Abstract
Purpose
To investigate the impact of virtual reality (VR) technologies on urological surgeries, specifically in the management of prostate cancer and renal cancer.
Methods
A non-systematic review of the literature was performed. Medline, Pubmed, and the Cochrane Database were screened for studies regarding the use of VR technologies in the management of prostate and renal cancer.
Results
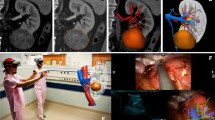
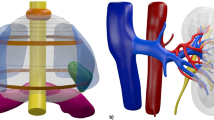
In the management of prostate cancer, VR technologies have been increasingly applied for diagnosis with magnetic resonance imaging/ultrasound fusion biopsy, surgical training using a simulator, surgical navigation in robot-assisted radical prostatectomy, and targeted focal therapy. In partial nephrectomy, surgical simulation and intra-surgical guidance with three-dimensional VR have been used for better understanding of the hilar vascular information, tumor location, and positional relationships of the tumor-feeding vessel and pyelocaliceal system.
Conclusions
VR contributes to the education, training, and simulation of surgical procedures as well as hel** the surgeons to tailor surgical planning on each patient. Further prospective studies are needed to assess the beneficial impacts of this technology for both the physician and patient by objective parameters.





Similar content being viewed by others
References
Bernhardt S, Nicolau SA, Soler L, Doignon C (2017) The status of aug-mented reality in laparoscopic surgery as of 2016. Med Image Anal 37:66–90
Ukimura O, Gill IS, Desai MM, Steinberg AP, Kilciler M, Ng CS, Abreu SC, Spaliviero M, Ramani AP, Kaouk JH, Kawauchi A, Miki T (2004) Real-time transrectal ultrasonography during laparoscopic radical prostatectomy. J Urol 172:112–118
Ukimura O, Magi-Galluzzi C, Gill IS (2006) Real-time transrectal ultrasound guidance during nerve-sparing laparoscopic radical prostatectomy: Impact on surgical margins. J Urol 175:1304–1310
Gill IS, Ukimura O (2007) Thermal energy-free laparoscopic nerve-sparing radical prostatectomy: one-year potency outcomes. Urology 70:309–314
Ukimura O, Troncoso P, Ramirez EI, Babaian RJ (1998) Prostate cancer staging: correlation between ultrasound determined tumor contact length and pathologically confirmed extraprostatic extension. J Urol 159:1251–1259
Ukimura O, Desai M, Palmer S, Valencerina S, Gross M, Abreu A, Aron M, Gill IS (2012) Three-dimensional elastic registration system of prostate biopsy location by real-time 3-dimensional transrectal ultrasound guidance with magnetic resonance/transrectal ultrasound image fusion. J Urol 187:1080–1086
Ukimura O, Abreu AL, Gill IS, Shoji S, Hung AJ, Bahn D (2013) Image-visibility of cancer to enhance targeting precision and spatial map** biopsy for focal therapy of prostate cancer. BJU Int 111(8):E354–E364
Ukimura O, Marien A, Palmer S et al (2015) Trans-rectal ultrasound visibility of prostate lesions identified by magnetic resonance imaging increases accuracy of image-fusion targeted biopsies. World J Urol 33(11):1669–1676
Baco E, Rud E, Eri LM, Moen G, Vlatkovic L, Svindland A, Eggesbø HB, Ukimura O (2016) A randomized controlled trial to assess and compare the outcomes of two-core prostate biopsy guided by fused magnetic resonance and transrectal ultrasound images and traditional 12-core systematic biopsy. Eur Urol 69(1):149–156
Shin T, Smyth TB, Ukimura O, Ahmadi N, de Castro Abreu AL, Ohe C, Oishi M, Mimata H, Gill IS (2018) Diagnostic accuracy of a five-point Likert scoring system for magnetic resonance imaging (MRI) evaluated according to results of MRI/ultrasonography image-fusion targeted biopsy of the prostate. BJU Int 121(1):77–83
Chalasani V, Cool DW, Sherebrin S, Fenster A, Chin J, Izawa JI (2011) Devel- opment and validation of a virtual reality transrectal ultrasound guided prostatic biopsy simulator. Can Urol Assoc J 5:19–26
Fiard G, Selmi SY, Promayon E, Vadcard L, Descotes JL, Troccaz J (2014) Initial validation of a virtual-reality learning environment for pros-tate biopsies: realism matters! J Endourol 28:453–458
Fiard G, Selmi SY, Promayon E, Descotes JL, Troccaz J (2019) Simulation-based training for prostate biopsies: towards the validation of the Biopsym simulator [published online ahead of print]. Minim Inva- sive Ther Allied Technol. https://doi.org/10.1080/13645706.2019.1653926
Yoshida S, Taniguchi N, Moriyama S, Matsuoka Y, Saito K, Fujii Y (2020) Application of virtual reality in patient explanation of magnetic resonance imaging-ultrasound fusion prostate biopsy. Int J Urol 27:471–472
Ukimura O, Gill IS (2008) Imaging-assisted endoscopic surgery: Cleveland Clinic experience. J Endourol 22:803–810
Kang SG et al (2014) The Tube 3 module designed for practicing vesicourethral anastomosis in a virtual reality robotic simulator: determination of face, content, and construct validity. Urology 84(2):345–350
Setty Y, Salzman O (2016) A methodological, task-based approach to procedure-specific simulations training. Int J CARS 11:2317–2324. https://doi.org/10.1007/s11548-016-1450-z
