Abstract
Purpose
This study aimed at investigating the prognostic value of Preoperative controlling nutritional status (CONUT) score in non-metastatic clear-cell renal cell carcinoma of ≤ 7 cm on preoperative imaging.
Methods
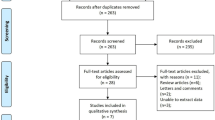
We retrospectively included 1046 among 1637 patients who underwent radical or partial nephrectomy for solid renal masses ≤ 7 cm (2005–2014) after excluding other pathology, conditions affecting CONUT score components, metastasis, regional lymphadenopathy, positive margin, and follow-up < 12 months. We defined high and low CONUT according to cut-off of (2). Multivariate Cox-regression analysis was used to predict factors affecting recurrence and survival. Kaplan–Meier curve was used for survival analysis.
Results
The median age and follow-up were 56 years and 63 months, respectively. 41 patients had recurrence (3.9%). CONUT was a predictor for recurrence-free, cancer-specific, and overall survival (HR 3.09, P = 0.003 and HR 4.66, P = 0.004 and HR 2.81, P = 0.003, respectively). A higher CONUT was significantly associated with worse 5 years recurrence-free (88.2% vs. 97.1%), cancer-specific (96.2% vs. 98.8%) and overall (90.9% vs. 96.5%) survival (log-rank, P = < 0.001, P = 0.006 and P = < 0.001, respectively).
Conclusions
The preoperative CONUT is an independent prognostic marker for survival after curative surgery for non-metastatic clear-cell renal cell carcinoma of ≤ 7 cm on preoperative imaging.


Similar content being viewed by others
References
Arends J et al (2017) ESPEN guidelines on nutrition in cancer patients. Clin Nutr 36(1):11–48. https://doi.org/10.1016/j.clnu.2016.07.015
Cengiz O, Kocer B, Sürmeli S, Santicky MJ, Soran A (2006) Are pretreatment serum albumin and cholesterol levels prognostic tools in patients with colorectal carcinoma? Med Sci Monit 12(6):CR240–C247
Edge SB, Compton CC (2010) The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncol 17:1471–1474. https://doi.org/10.1245/s10434-010-0985-4
Fuhrman SA, Lasky LC, Limas C (1982) Prognostic significance of morphologic parameters in renal cell carcinoma. Am J Surg Pathol 6:655–663
Ignacio de Ulíbarri J et al (2005) CONUT: a tool for controlling nutritional status. First validation in a hospital population. Nutr Hosp 20:38–45
Iseki Y et al (2015) Impact of the preoperative controlling nutritional status (CONUT) score on the survival after curative surgery for colorectal cancer. PLoS one 10:e0132488. https://doi.org/10.1371/journal.pone.0132488
Ishihara H, Kondo T, Omae K, Takagi T, Iizuka J, Kobayashi H, Tanabe K (2016) Sarcopenia and the modified Glasgow prognostic score are significant predictors of survival among patients with metastatic renal cell carcinoma who are receiving first-line sunitinib treatment. Target Oncol 11(5):605–617. https://doi.org/10.1007/s11523-016-0430-0
Ishihara H, Kondo T, Yoshida K, Omae K, Takagi T, Iizuka J, Tanabe K (2017) Preoperative Controlling Nutritional Status (CONUT) score as a novel predictive biomarker of survival in patients with localized urothelial carcinoma of the upper urinary tract treated with radical nephroureterectomy. Urol Oncol 35(9):539.e9–539.e16. https://doi.org/10.1016/j.urolonc.2017.04.012
Jeon HG et al (2016) Preoperative Prognostic Nutritional Index is a significant predictor of survival in renal cell carcinoma patients undergoing nephrectomy. Ann Surg Oncol 23(1):321–327. https://doi.org/10.1245/s10434-015-4614-0
Kang HW et al (2018) Low preoperative serum cholesterol level is associated with aggressive pathologic features and poor cancer-specific survival in patients with surgically treated renal cell carcinoma. Int J Clin Oncol 23(1):142–150. https://doi.org/10.1007/s10147-017-1172-4
Karl A, Rittler P, Buchner A, Fradet V, Speer R, Walther S, Stief GC (2009) Prospective assessment of malnutrition in urologic patients. Urology 73:1072–1076. https://doi.org/10.1016/j.urology.2008.12.037
Kim HL, Han KR, Zisman A, Figlin RA, Belldegrun AS (2004) Cachexia-like symptoms predict a worse prognosis in localized T1 renal cell carcinoma. J Urol 171:1810–1813. https://doi.org/10.1097/01.ju.0000121440.82581.d3
Ko K, Park YH, Lee JW, Ku JH, Kwak C, Kim HH (2013) Influence of nutritional deficiency on prognosis of renal cell carcinoma (RCC). BJU Int 112(6):775–780. https://doi.org/10.1111/bju.12275
Kunimura A et al (2017) Impact of nutritional assessment and Body Mass Index on cardiovascular outcomes in patients with stable coronary artery disease. Int J Cardiol 230:653–658. https://doi.org/10.1016/j.ijcard.2017.01.008
Kutikov A, Egleston BL, Wong YN, Uzzo RG (2010) Evaluating overall survival and competing risks of death in patients with localized renal cell carcinoma using a comprehensive nomogram. J Clin Oncol 28:311–317. https://doi.org/10.1200/JCO.2009.22.4816
