Abstract
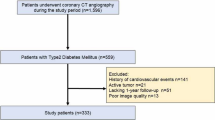
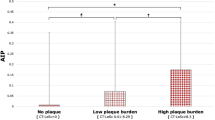
Pericoronary adipose tissue (PCAT) attenuation on coronary computed tomography angiography (CTA) has been emerged as a marker of pericoronary inflammation. We aimed to investigate the prognostic value of PCAT attenuation in patients with non-alcoholic fatty liver disease (NAFLD). We enrolled 232 NAFLD patients with suspected coronary artery disease and underwent coronary CTA. NAFLD was defined by abdominal CT as the ratio of hepatic attenuation to spleen attenuation less than 1.0. PCAT attenuation values were assessed by the crude analysis of mean CT attenuation value of the left anterior descending artery (LAD) and right coronary artery (RCA). As coronary CTA findings, luminal stenosis and high-risk plaque features were examined. Primary outcome was the composite of cardiovascular (CV) death, nonfatal acute coronary syndrome, and hospitalization for heart failure. During a median follow-up of 4.9 years, 17 patients had CV events. LAD-PCAT attenuation in patients with CV events was higher than that without CV events (−66.9 ± 7.0 versus −70.5 ± 6.6; p = 0.032), while RCA-PCAT attenuation was not. LAD-PCAT attenuation and high-risk plaque features were independent predictors of CV events. The addition of LAD-PCAT attenuation to high-risk plaque features increased the C-statistics and global chi-square from 0.66 to 0.75 (p = 0.042) and 6.8 to 12.7 (p = 0.015), respectively. The net reclassification achieved by adding LAD-PCAT attenuation to high-risk plaque features was 0.494 (p = 0.041). High-LAD-PCAT attenuation was an independent predictor of CV events in NAFLD patients, regardless of CTA-verified high-risk plaque features. In addition, LAD-PCAT attenuation had an incremental prognostic value over high-risk plaque features.




Similar content being viewed by others
References
Younossi ZM, Koenig AB, Abdelatif D, Fazel Y, Henry L, Wymer M (2016) Global epidemiology of nonalcoholic fatty liver disease—meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology 64:73–84
Hamaguchi M, Takeda N, Kojima T, Ohbora A, Kato T, Sarui H, Fukui M, Nagata C, Takeda J (2012) Identification of individuals with non-alcoholic fatty liver disease by the diagnostic criteria for the metabolic syndrome. World J Gastroenterol 18:1508–1516
Estes C, Anstee QM, Arias-Loste MT, Bantel H, Bellentani S, Caballeria J, Colombo M, Craxi A, Crespo J, Day CP, Eguchi Y, Geier A, Kondili LA, Kroy DC, Lazarus JV, Loomba R, Manns MP, Marchesini G, Nakajima A, Negro F, Petta S, Ratziu V, Romero-Gomez M, Sanyal A, Schattenberg JM, Tacke F, Tanaka J, Trautwein C, Wei L, Zeuzem S, Razavi H (2018) Modeling NAFLD disease burden in China, France, Germany, Italy, Japan, Spain, United Kingdom, and United States for the period 2016–2030. J Hepatol 69:896–904
Ichikawa K, Miyoshi T, Osawa K, Miki T, Toda H, Ejiri K, Yoshida M, Nakamura K, Morita H, Ito H (2021) Incremental prognostic value of non-alcoholic fatty liver disease over coronary computed tomography angiography findings in patients with suspected coronary artery disease. Eur J Prev Cardiol 28(18):2059–2066
Chalasani N, Younossi Z, Lavine JE, Charlton M, Cusi K, Rinella M, Harrison SA, Brunt EM, Sanyal AJ (2018) The diagnosis and management of nonalcoholic fatty liver disease: practice guidance from the American Association for the Study of Liver Diseases. Hepatology 67:328–357
Higashi S, Shiga Y, Yano M, Imaizumi T, Tashiro K, Idemoto Y, Kato Y, Kuwano T, Sugihara M, Miura SI (2021) Associations between smoking habits and major adverse cardiovascular events in patients who underwent coronary computed tomography angiography as screening for coronary artery disease. Heart Vessels 36:483–491
Sheta HM, Precht H, Busk C, Heinsen LJ, Nieman K, Egstrup K, Lambrechtsen J (2022) Dual-energy CT plaque characteristics of post mortem thin-cap fibroatheroma in comparison to infarct-related culprit lesions. Heart Vessels 37:400–410
