Abstract
Purpose
To assess the cumulative risk of progression in glaucomatous eyes in the severe stage of disease.
Methods
This was a retrospective observational study. Patients that had severe damage in at least one eye, as defined by three criteria including a mean deviation of ≤ − 20 dB, were included. Glaucoma progression was defined as a loss of ≥ 2 dB in mean deviation confirmed in three consecutive visual field tests, or a persistent loss of two or more lines of vision—not attributable to non-glaucomatous causes—in three consecutive follow-up examinations. Kaplan-Meier survival analysis was used to assess the cumulative incidence of progression of the first eye to reach endpoint in cases where both eyes were eligible.
Results
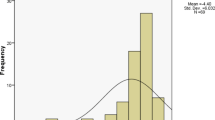
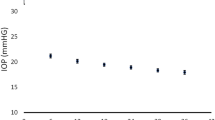
A total of 143 eyes from 119 patients, were studied over a mean period of 4.9 ± 2.9 years. Baseline mean deviation was − 25.3 ± 3.6 dB. Twenty-three eyes of 22 patients reached the progression endpoint: 14 eyes by visual field criteria and 9 by visual acuity criteria. The cumulative 5-year risk of progression estimated by Kaplan-Meier analysis was 14.6% (95% confidence interval: 6.1–22.2%).
Conclusions
In severe glaucoma patients, we found a cumulative incidence of progression of 2.9% per year during the first 5 years of follow-up. Similar incidences have been reported in other studies of glaucoma at different stages of severity.







Similar content being viewed by others
Data availability
Available at the study site.
Change history
17 February 2021
A Correction to this paper has been published: https://doi.org/10.1007/s00417-021-05115-1
References
Flaxman SR, Bourne RRA, Resnikoff S, Ackland P, Braithwaite T, Cicinelli MV, Das A, Jonas JB, Keeffe J, Kempen JH, Leasher J, Limburg H, Naidoo K, Pesudovs K, Silvester A, Stevens GA, Tahhan N, Wong TY, Taylor HR (2017) Global causes of blindness and distance vision impairment 1990-2020: a systematic review and meta-analysis. Lancet Glob Health 5(12):e1221–e1234. https://doi.org/10.1016/s2214-109x(17)30393-5
Mills RP, Budenz DL, Lee PP, Noecker RJ, Walt JG, Siegartel LR, Evans SJ, Doyle JJ (2006) Categorizing the stage of glaucoma from pre-diagnosis to end-stage disease. Am J Ophthalmol 141(1):24–30. https://doi.org/10.1016/j.ajo.2005.07.044
Peters D, Bengtsson B, Heijl A (2014) Factors associated with lifetime risk of open-angle glaucoma blindness. Acta Ophthalmol 92(5):421–425. https://doi.org/10.1111/aos.12203
Vernon SA (2011) Glaucoma with severe field loss at presentation? To operate or not to operate … that is the question. Clin Exp Ophthalmol 39(9):847–848. https://doi.org/10.1111/j.1442-9071.2011.02706.x
Burr J, Azuara-Blanco A, Avenell A (2005) Medical versus surgical interventions for open angle glaucoma. Cochrane Database Syst Rev (2):Cd004399. https://doi.org/10.1002/14651858.CD004399.pub2
Stead RE, King AJ (2011) Outcome of trabeculectomy with mitomycin C in patients with advanced glaucoma. Br J Ophthalmol 95(7):960–965. https://doi.org/10.1136/bjo.2010.185272
Stead R, Azuara-Blanco A, King AJ (2011) Attitudes of consultant ophthalmologists in the UK to initial management of glaucoma patients presenting with severe visual field loss: a national survey. Clin Exp Ophthalmol 39(9):858–864. https://doi.org/10.1111/j.1442-9071.2011.02574.x
King AJ, Fernie G, Azuara-Blanco A, Burr JM, Garway-Heath T, Sparrow JM, Vale L, Hudson J, MacLennan G, McDonald A, Barton K, Norrie J (2018) Treatment of Advanced Glaucoma Study: a multicentre randomised controlled trial comparing primary medical treatment with primary trabeculectomy for people with newly diagnosed advanced glaucoma - study protocol. Br J Ophthalmol 102(7):922–928. https://doi.org/10.1136/bjophthalmol-2017-310902
Holladay JT (1997) Proper method for calculating average visual acuity. J Refract Surg 13(4):388–391
