Abstract
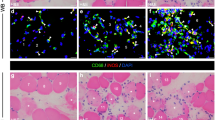
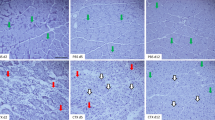
Following skeletal muscle injury, both myogenic and immune cells interact closely during the regenerative process. Although icing is still a common acute treatment for sports-related skeletal muscle injuries, icing after muscle injury has been shown to disrupt macrophage accumulation and impair muscle regeneration in animal models. However, it remains unknown whether icing shortly after injury affects macrophage-related phenomena during the early stages of muscle regeneration. Therefore, we focused on the distribution of M1/M2 macrophages and cytokines expressed predominantly by macrophages during the early stages of muscle regeneration after muscle crush injury. Icing resulted in a decrease, not retardation, in the accumulation of M1 macrophages, but not M2 macrophages, in injured muscles. Consistent with the decrease in M1 macrophage accumulation, icing led to a reduction, instead of delay, in the level of tumor necrosis factor-α (TNF-α) expression. Additionally, at subsequent timepoints, icing decreased the number of myogenic precursor cells in the regenerating area and the size of centrally nucleated regenerating myofibers. Together, our findings suggest that icing after acute muscle damage by crushing disturbs muscle regeneration through hindering tM1 macrophage-related phenomena.








Similar content being viewed by others
Data availability
The datasets analyzed during the current study are available from the corresponding author on reasonable request.
References
Arnold L, Henry A, Poron F et al (2007) Inflammatory monocytes recruited after skeletal muscle injury switch into antiinflammatory macrophages to support myogenesis. J Exp Med 204:1057–1069. https://doi.org/10.1084/jem.20070075
Bencze M, Negroni E, Vallese D et al (2012) Proinflammatory macrophages enhance the regenerative capacity of human myoblasts by modifying their kinetics of proliferation and differentiation. Mol Ther 20:2168–2179. https://doi.org/10.1038/mt.2012.189
Bleakley C, McDonough S, MacAuley D (2004) The use of ice in the treatment of acute soft-tissue injury: a systematic review of randomized controlled trials. Am J Sports Med 32:251–261. https://doi.org/10.1177/0363546503260757
Cassatella MA (1999) Neutrophil-derived proteins: selling cytokines by the pound. Adv Immunol 73:369–509. https://doi.org/10.1016/s0065-2776(08)60791-9
Chazaud B (2020) Inflammation and skeletal muscle regeneration: leave it to the macrophages! Trends Immunol 41:481–492. https://doi.org/10.1016/j.it.2020.04.006
Chen S, ** B, Li Y (2007) TNF-α regulates myogenesis and muscle regeneration by activating p38 MAPK. Am J Physiol Cell Physiol 292:1660–1671. https://doi.org/10.1152/ajpcell.00486.2006
Collins RA, Grounds MD (2001) The role of tumor necrosis factor-alpha (TNF-α) in skeletal muscle regeneration: studies in TNF-α (−/−) and TNF-α (−/−)/LT-α(−/−) mice. J Histochem Cytochem 49:989–1001. https://doi.org/10.1177/002215540104900807
Fan Y, Hao Y, Gao D et al (2021) Phenotype and function of macrophage polarization in monocrotaline-induced pulmonary arterial hypertension rat model. Physiol Res 70:213–226. https://doi.org/10.33549/physiolres.934456
Freitas LS, Freitas TP, Silveira PC et al (2007) Effect of therapeutic pulsed ultrasound on parameters of oxidative stress in skeletal muscle after injury. Cell Biol Int 31:482–488. https://doi.org/10.1016/j.cellbi.2006.11.015
Fujita N, Ono M, Tomioka T et al (2014) Effects of hyperbaric oxygen at 1.25 atmospheres absolute with normal air on macrophage number and infiltration during rat skeletal muscle regeneration. PLoS One 9:e115685. https://doi.org/10.1371/journal.pone.0115685
Goetsch SC, Hawke TJ, Gallardo TD et al (2003) Transcriptional profiling and regulation of the extracellular matrix during muscle regeneration. Physiol Genomics 14:261–271. https://doi.org/10.1152/physiolgenomics.00056.2003
Hatade T, Takeuchi K, Fujita N et al (2014) Effect of heat stress soon after muscle injury on the expression of MyoD and myogenin during regeneration process. J Musculoskelet Neuronal Interact 14:325–333
Huard J, Li Y, Fu FH (2002) Muscle injuries and repair: current trends in research. J Bone Joint Surg Am 84:822–832
Jarvinen TAH, Jarvinen TLN, Kaariainen M et al (2007) Muscle injuries: optimising recovery. Best Pract Res Clin Rheumatol 21:317–331. https://doi.org/10.1016/j.berh.2006.12.004
