Abstract
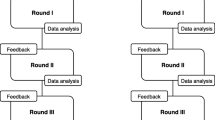
This study aimed to assess and develop consensus on the assessment of disordered eating in pregnancy. A three-round modified Delphi approach was used. Participants were international clinicians and researchers (N = 26) with extensive knowledge on and/or clinical experience with eating disorders, particularly in relation to pregnancy and/or women’s health. Clear consensus among the panel, defined as 75% agreement, was reached regarding the assessment of disordered eating in pregnancy, in addition to potential assessment methods. Antenatal assessment of disordered eating was perceived to be crucial and ideally occur in a routine manner. Despite agreement that various assessment methods would be relevant in assessing disordered eating in pregnancy, psychometrically sound brief screening instruments were perceived to be most feasible for practitioners and women accessing antenatal care; however, these instruments must be pregnancy-specific and delivered in an authentic and caring manner to be beneficial.
Similar content being viewed by others
References
Abraham S (2001) Obstetricians and maternal body weight and eating disorders during pregnancy. J Psychosom Obst Gyn 22(3):159–163. https://doi.org/10.3109/01674820109049968
Abraham S, King W, Llewellyn-Jones D (1994) Attitudes to body weight, weight gain and eating behavior in pregnancy. J Psychosom Obst Gyn 15(4):189–195. https://doi.org/10.3109/01674829409025645
Andersen AE, Ryan GL (2009) Eating disorders in the obstetric and gynecologic patient population. Obstet Gynecol 114(6):1353–1367. https://doi.org/10.1097/AOG.0b013e3181c070f9
Astrachan-Fletcher E, Veldhuis C, Lively N, Fowler C, Marcks B (2008) The reciprocal effects of eating disorders and the postpartum period: a review of the literature and recommendations for clinical care. J Women’s Health 17(2):227–239. https://doi.org/10.1089/jwh.2007.0550
Austin M-P, Highet N, the Guidelines Expert Advisory Committee (2011) Clinical practice guidelines for depression and related disorders – anxiety, bipolar disorder and puerperal psychosis – in the perinatal period. A guideline for primary care health professionals. beyondblue, Melbourne
Blais MA, Becker AE, Burwell RA, Flores AT, Nussbaum KM, Greenwood DN, Ekeblad ER, Herzog DB (2000) Pregnancy: outcome and impact on symptomatology in a cohort of eating-disordered women. Int J Eat Disord 27(2):140–149. https://doi.org/10.1002/(SICI)1098-108X(200003)
Broussard B (2012) Psychological and behavioural traits associated with eating disorders and pregnancy: a pilot study. J Midwifery Womens Health 57(1):61–66. https://doi.org/10.1111/j.1542-2011.2011.00089.x
Bulik CM, Von Holle A, Hamer R, Knoph Berg C, Torgersen L, Magnus P, Stoltenberg C, Siega-Riz AM, Sullivan P, Reichborn-Kjennerud T (2007) Patterns of remission, continuation and incidence of broadly defined eating disorders during early pregnancy in the Norwegian Mother and Child Cohort Study (MoBa). Psychol Med 37(08):1109–1118. https://doi.org/10.1017/S0033291707000724
Austin M-P, Highet N, the Expert Working Group (2017) Mental health care in the perinatal period: Australian clinical practice guideline. Centre of Perinatal Excellence, Melbourne.
Chizawsky LL, Newton MS (2006) Eating disorders: identification and treatment in obstetrical patients. Nurs Womens Health 10:482–488. https://doi.org/10.1111/j.1552-6356.2006.0097.x
Crow SJ, Agras WS, Crosby R, Halmi K, Mitchell JE (2008) Eating disorder symptoms in pregnancy: a prospective study. Int J Eat Disord 41(3):277–279. https://doi.org/10.1002/eat.20496
Diamond IR, Grant RC, Feldman BM, Pencharz PB, Ling SC, Moore AM, Wales PW (2014) Defining consensus: a systematic review recommends methodologic criteria for reporting Delphi studies. J Clin Epidemiol 67(4):401–409. https://doi.org/10.1016/j.jclinepi.2013.12.002
Easter A, Bye A, Taborelli E, Corfield F, Schmidt U, Treasure J, Micali N (2013) Recognising the symptoms: how common are eating disorders in pregnancy? Eur Eat Disord Rev 21(4):340–344. https://doi.org/10.1002/erc.2229
Fornari C, Dancyger I, Renz J, Skolnick R, Rochelson B (2014) Eating disorders and pregnancy: proposed treatment guidelines for obstetricians and gynecologists. Open J Obstet Gynecol 4(02):90–94. https://doi.org/10.4236/ojog.2014.42016
Franko DL, Spurrell EB (2000) Detection and management of eating disorders during pregnancy. Obstet Gynecol 95(6):942–946. https://doi.org/10.1016/S0029-7844(00)00792-4
