Abstract
Background
Current studies did not draw definitive conclusions on comparison of intracorporeal anastomosis (ICA) with extracorporeal anastomosis (ECA) in laparoscopic right colectomy. Whether the intraperitoneal contamination induced by ICA can result in higher risk of postoperative abdominal infection remains unclear. This study was aimed to compare the short-term outcomes, especially the risk of abdominal infection after ICA versus ECA.
Methods
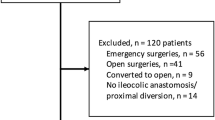
This was an observational cohort study as a secondary analysis of a randomized controlled trial (RCT)—RELARC trial (NCT02619942). The patients enrolled in the RELARC trial were diagnosed with primary colon adenocarcinoma without distant metastasis and underwent radical laparoscopic right colectomy between Jan 2016 and Dec 2019. In our study the patients who converted to open surgery in RELARC trial were excluded. The short-term outcomes were compared between ICA and ECA. The primary endpoint was abdominal infection. The inverse probability of treatment weighting (IPTW) and propensity score matching (PSM) was used for adjusting the potential confounders.
Results
This study enrolled 975 patients with 119 patients undergoing ICA and 856 patients undergoing ECA. The incidence of abdominal infection was higher in ICA group (9.2% versus 1.5%, RR from IPTW = 5.7 (95%CI: 2.6–12.6), P < 0.001) as well as the incidence of wound infection (14.3% vs 3.3%, RR from IPTW = 5.0 (95%CI: 2.9–8.6), P < 0.001). ICA was associated with higher incidence of Clavien–Dindo (CD) grade I and II complications (CD-I: 15.1% versus 6.8%, RR from IPTW = 2.4 (95%CI: 1.5–3.9), P < 0.001; CD-II: 26.9% versus 8.2%, RR from IPTW = 3.6 (95%CI: 2.5–5.1), P < 0.001) but similar incidence of CD-III ~ IV complications compared to ECA (3.4% vs 2.1%, RR from IPTW = 1.2 (95%CI: 0.4–4.0), P = 0.73). In ICA group, choosing another incision rather than lengthening main port site decreased the incidence of wound infection although without statistical significance (17.3% (14/81) versus 7.9% (3/38), crude RR = 2.2 (95%CI: 0.7–7.2), P = 0.17).
Conclusion
ICA is likely to be associated with higher risk of abdominal infection and CD-I ~ II complications.

Similar content being viewed by others
References
Bollo J et al (2020) Randomized clinical trial of intracorporeal versus extracorporeal anastomosis in laparoscopic right colectomy (IEA trial). Br J Surg 107(4):364–372
DeSouza A et al (2011) Incisional hernia, midline versus low transverse incision: what is the ideal incision for specimen extraction and hand-assisted laparoscopy? Surg Endosc 25(4):1031–1036
Lee L et al (2018) Incisional hernia after midline versus transverse specimen extraction incision: a randomized trial in patients undergoing laparoscopic colectomy. Ann Surg 268(1):41–47
Lendzion RJ, Gilmore AJ (2021) Laparoscopic right hemicolectomy with intracorporeal anastomosis and natural orifice surgery extraction/minimal extraction site surgery in the obese. ANZ J Surg 91(6):1180–1184
Allaix ME et al (2019) Intracorporeal or extracorporeal ileocolic anastomosis after laparoscopic right colectomy: a double-blinded randomized controlled trial. Ann Surg 270(5):762–767
Ferrer-Marquez M et al (2021) Intracorporeal versus extracorporeal anastomosis in patients undergoing laparoscopic right hemicolectomy: a multicenter randomized clinical trial (The IVEA-study). Surg Laparosc Endosc Percutan Tech 31(4):408–413
Anania G et al (2020) Laparoscopic right hemicolectomy: the SICE (Societa Italiana di Chirurgia Endoscopica e Nuove Tecnologie) network prospective trial on 1225 cases comparing intra corporeal versus extra corporeal ileo-colic side-to-side anastomosis. Surg Endosc 34(11):4788–4800
Aiolfi A et al (2020) Intracorporeal versus extracorporeal anastomosis in laparoscopic right colectomy: an updated systematic review and cumulative meta-analysis. J Laparoendosc Adv Surg Tech A 30(4):402–412
Widmar M et al (2020) Intracorporeal anastomoses in minimally invasive right colectomies are associated with fewer incisional hernias and shorter length of stay. Dis Colon Rectum 63(5):685–692
Ishizaki T et al (2021) Comparison of intra-abdominal infection risk between intracorporeal and extracorporeal anastomosis in laparoscopic right hemicolectomy for colon cancer: a single-center retrospective study. Am Surg 87(3):341–346
Vandenbroucke JP et al (2007) Strengthening the reporting of observational studies in epidemiology (STROBE): explanation and elaboration. PLoS Med 4(10):e297