Juban G, Chazaud B (2017) Metabolic regulation of macrophages during tissue repair: insights from skeletal muscle regeneration. FEBS Lett 591:3007–3021. https://doi.org/10.1002/1873-3468.12703
Kaliman P, Canicio J, Tester X et al (1999) Insulin-like growth factor-II, phosphatidylinositol 3-kinase, nuclear factor-kB and inducible nitric-oxide synthase define a common myogenic signaling pathway. J Biol Chem 274:17437–17444. https://doi.org/10.1074/jbc.274.25.17437
Kawashima M, Miyakawa M, Sugiyama M et al (2020) Unloading during skeletal muscle regeneration retards iNOS-expressing macrophage recruitment and perturbs satellite cell accumulation. Histochem Cell Biol 154:355–367. https://doi.org/10.1007/s00418-020-01897-3
Kawashima M, Kawanishi N, Tominaga T et al (2021a) Icing after eccentric contraction-induced muscle damage perturbs the disappearance of necrotic muscle fibers and phenotypic dynamics of macrophages in mice. J Appl Physiol 130:1410–1420. https://doi.org/10.1152/japplphysiol.01069.2020
Kawashima M, Iguchi S, Fujita N et al (2021b) Structural changes in skeletal muscle fibers after icing or heating on downhill running in mice. Kobe J Med Sci 67:48–54
Le Moal E, Juban G, Bernard AS et al (2018) Macrophage-derived superoxide production and antioxidant response following skeletal muscle injury. Free Radic Biol Med 120:33–40. https://doi.org/10.1016/j.freeradbiomed.2018.02.024
Li Y (2003) TNF-α is a mitogen in skeletal muscle. Am J Physiol Cell Physiol 285:370–376. https://doi.org/10.1152/ajpcell.00453.2002
Li Q, Bai Y, Xu Y et al (2010) Autografting satellite cells to repair damaged muscle induced by repeated compression: an animal model. Foot Ankle Int 31:706–711. https://doi.org/10.3113/fai.2010.0706
Liu X, Liu Y, Zhao L et al (2017) Macrophage depletion impairs skeletal muscle regeneration: the roles of regulatory factors for muscle regeneration. Cell Biol Int 41:228–238. https://doi.org/10.1002/cbin.10705
Lovering RM, De Deyne PG (2004) Contractile function, sarcolemma integrity, and the loss of dystrophin after skeletal muscle eccentric contraction-induced injury. Am J Physiol Cell Physiol 286:230–238. https://doi.org/10.1152/ajpcell.00199.2003
Mantovani A, Sica A, Sozzani S et al (2004) The chemokine system in diverse forms of macrophage activation and polarization. Trends Immunol 25:677–686. https://doi.org/10.1016/j.it.2004.09.015
Miyakawa M, Kawashima M, Haba D et al (2020) Inhibition of the migration of MCP-1 positive cells by icing applied soon after crush injury to rat skeletal muscle. Acta Histochem 122:151511. https://doi.org/10.1016/j.acthis.2020.151511
Oyaizu T, Enomoto M, Yamamoto N et al (2018) Hyperbaric oxygen reduces inflammation, oxygenates injured muscle, and regenerates skeletal muscle via macrophage and satellite cell activation. Sci Rep 8:1288. https://doi.org/10.1038/s41598-018-19670-x
Ramos GV, Pinheiro CM, Messa SP et al (2016) Cryotherapy reduces inflammatory response without altering muscle regeneration process and extracellular matrix remodeling of rat muscle. Sci Rep 6:18525. https://doi.org/10.1038/srep18525
Rayagiri SS, Ranaldi D, Raven A et al (2018) Basal lamina remodeling at the skeletal muscle stem cell niche mediates stem cell self-renewal. Nat Commun 9:1075. https://doi.org/10.1038/s41467-018-03425-3
Santa FD, Vitiello L, Torcinaro A et al (2019) The role of metabolic remodeling in macrophage polarization and its effect on skeletal muscle regeneration. Antioxid Redox Signal 30:1553–1598. https://doi.org/10.1089/ars.2017.7420
Sciorati C, Rigamonti E, Manfredi AA et al (2016) Cell death, clearance and immunity in the skeletal muscle. Cell Death Differ 23:927–937. https://doi.org/10.1038/cdd.2015.171
Shibaguchi T, Sugiura T, Fujitsu T et al (2016) Effects of icing or heat stress on the induction of fibrosis and/or regeneration of injured rat soleus muscle. J Physiol Sci 66:345–357. https://doi.org/10.1007/s12576-015-0433-0
Smith C, Kruger MJ, Smith RM et al (2008) The inflammatory response to skeletal muscle injury. Sports Med 38:947–969. https://doi.org/10.2165/00007256-200838110-00005
Srikuea R, Pholpramool C, Kitiyanant Y et al (2010) Satellite cell activity in muscle regeneration after contusion in rats. Clin Exp Pharmacol Physiol 37:1078–1086. https://doi.org/10.1111/j.1440-1681.2010.05439.x
