Abstract
Purpose
Monitoring circulating endothelial cells (CECs) count reflects the tumor vasculature in cancer patients and might be a predictor of response to chemotherapy. We therefore investigated the clinical significance of changes in CECs count after three cycles of platinum-based chemotherapy in patients with advanced non-small cell lung cancer (NSCLC).
Methods
Peripheral blood samples were collected from 89 naive NSCLC patients at diagnosis and after chemotherapy. The CECs were quantified by an immuno-magnetic technique and fluorescent microscopy. After chemotherapy, patients were assessed according to the response evaluation criteria in solid tumors as partial response (PR), stable disease (SD) or progression disease (PD).
Results
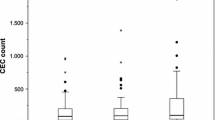
Baseline CECs levels were significantly higher in PR patients (n = 62) than those in patients with SD/PD (n = 27) (p = 0.0007). Although there was no significant correlation between baseline CECs levels and progression-free survival (PFS) (p = 0.287), patients with high percentage change in CECs count after chemotherapy had significantly longer PFS than those with low percentage change (p = 0.048). Regarding treatment efficacy, CECs count significantly decreased after chemotherapy in comparison with CECs count at baseline in patients with PR (p < 0.0001). By contrast, CECs levels after chemotherapy were significantly higher than those at diagnosis in patients with PD (p = 0.002). Moreover, there was no significant change between pre- and post-treatment CECs amount in patients with SD (p = 0.681).
Conclusions
Baseline CECs levels might be an early predictive biomarker for treatment efficacy in advanced NSCLC patients. Our results suggest the change in CECs count after chemotherapy as a prognostic factor for tumor response and PFS in NSCLC.






Similar content being viewed by others
References
Beerpoot LV, Mehra N, Vermaat JS, Zonnenberg BA, Gebbink MFBG, Voest EE (2004) Increased levels of viable circulating endothelial cells are an indicator of progressive disease in cancer patients. Ann Oncol 15(1):139–145
Bidard FC, Mathiot C, Degeorges A, Etienne-Grimaldi MC, Delva R, Pivot X, Veyret C, Bergougnoux L, de Cremoux P, Milano G, Pierga JY (2010) Clinical value of circulating endothelial cells and circulating tumoral cells in metastatic breast cancer patients treated first line with bevacizumab and chemotherapy. Ann Oncol 21(9):1765–1771
Calleri A, Bono A, Bangardi V, Quarna J, Mancuso P, Rabascio C, Dellapasqua S, Campagnoli E, Shaked Y, Goldhirsch A, Colleoni M, Bertolini F (2009) Predictive Potential of angiogenic growth factor and circulating endothelial cells in breast cancer patients receiving metronomic chemotherapy plus bevacizumab. Clin Cancer Res 15(24):7652–7657
Erdbruegger U, Dhaygude A, Haubitz M, Woywoodt A (2010) Circulating endothelial cells: markers and mediators of vascular damage. Curr Stem Cell Res Ther 5(4):294–302
Fleitas T, Martinez-Sales V, Vila V, Reganon E, Mesado D, Martin M, Gomez-Codina J, Motalar J, Reynes G (2012) Circulating endothelial cells and microparticles as prognostic markers in advanced non-small cell lung cancer. PLoS ONE 7(10):e47365. doi:10.1371/journalpone0047365
Goldstraw P, Crowley J, Chansky K, Giroux DJ, Groome PA, Rami-Porta R, Postmus PE, Rusch V, Sobin L (2007) The IASLC lung cancer staging project: proposal for the revision of the TNM stage grou**s in the forthcoming (seventh) of the TNM classification of malignant tumors. J Thorac Oncol 2(8):706–714
