Abstract
Introduction
Tibial component design and positioning contribute more to patient satisfaction than previously realized. A surgeon needs to decide on the size and rotation, bearing in mind that coverage should be as high as possible, whilst malrotation and overhang should be avoided. No study investigates the impact of each of these components on clinical outcomes in a single cohort.
Materials and methods
This is a retrospective analysis of 1-year postoperative outcomes measured with the Knee Injury and Osteoarthritis Outcome (KOOS) Score, as well as a previously validated rotational CT protocol. Coverage, rotation from Insall’s axis, and overhang of an asymmetric tibial baseplate were measured, and positive and negative correlations to clinical outcomes were calculated.
Results
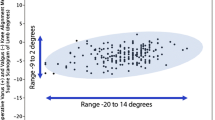
A total of 499 knees were analyzed. Patient average age was 68.4 years. Rotation within 7° internal and 5° external from Insall’s axis was a “safe zone”. Mean coverage was 76%. A total of 429 knees (94%) had a coverage of at least 70% and 102 knees (22%) greater than 80%. Overhang was detected in 23% of the cohort. Increased coverage was correlated to increased KOOS score and overhang correlated with a decreased KOOS score (p = 0.008).
Conclusions
This study demonstrates the individual role of three aspects of tibial component implantation properties in postoperative pain and short-term functional outcomes. Upsizing to the point of overhang with rotational tolerance of 7° internal and 3° external to Insall’s axis demonstrates best patient reported outcomes. Overhang decreases the clinical outcome by the same margin as loss of 16% of coverage.



Similar content being viewed by others
References
National Joint Registry for England, Wales, Northern Ireland and the Isle of Man (2019) The National Joint Registry Annual Report 2019. https://www.hqip.org.uk/wp-content/uploads/2018/11/NJR-15th-Annual-Report-2018.pdf
Dunbar MJ, Richardson G, Robertsson O (2013) I can’t get no satisfaction after my total knee replacement: rhymes and reasons. Bone Jt J 95-B:148–152. https://doi.org/10.1302/0301-620X.95B11.32767
Nicoll D, Rowley DI (2010) Internal rotational error of the tibial component is a major cause of pain after total knee replacement. J Bone Jt Surg Br 92:1238–1244. https://doi.org/10.1302/0301-620X.92B9.23516
Bell SW, Young P, Drury C et al (2014) Component rotational alignment in unexplained painful primary total knee arthroplasty. Knee 21:272–277. https://doi.org/10.1016/j.knee.2012.09.011
Bonnin MP, Saffarini M, Mercier P-E et al (2011) Is the anterior tibial tuberosity a reliable rotational landmark for the tibial component in total knee arthroplasty? J Arthroplast 26(260–267):e1–2. https://doi.org/10.1016/j.arth.2010.03.015
Mitsuhashi S, Akamatsu Y, Kobayashi H et al (2018) Combined CT-based and image-free navigation systems in TKA reduces postoperative outliers of rotational alignment of the tibial component. Arch Orthop Trauma Surg 138:259–266. https://doi.org/10.1007/s00402-017-2837-1
Panni AS, Ascione F, Rossini M et al (2018) Tibial internal rotation negatively affects clinical outcomes in total knee arthroplasty: a systematic review. Knee Surg Sports Traumatol Arthrosc 26:1636–1644. https://doi.org/10.1007/s00167-017-4823-0
Wernecke GC, Harrris IA, Seeto BG et al (2016) Normal femorotibial rotational alignment and implications for total knee arthroplasty: an MRI analysis. HSS J 12:216–222. https://doi.org/10.1007/s11420-016-9491-y
Cobb JP, Dixon H, Dandachli W, Iranpour F (2008) The anatomical tibial axis: reliable rotational orientation in knee replacement. J Bone Jt Surg Br 90:1032–1038. https://doi.org/10.1302/0301-620X.90B8.19905
Scott RD (2013) Femoral and tibial component rotation in total knee arthroplasty: methods and consequences. Bone Jt J 95-B:140–143. https://doi.org/10.1302/0301-620X.95B11.32765
