Abstract
Purpose
To compare the survival outcome of neoadjuvant therapy (NAT) (chemotherapy or chemotherapy and intracavitary brachytherapy (ICBT) followed by radical surgery and of concomitant chemotherapy and radiotherapy (CCRT) in patients with locally advanced cervical adenocarcinoma and identify predictors of cervical adenocarcinoma.
Methods
We retrospectively reviewed our medical records of cervical adenocarcinoma patients treated with either NAT + surgery or CCRT in our institution from January 2013 to December 2017. The patients were treated with two-dimensional radiotherapy or three-dimensional-conformal or intensity-modulated radiotherapy combined with intracavitary brachytherapy. The regimen of concomitant chemotherapy was weekly cisplatin. The neoadjuvant chemotherapy (NACT) was paclitaxel plus cisplatin. The primary end points were overall survival (OS) and progression-free survival (PFS).
Results
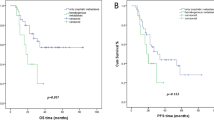
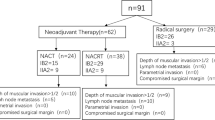
We enrolled 121 patients. There were 42 (34.7%) patients in the NAT + surgery group and 79 (65.3%) in the CCRT group. After univariate multivariate analysis, NAT was an independent predictor of OS (p = 0.008) and PFS (p = 0.006). After propensity score matching, the 5-year OS rates in the NAT + surgery and CCRT groups were 25% and 4%, respectively (p = 0.00014), and the 5-year PFS rates were 25% and 4%, respectively (p = 0.00015). Subgroup analysis showed that the 5-year OS and PFS rates in the NACT + surgery and CCRT groups were both 20% and 8%, respectively (p = 0.015).
Conclusion
Compared with CCRT, NAT followed by radical surgery had better OS and PFS in locally advanced cervical adenocarcinoma. In subgroup analysis, OS and PFS were longer for NACT + surgery than for CCRT.



Similar content being viewed by others
Availability of data and materials
The data reported in this paper have been deposited in the Open Science Framework (OSF), https://osf.io/x2dtq/files/.
Code availability
R statistical software is free, we can download the software from https://www.r-project.org. code used in this paper is available at https://osf.io/x2dtq/files/.
References
Arbyn M, Weiderpass E, Bruni L, de Sanjosé S, Saraiya M, Ferlay J et al (2020) Estimates of incidence and mortality of cervical cancer in 2018: a worldwide analysis. Lancet Glob Heal 8:e191–203
do Rozario S, da Silva IF, Koifman RJ, da Silva IF (2019) Characterization of women with cervical cancer assisted at Inca by histological type. Rev Saude Publica 53:88
Brisson M, Kim JJ, Canfell K, Drolet M, Gingras G, Burger EA et al (2020) Impact of HPV vaccination and cervical screening on cervical cancer elimination: a comparative modelling analysis in 78 low-income and lower-middle-income countries. Lancet 395:575–590
Bray F, Carstensen B, Møller H, Zappa M, Žakelj MP, Lawrence G et al (2005) Incidence trends of adenocarcinoma of the cervix in 13 European countries. Cancer Epidemiol Biomarkers Prev 14:2191–2199
Galic V, Herzog TJ, Lewin SN, Neugut AI, Burke WM, Lu Y et al (2012) Prognostic significance of adenocarcinoma histology in women with cervical cancer. Gynecol Oncol 125:287–291. https://doi.org/10.1016/j.ygyno.2012.01.012(Internet)
Hu Z, Zhu D, Wang W, Li W, Jia W, Zeng X et al (2015) Genome-wide profiling of HPV integration in cervical cancer identifies clustered genomic hot spots and a potential microhomology-mediated integration mechanism. Nat Genet 47:158–163
Hu K, Wang W, Liu X, Meng Q, Zhang F (2018) Comparison of treatment outcomes between squamous cell carcinoma and adenocarcinoma of cervix after definitive radiotherapy or concurrent chemoradiotherapy. Radiat Oncol 13:1–7
Yin K, Lu C, Lin J, Hsu C, Wang L (2018) Treatment outcomes of locally advanced cervical cancer by histopathological types in a single institution: a propensity score matching study. J Formos Med Assoc. https://doi.org/10.1016/j.jfma.2018.07.002(Internet)
Thomas GM (2015) Locally advanced adenocarcinoma and adenosquamous carcinomas of the cervix compared to squamous cell carcinomas of the cervix in Gynecologic Oncology Group trials of cisplatin-based chemoradiation. Gynecol Oncol 135:208–212
Bhatla N, Aoki D, Sharma DN, Sankaranarayanan R (2018) Cancer of the cervix uteri. Int J Gynecol Obstet 143:22–36
Cibula D, Pötter R, Planchamp F, Avall-Lundqvist E, Fischerova D, Haie Meder C et al (2018) The European Society of Gynaecological Oncology/European Society for Radiotherapy and Oncology/European Society of Pathology guidelines for the management of patients with cervical cancer. Int J Gynecol Cancer 28:641–655
Koh W, Abu-rustum NR, Bean S, Bradley K, Campos SM, Cho KR, et al. (2019) Cervical Cancer, Version 3.2019. 17:64–84
Vale C, Tierney JF, Stewart LA, Brady M, Dinshaw K, Jakobsen A et al (2008) Reducing uncertainties about the effects of chemoradiotherapy for cervical cancer: a systematic review and meta-analysis of individual patient data from 18 randomized trials. J Clin Oncol 26:5802–5812
