evaluation of an inflammation-based prognostic score for the identification of patients requiring postoperative adjuvant chemotherapy for stage II colorectal cancer, (in eng). Exp Ther Med 2(1):95–101. https://doi.org/10.3892/etm.2010.175
Tham T, Olson C, Khaymovich J, Herman SW, Costantino PD (2018) The lymphocyte-to-monocyte ratio as a prognostic indicator in head and neck cancer: a systematic review and meta-analysis, (in eng). Eur Arch Otorhinolaryngol 275(7):1663–1670. https://doi.org/10.1007/s00405-018-4972-x
Kanda M et al (2016) Nutritional predictors for postoperative short-term and long-term outcomes of patients with gastric cancer, (in eng). Medicine (Baltimore) 95(24):e3781. https://doi.org/10.1097/MD.0000000000003781
Kalinkovich A, Livshits G (2017) Sarcopenic obesity or obese sarcopenia: A cross talk between age-associated adipose tissue and skeletal muscle inflammation as a main mechanism of the pathogenesis, (in eng). Ageing Res Rev 35:200–221. https://doi.org/10.1016/j.arr.2016.09.008
Katagiri T, Ohyama Y, Miyamoto H, Egawa Y, Moriki T, Hasegawa K (2020) Pathological responses to low-dose irradiation and Pepleomycin in Oral squamous cell carcinoma are predictive of Locoregional control, (in eng). BMC Cancer 20(1):1216. https://doi.org/10.1186/s12885-020-07707-2
Lee J et al (2021) Sarcopenia and systemic inflammation synergistically impact survival in oral cavity cancer, (in eng). Laryngoscope 131(5):E1530–E1538. https://doi.org/10.1002/lary.29221
McMillan DC (2008) An inflammation-based prognostic score and its role in the nutrition-based management of patients with cancer, (in eng). Proc Nutr Soc 67(3):257–262. https://doi.org/10.1017/S0029665108007131
Fukuhara-Makiyama N et al (2021) Personality traits and BMI trends over three years in Japanese university students, (in eng). PLoS ONE 16(3):e0248833. https://doi.org/10.1371/journal.pone.0248833
Yamamoto E, Kohama G, Sunakawa H, Iwai M, Hiratsuka H (1983) Mode of invasion, bleomycin sensitivity, and clinical course in squamous cell carcinoma of the oral cavity, (in eng). Cancer 51(12):2175–2180. https://doi.org/10.1002/1097-0142(19830615)51:12%3c2175::aid-cncr2820511205%3e3.0.co;2-m
Kanda Y (2013) Investigation of the freely available easy-to-use software “EZR” for medical statistics, (in eng). Bone Marrow Transplant 48(3):452–458. https://doi.org/10.1038/bmt.2012.244
Cruz-Jentoft AJ et al (2010) Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People, (in eng). Age Ageing 39(4):412–423. https://doi.org/10.1093/ageing/afq034
Yoshimura T et al (2021) Prognostic role of preoperative sarcopenia evaluation of cervical muscles with long-term outcomes of patients with oral squamous cell carcinoma, (in eng). Cancers (Basel) 13(18):4725. https://doi.org/10.3390/cancers13184725
Cruz-Jentoft AJ et al (2019) Sarcopenia: revised European consensus on definition and diagnosis, (in eng). Age Ageing 48(4):601. https://doi.org/10.1093/ageing/afz046
Cesari M et al (2012) Biomarkers of sarcopenia in clinical trials-recommendations from the International Working Group on Sarcopenia, (in eng). J Cachexia Sarcopenia Muscle 3(3):181–190. https://doi.org/10.1007/s13539-012-0078-2
Baracos VE (2017) Psoas as a sentinel muscle for sarcopenia: a flawed premise, (in eng). J Cachexia Sarcopenia Muscle 8(4):527–528. https://doi.org/10.1002/jcsm.12221
Maeda K, Koga T, Akagi J (2016) Tentative nil per os leads to poor outcomes in older adults with aspiration pneumonia, (in eng). Clin Nutr 35(5):1147–52. https://doi.org/10.1016/j.clnu.2015.09.011
Wong A, Zhu D, Kraus D, Tham T (2021) Radiologically defined sarcopenia affects survival in head and neck cancer: a meta-analysis, (in eng). Laryngoscope 131(2):333–341. https://doi.org/10.1002/lary.28616
Bril SI et al (2019) Interobserver agreement of skeletal muscle mass measurement on head and neck CT imaging at the level of the third cervical vertebra, (in eng). Eur Arch Otorhinolaryngol 276(4):1175–1182. https://doi.org/10.1007/s00405-019-05307-w
