Abstract
Objective
Brain tumors are the second most common pediatric malignancy and the most common cause of cancer-related mortality and morbidities. Major advances in terms of surgery, radiation, and chemotherapy have led to better outcomes in developed countries. Delayed diagnosis, advanced disease at presentation, late referrals, nosocomial infections, delays to radiotherapy, and poor support services are the major reasons for poorer outcomes in develo** countries. Little is known about the profile of brain tumors in Pakistan. This study aims to evaluate the epidemiology, management, and clinical outcomes of children with brain tumors in Pakistan in a single tertiary care center.
Methods/materials
All children (0–16 years) with primary CNS tumors from 2004 to 2014 at Aga Khan University Hospital were reviewed retrospectively for clinical data, demographics, radiological findings, management, and outcome.
Results
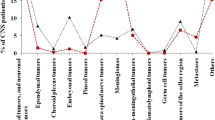
One hundred seventy-five children were included in the study. Male to female ratio was 1.4:1. Most of the patients were in 5–10 years age group (38.9%). Most common presenting complains were headache 115 (65.7%) and vomiting 100 (57.1%). Predominant site was infratentorial 93 (53%). Glial tumors were 105 (60%) followed by embryonal 40(22.9%), craniopharyngiomas 25 (14.3%), and germ cell 1 (0.6%). Astrocytomas (25.7%) were the most common glial tumors while medulloblastoma (15.4%) was the most common embryonal tumor. Majority of the patients underwent surgical resection (78.8%). Radiation was given to 47 (26.8%) patients. A half of the patients, 89 (50%), were lost to follow-up. Forty-two (24%) patients expired, 20 (11.4%) are alive with residual disease while 15 patients (8.5%) were cured with no evidence of recurrence and regular follow-ups.
Conclusion
This is the only study from Pakistan showing demographics of the childhood brain tumors. Significant improvement needs to be made for timely diagnosis, early referrals, and collaborated team efforts with multidisciplinary tumor board to improve outcome.






Similar content being viewed by others
References
Ahmed N, Bhurgri Y, Sadiq S, Shakoor KA (2003) Pediatric brain tumours at a tertiary care hospital in Karachi. Asian Pac J Cancer Prev 8:399
Baldwin RT, Preston-Martin S (2004) Epidemiology of brain tumors in childhood—a review. Toxicol Appl Pharmacol 199:118–131
Bleyer WA (1999) Epidemiologic impact of children with brain tumors. Childs Nerv Syst 15:758–763
Brown S, Belgaumi A, Ajarim D, Kofide A, Al Saad R, Sabbah R et al (2004) Loss to follow-up of patients with malignant lymphoma. Eur J Cancer Care (Engl) 13:180–184
Cho KT, Wang KC, Kim SK, Shin SH, Chi JG, Cho BK (2002) Pediatric brain tumors: statistics of SNUH, Korea (1959–2000). Childs Nerv Syst 18:30–37
El-Gaidi MA (2011) Descriptive epidemiology of pediatric intracranial neoplasms in Egypt. J Neurosurg Pediatr 47:385–395
Ferlay J, Heanue M, Boyle P (2007) Cancer incidence in five continents, Volume IX. IARC Scientific Publications
Horner M, Ries L, Krapcho M, Neyman N, Aminou R, Howlader N, et al (2009) SEER cancer statistics review, 1975-2006, National Cancer Institute. Bethesda, MD
Kadri H, Mawla AA, Murad L (2005) Incidence of childhood brain tumors in Syria (1993–2002). J Neurosurg Pediatr 41:173–177
Keene DL, Hsu E, Ventureyra E (1999) Brain tumors in childhood and adolescence. Pediatr Neurol 20:198–203
Luo XQ, Ke ZY, Huang LB, Guan XQ, Zhang YC, Zhang XL (2009) High-risk childhood acute lymphoblastic leukemia in China: factors influencing the treatment and outcome. Pediatr Blood Cancer 52:191–195
Magnani C, Aareleid T, Viscomi S, Pastore G, Berrino F, Group EW (2001) Variation in survival of children with central nervous system (CNS) malignancies diagnosed in Europe between 1978 and 1992: the EUROCARE study. Eur J Cancer Care (Engl) 37:711–721
Memon F, Rathi SL, Memon MH (2007) Pattern of solid paediatric malignant neoplasm at LUMHS, Jamshoro, Pakistan. J Ayub Med Coll Abbottabad 19:55–57
Ostrom QT, Gittleman H, Farah P, Ondracek A, Chen Y, Wolinsky Y et al (2013) CBTRUS statistical report: primary brain and central nervous system tumors diagnosed in the United States in 2006-2010. J Neuro-Oncol 15:ii1–ii56
Parkin D, Kramarova E, Draper G, Masuyer E, Michaelis J, Neglia J, et al (1998) International incidence of childhood cancer, Volume II. IARC Scientific Publications
Peris-Bonet R, Martínez-García C, Lacour B, Petrovich S, Giner-Ripoll B, Navajas A, Steliarova-Foucher E (2006) Childhood central nervous system tumours–incidence and survival in Europe (1978–1997): report from automated childhood cancer information system project. Eur J Cancer Care (Engl) 42:2064–2080
Madhavan R, Kannabiran B, Nithya A, Kani J, Balasubramaniam P, Shanmugakumar S (2016) Pediatric brain tumors: an analysis of 5 years of data from a tertiary cancer care center, India. Indian J Cancer 53:562–565
Suresh SG, Srinivasan A, Scott JX, Rao SM, Chidambaram B, Chandrasekar S (2017) Profile and outcome of pediatric brain tumors–experience from a tertiary care pediatric oncology unit in South India. Eur J Paediatr Neurol 12:237
Bellil S, Limaiem F, Mahfoudhi H, Bellil K, Chelly I, Mekni A et al (2008) Descriptive epidemiology of childhood central nervous system tumours in Tunisia. J Neurosurg Pediatr 44:382–387
Ezzat S, Kamal M, El-Khateeb N, El-Beltagy M, Taha H, Refaat A et al (2016) Pediatric brain tumors in a low/middle income country: does it differ from that indeveloped world? J Neuro-Oncol 126:371–376
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Research involving human participants and/or animals
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Riaz, Q., Naeem, E., Fadoo, Z. et al. Intracranial tumors in children: a 10-year review from a single tertiary health-care center. Childs Nerv Syst 35, 2347–2353 (2019). https://doi.org/10.1007/s00381-019-04260-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-019-04260-7