Abstract
Purpose
To perform a systematic review of the current level of evidence on post-operative management following brain metastasectomy (namely: adjuvant stereotactic radiosurgery, whole brain radiotherapy or observation), and to propose a GRADE-based dedicated recommendation to inform Radiation Oncologists’ clinical practice.
Methods
A panel of expert Radiation Oncologists from the Italian Association of Radiotherapy and Clinical Oncology had defined the search question per the PICO methodology. Electronic databases were independently screened; the Preferred Reporting Items for Systematic Reviews and Meta-Analyses was adopted. The individual and pooled hazard ratios with 95% confidence intervals (CI), as well as the pooled risk ratio (RR) were calculated using a fixed- or random-effects model.
Results
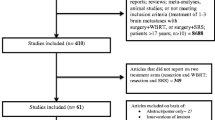
Eight full-texts were retrieved: six retrospective studies and two randomized clinical trials. Outcomes of benefit and damage were analyzed for SRS + observation (PICO A) and SRS + WBRT. SRS allowed for increased rates of local control when compared to both observation and WBRT, while evidence was less conclusive for distant brain control, leptomeningeal disease control and overall survival. In the SRS, the incidence of severe radionecrosis was higher as compared to WBRT, despite neurocognitive deterioration rates were lower. Overall, SRS seems to favorably compare with observation and whole brain RT, despite the level of evidence for the recommendation was low and very low, respectively.
Conclusion
Despite low level of evidence, the panel concluded that the risk/benefit ratio probably favors adjuvant SRS as compared to the observation and whole brain RT as adjuvant treatments following brain metastasectomy (5 votes/5 participants, 100% attendance).



Similar content being viewed by others
References
Andrews J, Guyatt G, Oxman AD, Alderson P, Dahm P, Falck-Ytter Y et al (2013) GRADE guidelines: 14. Going from evidence to recommendations: the significance and presentation of recommendations. J Clin Epidemiol 66:719–725. https://doi.org/10.1016/j.jclinepi.2012.03.013
Brown PD, Jaeckle K, Ballman KV, Farace E, Cerhan JH, Anderson SK et al (2016) Effect of radiosurgery alone vs radiosurgery with whole brain radiation therapy on cognitive function in patients with 1 to 3 brain metastases: a randomized clinical trial. JAMA 316:401. https://doi.org/10.1001/jama.2016.9839
Chang EL, Wefel JS, Hess KR, Allen PK, Lang FF, Kornguth DG et al (2009) Neurocognition in patients with brain metastases treated with radiosurgery or radiosurgery plus whole-brain irradiation: a randomised controlled trial. Lancet Oncol 10:1037–1044. https://doi.org/10.1016/S1470-2045(09)70263-3
Chung SY, Chang JH, Kim HR, Cho BC, Lee CG, Suh C-O (2017) Optimal dose and volume for postoperative radiotherapy in brain oligometastases from lung cancer: a retrospective study. Radiat Oncol J 35:153–162. https://doi.org/10.3857/roj.2017.00094
Gaspar L, Scott C, Rotman M, Asbell S, Phillips T, Wasserman T et al (1997) Recursive partitioning analysis (RPA) of prognostic factors in three radiation therapy oncology group (RTOG) brain metastases trials. Int J Radiat Oncol 37:745–751. https://doi.org/10.1016/S0360-3016(96)00619-0
Hwang SW, Abozed MM, Hale A, Eisenberg RL, Dvorak T, Yao K et al (2010) Adjuvant Gamma Knife radiosurgery following surgical resection of brain metastases: a 9-year retrospective cohort study. J Neurooncol 98:77–82. https://doi.org/10.1007/s11060-009-0051-x
Kępka L, Tyc-Szczepaniak D, Bujko K, Olszyna-Serementa M, Michalski W, Sprawka A et al (2016) Stereotactic radiotherapy of the tumor bed compared to whole brain radiotherapy after surgery of single brain metastasis: results from a randomized trial. Radiother Oncol 121:217–224. https://doi.org/10.1016/j.radonc.2016.10.005
Kepka L, Tyc-Szczepaniak D, Osowiecka K, Sprawka A, Trąbska-Kluch B, Czeremszynska B (2018) Quality of life after whole brain radiotherapy compared with radiosurgery of the tumor bed: results from a randomized trial. Clin Transl Oncol 20:150–159. https://doi.org/10.1007/s12094-017-1703-5
Lee C-H, Kim DG, Kim JW, Han JH, Kim YH, Park C-K et al (2013) The role of surgical resection in the management of brain metastasis: a 17-years longitudinal study. Acta Neurochir (Wien) 155:389–397. https://doi.org/10.1007/s00701-013-1619-y