Kawamura T et al (2018) Long-term outcomes of gastric cancer patients with preoperative sarcopenia, (in eng). Ann Surg Oncol 25(6):1625–1632. https://doi.org/10.1245/s10434-018-6452-3
Vergara-Fernandez O, Trejo-Avila M, Salgado-Nesme N (2020) Sarcopenia in patients with colorectal cancer: A comprehensive review, (in eng). World J Clin Cases 8(7):1188–1202. https://doi.org/10.12998/wjcc.v8.i7.1188
Shinohara S, Otsuki R, Kobayashi K, Sugaya M, Matsuo M, Nakagawa M (2020) Impact of sarcopenia on surgical outcomes in non-small cell lung cancer, (in eng). Ann Surg Oncol 27(7):2427–2435. https://doi.org/10.1245/s10434-020-08224-z
Terazawa K, Ohashi T, Shibata H, Ishihara T, Ogawa T (2022) Immune-modified Glasgow prognostic score: A new prognostic marker for head and neck cancer, (in eng). Head Neck. https://doi.org/10.1002/hed.27170
Szilasi Z et al (2020) Neutrophil-To-Lymphocyte and Platelet-To-Lymphocyte ratios as prognostic markers of survival in patients with head and neck tumours-results of a retrospective multicentric study, (in eng). Int J Environ Res Public Health 17(5):1742. https://doi.org/10.3390/ijerph17051742
Ruiz-Ranz M et al (2022) Prognostic implications of preoperative systemic inflammatory markers in oral squamous cell carcinoma, and correlations with the local immune tumor microenvironment, (in eng). Front Immunol 13:941351. https://doi.org/10.3389/fimmu.2022.941351
Buzby GP, Mullen JL, Matthews DC, Hobbs CL, Rosato EF (1980) Prognostic nutritional index in gastrointestinal surgery, (in eng). Am J Surg 139(1):160–167. https://doi.org/10.1016/0002-9610(80)90246-9
Abbass T, Dolan RD, Laird BJ, McMillan DC (2019) The relationship between imaging-based body composition analysis and the systemic inflammatory response in patients with cancer: a systematic review, (in eng). Cancers (Basel) 11(9):1304. https://doi.org/10.3390/cancers11091304
Feliciano EMC et al (2017) Association of Systemic Inflammation and Sarcopenia With Survival in Nonmetastatic Colorectal Cancer: Results From the C SCANS Study, (in eng). JAMA Oncol 3(12):e172319. https://doi.org/10.1001/jamaoncol.2017.2319
Sugawara K et al (2020) Associations of systemic inflammation and sarcopenia with survival of esophageal carcinoma patients, (in eng). Ann Thorac Surg 110(2):374–382. https://doi.org/10.1016/j.athoracsur.2020.03.013
Dolan RD, Almasaudi AS, Dieu LB, Horgan PG, McSorley ST, McMillan DC (2019) The relationship between computed tomography-derived body composition, systemic inflammatory response, and survival in patients undergoing surgery for colorectal cancer, (in eng). J Cachexia Sarcopenia Muscle 10(1):111–122. https://doi.org/10.1002/jcsm.12357
Inoue T et al (2016) Changes in exercise capacity, muscle strength, and health-related quality of life in esophageal cancer patients undergoing esophagectomy, (in eng). BMC Sports Sci Med Rehabil 8:34. https://doi.org/10.1186/s13102-016-0060-y
Soares SM, Nucci LB, da Silva MM, Campacci TC (2013) Pulmonary function and physical performance outcomes with preoperative physical therapy in upper abdominal surgery: a randomized controlled trial, (in eng). Clin Rehabil 27(7):616–627. https://doi.org/10.1177/0269215512471063
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and data analysis were performed by Yoshio Ohyama, Yoshinori Inaba, Tomoki Kanemaru, and Mako Kubota. The first draft of the manuscript was written by Yoshio Ohyama and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was approved by the Research Ethics Committee of Shizuoka City Shizuoka Hospital (Registry No.20–40) and was performed in accordance with the latest version of the Declaration of Helsinki.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
Informed consent was obtained from all individual participants included in the study.
Competing interests
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ohyama, Y., Inaba, Y., Kubota, M. et al. CT-assessed sarcopenia and prognostic nutritional index are associated with poor prognosis in oral squamous cell carcinoma. Oral Maxillofac Surg 28, 659–666 (2024). https://doi.org/10.1007/s10006-023-01191-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10006-023-01191-1