Incavo SJ, Ronchetti PJ, Howe JG, Tranowski JP (1994) Tibial plateau coverage in total knee arthroplasty. Clin Orthop Relat Res 299:81–85
Berend ME, Ritter MA, Hyldahl HC et al (2008) Implant migration and failure in total knee arthroplasty is related to body mass index and tibial component size. J Arthroplast 23:104–109. https://doi.org/10.1016/j.arth.2008.05.020
Hartel MJ, Loosli Y, Delfosse D et al (2014) The influence of tibial morphology on the design of an anatomical tibial baseplate for TKA. Knee 21:415–419. https://doi.org/10.1016/j.knee.2014.01.003
Martin S, Saurez A, Ismaily S et al (2014) Maximizing tibial coverage is detrimental to proper rotational alignment. Clin Orthop Relat Res 472:121–125. https://doi.org/10.1007/s11999-013-3047-y
Simsek ME, Akkaya M, Gursoy S et al (2018) Posterolateral overhang affects patient quality of life after total knee arthroplasty. Arch Orthop Trauma Surg 138:409–418. https://doi.org/10.1007/s00402-017-2850-4
Bonnin MP, Saffarini M, Shepherd D et al (2016) Oversizing the tibial component in TKAs: incidence, consequences and risk factors. Knee Surg Sports Traumatol Arthrosc 24:2532–2540. https://doi.org/10.1007/s00167-015-3512-0
Lemaire P, Pioletti DP, Meyer FM et al (1997) Tibial component positioning in total knee arthroplasty: bone coverage and extensor apparatus alignment. Knee Surg Sports Traumatol Arthrosc 5:251–257. https://doi.org/10.1007/s001670050059
Mori S, Akagi M, Asada S et al (2013) Tibia vara affects the aspect ratio of tibial resected surface in female Japanese patients undergoing TKA. Clin Orthop Relat Res 471:1465–1471. https://doi.org/10.1007/s11999-013-2800-6
Wakelin EA, Tran L, Twiggs JG et al (2018) Accurate determination of post-operative 3D component positioning in total knee arthroplasty: the AURORA protocol. J Orthop Surg Res 13:275. https://doi.org/10.1186/s13018-018-0957-0
Twiggs JG, Dickison DM, Kolos EC et al (2018) Patient variation limits use of fixed references for femoral rotation component alignment in total knee arthroplasty. J Arthroplasty 33:67–74. https://doi.org/10.1016/j.arth.2017.08.023
Hutt J, Massé V, Lavigne M, Vendittoli P-A (2016) Functional joint line obliquity after kinematic total knee arthroplasty. Int Orthop 40:29–34. https://doi.org/10.1007/s00264-015-2733-7
Lakstein D, Zarrabian M, Kosashvili Y et al (2010) Revision total knee arthroplasty for component malrotation is highly beneficial: a case control study. J Arthroplast 25:1047–1052. https://doi.org/10.1016/j.arth.2009.07.004
Kuriyama S, Ishikawa M, Furu M et al (2014) Malrotated tibial component increases medial collateral ligament tension in total knee arthroplasty. J Orthop Res 32:1658–1666. https://doi.org/10.1002/jor.22711
Howell SM, Chen J, Hull ML (2013) Variability of the location of the tibial tubercle affects the rotational alignment of the tibial component in kinematically aligned total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 21:2288–2295. https://doi.org/10.1007/s00167-012-1987-5
Graw BP, Harris AH, Tripuraneni KR, Giori NJ (2010) Rotational references for total knee arthroplasty tibial components change with level of resection. Clin Orthop Relat Res 468:2734–2738. https://doi.org/10.1007/s11999-010-1330-8
Kim JI, Jang J, Lee KW et al (2017) Anterior tibial curved cortex is a reliable landmark for tibial rotational alignment in total knee arthroplasty. BMC Musculoskelet Disord. https://doi.org/10.1186/s12891-017-1609-y
Baldini A, Indelli PF, Luca DEL et al (2013) Rotational alignment of the tibial component in total knee arthroplasty: the anterior tibial cortex is a reliable landmark. Joints 1:155–160
Aglietti P, Sensi L, Cuomo P, Ciardullo A (2008) Rotational position of femoral and tibial components in TKA using the femoral transepicondylar axis. Clin Orthop Relat Res 466:2751–2755. https://doi.org/10.1007/s11999-008-0452-8
Akagi M, Mori S, Nishimura S et al (2005) Variability of extraarticular tibial rotation references for total knee arthroplasty. Clin Orthop Relat Res 436:172–176