Liang RF, Li JH, Li M, Yang Y, Liu YH (2017) The prognostic role of controlling nutritional status scores in patients with solid tumors. Clin Chim Acta 474:155–158. https://doi.org/10.1016/j.cca.2017.09.021
Linehan WM, Ricketts CJ (2013) The metabolic basis of kidney cancer. Semin Cancer Biol 3(1):46–55. https://doi.org/10.1016/j.semcancer.2012.06.002
Lipschitz DA (1988) Protein-energy malnutrition. Hosp Pract (Off Ed) 23:87–99. https://doi.org/10.1080/21548331.1988.11703582
Llop JM et al (2001) Serum albumin as indicator of clinical evolution in patients on parenteral nutrition. Multivar Study Clin Nutr 20:77–81. https://doi.org/10.1054/clnu.2000.0159
Lucca I, de Martino M, Hofbauer SL, Zamani N, Shariat SF, Klatte T (2015) Comparison of the prognostic value of pretreatment measurements of systemic inflammatory response in patients undergoing curative resection of clear cell renal cell carcinoma. World J Urol 33(12):2045–2052. https://doi.org/10.1007/s00345-015-1559-7
Mantovani A, Allavena P, Sica A, Balkwill F (2008) Cancer-related inflammation. Nature 454:436–444. https://doi.org/10.1038/nature07205
Mimatsu K, Fukino N, Ogasawara Y, Saino Y, Oida T (2017) Utility of inflammatory marker- and nutritional status-based prognostic factors for predicting the prognosis of stage IV gastric cancer patients undergoing non-curative surgery. Anticancer Res 37:4215–4222. https://doi.org/10.21873/anticanres.11812
Morgan T et al (2011) Preoperative nutritional status is an important predictor of survival in patients undergoing surgery for renal cell carcinoma. Eur Urol 59:923–928. https://doi.org/10.1016/j.eururo.2011.01.034
Park YH, Baik KD, Lee YJ, Ku JH, Kim HH, Kwak C (2012) Late recurrence of renal cell carcinoma> 5 years after surgery: clinicopathological characteristics and prognosis. BJU Int 110:E553. https://doi.org/10.1111/j.1464-410X.2012.11246.x
Prado CM, Wells JC, Smith SR, Stephan BC, Siervo M (2012) Sarcopenic obesity: acritical appraisal of the current evidence. Clin Nutr 31:583–601. https://doi.org/10.1016/j.clnu.2012.06.010
Saroha S, Uzzo RG, Plimack ER, Ruth K, Al-Saleem T (2013) Lymphopenia is an independent predictor of inferior outcome in clear cell renal carcinoma. J Urol 189:454–461. https://doi.org/10.1016/j.juro.2012.09.166
Shoji F et al (2017) The preoperative controlling nutritional status score predicts survival after curative surgery in patients with pathological stage I non-small cell lung cancer. Anticancer Res 37(2):741–747. https://doi.org/10.21873/anticanres.11372
Shuch B et al (2015) Understanding pathologic variants of renal cell carcinoma: distilling therapeutic opportunities from biologic complexity. Eur Urol 97:67–85. https://doi.org/10.1016/j.eururo.2014.04.029
Takamori S et al (2017) The controlling nutritional status score is a significant independent predictor of poor prognosis in patients with malignant pleural mesothelioma. Clin Lung Cancer 18:e303–e313. https://doi.org/10.1016/j.cllc.2017.01.008
Toyokawa T et al (2016) The pretreatment controlling nutritional status (CONUT) score is an independent prognostic factor in patients with resectable thoracic esophageal squamous cell carcinoma: results from a retrospective study. BMC Cancer 16(1):722. https://doi.org/10.1186/s12885-016-2696-0
Acknowledgements
This research was supported by a grant of the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), funded by the Ministry of Health & Welfare, Republic of Korea (grant number: HI17C1095).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflict exists.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was not required for the purposes of this study, as the study was based on retrospective anonymous patient data and did not involve patient intervention or the use of human tissue samples.
Additional information
Elghiaty A, Ham WS. Preoperative Controlling Nutritional Status (CONUT) Score as a Novel Immune-Nutritional Predictor of Survival Among Patients with Non-Metastatic Clear Cell Renal Cell Carcinoma of ≤ 7 cm on Preoperative Imaging [abstract]. In: Proceedings of the 38th annual congress of the Société Internationale d’Urologie; 2018 Oct 4–7; Seoul, South Korea.
Rights and permissions
About this article
Cite this article
Elghiaty, A., Kim, J., Jang, W.S. et al. Preoperative controlling nutritional status (CONUT) score as a novel immune-nutritional predictor of survival in non-metastatic clear cell renal cell carcinoma of ≤ 7 cm on preoperative imaging. J Cancer Res Clin Oncol 145, 957–965 (2019). https://doi.org/10.1007/s00432-019-02846-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-019-02846-x