Swenson C, Sward L, Karlsson J (1996) Cryotherapy in sports medicine. Scand J Med Sci Sports 6:193–200. https://doi.org/10.1111/j.1600-0838.1996.tb00090.x
Takagi R, Fujita N, Arakawa T et al (2011) Influence of icing on muscle regeneration after crush injury to skeletal muscles in rats. J Appl Physiol 110:382–388. https://doi.org/10.1152/japplphysiol.01187.2010
Takeuchi K, Hatade T, Wakamiya S et al (2014) Heat stress promotes skeletal muscle regeneration after crush injury in rats. Acta Histochem 116:327–334. https://doi.org/10.1016/j.acthis.2013.08.010
Taylor PR, Martinez-Pomares L, Stacey M et al (2005) Macrophage receptors and immune recognition. Annu Rev Immunol 23:90–144. https://doi.org/10.1146/annurev.immunol.23.021704.115816
Tian Z, Jiang S, Zhang M et al (2016) Detection of satellite cells during skeletal muscle wound healing in rats: time-dependent expressions of Pax7 and MyoD in relation to wound age. Int J Legal Med 130:163–172. https://doi.org/10.1007/s00414-015-1251-x
Tidball JG (1995) Inflammatory cell response to acute muscle injury. Med Sci Sports Exerc 27:1022–1032. https://doi.org/10.1249/00005768-199507000-00011
Tidball JG (2011) Mechanisms of muscle injury, repair, and regeneration. Compr Physiol 1:2029–2062. https://doi.org/10.1002/cphy.c100092
Tidball JG (2017) Regulation of muscle growth and regeneration by the immune system. Nat Rev Immunol 17:165–178. https://doi.org/10.1038/nri.2016.150
Tidball JG, Villalta SA (2010) Regulatory interactions between muscle and the immune system during muscle regeneration. Am J Physiol Regul Integr Comp Physiol 298:1173–1187. https://doi.org/10.1152/ajpregu.00735.2009
Tidball JG, Dorshkind K, Wehling-Henricks M (2014) Shared signaling systems in myeloid cell-mediated muscle regeneration. Development 141:1184–1196. https://doi.org/10.1242/dev.098285
Tonkin J, Temmerman L, Sampson RD et al (2015) Monocyte/macrophage-derived IGF-1 orchestrates murine skeletal muscle regeneration and modulates autocrine polarization. Mol Ther 23:1189–1200. https://doi.org/10.1038/mt.2015.66
Tracey KJ, Cerami A (1994) Tumor necrosis factor: a pleiotropic cytokine and therapeutic target. Annu Rev Med 45:491–503. https://doi.org/10.1146/annurev.med.45.1.491
Vannella KM, Wynn TA (2016) Mechanisms of organ injury and repair by macrophages. Annu Rev Physiol 79:593–617. https://doi.org/10.1146/annurev-physiol-022516-034356
Villalta SA, Rinaldi C, Deng B et al (2011) Interleukin-10 reduces the pathology of mdx muscular dystrophy by deactivating M1 macrophages and modulating macrophage phenotype. Hum Mol Genet 20:790–805. https://doi.org/10.1093/hmg/ddq523
Wang H, Melton DW, Porter L et al (2014) Altered macrophage phenotype transition impairs skeletal muscle regeneration. Am J Pathol 184:1167–1184. https://doi.org/10.1016/j.ajpath.2013.12.020
Watanabe S, Alexander M, Misharin AV et al (2019) The role of macrophages in the resolution of Inflammation. J Clin Invest 129:2619–2628. https://doi.org/10.1172/jci124615
Yin H, Price F, Rudnicki MA (2013) Satellite cells and the muscle stem cell niche. Physiol Rev 93:23–67. https://doi.org/10.1152/physrev.00043.2011
Acknowledgements
The authors thank the members of our laboratory for cooperation. We also would like to thank Enago (www.enago.jp) for the English language review.
Funding
Financial support for this study was provided by JSPS KAKENHI (grant number 21K11238).
Author information
Authors and Affiliations
Contributions
Conceptualization: AM, MK, and TA; methodology: AM, MK, MMiyakawa, MS, and TA; formal analysis and investigation: AM, MK, IN, MMiyakawa, MMiyoshi, TSakuraya, and TSonomura; writing—original draft preparation: AM; writing—review and editing: AM, MK, IN, and TA; funding acquisition: TA; supervision: TA All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethical approval
This study was approved by the Institutional Animal Care and Use Committee and was conducted in accordance with the Kobe University Animal Experimentation Regulations (approval numbers P180706 and P200906).
Informed consent
N/a (animal experiment).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Miyazaki, A., Kawashima, M., Nagata, I. et al. Icing after skeletal muscle injury decreases M1 macrophage accumulation and TNF-α expression during the early phase of muscle regeneration in rats. Histochem Cell Biol 159, 77–89 (2023). https://doi.org/10.1007/s00418-022-02143-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-022-02143-8