Sahin N, Atıcı T, Öztürk A et al (2012) Accuracy of anatomical references used for rotational alignment of tibial component in total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 20:565–570. https://doi.org/10.1007/s00167-011-1606-x
Devji T, Guyatt GH, Lytvyn L et al (2017) Application of minimal important differences in degenerative knee disease outcomes: a systematic review and case study to inform BMJ rapid recommendations. BMJ Open 7:e015587. https://doi.org/10.1136/bmjopen-2016-015587
Liau JJ, Cheng CK, Huang CH, Lo WH (2002) The effect of malalignment on stresses in polyethylene component of total knee prostheses–a finite element analysis. Clin Biomech (Bristol, Avon) 17:140–146
Dai Y, Scuderi GR, Bischoff JE et al (2014) Anatomic tibial component design can increase tibial coverage and rotational alignment accuracy: a comparison of six contemporary designs. Knee Surg Sports Traumatol Arthrosc 22:2911–2923. https://doi.org/10.1007/s00167-014-3282-0
Ma Y, Mizu-Uchi H, Okazaki K et al (2018) Effects of tibial baseplate shape on rotational alignment in total knee arthroplasty: three-dimensional surgical simulation using osteoarthritis knees. Arch Orthop Trauma Surg 138:105–114. https://doi.org/10.1007/s00402-017-2828-2
Nielsen CS, Nebergall A, Huddleston J et al (2018) Medial overhang of the tibial component is associated with higher risk of inferior knee injury and osteoarthritis outcome score pain after knee replacement. J Arthroplast 33:1394–1398. https://doi.org/10.1016/j.arth.2017.12.027
Abram SGF, Marsh AG, Brydone AS et al (2014) The effect of tibial component sizing on patient reported outcome measures following uncemented total knee replacement. Knee 21:955–959. https://doi.org/10.1016/j.knee.2014.05.010
Heyse TJ, Tibesku CO (2014) Improved femoral component rotation in TKA using patient-specific instrumentation. Knee 21:268–271. https://doi.org/10.1016/j.knee.2012.10.009
Heyse TJ, El-Zayat BF, De Corte R et al (2018) Internal femoral component malrotation in TKA significantly alters tibiofemoral kinematics. Knee Surg Sports Traumatol Arthrosc 26:1767–1775. https://doi.org/10.1007/s00167-017-4778-1
Nedopil AJ, Howell SM, Hull ML (2017) What mechanisms are associated with tibial component failure after kinematically-aligned total knee arthroplasty? Int Orthop 41:1561–1569. https://doi.org/10.1007/s00264-017-3490-6
National Joint Replacement Registry AOA (2019) 2019 Hip, knee and shoulder arthroplasty annual report. https://aoanjrr.sahmri.com/documents/10180/668596/Hip%2C+Knee+%26+Shoulder+Arthroplasty/c287d2a3-22df-a3bb-37a2-91e6c00bfcf0
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Antonio Klasan has received research support from Implantcast. Joshua Twiggs is an employee of 360 Knee Systems. Brett Fritsch has been paid for presentations by and is a consultant for Arthrex and Omni. He has stock options in 360 Knee Systems, he has received research support from Arthrex, Smith & Nephew and Zimmer. Brad Miles has Stock Options in 360 Knee Systems. Thomas Heyse has been paid for presentations by Smith & Nephew, Zimmer Biomet and Implantcast, he has received research support from Smith & Nephew, Zimmer Biomet and Implantcast and he is a consultant to Smith & Nephew. Michael Solomon receives royalties from Corin and Medacta, has been paid for presentations and received research support from Corin. David Parker has been paid for presentations by Arthrex and Smith & Nephew, he is a consultant for Arthrex and Global, has stock options in 360 Knee Systems and Trium.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Klasan, A., Twiggs, J.G., Fritsch, B.A. et al. Correlation of tibial component size and rotation with outcomes after total knee arthroplasty. Arch Orthop Trauma Surg 140, 1819–1824 (2020). https://doi.org/10.1007/s00402-020-03550-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-020-03550-z