Abstract
Objective
To investigate whether artificial intelligence–based computer-aided diagnosis (AI-CAD) can improve radiologists’ performance when used to support radiologists’ interpretation of digital mammography (DM) in breast cancer screening.
Methods
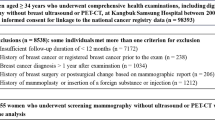
A retrospective database search identified 3158 asymptomatic Korean women who consecutively underwent screening DM between January and December 2019 without AI-CAD support, and screening DM between February and July 2020 with image interpretation aided by AI-CAD in a tertiary referral hospital using single reading. Propensity score matching was used to match the DM with AI-CAD group in a 1:1 ratio with the DM without AI-CAD group according to age, breast density, experience level of the interpreting radiologist, and screening round. Performance measures were compared with the McNemar test and generalized estimating equations.
Results
A total of 1579 women who underwent DM with AI-CAD were matched with 1579 women who underwent DM without AI-CAD. Radiologists showed higher specificity (96% [1500 of 1563] vs 91.6% [1430 of 1561]; p < 0.001) and lower abnormal interpretation rates (AIR) (4.9% [77 of 1579] vs 9.2% [145 of 1579]; p < 0.001) with AI-CAD than without. There was no significant difference in the cancer detection rate (CDR) (AI-CAD vs no AI-CAD, 8.9 vs 8.9 per 1000 examinations; p = 0.999), sensitivity (87.5% vs 77.8%; p = 0.999), and positive predictive value for biopsy (PPV3) (35.0% vs 35.0%; p = 0.999) according to AI-CAD support.
Conclusions
AI-CAD increases the specificity for radiologists without decreasing sensitivity as a supportive tool in the single reading of DM for breast cancer screening.
Clinical relevance statement
This study shows that AI-CAD could improve the specificity of radiologists’ DM interpretation in the single reading system without decreasing sensitivity, suggesting that it can benefit patients by reducing false positive and recall rates.
Key Points
• In this retrospective-matched cohort study (DM without AI-CAD vs DM with AI-CAD), radiologists showed higher specificity and lower AIR when AI-CAD was used to support decision-making in DM screening.
• CDR, sensitivity, and PPV for biopsy did not differ with and without AI-CAD support.



Similar content being viewed by others
Abbreviations
- AI-CAD:
-
Artificial intelligence-based computer-aided diagnosis
- AIR:
-
Abnormal interpretation rate
- BI-RADS:
-
Breast Imaging Reporting and Data System
- CDR:
-
Cancer detection rate
- DM:
-
Digital mammography
- PPV:
-
Positive predictive value
References
Duffy SW, Vulkan D, Cuckle H et al (2020) Effect of mammographic screening from age 40 years on breast cancer mortality (UK Age trial): final results of a randomised, controlled trial. Lancet Oncol 21:1165–1172
Lauby-Secretan B, Scoccianti C, Loomis D et al (2015) Breast-cancer screening–viewpoint of the IARC Working Group. N Engl J Med 372:2353–2358
Schünemann HJ, Lerda D, Quinn C et al (2020) Breast cancer screening and diagnosis: a synopsis of the european breast guidelines. Ann Intern Med 172:46–56
Pisano ED, Gatsonis C, Hendrick E et al (2005) Diagnostic performance of digital versus film mammography for breast-cancer screening. N Engl J Med 353:1773–1783
Hong S, Song SY, Park B et al (2020) Effect of digital mammography for breast cancer screening: a comparative study of more than 8 million Korean women. Radiology 294:247–255
Prummel MV, Muradali D, Shumak R et al (2016) Digital compared with screen-film mammography: measures of diagnostic accuracy among women screened in the ontario breast screening program. Radiology 278:365–373
Kerlikowske K, Hubbard RA, Miglioretti DL et al (2011) Comparative effectiveness of digital versus film-screen mammography in community practice in the United States: a cohort study. Ann Intern Med 155:493–502