Harris AA (2010) Prenatal advice for caring for women with eating disorders during the perinatal period. J Midwifery Womens Health 55(6):579–586. https://doi.org/10.1016/j.mwh.2010.07.008
Hasson F, Keeney S, McKenna H (2000) Research guidelines for the Delphi survey technique. J Adv Nurs 32(4):1008–1015. https://doi.org/10.1046/j.1365-2648.2000.01567.x
Hawkins LK, Gottlieb B (2013) Screening for eating disorders in pregnancy: how uniform screening during a high risk period could minimise under-recognition. J Women’s Health 22(4):390–392. https://doi.org/10.1089/jwh.2013.4313
Honikman S, van Heyningen T, Field S, Baron E, Tomlinson M (2012) Stepped care for maternal mental health: a case study of the perinatal mental health project in South Africa. PLoS Med 9(5):e1001222. https://doi.org/10.1371/journal.pmed.1001222
Hubin-Gayte M, Squires C (2012) Étude de l’impact de la grossesse sur les comportements alimentaires à travers l’utilisation du questionnaire SCOFF. Evol Psychiatr 77(2):201–212. https://doi.org/10.1016/j.evopsy.2012.01.002
Jorm AF (2015) Using the Delphi expert consensus method in mental health research. Aust N Z J Psychiatry 49(10):887–897. https://doi.org/10.1177/0004867415600891
Kingston D, Austin M-P, McDonald SW, Vermeyden L, Heaman M, Hegadoren K, Lasiuk G, Kingston J, Sword W, Jarema K, van Zanten V, McDonald SD, Biringer A (2015) Pregnant women’s perceptions of harms and benefits of mental health screening. PLoS One 10(12):145–189. https://doi.org/10.1371/journal.pone.0145189
Kotelchuck M (2010) Evaluating the healthy start program: a life course perspective. Matern Child Health J 14(5):649–653. https://doi.org/10.1007/s10995-010-0629-0
Koubaa S, Hallstrom T, Lindholm C, Hirschberg AL (2005) Pregnancy and neonatal outcomes in women with eating disorders. Obstet Gynecol 105(2):255–260. https://doi.org/10.1097/01.AOG.0000148265.90984.c3
Leddy MA, Jones C, Morgan MA, Schulkin J (2009) Eating disorders and obstetric-gynecologic care. J Women’s Health 18(9):1395–1401. https://doi.org/10.1089/jwh.2008.1183
Leung SSL, Leung C, Lam TH, Hung SF, Chan R, Yeung T, Miao M, Cheng S, Leung SH, Lau A, Lee DTS (2011) Outcome of a postnatal depression screening programme using the Edinburgh Postnatal Depression Scale: a randomized controlled trial. J Public Health 33(2):292–301. https://doi.org/10.1093/pubmed/fdq075
Linna MS, Raevuori A, Haukka J, Suvisaari JM, Suokas JT, Gissler M (2013) Reproductive health outcomes in eating disorders. Int J Eat Disord 46(8):826–833. https://doi.org/10.1002/eat.22179
Linstone HA, Turoff M (2002) Introduction. In: Linstone HA, Turoff M (eds) The Delphi method: techniques and applications. Addison-Wesley Publishing Company, Reading, pp 3–12
Lowes H, Kopeika J, Micali N, Ash A (2012) Anorexia nervosa in pregnancy. The Obstet Gynaecol 14(3):179–187. https://doi.org/10.1111/j.1744-4667.2012.00110.x
McFarlane L, Owens G, Del Pozo Cruz B (2016) Identifying the features of an exercise addiction: a Delphi study. J Behav Addict 5(3):474–484. https://doi.org/10.1556/2006.5.2016.060
McKenna H (1994) The Delphi technique: a worthwhile research approach for nursing? J Adv Nurs 19(6):1221–1225. https://doi.org/10.1111/j.1365-2648.1994.tb01207.x
Micali N, Treasure J (2009) Biological effects of maternal ED on pregnancy and foetal development: a review. Eur Eat Disord Rev 17(6):448–454. https://doi.org/10.1002/erv.963
Micali N, Treasure J, Simonoff E (2007) Eating disorders symptoms in pregnancy: a longitudinal study of women with recent and past eating disorders and obesity. J Psychosom Obst Gyn 63(3):297–303. https://doi.org/10.1016/j.jpsychores.2007.05.003
Mittnacht AM, Bulik CM (2015) Best nutrition counseling practices for the treatment of anorexia nervosa: a Delphi study. Int J Eat Disord 48(1):111–122. https://doi.org/10.1002/eat.22319
Morgan JF (1999) Eating disorders and gynecology: knowledge and attitudes among clinicians. Acta Obstet Gynecol Scand 78(3):233–239. https://doi.org/10.1080/k.1600-0412.1999.780311.x
Morgan JF, Reid F, Lacey JH (1999) The SCOFF questionnaire: assessment of a new screening tool for eating disorders. B Med J 319(7223):1467–1468. https://doi.org/10.1136/bmj.319.7223.1467
National Eating Disorders Collaboration (2015) Pregnancy and eating disorders: a professional’s guide to assessment and referral. NEDC, Crows Nest, NSW
