Abstract
Objectives
Friedreich ataxia is (FRDA) an autosomal recessive neurodegenerative disorder associated with intrinsic oxidative damage, suggesting that decreasing lipid peroxidation (LPO) might ameliorate disease progression. The present study tested the ability of RT001, a deuterated form of linoleic acid (D2-LA), to alter disease severity in patients with FRDA in a double-blind placebo-controlled trial.
Methods
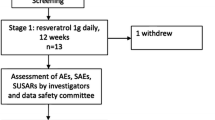
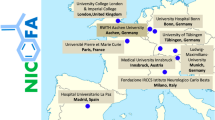
Sixty-five subjects were recruited across six sites and received either placebo or active drug for an 11-month study. Subjects were evaluated at 0, 4, 9, and 11 months, with the primary outcome measure being maximum oxygen consumption (MVO2) during cardiopulmonary exercise testing (CPET). A key secondary outcome measure was a composite statistical test using results from the timed 1-min walk (T1MW), peak workload, and MVO2.
Results
Forty-five subjects completed the protocol. RT001 was well tolerated, with no serious adverse events related to drug. Plasma and red blood cell (RBC) membrane levels of D2-LA and its primary metabolite deuterated arachidonic acid (D2-AA) achieved steady-state concentrations by 4 months. No significant changes in MVO2 were observed for RT001 compared to placebo. Similarly, no differences between the groups were found in secondary or exploratory outcome measures. Post hoc evaluations also suggested minimal effects of RT001 at the dosages used in this study.
Interpretations
The results of this study provide no evidence for a significant benefit of RT001 at the dosages tested in this Friedreich ataxia patient population.





Similar content being viewed by others
Data availability
Data will not be made publicly available at the present time.
References
Santos R, Lefevre S, Sliwa D et al (2010) Friedreich ataxia: molecular mechanisms, redox considerations, and therapeutic opportunities. Antioxid Redox Signal 13:651–690
Armstrong JS, Khdour O, Hecht SM (2010) Does oxidative stress contribute to the pathology of Friedreich’s ataxia? A radical question. FASEB J 24:2152–2163
Strawser C, Schadt K, Hauser L et al (2017) Pharmacological therapeutics in Friedreich ataxia: the present state. Expert Rev Neurother 17:895–907
Babady NE, Carelle N, Wells RD et al (2007) Advancements in the pathophysiology of Friedreich’s Ataxia and new prospects for treatments. Mol Genet Metab 92:23–35
Tsou AY, Paulsen EK, Lagedrost SJ et al (2011) Mortality in Friedreich ataxia. J Neurol Sci 307:46–49
Martelli A, Napierala M, Puccio H (2012) Understanding the genetic and molecular pathogenesis of Friedreich’s ataxia through animal and cellular models. Dis Model Mech 5:165–176
Martelli A, Puccio H (2014) Dysregulation of cellular iron metabolism in Friedreich ataxia: from primary iron-sulfur cluster deficit to mitochondrial iron accumulation. Front Pharmacol 3(5):130
Foury F, Cazzalini O (1997) Deletion of the yeast homologue of the human gene associated with Friedreich’s ataxia elicits iron accumulation in mitochondria. FEBS Lett 411:373–377
Qian SY, Buettner GR (1999) Iron and dioxygen chemistry is an important route to initiation of biological free radical oxidations: an electron paramagnetic resonance spin trap** study. Free Radic Biol Med 26:1447–1456
Guéraud F, Atalay M, Bresgen N et al (2010) Chemistry and biochemistry of lipid peroxidation products. Free Radic Res 44:1098–1124
Chen CT, Green JT, Orr SK, Bazinet RP (2008) Regulation of brain polyunsaturated fatty acid uptake and turnover. Prostaglandins Leukot Essent Fatty Acids 79:85–91
Hill S, Lamberson CR, Xu L et al (2012) Small amounts of isotope-reinforced polyunsaturated fatty acids suppress lipid autoxidation. Free Radic Biol Med 53:893–906