Majid AS, de Paredes ES, Doherty RD, Sharma NR, Salvador X (2003) Missed breast carcinoma: pitfalls and pearls. Radiographics 23:881–895
Houssami N, Hunter K (2017) The epidemiology, radiology and biological characteristics of interval breast cancers in population mammography screening. NPJ Breast Cancer 3:12
Lehman CD, Arao RF, Sprague BL et al (2017) National performance benchmarks for modern screening digital mammography: update from the Breast Cancer Surveillance Consortium. Radiology 283:49–58
Giess CS, Wang A, Ip IK, Lacson R, Pourjabbar S, Khorasani R (2019) Patient, radiologist, and examination characteristics affecting screening mammography recall rates in a large academic practice. J Am Coll Radiol 16:411–418
Wing P, Langelier MH (2009) Workforce shortages in breast imaging: impact on mammography utilization. AJR Am J Roentgenol 192:370–378
Rodriguez-Ruiz A, Lång K, Gubern-Merida A et al (2019) Stand-alone artificial intelligence for breast cancer detection in mammography: comparison with 101 radiologists. J Natl Cancer Inst 111:916–922
Yoon JH, Kim EK (2021) Deep learning-based artificial intelligence for mammography. Korean J Radiol 22:1225–1239
Kim HE, Kim HH, Han BK et al (2020) Changes in cancer detection and false-positive recall in mammography using artificial intelligence: a retrospective, multireader study. Lancet Digit Health 2:e138–e148
McKinney SM, Sieniek M, Godbole V et al (2020) International evaluation of an AI system for breast cancer screening. Nature 577:89–94
Rodriguez-Ruiz A, Krupinski E, Mordang JJ et al (2019) Detection of breast cancer with mammography: effect of an artificial intelligence support system. Radiology 290:305–314
Pacile S, Lopez J, Chone P, Bertinotti T, Grouin JM, Fillard P (2020) Improving breast cancer detection accuracy of mammography with the concurrent use of an artificial intelligence tool. Radiol Artif Intell 2:e190208
Watanabe AT, Lim V, Vu HX et al (2019) Improved cancer detection using artificial intelligence: a retrospective evaluation of missed cancers on mammography. J Digit Imaging 32:625–637
Larsen M, Aglen CF, Hoff SR, Lund-Hanssen H, Hofvind S (2022) Possible strategies for use of artificial intelligence in screen-reading of mammograms, based on retrospective data from 122,969 screening examinations. Eur Radiol 32:8238–8246
Romero-Martin S, Elias-Cabot E, Raya-Povedano JL, Gubern-Merida A, Rodriguez-Ruiz A, Alvarez-Benito M (2022) Stand-alone use of artificial intelligence for digital mammography and digital breast tomosynthesis screening: a retrospective evaluation. Radiology 302:535–542
Salim M, Wåhlin E, Dembrower K et al (2020) External evaluation of 3 commercial artificial intelligence algorithms for independent assessment of screening mammograms. JAMA Oncol 6:1581–1588
Freeman K, Geppert J, Stinton C et al (2021) Use of artificial intelligence for image analysis in breast cancer screening programmes: systematic review of test accuracy. BMJ 374:n1872
Lee SE, Han K, Yoon JH, et al (2022) Depiction of breast cancers on digital mammograms by artificial intelligence-based computer-assisted diagnosis according to cancer characteristics. Eur Radiol 32:7400–7408. https://doi-doiorg.libproxy.samsunghospital.com/10.1007/s00330-022-08718-2
Sickles EA, D’Orsi CJ, Bassett LW, Appleton CM, Berg WA, Burnside ES (2013) ACR BI-RADS® Atlas, Breast imaging reporting and data system. Reston, VA: American College of Radiology 39–48
Yi C, Tang Y, Ouyang R et al (2022) The added value of an artificial intelligence system in assisting radiologists on indeterminate BI-RADS 0 mammograms. Eur Radiol 32:1528–1537
Lang K, Dustler M, Dahlblom V, Akesson A, Andersson I, Zackrisson S (2021) Identifying normal mammograms in a large screening population using artificial intelligence. Eur Radiol 31:1687–1692