National Institute for Health and Care Excellence (2016) Antenatal and postnatal mental health. NICE, Manchester
National Institute for Health and Care Excellence (2010) Weight management before, during, and after pregnancy. NICE, Manchester
National Institute for Health and Care Excellence (2017) Eating disorders: recognition and treatment. NICE, Manchester
Noetel M, Dawson L, Hay P, Touyz S (2017) The assessment and treatment of unhealthy exercise in adolescents with anorexia nervosa: a Delphi study to synthesize clinical knowledge. Int J Eat Disord 50(4):378–388. https://doi.org/10.1002/eat.22657
Patel P, Wheatcroft R, Park RJ, Stein A (2002) The children of mothers with eating disorders. Clin Child Fam Psychol Rev 5(1):1–19. https://doi.org/10.1023/A:1014524207660
Pettersson CB, Zandian M, Clinton D (2016) Eating disorder symptoms pre- and postpartum. Arch Womens Ment Health 19(4):675–680. https://doi.org/10.1007/s00737-016-0619-3
Reilly N, Harris S, Loxton D, Chojenta C, Forder P, Milgrom J, Austin M-P (2013) Referral for management of emotional health issues during the perinatal period: does mental health assessment make a difference? Birth 40(4):297–306. https://doi.org/10.1111/birt.12067
Reilly N, Harris S, Loxton D, Chojenta C, Forder P, Milgrom J, Austin M-P (2014) The impact of routine assessment of past or current mental health on help-seeking in the perinatal period. Women Birth 27(4):20–27. https://doi.org/10.1016/j.wombi.2014.07.003
Squires C, Lalanne C, Murday N, Simoglou V, Vaivre-Douret L (2015) The influence of eating disorders on mothers’ sensitivity and adaptation during feeding: A longitudinal observational study. BMC Pregnancy Childbirth 14:274-283. https://doi.org/10.1186/1471-2393-14-274
Ward VB (2008) Eating disorders in pregnancy. B Med J 336(7635):93–96. https://doi.org/10.1136/bmj.39393.689595.BE
Watson HJ, Torgersen L, Zerwas S, Reichborn-Kjennerud T, Knoph C, Stoltenberg C, Siega-Riz AM, Von Holle A et al (2014) Eating disorders, pregnancy, and the postpartum period: findings from the Norwegian Mother and Child Cohort Study (MoBa). Nor Epidemiol 24(1-2):51–62. https://doi.org/10.5324/nje.v24i1-2.1758
Wiles R (1994) I’m not fat, I’m pregnant. In: Wilkinson S, Kitzinger C (eds) Women and health: feminist perspectives. Taylor Francis, London, pp 33–48
Williams M, Haverkamp BE (2010) Identifying critical competencies for psychotherapeutic practice with eating disordered clients: a Delphi study. Eat Disord 18(2):91–109. https://doi.org/10.1080/10640260903585524
World Health Organisation (2009) Maternal mental health and child health and development in resource-constrained settings. Geneva, Switzerland WHO
World Health Organisation (2016) WHO recommendations on antenatal care for a positive pregnancy experience. Geneva, Switzerland WHO
Yawn BP, Dietrich AJ, Wollan P, Bertram S, Graham D, Huff J, Kurland M, Madison S, Pace WD, TRIPPD Practices (2012) TRIPPD: a practice-based network effectiveness study of postpartum depression screening and management. Ann Fam Med 10(4):320–329. https://doi.org/10.1370/afm.1418
Acknowledgements
The authors wish to express their sincerest gratitude to all the panel members who generously contributed their time and expertise to this study. The authors gratefully acknowledge the following panel members, who have consented to be recognised for their contributions: Ms. Jacqueline Byrne, Ms. Amanda Davis, Dr. Justine Ebenreuter, Dr. Melissa Freizinger, Dr. Christine Furber, Dr. Anthea Fursland, Ms. Kelly Gall, Dr. Marcia Herrin, Professor Angelica Lindén Hirschberg, Associate Professor Mimi Israël, Emeritus Professor Michael Levine, Ms. Shelly Read, Associate Professor Elizabeth Rieger, Professor Helen Skouteris, Dr. Stephanie Tierney, Ms. Natalie Watson, Associate Professor Jennifer Wildes and Associate Professor Stephanie Zerwas.
Funding
This research was supported by a Research Training Program Scholarship funded by the Australian Government.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Appendix
Appendix
Relevant Tables.
Rights and permissions
About this article
Cite this article
Bannatyne, A.J., Hughes, R., Stapleton, P. et al. Consensus on the assessment of disordered eating in pregnancy: an international Delphi study. Arch Womens Ment Health 21, 383–390 (2018). https://doi.org/10.1007/s00737-017-0806-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00737-017-0806-x