Abstract
Introduction
Osteonecrosis of the jaw (ONJ) occurring after invasive dental treatment often adversely affects patients’ activities of daily living. Long-term administration of strong anti-bone resorptive agents such as bisphosphonates prior to invasive dental treatment is considered an ONJ risk factor; however, pathological mechanisms underlying ONJ development remain unclear.
Materials and Methods
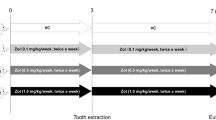
We developed an ONJ mouse model in which a tooth is extracted during treatment with the bisphosphonate zoledronate.
Results
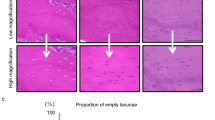
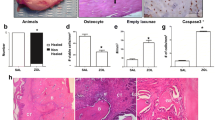
We observed induction of apoptosis in osteocytes, resulting in formation of empty lacunae in jaw bones at sites of tooth extraction but not in other bones of the same mice. We also observed elevated levels of inflammatory cytokines such as TNFα, IL-6 and IL-1 in jaw bone at the extraction site relative to other sites in zoledronate-treated mice. We also report that treatment in vitro with either zoledronate or an extract from Porphyromonas gingivalis, an oral bacteria, promotes expression of inflammatory cytokines in osteoclast progenitor cells. We demonstrate that gene-targeting of either TNFα, IL-6 or IL-1 or treatment with etanercept, a TNFα inhibitor, or a neutralizing antibody against IL-6 can antagonize ONJ development caused by combined tooth extraction and zoledronate treatment.
Conclusions
Taken together, the cytokine storm induced by invasive dental treatment under bisphosphonate treatment promotes ONJ development due to elevated levels of inflammatory cytokine-producing cells. Our work identifies novel targets potentially useful to prevent ONJ.







Similar content being viewed by others
References
Marx RE (2003) Pamidronate (Aredia) and zoledronate (Zometa) induced avascular necrosis of the jaws: a growing epidemic. J Oral Maxillofac Surg 61:1115–1117
Ruggiero SL, Dodson TB, Fantasia J, Goodday R, Aghaloo T, Mehrotra B, O’Ryan F (2014) American Association of Oral and Maxillofacial Surgeons position paper on medication-related osteonecrosis of the jaw–2014 update. J Oral Maxillofac Surg 72:1938–1956
Miksad RA, Lai KC, Dodson TB, Woo SB, Treister NS, Akinyemi O, Bihrle M, Maytal G, August M, Gazelle GS, Swan JS (2011) Quality of life implications of bisphosphonate-associated osteonecrosis of the jaw. Oncologist 16:121–132
Khamaisi M, Regev E, Yarom N, Avni B, Leitersdorf E, Raz I, Elad S (2007) Possible association between diabetes and bisphosphonate-related jaw osteonecrosis. J Clin Endocrinol Metab 92:1172–1175
Molcho S, Peer A, Berg T, Futerman B, Khamaisi M (2013) Diabetes microvascular disease and the risk for bisphosphonate-related osteonecrosis of the jaw: a single center study. J Clin Endocrinol Metab 98:E1807–1812
Berti-Couto SA, Vasconcelos AC, Iglesias JE, Figueiredo MA, Salum FG, Cherubini K (2014) Diabetes mellitus and corticotherapy as risk factors for alendronate-related osteonecrosis of the jaws: a study in Wistar rats. Head Neck 36:84–93
Kastritis E, Melea P, Bagratuni T, Melakopoulos I, Gavriatopoulou M, Roussou M, Migkou M, Eleutherakis-Papaiakovou E, Terpos E, Dimopoulos MA (2017) Genetic factors related with early onset of osteonecrosis of the jaw in patients with multiple myeloma under zoledronic acid therapy. Leuk Lymphoma 58:2304–2309
Rachner TD, Platzbecker U, Felsenberg D, Hofbauer LC (2013) Osteonecrosis of the jaw after osteoporosis therapy with denosumab following long-term bisphosphonate therapy. Mayo Clin Proc 88:418–419
Hoff AO, Toth BB, Altundag K, Johnson MM, Warneke CL, Hu M, Nooka A, Sayegh G, Guarneri V, Desrouleaux K, Cui J, Adamus A, Gagel RF, Hortobagyi GN (2008) Frequency and risk factors associated with osteonecrosis of the jaw in cancer patients treated with intravenous bisphosphonates. J Bone Miner Res 23:826–836