Harrison P et al (2018) The validation of a novel robot-assisted radical prostatectomy virtual reality module. J Surg Educ 75(3):758–766
Ukimura O, Aron M, Nakamoto M, Shoji S, Abreu AL, Matsugasumi T, Berger A, Desai M, Gill IS (2014) Three-dimensional surgical navigation model with TilePro display during robot-assisted radical prostatectomy. J Endourol 28(6):625–630
Shin T, Ukimura O, Gill IS (2016) Three-dimensional printed model of prostate anatomy and targeted biopsy-proven index tumor to facilitate nerve-sparing prostatectomy. Eur Urol 69(2):377–379
Mehralivand S et al (2019) A multiparametric magnetic resonance imaging-based virtual reality surgical navigation tool for robotic-assisted radical prostatectomy. Turk J Urol 45(5):357
Samei G et al (2020) A partial augmented reality system with live ultrasound and registered preoperative MRI for guiding robot-assisted radical prostatectomy. Med Image Anal 60:101588
Porpiglia F, Checcucci E, Amparore D et al (2019) Three-dimensional elastic augmented-reality robot-assisted radical prostatectomy using hyperaccuracy three-dimensional reconstruction technology: a step further in the identification of capsular involvement. Eur Urol 76:505–514. https://doi.org/10.1016/j.eururo.2019.03.037
Schiavina R, Bianchi L, Lodi S et al (2020) Real-time augmented reality three-dimensional guided robotic radical prostatectomy: preliminary experience and evaluation of the impact on surgical planning. Eur Urol Focus S2405–4569(20):30217. https://doi.org/10.1016/j.euf.2020.08.004
Ukimura O et al (2008) Real-time virtual ultrasonographic radiofrequency ablation of renal cell carcinoma. BJU Int 101(6):707–711
Ukimura O, Nakamoto M, Gill IS (2012) Three-dimensional reconstruction of renovascular-tumor anatomy to facilitate zero-ischemia partial nephrectomy. Eur Urol 61(1):211–217
Porpiglia F, Fiori C, Checcucci E, Amparore D, Bertolo R (2018) Hyperaccuracy three-dimensional reconstruction is able to maximize the efficacy of selective clam** during robot-assisted partial nephrectomy for complex renal masses. Eur Urol 74:651–660
Ueno D, Makiyama K, Yamanaka H, Ijiri T, Yokota H, Kubota Y (2014) Prediction of open urinary tract in laparoscopic partial nephrectomy by virtual resection plane visualization. BMC Urol 14(1):1–6
Kobayashi S, Cho B, Huaulume A et al (2019) Assessment of surgical skills by using surgical navigation in robot-assisted partial nephrectomy. Int J Comput Assist Radiol Surg 148:1449–1459
Shirk JD, Thiel DD, Wallen EM, Linehan JM, White WM, Badani KK, Porter JR (2019) Effect of 3-dimensional virtual reality models for surgical planning of robotic-assisted partial nephrectomy on surgical outcomes: a randomized clinical trial. JAMA Netw Open 2(9):e1911598. https://doi.org/10.1001/jamanetworkopen.2019.11598 (PMID: 31532520; PMCID: PMC6751754)
Hyde ER, Berger LU, Ramachandran N, Hughes-Hallett A, Pavithran NP, Tran MGB, Ourselin S, Bex A, Mumtaz FH (2019) Interactive virtual 3D models of renal cancer patient anatomies alter partial nephrectomy surgical planning decisions and increase surgeon confidence compared to volume-rendered images. Int J Comput Assist Radiol Surg 14(4):723–732
Bertolo R, Autorino R, Fiori C et al (2019) Expanding the indications of robotic partial nephrectomy for highly complex renal tumors: urologists’ perception of the impact of hyperaccuracy three-dimensional reconstruction. J Laparoendosc Adv Surg Tech A 29:233–239. https://doi.org/10.1089/lap.2018.0486
Saito Yu et al (2020) Intraoperative 3D hologram support with mixed reality techniques in liver surgery. Ann Surg 271(1):e4–e7
Yamada Y, Inoue Y, Kaneko M, Fujihara A, Hongo F, Ukimura O (2019) Virtual reality of three-dimensional surgical field for surgical planning and intraoperative management. Int J Uol 26(9):942–943
Yoshida S, Sugimoto M, Fukuda S, Taniguchi N, Saito K, Fujii Y (2019) Mixed reality computed tomography-based surgical planning for partial nephrectomy using a head-mounted holographic computer. Int J Uol 26:681–682
Antonelli A, Veccia A, Palumbo C, Peroni A, Mirabella G, Cozzoli A, Martucci P, Ferrari F, Simeone C, Artibani W (2019) Holographic reconstructions for preoperative planning before partial nephrectomy: a head-to-head comparison with standard CT scan. Urol Int 102(2):212–217. https://doi.org/10.1159/000495618 (Epub 2018 Dec 12 PMID: 30540991)
Author information
Authors and Affiliations
Contributions
AF: Drafting the article. OU: Critical revision of the article for important intellectual content.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving Human Participants and/or Animals
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fujihara, A., Ukimura, O. Virtual reality of three-dimensional surgical field for surgical planning and intraoperative management. World J Urol 40, 687–696 (2022). https://doi.org/10.1007/s00345-021-03841-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-021-03841-z