Shrivastava S, Mahantshetty U, Engineer R, Chopra S, Hawaldar R, Hande V et al (2018) Cisplatin chemoradiotherapy vs radiotherapy in FIGO stage IIIB squamous cell carcinoma of the uterine cervix a randomized clinical trial. JAMA Oncol 4:506–513
Rydzewska L, Tierney J, Vale CL, Symonds PR (2012) Neoadjuvant chemotherapy plus surgery versus surgery for cervical cancer. Cochrane Database Syst Rev 2012
Chen H, Liang C, Zhang L, Huang S, Wu X (2008) Clinical efficacy of modified preoperative neoadjuvant chemotherapy in the treatment of locally advanced (stage IB2 to IIB) ervical ancer: randomized study. Gynecol Oncol 110:308–315. https://doi.org/10.1016/j.ygyno.2008.05.026(Internet)
Cai HB, Chen HZ, Yin HH (2006) Randomized study of preoperative chemotherapy versus primary surgery for stage IB cervical cancer. J Obstet Gynaecol Res 32:315–323
Katsumata N, Yoshikawa H, Kobayashi H, Saito T, Kuzuya K, Nakanishi T et al (2013) Phase III randomised controlled trial of neoadjuvant chemotherapy plus radical surgery vs radical surgery alone for stages IB2, IIA2, and IIB cervical cancer: a Japan Clinical Oncology Group trial (JCOG 0102). Br J Cancer 108:1957–1963. https://doi.org/10.1038/bjc.2013.179(Internet)
Eddy GL, Bundy BN, Creasman WT, Spirtos NM, Mannel RS, Hannigan E et al (2007) Treatment of (“bulky”) stage IB cervical cancer with or without neoadjuvant vincristine and cisplatin prior to radical hysterectomy and pelvic/para-aortic lymphadenectomy: a phase III trial of the gynecologic oncology group. Gynecol Oncol 106:362–369
Gupta S, Maheshwari A, Parab P, Mahantshetty U, Hawaldar R, Sastri S, Kerkar R et al (2018) Neoadjuvant chemotherapy followed by radical surgery versus concomitant chemotherapy and radiotherapy in patients with stage IB2, IIA, or IIB squamous cervical cancer: a randomized controlled trial. J Clin Oncol 36:1548–1555
Yin M, Zhao F, Lou G, Zhang H, Sun M, Li C et al (2011) The long-term efficacy of neoadjuvant chemotherapy followed by radical hysterectomy compared with radical surgery alone or concurrent chemoradiotherapy on locally advanced-stage cervical cancer. Int J Gynecol Cancer 21:92–99
Minig L, Colombo N, Zanagnolo V, Landoni F, Bocciolone L, Cárdenas-Rebollo JM et al (2013) Platinum-based neoadjuvant chemotherapy followed by radical surgery for cervical carcinoma international federation of gynecology and obstetrics stage IB2-IIB. Int J Gynecol Cancer 23:1647–1654
Wang W, Liu X, Meng Q, Zhang F, Hu K (2018) Prophylactic extended-field irradiation for patients with cervical cancer treated with concurrent chemoradiotherapy: a propensity-score matching analysis. Int J Gynecol Cancer 28:1584–1591
Platt SL, Patel A, Humphrey PJ, Al-Booz H, Bailey J (2019) Completion surgery after chemoradiotherapy for cervical cancer–is there a role? UK Cancer Centre experience of hysterectomy post chemo-radiotherapy treatment for cervical cancer. J Obstet Gynaecol 39:68–73. https://doi.org/10.1080/01443615.2018.1463205(Internet)
Favero G, Pierobon J, Genta ML, Araújo MP, Miglino G, Del Carmen Pilar Diz M et al (2014) Laparoscopic extrafascial hysterectomy (completion surgery) after primary chemoradiation in patients with locally advanced cervical cancer: technical aspects and operative outcomes. Int J Gynecol Cancer 24:608–614
Yang J, Yang J, Cao D, Shen K, Ma J, Zhang F (2020) Completion hysterectomy after chemoradiotherapy for locally advanced adeno-type cervical carcinoma: updated survival outcomes and experience in post radiation surgery. J Gynecol Oncol 31:1–12
Acknowledgements
Thanks for The Third Affiliated Hospital of Kunming Medical University supporting the writing of this manuscript. Thanks to Xudong Gao, Yunhe Ju and **ang Ding for their financial support for this research.
Funding
None.
Author information
Authors and Affiliations
Contributions
TT: project development, data collection, data analysis, manuscript writing. YA: administrative support. XG: financial support. YJ: financial support. XD: financial support.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
Institutional review board approval (IRB) of the Third Affiliated Hospital of Kunming Medical University was obtained for this study. This study was conducted in concordance with the Helsinki Declaration.
Consent to participate
Informed consent included in the study was obtained from individual participants or next of kin of dead patients.
Consent for publish
Agree to publish.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tian, T., Gao, X., Ju, Y. et al. Comparison of the survival outcome of neoadjuvant therapy followed by radical surgery with that of concomitant chemoradiotherapy in patients with stage IB2–IIIB cervical adenocarcinoma. Arch Gynecol Obstet 303, 793–801 (2021). https://doi.org/10.1007/s00404-020-05826-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-020-05826-6