Otto S, Troltzsch M, Jambrovic V, Panya S, Probst F, Ristow O, Ehrenfeld M, Pautke C (2015) Tooth extraction in patients receiving oral or intravenous bisphosphonate administration: a trigger for BRONJ development? J Craniomaxillofac Surg 43:847–854
Ripamonti CI, Maniezzo M, Campa T, Fagnoni E, Brunelli C, Saibene G, Bareggi C, Ascani L, Cislaghi E (2009) Decreased occurrence of osteonecrosis of the jaw after implementation of dental preventive measures in solid tumour patients with bone metastases treated with bisphosphonates. The experience of the National Cancer Institute of Milan. Ann Oncol 20:137–145
Sakaguchi O, Kokuryo S, Tsurushima H, Tanaka J, Habu M, Uehara M, Nishihara T, Tominaga K (2015) Lipopolysaccharide aggravates bisphosphonate-induced osteonecrosis in rats. Int J Oral Maxillofac Surg 44:528–534
Manzano-Moreno FJ, Ramos-Torrecillas J, De Luna-Bertos E, Ruiz C, Garcia-Martinez O (2015) High doses of bisphosphonates reduce osteoblast-like cell proliferation by arresting the cell cycle and inducing apoptosis. J Craniomaxillofac Surg 43:396–401
Marx RE (2014) A decade of bisphosphonate bone complications: what it has taught us about bone physiology. Int J Oral Maxillofac Implants 29:e247–258
Fliefel R, Troltzsch M, Kuhnisch J, Ehrenfeld M, Otto S (2015) Treatment strategies and outcomes of bisphosphonate-related osteonecrosis of the jaw (BRONJ) with characterization of patients: a systematic review. Int J Oral Maxillofac Surg 44:568–585
Kang B, Cheong S, Chaichanasakul T, Bezouglaia O, Atti E, Dry SM, Pirih FQ, Aghaloo TL, Tetradis S (2013) Periapical disease and bisphosphonates induce osteonecrosis of the jaws in mice. J Bone Miner Res 28:1631–1640
Park S, Kanayama K, Kaur K, Tseng HC, Banankhah S, Quje DT, Sayre JW, Jewett A, Nishimura I (2015) Osteonecrosis of the jaw developed in mice: disease variants regulated by gammadelta t cells in oral mucosal barrier immunity. J Biol Chem 290:17349–17366
Soundia A, Hadaya D, Esfandi N, de Molon RS, Bezouglaia O, Dry SM, Pirih FQ, Aghaloo T, Tetradis S (2016) Osteonecrosis of the jaws (ONJ) in mice after extraction of teeth with periradicular disease. Bone 90:133–141
Sun Y, Kaur K, Kanayama K, Morinaga K, Park S, Hokugo A, Kozlowska A, McBride WH, Li J, Jewett A, Nishimura I (2016) Plasticity of Myeloid Cells during Oral Barrier Wound Healing and the Development of Bisphosphonate-related Osteonecrosis of the Jaw. J Biol Chem 291:20602–20616
Kuroshima S, Sasaki M, Nakajima K, Tamaki S, Hayano H, Sawase T (2018) Transplantation of noncultured stromal vascular fraction cells of adipose tissue ameliorates osteonecrosis of the jaw-like lesions in mice. J Bone Miner Res 33:154–166
Bi Y, Gao Y, Ehirchiou D, Cao C, Kikuiri T, Le A, Shi S, Zhang L (2010) Bisphosphonates cause osteonecrosis of the jaw-like disease in mice. Am J Pathol 177:280–290
Kikuiri T, Kim I, Yamaza T, Akiyama K, Zhang Q, Li Y, Chen C, Chen W, Wang S, Le AD, Shi S (2010) Cell-based immunotherapy with mesenchymal stem cells cures bisphosphonate-related osteonecrosis of the jaw-like disease in mice. J Bone Miner Res 25:1668–1679
Zhao Y, Wang L, Liu Y, Akiyama K, Chen C, Atsuta I, Zhou T, Duan X, ** Y, Shi S (2012) Technetium-99 conjugated with methylene diphosphonate ameliorates ovariectomy-induced osteoporotic phenotype without causing osteonecrosis in the jaw. Calcif Tissue Int 91:400–408
Zandi M, Dehghan A, Malekzadeh H, Janbaz P, Ghadermazi K, Amini P (2016) Introducing a protocol to create bisphosphonate-related osteonecrosis of the jaw in rat animal model. J Craniomaxillofac Surg 44:271–278
Allen MR (2015) Medication-related osteonecrosis of the jaw: basic and translational science updates. Oral Maxillofac Surg Clin North Am 27:497–508
Aghaloo TL, Cheong S, Bezouglaia O, Kostenuik P, Atti E, Dry SM, Pirih FQ, Tetradis S (2014) RANKL inhibitors induce osteonecrosis of the jaw in mice with periapical disease. J Bone Miner Res 29:843–854
Conte Neto N, Spolidorio LC, Andrade CR, Bastos S, Guimaraes M, Marcantonio E Jr (2013) Experimental development of bisphosphonate-related osteonecrosis of the jaws in rodents. Int J Exp Pathol 94:65–73