Ling DC, Vargo JA, Wegner RE, Flickinger JC, Burton SA, Engh J et al (2015) Postoperative stereotactic radiosurgery to the resection cavity for large brain metastases. Neurosurgery 76:150–157. https://doi.org/10.1227/NEU.0000000000000584
Mahajan A, Ahmed S, McAleer MF, Weinberg JS, Li J, Brown P et al (2017) Post-operative stereotactic radiosurgery versus observation for completely resected brain metastases: a single-centre, randomised, controlled, phase 3 trial. Lancet Oncol 18:1040–1048. https://doi.org/10.1016/S1470-2045(17)30414-X
McPherson CM, Suki D, Feiz-Erfan I, Mahajan A, Chang E, Sawaya R et al (2010) Adjuvant whole-brain radiation therapy after surgical resection of single brain metastases. Neuro-Oncol 12:711–719. https://doi.org/10.1093/neuonc/noq005
Minniti G, Esposito V, Clarke E, Scaringi C, Lanzetta G, Salvati M et al (2013) Multidose stereotactic radiosurgery (9 Gy × 3) of the postoperative resection cavity for treatment of large brain metastases. Int J Radiat Oncol 86:623–629. https://doi.org/10.1016/j.ijrobp.2013.03.037
Owonikoko TK, Arbiser J, Zelnak A, Shu H-KG, Shim H, Robin AM et al (2014) Current approaches to the treatment of metastatic brain tumours. Nat Rev Clin Oncol 11:203–222
Patchell RA, Tibbs PA, Walsh JW, Dempsey RJ, Maruyama Y, Kryscio RJ et al (1990) A randomized trial of surgery in the treatment of single metastases to the brain. N Engl J Med 322:494–500. https://doi.org/10.1056/NEJM199002223220802
Patel KR, Prabhu RS, Kandula S, Oliver DE, Kim S, Hadjipanayis C et al (2014) Intracranial control and radiographic changes with adjuvant radiation therapy for resected brain metastases: whole brain radiotherapy versus stereotactic radiosurgery alone. J Neurooncol 120:657–663. https://doi.org/10.1007/s11060-014-1601-4
Santos CMC, Pimenta CAM, Nobre MRC (2007) The PICO strategy for the research question construction and evidence search. Rev Lat Am Enfermagem 15:508–511. https://doi.org/10.1590/S0104-11692007000300023
Scheitler-Ring K, Ge B, Petroski G, Biedermann G, Litofsky NS (2016) Radiosurgery to the postoperative tumor bed for metastatic carcinoma vs. whole brain radiation after surgery. Cureus. https://doi.org/10.7759/cureus.885
Soffietti R, Abacioglu U, Baumert B, Combs SE, Kinhult S, Kros JM et al (2017) Diagnosis and treatment of brain metastases from solid tumors: guidelines from the European Association of Neuro-Oncology (EANO). Neuro-Oncol 19:162–174. https://doi.org/10.1093/neuonc/now241
Sperduto PW, Chao ST, Sneed PK, Luo X, Suh J, Roberge D et al (2010) Diagnosis-specific prognostic factors, indexes, and treatment outcomes for patients with newly diagnosed brain metastases: a multi-institutional analysis of 4259 patients. Int J Radiat Oncol 77:655–661. https://doi.org/10.1016/j.ijrobp.2009.08.025
Vecht CJ, Haaxma-Reiche H, Noordijk EM, Padberg GW, Voormolen JHC, Hoekstra FH et al (1993) Treatment of single brain metastasis: radiotherapy alone or combined with neurosurgery. Ann Neurol 33:583–590. https://doi.org/10.1002/ana.410330605
Vuong DA, Rades D, van Eck ATC, Horstmann GA, Busse R (2013) Comparing the cost-effectiveness of two brain metastasis treatment modalities from a payer’s perspective: Stereotactic radiosurgery versus surgical resection. Clin Neurol Neurosurg 115:276–284. https://doi.org/10.1016/j.clineuro.2012.05.005
Acknowledgements
The authors would like to jointly thank the Scientific Committee and the Board of AIRO for the critical revision of the paper. Stefania Volpe was partially supported by the Italian Ministry of Health with “Progetto di Eccellenza”. Stefania Volpe MD is a Ph.D. student within the European School of Molecular Medicine (SEMM).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author have no conflict/competing interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Reverberi, C., Volpe, S., Balestrini, D. et al. Post-operative management of brain metastases: GRADE-based clinical practice recommendations on behalf of the Italian Association of Radiotherapy and Clinical Oncology (AIRO). J Cancer Res Clin Oncol 147, 793–802 (2021). https://doi.org/10.1007/s00432-021-03515-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-021-03515-8