Huang C, Li K, Wei XY, Niu RF, Sun Y, Wang JW, Zhu YZ, Xu LY, Liu XQ, Gao HJ, Zhou JM, Wang XW (2006) Circulating endothelial cells in the peripheral blood of advanced NSCLC patients. Zhonghua Zhong Liu Za Zhi 28(10):780–783
Ilie M, Long E, Hofman V, Selva E, Bonnetaud C, Boyer J, Venissac N, Sanfiorenzo C, Ferrua B, Marquette C-H, Moroux J, Hofman P (2014) Clinical value of circulating endothelial cells and of soluble CD146 levels in patients undergoing surgery for non-small cell lung cancer. Br J Cancer 110(5):1236–1243
Johnson DH, Fehrenbacher L, Novotny WF, Herbst RS, Nemunaitis JJ, Jablons DM, Langer CJ, DeVore RF 3rd, Gaudreault J, Damico LA, Holmgren E, Kabbinavar F (2004) Randomized phase II trial comparing bevacizumab plus carboplatin and paclitaxel with carboplatin and paclitaxel alone in previously untreated locally advanced or metastatic non-small cell lung cancer. J Clin Oncol 22:2184–2191
Kawaishi M, Fujiwara Y, Fukui T, Kato T, Yamada K, Ohe Y, Kunitoh H, Sekine I, Yamamoto N, Nokihara H, Watabe T, Shimoda Y, Arao T, Nishio K, Tamura T, Koizumi F (2009) Circulating endothelial cells in non-small cell lung cancer patients treated with carboplatin and paclitaxel. J Thorac Oncol 4(2):208–213
Kraan J, Sleijfer S, Foekans JA, Gratama JW (2012) Clinical value of circulating endothelial cell detection in oncology. Drug Discov Today 17(13–14):710–717
Malka D, Boige V, Jacques N, Vimond N, Adenis A, Boucher E, Pierga JY, Conroy T, Chauffert B, Francois E, Guichard P, Galais MP, Cvitkovic F, Ducreux M, Farace F (2012) Clinical value of circulating endothelial cell levels in metastatic colorectal cancer patients treated with first-line chemotherapy and bevacizumab. Ann Oncol 23(4):919–927
Mancuso P, Burlini A, Pruneri G, Goldhirsch A, Martinelli G, Bertolini F (2001) Resting and activated endothelial cells are increased in the peripheral blood of cancer patients. Blood 97(11):3658–3661
Mancuso P, Colleoni M, Calleri A, Orlando L, Maisonneuve P, Pruneri G, Agliano A, Goldhirsch A, Shaked Y, Kerbel RS, Bertolini F (2006) Circulating endothelial cells kinetics and viability predict survival in breast cancer patients receiving metronomic chemotherapy. Blood 108(2):452–459
Ronzoni M, Manzoni M, Mariucci S, Loupakis F, Brugnatelli S, Bencardino K, Rovati B, Tinelli C, Falcone A, Villa E, Danova M (2010) Circulating endothelial cells and endothelial progenitors as predictive marker of clinical response to bevacizumab-based first-line treatment in advanced colorectal cancer patients. Ann Oncol 21(12):2382–2389
Roodhart JM, Langenberg MH, Vermaat JS, Lolkema MP, Baars A, Giles RH, Witteveen EO, Voest EE (2010) Late release of circulating endothelial cells and endothelial progenitor cells after chemotherapy predicts response and survival in cancer patients. Neoplasia 12(1):87–94
Rowand JL, Martin G, Doyle GV, Miller MC, Pierce MS, Connelly MC, Rao C, Terstappen LW (2007) Endothelial cells in the peripheral blood of healthy subject and patients with metastatic carcinomas. Cytometry A 71(2):105–113
Scagliotti GV, Parikh P, von Pawel J, Biesma B, Vansteenkiste J, Manegold C, Serwatowski P, Gatzemeier U, Digumarti R, Zukin M, Lee JS, Mellemgaard A, Park K, Patil S, Rolski J, Goksel T, de Marinis F, Simms L, Sugarman KP, Gandara D (2008) Phase III study comparing cisplatin plus gemcitabin with cisplatin plus pemertrexed in chemotherapy-naïve patients with advanced stage non-small cell lung cancer. J Clin Oncol 26(21):3543–3551