Hill S, Hirano K, Shmanai VV et al (2011) Isotope-reinforced polyunsaturated fatty acids protect yeast cells from oxidative stress. Free Radic Biol Med 50:130–138
Cotticelli MG, Crabbe AM, Wilson RB, Shchepinov MS (2013) Insights into the role of oxidative stress in the pathology of Friedreich ataxia using peroxidation resistant polyunsaturated fatty acids. Redox Biol 1:398–404
Abeti R, Uzun E, Renganathan I et al (2015) Targeting lipid peroxidation and mitochondrial imbalance in Friedreich’s ataxia. Pharmacol Res 99:344–350
Andreyev AY, Tsui HS, Milne GL et al (2015) Isotope-reinforced polyunsaturated fatty acids protect mitochondria from oxidative stress. Free Radic Biol Med 82:63–72
Hatami A, Zhu C, Relaño-Gines A et al (2018) Deuterium-reinforced linoleic acid lowers lipid peroxidation and mitigates cognitive impairment in the Q140 knock in mouse model of Huntington’s disease. FEBS J 285:3002–3012
Elharram A, Czegledy NM, Golod M et al (2017) Deuterium-reinforced polyunsaturated fatty acids improve cognition in a mouse model of sporadic Alzheimer’s disease. FEBS J 284:4083–4095
Shchepinov MS, Chou VP, Pollock E et al (2011) Isotopic reinforcement of essential polyunsaturated fatty acids diminishes nigrostriatal degeneration in a mouse model of Parkinson’s disease. Toxicol Lett 207:97–103
Bedlack R (2019) ALS Untangled No. 47: RT001. Amyotroph Lateral Scler Frontotemporal Degener 20:294–297
Angelova PR, Andruska KM, Midei MG et al (2021) RT001 in progressive supranuclear palsy-clinical and in-vitro observations. Antioxidants (Basel) 10:1021
Adams D, Midei M, Dastgir J et al (2020) Treatment of infantile neuroaxonal dystrophy with RT001: a di-deuterated ethyl ester of linoleic acid: Report of two cases. JIMD Rep 54:54–60
Zesiewicz T, Heerinckx F, De Jager R et al (2018) Randomized, clinical trial of RT001: early signals of efficacy in Friedreich’s ataxia. Mov Disord 33:1000–1005
Lynch DR, Farmer J, Hauser L et al (2018) Safety, pharmacodynamics, and potential benefit of omaveloxolone in Friedreich ataxia. Ann Clin Transl Neurol 6:15–26
Lynch DR, Chin MP, Delatycki MB et al (2021) Safety and efficacy of omaveloxolone in Friedreich Ataxia (MOXIe Study). Ann Neurol 89:212–225
Drinkard BE, Keyser RE, Paul SM et al (2010) Exercise capacity and idebenone intervention in children and adolescents with Friedreich ataxia. Arch Phys Med Rehabil 91:1044–1050
Rummey C, Corben LA, Delatycki MB et al (2019) Psychometric properties of the Friedreich Ataxia Rating Scale. Neurol Genet 5:371
Patel M, Isaacs CJ, Seyer L et al (2016) Progression of Friedreich ataxia: quantitative characterization over 5 years. Ann Clin Transl Neurol 3:684–694
Friedman LS, Farmer JM, Perlman S et al (2010) Measuring the rate of progression in Friedreich ataxia: implications for clinical trial design. Mov Disord 25:426–432
Lynch DR, Farmer JM, Tsou AY et al (2006) Measuring Friedreich ataxia: complementary features of examination and performance measures. Neurology 66:1711–1716
Subramony SH, May W, Lynch D et al (2005) Measuring Friedreich ataxia: interrater reliability of a neurologic rating scale. Neurology 64:1261–1262
Lai JS, Cella D, Chang CH et al (2003) Item banking to improve, shorten and computerize self-reported fatigue: an illustration of steps to create a core item bank from the FACIT-Fatigue Scale. Qual Life Res 12:485–501
Brenna JT, James G, Midei M et al (2020) Plasma and red blood cell membrane accretion and pharmacokinetics of RT001 (bis-Allylic 11,11-D2-Linoleic Acid Ethyl Ester) during Long Term Dosing in Patients. J Pharm Sci 109:3496–3503
Worth AJ, Basu SS, Deutsch EC et al (2015) Stable isotopes and LC-MS for monitoring metabolic disturbances in Friedreich’s ataxia platelets. Bioanalysis 7:1843–1855