Lu JY et al (2016) The radical extent of lymphadenectomy - D2 dissection versus complete mesocolic excision of laparoscopic right colectomy for right-sided colon cancer (RELARC) trial: study protocol for a randomized controlled trial. Trials 17(1):582
Xu L et al (2021) Short-term outcomes of complete mesocolic excision versus D2 dissection in patients undergoing laparoscopic colectomy for right colon cancer (RELARC): a randomised, controlled, phase 3, superiority trial. Lancet Oncol 22(3):391–401
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Austin PC, Stuart EA (2015) Moving towards best practice when using inverse probability of treatment weighting (IPTW) using the propensity score to estimate causal treatment effects in observational studies. Stat Med 34(28):3661–3679
Austin PC (2016) Variance estimation when using inverse probability of treatment weighting (IPTW) with survival analysis. Stat Med 35(30):5642–5655
Mar R-G et al (2013) Model building in nonproportional hazard regression. Stat Med 32:5301–5314
Huimin L et al (2015) Statistical inference methods for two crossing survival curves: a comparison of methods. PLoS One 10:e0116774
Bertelsen CA et al (2016) Short-term outcomes after complete mesocolic excision compared with “conventional” colonic cancer surgery. Br J Surg 103(5):581–589
Yamamoto S et al (2014) Short-term surgical outcomes from a randomized controlled trial to evaluate laparoscopic and open D3 dissection for stage II/III colon cancer: Japan clinical oncology group study JCOG 0404. Ann Surg 260(1):23–30
Lee KH et al (2016) Comparison of anastomotic configuration after laparoscopic right hemicolectomy under enhanced recovery program: side-to-side versus end-to-side anastomosis. Surg Endosc 30(5):1952–1957
Selvy M et al (2020) Intra-versus extracorporeal anastomosis in laparoscopic right colectomy: a meta-analysis of 3699 patients. Int J Colorectal Dis 35(9):1673–1680
Emile SH et al (2019) Intracorporeal versus extracorporeal anastomosis in minimally invasive right colectomy: an updated systematic review and meta-analysis. Tech Coloproctol 23(11):1023–1035
Hanna MH et al (2016) Laparoscopic right hemicolectomy: short- and long-term outcomes of intracorporeal versus extracorporeal anastomosis. Surg Endosc 30(9):3933–3942
Acknowledgements
The authors acknowledge Dr. Hao Zhao for statistical analysis in R. RELARC Study Group: Lai Xu, **angqian Su, **angqian He, **angqian Zhang, **angqian Lu, Lei Chen, Guannan Zhang, Bo Feng, Lu Zang, Junjun Ma, Yueming Sun, Yifei Feng, Dongjian Ji, **aohui Du, Changzheng He, Ze Fu, Pan Chi, Ying Huang, Weizhong Jiang, Ziqiang Wang, Qingbin Wu, Ming Zhong, Minhao Yu, Aiwen Wu, Pengju Chen, Anlong Zhu, Wenlong Guan, Bin Wu, Fei Li, Ang Li, Jianmin Xu, Guodong He, Liang Kang, **aowen He, Jian Suo, Daguang Wang, Haijun Deng, Yanan Wang, Yingjiang Ye, Kai Shen, Guole Lin, Hongwei Yao, Huizhong Qiu, Kefeng Ding, Tao Xu, Zhiyong Liang, Weixun Zhou, Huadan Xue, Bin Li, Zhongtao Zhang, Minhua Zheng, Yi **ao.
Funding
Funding for the study was provided by the Capital Characteristic Clinical Project of Bei**g Municipal Science & Technology Commission (Z161100000516014), the Non-profit Central Research Institute Fund of the Chinese Academy of Medical Sciences (2019XK320003) and National Natural Science Foundation of China (Project No. 62172437).
Author information
Authors and Affiliations
Consortia
Corresponding authors
Ethics declarations
Conflict of interest
There is no personal conflicts of interest or financial conflicts of interest of any of the authors.
Ethics approval
This research was performed as a sub-study of RELARC trial (NCT02619942). The RELARC study protocol and all amendments were approved by the Ethics Committee of Peking Union Medical College Hospital. Patient consent was acquired before enrollment.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix
Appendix
The packages used in R included MatchIt, reportReg, tableone, survey, reshape2, ggplot2, foreign, survival, survminer, table1, riskRegression, epiR, epitools, pwr, Rcpp, base and ComparisonSurv.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sun, R., Zhang, Y., Feng, B. et al. Intracorporeal Anastomosis Versus Extracorporeal Anastomosis in Laparoscopic Right Colectomy: An Observational Cohort Study. World J Surg 47, 785–795 (2023). https://doi.org/10.1007/s00268-022-06834-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-022-06834-0