Schiller JH, Harrington D, Belani C, Langer C, Sandler A, Krook J, Zhu J, Johnson DH (2002) Comparison of four chemotherapy regimens for advanced non-small cell lung cancer. N Engl J Med 346:92–98
Simkens LH, Tol J, Terstappen LW, Teerenstra S, Punt CJ, Nagtegaal ID (2010) The predictive and prognostic value of circulating endothelial cells in advanced colorectal cancer patients receiving first-line chemotherapy and bevacizumab. Ann Oncol 21:1765–1771
Spiro SG, Silvestri GA (2005) One hundred years of lung cancer. Am J Respir Crit Care Med 172(5):523–529
Therasse P, Arbuck SG, Eisenhauer EA, Wanders J, Kaplan RS, Rubinstein L, Verweij J, Van Glabbeke M, van Oosterom AT, Christian MC, Gwyther SG (2000) New guidelines to evaluate the response to treatment in solid tumors (RECIST Guidelines). J Natl Cancer Inst 92(3):205–216
Timar J, Dome B, Fazekas K, Janovics A, Paku S (2001) Angiogenesis-dependant diseases and angiogenesis therapy. Pathol Oncol Res 7(2):85–94
Torrisi R, Bagnardi V, Cardillo A, Bertolini F, Scarano E, Orlando L, Mancuso P, Luini A, Calleri A, Vial G, Goldhirsch A, Colleoni M (2008) Preoperative bevacizumab combined with letrozole and chemotherapy in locally advanced ER- and/or PgR-positive breast cancer: clinical and biological activity. Br J Cancer 99(10):1564–1571
Tufman A, Huber RM (2010) Biological markers in lung cancer: a clinician’s perspective. Cancer Biomark 6(3–4):123–135
Wang J, Lou P, Lesniewski R, Henkin J (2003) Paclitaxel at ultra low concentrations inhibits angiogenesis without affecting cellular microtubule assembly. Anticancer Drugs 14(1):13–19
Wang J, Huang C, Wei X, Qi D, Gong L, Mu H, Yao Q, Kai L (2008) Changes of activated circulating endothelial cells and surviving in patients with non-small cell lung cancer after antiangiogenesis therapy. Chin Med J 121(22):2234–2240
Wang J, **ao J, Wei X, Wang L, Lin L, Liu Z, Wang X, Sun B, Li K (2013) Circulating endothelial cells and tumour blood volume as predictors in lung cancer. Cancer Sci 104(4):445–452
Weis SM, Cheresh DA (2011) Tumour angiogenesis: molecular pathway and therapeutic targets. Nat Med 17(11):1359–1370
Woywodt A, Goldberg C, Scheer J, Regelsberger H, Haller H, Haubitz M (2004) An improved assay for enumeration of circulating endothelial cells. Ann Hematol 83(8):491–494
Woywodt A, Blann AD, Kirsch T, Erdbruegcer U, Banzet N, Haubitz M, Dignat-George F (2005) Isolation and enumeration of circulating endothelial cells by immunomagnetic isolation: proposal of a definition and a consensus protocol. J Thromb Haemost 4(3):671–677
Acknowledgments
The preliminary results of this study were in part presented at the 38th meeting of European cancer congress (Amsterdam, The Netherland, September 27, 2013). The first author would like to thank Pr. I Othman, Director General of AECS, for his cooperation in this project. The authors also thank Ms. Israa Banat for technical assistance and Mr. Ali Mohammad for his aide in statistical analyses.
Conflict of interest
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Najjar, F., Alammar, M., Bachour, M. et al. Predictive and prognostic value of circulating endothelial cells in non-small cell lung cancer patients treated with standard chemotherapy. J Cancer Res Clin Oncol 141, 119–125 (2015). https://doi.org/10.1007/s00432-014-1778-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-014-1778-0