Myers LM, Lynch DR, Farmer JM et al (2008) Urinary isoprostanes in Friedreich ataxia: lack of correlation with disease features. Mov Disord 23:1920–1922
Schulz JB, Dehmer T, Schöls L et al (2000) Oxidative stress in patients with Friedreich ataxia. Neurology 55:1719–1721
Di Prospero NA, Baker A, Jeffries N, Fischbeck KH (2007) Neurological effects of high-dose idebenone in patients with Friedreich’s ataxia: a randomised, placebo-controlled trial. Lancet Neurol 6:878–886
DeBrosse C, Nanga RPR, Wilson N et al (2016) Muscle oxidative phosphorylation quantitation using creatine chemical exchange saturation transfer (CrCEST) MRI in mitochondrial disorders. JCI Insight 1:e88207
Chandran V, Gao K, Swarup V et al (2017) Inducible and reversible phenotypes in a novel mouse model of Friedreich’s Ataxia. Elife 6:e30054
Weng L, Laboureur L, Wang Q et al (2020) Extra-mitochondrial mouse frataxin and its implications for mouse models of Friedreich’s ataxia. Sci Rep 10:15788
Guo L, Wang Q, Weng L et al (2018) Characterization of a new N-terminally acetylated extra-mitochondrial isoform of frataxin in human erythrocytes. Sci Rep 8:17043
Pane C, Salzano A, Trinchillo A et al (2022) Safety and feasibility of upper limb cardiopulmonary exercise test in Friedreich ataxia. Eur J Prev Cardiol 29:445–451
Drinkard BE, Keyser RE, Paul SM, Arena R, Plehn JF, Yanovski JA, Di Prospero NA (2010) Exercise capacity and idebenone intervention in children and adolescents with Friedreich ataxia. Arch Phys Med Rehabil 91:1044–1050
Vorgerd M, Schöls L, Hardt C, Ristow M, Epplen JT, Zange J (2000) Mitochondrial impairment of human muscle in Friedreich ataxia in vivo. Neuromuscul Disord 10:430–435
Reetz K, Dogan I, Hilgers R-D et al (2021) Progression characteristics of the European Friedreich’s Ataxia Consortium for Translational Studies (EFACTS): a 4-year cohort study. Lancet Neurol 20:362–372
Acknowledgements
The authors wish to acknowledge the participation of the subjects, the efforts of the site coordinators, and the aid in recruitment from the Friedreich Ataxia Research Alliance.
Funding
The present study was funded by grants to each Institution for Retrotope pharmaceutical. Dr Lynch receives grant money through the Children’s Hospital of Philadelphia from Reata, PTC, Design, FARA, NIH and the FDA. Employment: Drs Midei, Krtolica, Litterman, van der Ploeg, Heerinckx, and Milner are employees of Retrotope, who sponsored the study. Dr Vogel is an employee of Redenlab, who provided speech testing for the study.
Author information
Authors and Affiliations
Contributions
Drs Lynch, Mathews. Perlman, Zesiecz, Vogel, Omidvar and Subramony performed the exams, and supervised data collections at individuals sites. Drs. Krtolica, Litterman, van der Ploeg, Heerinckx, Milner, and Midei designed the experiment, supervised data management at the central site, and performed statistical calculations. Dr. Lynch wrote the initial draft, and all authors provide critical revision.
Corresponding author
Ethics declarations
Conflicts of interest
The authors report no other conflicts of interest.
Ethical approval
IRB approval was obtained by the Institutional Review Board at each Institution.
Consent to participate
Written informed consent was obtained from all subjects before initiation of study procedures.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lynch, D.R., Mathews, K.D., Perlman, S. et al. Double blind trial of a deuterated form of linoleic acid (RT001) in Friedreich ataxia. J Neurol 270, 1615–1623 (2023). https://doi.org/10.1007/s00415-022-11501-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-022-11501-4