Otto S, Pautke C, Martin Jurado O, Nehrbass D, Stoddart MJ, Ehrenfeld M, Zeiter S (2017) Further development of the MRONJ minipig large animal model. J Craniomaxillofac Surg 45:1503–1514
Morita M, Iwasaki R, Sato Y, Kobayashi T, Watanabe R, Oike T, Nakamura S, Keneko Y, Miyamoto K, Ishihara K, Iwakura Y, Ishii K, Matsumoto M, Nakamura M, Kawana H, Nakagawa T, Miyamoto T (2017) Elevation of pro-inflammatory cytokine levels following anti-resorptive drug treatment is required for osteonecrosis development in infectious osteomyelitis. Sci Rep 7:46322
Oike T, Kanagawa H, Sato Y, Kobayashi T, Nakatsukasa H, Miyamoto K, Nakamura S, Kaneko Y, Kobayashi S, Harato K, Yoshimura A, Iwakura Y, Takeuchi T, Matsumoto M, Nakamura M, Niki Y, Miyamoto T (2018) IL-6, IL-17 and Stat3 are required for auto-inflammatory syndrome development in mouse. Sci Rep 8:15783
Mori T, Sato Y, Miyamoto K, Kobayashi T, Shimizu T, Kanagawa H, Katsuyama E, Fujie A, Hao W, Tando T, Iwasaki R, Kawana H, Morioka H, Matsumoto M, Saya H, Toyama Y, Miyamoto T (2014) TNFalpha promotes osteosarcoma progression by maintaining tumor cells in an undifferentiated state. Oncogene 33:4236–4241
Brunner JS, Vulliard L, Hofmann M, Kieler M, Lercher A et al (2020) Environmental arginine controls multinuclear giant cell metabolism and formation. Nat Commun 11:431
Gurt I, Artsi H, Cohen-Kfir E, Hamdani G, Ben-Shalom G, Feinstein B, El-Haj M, Dresner-Pollak R (2015) The Sirt1 activators SRT2183 and SRT3025 inhibit RANKL-induced osteoclastogenesis in bone marrow-derived macrophages and down-regulate Sirt3 in Sirt1 null cells. PLoS ONE 10:e0134391
Sato Y, Miyauchi Y, Yoshida S, Morita M, Kobayashi T, Kanagawa H, Katsuyama E, Fujie A, Hao W, Tando T, Watanabe R, Miyamoto K, Morioka H, Matsumoto M, Toyama Y, Miyamoto T (2014) The vitamin D analogue ED71 but Not 1,25(OH)2D3 targets HIF1α protein in osteoclasts. PLoS ONE 9:e111845–e111845
Katsuyama E, Miyamoto H, Kobayashi T, Sato Y, Hao W, Kanagawa H, Fujie A, Tando T, Watanabe R, Morita M, Miyamoto K, Niki Y, Morioka H, Matsumoto M, Toyama Y, Miyamoto T (2015) Interleukin-1 receptor-associated kinase-4 (IRAK4) promotes inflammatory osteolysis by activating osteoclasts and inhibiting formation of foreign body giant cells. J Biol Chem 290:716–726
Saad F, Gleason DM, Murray R, Tchekmedyian S, Venner P, Lacombe L, Chin JL, Vinholes JJ, Goas JA, Zheng M (2004) Long-term efficacy of zoledronic acid for the prevention of skeletal complications in patients with metastatic hormone-refractory prostate cancer. J Natl Cancer Inst 96:879–882
Rosen LS, Gordon DH, Dugan W Jr, Major P, Eisenberg PD, Provencher L, Kaminski M, Simeone J, Seaman J, Chen BL, Coleman RE (2004) Zoledronic acid is superior to pamidronate for the treatment of bone metastases in breast carcinoma patients with at least one osteolytic lesion. Cancer 100:36–43
Lipton A, Fizazi K, Stopeck AT, Henry DH, Brown JE, Yardley DA, Richardson GE, Siena S, Maroto P, Clemens M, Bilynskyy B, Charu V, Beuzeboc P, Rader M, Viniegra M, Saad F, Ke C, Braun A, Jun S (2012) Superiority of denosumab to zoledronic acid for prevention of skeletal-related events: a combined analysis of 3 pivotal, randomised, phase 3 trials. Eur J Cancer 48:3082–3092
Saad F, Brown JE, Van Poznak C, Ibrahim T, Stemmer SM, Stopeck AT, Diel IJ, Takahashi S, Shore N, Henry DH, Barrios CH, Facon T, Senecal F, Fizazi K, Zhou L, Daniels A, Carriere P, Dansey R (2012) Incidence, risk factors, and outcomes of osteonecrosis of the jaw: integrated analysis from three blinded active-controlled phase III trials in cancer patients with bone metastases. Ann Oncol 23:1341–1347
Khan AA, Morrison A, Hanley DA, Felsenberg D, McCauley LK et al (2015) Diagnosis and management of osteonecrosis of the jaw: a systematic review and international consensus. J Bone Miner Res 30:3–23
Allen MR (2009) Bisphosphonates and osteonecrosis of the jaw: moving from the bedside to the bench. Cells Tissues Organs 189:289–294