Puchner SB, Liu T, Mayrhofer T, Truong QA, Lee H, Fleg JL, Nagurney JT, Udelson JE, Hoffmann U, Ferencik M (2014) High-risk plaque detected on coronary CT angiography predicts acute coronary syndromes independent of significant stenosis in acute chest pain: results from the ROMICAT-II trial. J Am Coll Cardiol 64:684–692
Takamura K, Fujimoto S, Kondo T, Hiki M, Kawaguchi Y, Kato E, Daida H (2017) Incremental prognostic value of coronary computed tomography angiography: high-risk plaque characteristics in asymptomatic patients. J Atheroscler Thromb 24:1174–1185
Halon DA, Lavi I, Barnett-Griness O, Rubinshtein R, Zafrir B, Azencot M, Lewis BS (2019) Plaque morphology as predictor of late plaque events in patients with asymptomatic type 2 diabetes: a long-term observational study. JACC Cardiovasc Imaging 12:1353–1363
Ichikawa K, Miyoshi T, Osawa K, Miki T, Nakamura K, Ito H (2020) prognostic value of coronary computed tomographic angiography in patients with nonalcoholic fatty liver disease. JACC Cardiovasc Imaging 13:1628–1630
Oikonomou EK, Marwan M, Desai MY, Mancio J, Alashi A, Hutt Centeno E, Thomas S, Herdman L, Kotanidis CP, Thomas KE, Griffin BP, Flamm SD, Antonopoulos AS, Shirodaria C, Sabharwal N, Deanfield J, Neubauer S, Hopewell JC, Channon KM, Achenbach S, Antoniades C (2018) Non-invasive detection of coronary inflammation using computed tomography and prediction of residual cardiovascular risk (the CRISP CT study): a post-hoc analysis of prospective outcome data. Lancet 392:929–939
van Diemen PA, Bom MJ, Driessen RS, Schumacher SP, Everaars H, de Winter RW, van de Ven PM, Freiman M, Goshen L, Heijtel D, Langzam E, Min JK, Leipsic JA, Raijmakers PG, van Rossum AC, Danad I, Knaapen P (2021) Prognostic value of RCA pericoronary adipose tissue CT-attenuation beyond high-risk plaques, plaque volume, and ischemia. JACC Cardiovasc Imaging 14:1598–1610
Zeb I, Li D, Nasir K, Katz R, Larijani VN, Budoff MJ (2012) Computed tomography scans in the evaluation of fatty liver disease in a population based study: the multi-ethnic study of atherosclerosis. Acad Radiol 19:811–818
Ichikawa K, Miyoshi T, Osawa K, Miki T, Toda H, Ejiri K, Yoshida M, Nanba Y, Yoshida M, Nakamura K, Morita H, Ito H (2021) Prognostic value of non-alcoholic fatty liver disease for predicting cardiovascular events in patients with diabetes mellitus with suspected coronary artery disease: a prospective cohort study. Cardiovasc Diabetol 20:8
Cury RC, Abbara S, Achenbach S, Agatston A, Berman DS, Budoff MJ, Dill KE, Jacobs JE, Maroules CD, Rubin GD, Rybicki FJ, Schoepf UJ, Shaw LJ, Stillman AE, White CS, Woodard PK, Leipsic JA (2016) CAD-RADS(TM) coronary artery disease—reporting and data system. An expert consensus document of the Society of Cardiovascular Computed Tomography (SCCT), the American College of Radiology (ACR) and the North American Society for Cardiovascular Imaging (NASCI). Endorsed by the American College of Cardiology. J Cardiovasc Comput Tomogr 10:269–281
Hoshino M, Yang S, Sugiyama T, Zhang J, Kanaji Y, Yamaguchi M, Hada M, Sumino Y, Horie T, Nogami K, Ueno H, Misawa T, Usui E, Murai T, Lee T, Yonetsu T, Kakuta T (2020) Peri-coronary inflammation is associated with findings on coronary computed tomography angiography and fractional flow reserve. J Cardiovasc Comput Tomogr 14:483–489
Suruga K, Miyoshi T, Kotani K, Ichikawa K, Miki T, Osawa K, Ejiri K, Toda H, Nakamura K, Morita H, Ito H (2021) Higher oxidized high-density lipoprotein to apolipoprotein A-I ratio is associated with high-risk coronary plaque characteristics determined by CT angiography. Int J Cardiol 324:193–198
Goda A, Masuyama T (2016) Obesity and overweight in Asian people. Circ J 80:2425–2426