Heijl A, Leske MC, Bengtsson B, Hyman L, Bengtsson B, Hussein M (2002) Reduction of intraocular pressure and glaucoma progression: results from the Early Manifest Glaucoma Trial. Arch Ophthalmol 120(10):1268–1279. https://doi.org/10.1001/archopht.120.10.1268
Smith SD, Katz J, Quigley HA (1996) Analysis of progressive change in automated visual fields in glaucoma. Invest Ophthalmol Vis Sci 37(7):1419–1428
Nouri-Mahdavi K, Hoffman D, Coleman AL, Liu G, Li G, Gaasterland D, Caprioli J (2004) Predictive factors for glaucomatous visual field progression in the Advanced Glaucoma Intervention Study. Ophthalmology 111(9):1627–1635. https://doi.org/10.1016/j.ophtha.2004.02.017
Ederer F, Gaasterland DE, Sullivan EK, Investigators A (1994) The Advanced Glaucoma Intervention Study (AGIS): 1. Study design and methods and baseline characteristics of study patients. Control Clin Trials 15(4):299–325
Kim J, Dally LG, Ederer F, Gaasterland DE, VanVeldhuisen PC, Blackwell B, Sullivan EK, Prum B, Shafranov G, Beck A, Spaeth GL (2004) The Advanced Glaucoma Intervention Study (AGIS): 14. Distinguishing progression of glaucoma from visual field fluctuations. Ophthalmology 111(11):2109–2116. https://doi.org/10.1016/j.ophtha.2004.06.029
Rao HL, Kumar AU, Babu JG, Senthil S, Garudadri CS (2011) Relationship between severity of visual field loss at presentation and rate of visual field progression in glaucoma. Ophthalmology 118(2):249–253. https://doi.org/10.1016/j.ophtha.2010.05.027
Musch DC, Gillespie BW, Lichter PR, Niziol LM, Janz NK (2009) Visual field progression in the Collaborative Initial Glaucoma Treatment Study the impact of treatment and other baseline factors. Ophthalmology 116(2):200–207. https://doi.org/10.1016/j.ophtha.2008.08.051
de Moraes CG, Liebmann JM, Medeiros FA, Weinreb RN (2016) Management of advanced glaucoma: characterization and monitoring. Surv Ophthalmol 61(5):597–615. https://doi.org/10.1016/j.survophthal.2016.03.006
Caprioli J, Mohamed L, Morales E, Rabiolo A, Sears N, Pradtana H, Alizadeh R, Yu F, Afifi AA, Coleman AL, Nouri-Mahdavi K (2018) A method to measure the rate of glaucomatous visual field change. Transl Vis Sci Technol 7(6):14. https://doi.org/10.1167/tvst.7.6.14
Ng WS, Agarwal PK, Sidiki S, McKay L, Townend J, Azuara-Blanco A (2010) The effect of socio-economic deprivation on severity of glaucoma at presentation. Br J Ophthalmol 94(1):85–87. https://doi.org/10.1136/bjo.2008.153312
Kooner KS, AlBdoor M, Cho BJ, Adams-Huet B (2008) Risk factors for progression to blindness in high tension primary open angle glaucoma: comparison of blind and nonblind subjects. Clin Ophthalmol 2(4):757–762. https://doi.org/10.2147/opth.s3139
Forchheimer I, de Moraes CG, Teng CC, Folgar F, Tello C, Ritch R, Liebmann JM (2011) Baseline mean deviation and rates of visual field change in treated glaucoma patients. Eye (Lond) 25(5):626–632. https://doi.org/10.1038/eye.2011.33
Funding
This project was developed within the framework of the Department of Ophthalmology at Pontificia Universidad Catolica de Chile Medical School and had no funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
This study was conducted in accordance with the ethical standards stated in the Declaration of Helsinki. It was approved by the Institutional Review Board (IRB) at Pontificia Universidad Católica de Chile and was granted project ID number 170922006.
Consent to participate
It was waived by the IRB due to the retrospective nature of the study.
Conflict of interest
The authors declare that they have no conflict of interest.
Code availability
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Maul, E.J., Kastner, A., Schmidt, J. et al. Visual field progression in patients with severe glaucoma. Graefes Arch Clin Exp Ophthalmol 259, 1579–1586 (2021). https://doi.org/10.1007/s00417-020-05036-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-020-05036-5