Cheung A, Seeman E (2010) Teriparatide therapy for alendronate-associated osteonecrosis of the jaw. N Engl J Med 363:2473–2474
Kwon YD, Lee DW, Choi BJ, Lee JW, Kim DY (2012) Short-term teriparatide therapy as an adjunctive modality for bisphosphonate-related osteonecrosis of the jaws. Osteoporos Int 23:2721–2725
Harper RP, Fung E (2007) Resolution of bisphosphonate-associated osteonecrosis of the mandible: possible application for intermittent low-dose parathyroid hormone [rhPTH(1-34)]. J Oral Maxillofac Surg 65:573–580
Miyamoto T, Ohneda O, Arai F, Iwamoto K, Okada S, Takagi K, Anderson DM, Suda T (2001) Bifurcation of osteoclasts and dendritic cells from common progenitors. Blood 98:2544–2554
Kassem A, Henning P, Lundberg P, Souza PP, Lindholm C, Lerner UH (2015) Porphyromonas gingivalis stimulates bone resorption by enhancing RANKL (receptor activator of NF-κB ligand) through activation of toll-like receptor 2 in osteoblasts. J Biol Chem 290:20147–20158
Kanagawa H, Niki Y, Kobayashi T, Sato Y, Katsuyama E, Fujie A, Hao W, Miyamoto K, Tando T, Watanabe R, Morita M, Morioka H, Matsumoto M, Toyama Y, Miyamoto T (2015) Mycobacterium tuberculosis promotes arthritis development through Toll-like receptor 2. J Bone Miner Metab 33:135–141
Miyamoto K, Yoshida S, Kawasumi M, Hashimoto K, Kimura T et al (2011) Osteoclasts are dispensable for hematopoietic stem cell maintenance and mobilization. J Exp Med 208:2175–2181
Kotian P, Boloor A, Sreenivasan S (2016) Study of adverse effect profile of parenteral zoledronic acid in female patients with osteoporosis. J Clin Diagn Res 10:04–06
Hewitt RE, Lissina A, Green AE, Slay ES, Price DA, Sewell AK (2005) The bisphosphonate acute phase response: rapid and copious production of proinflammatory cytokines by peripheral blood gd T cells in response to aminobisphosphonates is inhibited by statins. Clin Exp Immunol 139:101–111
Park W, Kim NK, Kim MY, Rhee YM, Kim HJ (2010) Osteonecrosis of the jaw induced by oral administration of bisphosphonates in Asian population: five cases. Osteoporos Int 21:527–533
Malden N, Beltes C, Lopes V (2009) Dental extractions and bisphosphonates: the assessment, consent and management, a proposed algorithm. Br Dent J 206:93–98
Fedele S, Porter SR, D’Aiuto F, Aljohani S, Vescovi P, Manfredi M, Arduino PG, Broccoletti R, Musciotto A, Di Fede O, Lazarovici TS, Campisi G, Yarom N (2010) Nonexposed variant of bisphosphonate-associated osteonecrosis of the jaw: a case series. Am J Med 123:1060–1064
Acknowledgements
T. Miyamoto was supported by a grant-in-aid for Scientific Research in Japan and a grant from the Japan Agency for Medical Research and Development. Y. Sato and K. Miyamoto were supported by a grant-in-aid for Scientific Research in Japan. This study was supported in part by Tei**.
Author information
Authors and Affiliations
Contributions
Investigation: TS, YS, and TK; conceptualization: TM; data curation: SN, YK, EI, HO, HW, and KM; funding acquisition: RI, YS, KM, and TM; supervision: RI, MM, MN, SA, HK, and TN; writing: TM.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest with the contents of this article.
Ethical approval
Animals were maintained under specific pathogen-free conditions in animal facilities certified by the Keio University Institutional Animal Care and Use Committee, and animal protocols were approved by that committee. All animal studies were performed in accordance with Institutional Guidelines on Animal Experimentation at Keio University of The Keio University Institutional Animal Care and Use Committee.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Soma, T., Iwasaki, R., Sato, Y. et al. Tooth extraction in mice administered zoledronate increases inflammatory cytokine levels and promotes osteonecrosis of the jaw. J Bone Miner Metab 39, 372–384 (2021). https://doi.org/10.1007/s00774-020-01174-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-020-01174-2