Iwasaki Y, Shiina K, Matsumoto C, Nakano H, Fujii M, Yamashina A, Chikamori T, Tomiyama H (2021) Correlation of the fatty liver index with the pathophysiological abnormalities associated with cardiovascular risk markers in Japanese men without any history of cardiovascular disease: comparison with the fibrosis-4 score. J Atheroscler Thromb 28:524–534
Antonopoulos AS, Sanna F, Sabharwal N, Thomas S, Oikonomou EK, Herdman L, Margaritis M, Shirodaria C, Kampoli AM, Akoumianakis I, Petrou M, Sayeed R, Krasopoulos G, Psarros C, Ciccone P, Brophy CM, Digby J, Kelion A, Uberoi R, Anthony S, Alexopoulos N, Tousoulis D, Achenbach S, Neubauer S, Channon KM, Antoniades C (2017) Detecting human coronary inflammation by imaging perivascular fat. Sci Transl Med 9 (398):eaal2658
Fricker ZP, Pedley A, Massaro JM, Vasan RS, Hoffmann U, Benjamin EJ, Long MT (2019) Liver fat is associated with markers of inflammation and oxidative stress in analysis of data from the Framingham Heart Study. Clin Gastroenterol Hepatol 17(6):1157-1164 e1154
Ichikawa K, Miyoshi T, Osawa K, Miki T, Morimitsu Y, Akagi N, Nakashima M, Ito H (2021) Association between higher pericoronary adipose tissue attenuation measured by coronary computed tomography angiography and nonalcoholic fatty liver disease: a matched case-control study. Medicine (Baltimore) 100:e27043
Dulai PS, Singh S, Patel J, Soni M, Prokop LJ, Younossi Z, Sebastiani G, Ekstedt M, Hagstrom H, Nasr P, Stal P, Wong VW, Kechagias S, Hultcrantz R, Loomba R (2017) Increased risk of mortality by fibrosis stage in nonalcoholic fatty liver disease: systematic review and meta-analysis. Hepatology 65:1557–1565
Mantovani A, Csermely A, Petracca G, Beatrice G, Corey KE, Simon TG, Byrne CD, Targher G (2021) Non-alcoholic fatty liver disease and risk of fatal and non-fatal cardiovascular events: an updated systematic review and meta-analysis. Lancet Gastroenterol Hepatol 6:903–913
Glass O, Henao R, Patel K, Guy CD, Gruss HJ, Syn WK, Moylan CA, Streilein R, Hall R, Mae Diehl A, Abdelmalek MF (2018) Serum interleukin-8, osteopontin, and monocyte chemoattractant protein 1 are associated with hepatic fibrosis in patients with nonalcoholic fatty liver disease. Hepatol Commun 2:1344–1355
Goeller M, Achenbach S, Herrmann N, Bittner DO, Kilian T, Dey D, Raaz-Schrauder D, Marwan M (2021) Pericoronary adipose tissue CT attenuation and its association with serum levels of atherosclerosis-relevant inflammatory mediators, coronary calcification and major adverse cardiac events. J Cardiovasc Comput Tomogr 15:449–454
Elnabawi YA, Oikonomou EK, Dey AK, Mancio J, Rodante JA, Aksentijevich M, Choi H, Keel A, Erb-Alvarez J, Teague HL, Joshi AA, Playford MP, Lockshin B, Choi AD, Gelfand JM, Chen MY, Bluemke DA, Shirodaria C, Antoniades C, Mehta NN (2019) Association of biologic therapy with coronary inflammation in patients with psoriasis as assessed by perivascular fat attenuation index. JAMA Cardiol 4:885–891
Thampanitchawong P, Piratvisuth T (1999) Liver biopsy:complications and risk factors. World J Gastroenterol 5:301–304
Acknowledgements
None.
Funding
This work was supported by the Japan Society for the Promotion of Science KAKENHI (Grant Number JP 21K16024).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no conflicts of interest regarding the materials presented in this article.
Ethics approval
This study was conducted according to the principles expressed in the Declaration of Helsinki and was approved by the institutional review board of the Okayama University Graduate School of Medicine. All the enrolled patients provided written informed consent to participate.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ichikawa, K., Miyoshi, T., Nakashima, M. et al. Prognostic value of pericoronary adipose tissue attenuation in patients with non-alcoholic fatty liver disease with suspected coronary artery disease. Heart Vessels 37, 1977–1984 (2022). https://doi.org/10.1007/s00380-022-02107-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-022-02107-x