Raya-Povedano JL, Romero-Martin S, Elias-Cabot E, Gubern-Merida A, Rodriguez-Ruiz A, Alvarez-Benito M (2021) AI-based strategies to reduce workload in breast cancer screening with mammography and tomosynthesis: a retrospective evaluation. Radiology 300:57–65
Yala A, Schuster T, Miles R, Barzilay R, Lehman C (2019) A Deep learning model to triage screening mammograms: a simulation study. Radiology 293:38–46
Shaw CM, Flanagan FL, Fenlon HM, McNicholas MM (2009) Consensus review of discordant findings maximizes cancer detection rate in double-reader screening mammography: Irish National Breast Screening Program experience. Radiology 250:354–362
Hofvind S, Geller BM, Rosenberg RD, Skaane P (2009) Screening-detected breast cancers: discordant independent double reading in a population-based screening program. Radiology 253:652–660
Taylor P, Potts HW (2008) Computer aids and human second reading as interventions in screening mammography: two systematic reviews to compare effects on cancer detection and recall rate. Eur J Cancer 44:798–807
Perry N, Broeders M, de Wolf C, Törnberg S, Holland R, von Karsa L (2008) European guidelines for quality assurance in breast cancer screening and diagnosis. Fourth edition–summary document. Ann Oncol 19:614–622
Dinnes J, Moss S, Melia J, Blanks R, Song F, Kleijnen J (2001) Effectiveness and cost-effectiveness of double reading of mammograms in breast cancer screening: findings of a systematic review. Breast 10:455–463
Posso MC, Puig T, Quintana MJ, Sola-Roca J, Bonfill X (2016) Double versus single reading of mammograms in a breast cancer screening programme: a cost-consequence analysis. Eur Radiol 26:3262–3271
Taplin SH, Rutter CM, Elmore JG, Seger D, White D, Brenner RJ (2000) Accuracy of screening mammography using single versus independent double interpretation. AJR Am J Roentgenol 174:1257–1262
Lang K, Hofvind S, Rodriguez-Ruiz A, Andersson I (2021) Can artificial intelligence reduce the interval cancer rate in mammography screening? Eur Radiol 31:5940–5947
Boyd NF, Guo H, Martin LJ et al (2007) Mammographic density and the risk and detection of breast cancer. N Engl J Med 356:227–236
Miglioretti DL, Gard CC, Carney PA et al (2009) When radiologists perform best: the learning curve in screening mammogram interpretation. Radiology 253:632–640
Sala M, Comas M, Macià F, Martinez J, Casamitjana M, Castells X (2009) Implementation of digital mammography in a population-based breast cancer screening program: effect of screening round on recall rate and cancer detection. Radiology 252:31–39
Kim YJ, Lee EH, Jun JK et al (2017) Analysis of participant factors that affect the diagnostic performance of screening mammography: a report of the Alliance for Breast Cancer Screening in Korea. Korean J Radiol 18:624–631
Lee EH, Kim KW, Kim YJ et al (2016) Performance of screening mammography: a report of the Alliance for Breast Cancer Screening in Korea. Korean J Radiol 17:489–496
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Ji Soo Choi.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
One of the authors has significant statistical expertise: Kyunga Kim.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
This retrospective study received ethical approval from the Institutional Review Board of Samsung Medical Center (IRB File No.: SMC 2021-06-011).
Study subjects or cohorts overlap
Not applicable.
Methodology
-
retrospective
-
diagnostic or prognostic study
-
performed at one institution
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kim, H., Choi, J.S., Kim, K. et al. Effect of artificial intelligence–based computer-aided diagnosis on the screening outcomes of digital mammography: a matched cohort study. Eur Radiol 33, 7186–7198 (2023). https://doi.org/10.1007/s00330-023-09692-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-023-09692-z