Abstract
Background
Determining whether prompt surgery is required for patient with ingested foreign bodies is clinically important.
Purpose
To evaluate the potential value of computed tomography (CT) in guiding the selection of surgical treatment for patients with ingested foreign bodies in the lower gastrointestinal tract.
Methods
Between January 2014 and December 2023, we analyzed the data of 58 patients (median age: 65.4 years; range, 31–96 years) with ingested foreign bodies in the lower gastrointestinal tract who underwent CT examinations. Patients were treated either conservatively (35 cases) or surgically (23 cases). The angle between the long axis of the foreign body and the intestinal canal (FB-IC angle) was measured. CT findings and clinical variables were evaluated to identify potential indicators for surgical treatment through univariate and multivariate logistic regression analyses.
Results
Univariate analysis revealed the FB-IC angle (P = 0.002), presence of free peritoneal gas (P = 0.002), white blood cell count (P = 0.018), and neutrophil count (P = 0.007) as significant factors associated with surgical treatment. Multivariate analysis demonstrated that the FB-IC angle (odds ratio, 1.033; P = 0.045) and the presence of free peritoneal gas (odds ratio, 41.335; P = 0.002) are independent indicators for surgical management. The FB-IC angle showed an area under the receiver operating characteristic curve of 0.755, with a cutoff value of 51.25 degrees.
Conclusion
The FB-IC angle and presence of free peritoneal gas serve as potential predictive imaging markers for surgical intervention.
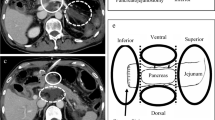
Graphical Abstract








Similar content being viewed by others
References
V. Selivanov, G.F. Sheldon, J.P. Cello, R.A. Crass, Management of foreign body ingestion, Ann Surg 199(2) (1984) 187-91.
G. Bathla, L.L. Teo, S. Dhanda, Pictorial essay: Complications of a swallowed fish bone, Indian J Radiol Imaging 21(1) (2011) 63-8.
X. Wang, J. Zhao, Y. Jiao, X. Wang, D. Jiang, Upper gastrointestinal foreign bodies in adults: A systematic review, Am J Emerg Med 50 (2021) 136-141.
D.E. McCanse, A. Kurchin, J.R. Hinshaw, Gastrointestinal foreign bodies, Am J Surg 142(3) (1981) 335-7.
M. Guelfguat, V. Kaplinskiy, S.H. Reddy, J. DiPoce, Clinical guidelines for imaging and reporting ingested foreign bodies, AJR Am J Roentgenol 203(1) (2014) 37-53.
M. Hashmonai, T. Kaufman, A. Schramek, Silent perforations of the stomach and duodenum by needles, Arch Surg 113(12) (1978) 1406-9.
W. Cheng, P.K. Tam, Foreign-body ingestion in children: experience with 1,265 cases, J Pediatr Surg 34(10) (1999) 1472-6.
P. Ambe, S.A. Weber, M. Schauer, W.T. Knoefel, Swallowed Foreign Bodies in Adults, Deutsches Ärzteblatt international 109(50) (2012) 869.
G. Gayer, I. Petrovitch, R.B. Jeffrey, Foreign objects encountered in the abdominal cavity at CT, Radiographics 31(2) (2011) 409-28.
B.K. Goh, Y.M. Tan, S.E. Lin, P.K. Chow, F.K. Cheah, L.L. Ooi, W.K. Wong, CT in the preoperative diagnosis of fish bone perforation of the gastrointestinal tract, AJR Am J Roentgenol 187(3) (2006) 710-4.
T.S. Paixao, R.V. Leao, N. de Souza Maciel Rocha Horvat, P.C. Viana, C. Da Costa Leite, R.L. de Azambuja, R.S. Damasceno, C.D. Ortega, M.R. de Menezes, G.G. Cerri, Abdominal manifestations of fishbone perforation: a pictorial essay, Abdom Radiol (NY) 42(4) (2017) 1087-1095.
H.M. Noh, F.S. Chew, Small-bowel perforation by a foreign body, AJR Am J Roentgenol 171(4) (1998) 1002.
M.A. Deniz, M. Turmak, CT Evaluation of Swallowed Foreign Bodies Located in the Gastrointestinal System, Cureus 14(6) (2022) e26355.
A. Mutlu, E. Uysal, L. Ulusoy, C. Duran, D. Selamoglu, A fish bone causing ileal perforation in the terminal ileum, Turkish Journal of Trauma and Emergency Surgery 18(1) (2012) 89-91.
E.S. GS, N.B.N. Gomes, E.O. Pacheco, F.M.R. Bezerra, R.B. Nunes, H.L. McPhee, U.S. Torres, G. D'Ippolito, Emergency CT of abdominal complications of ingested fish bones: what not to miss, Emerg Radiol 28(1) (2021) 165-170.
J.F. Cohen, D.A. Korevaar, D.G. Altman, D.E. Bruns, C.A. Gatsonis, L. Hooft, L. Irwig, D. Levine, J.B. Reitsma, H.C. de Vet, P.M. Bossuyt, STARD 2015 guidelines for reporting diagnostic accuracy studies: explanation and elaboration, BMJ Open 6(11) (2016) e012799.
M. de la Vega, J.C. Rivero, L. Ruiz, S. Suarez, A fish bone in the liver, Lancet 358(9286) (2001) 982.
D. Ji, J.D. Lu, Z.G. Zhang, X.P. Mao, Misdiagnosis of food-borne foreign bodies outside of the digestive tract on magnetic resonance imaging: Two case reports, World J Clin Cases 11(7) (2023) 1650-1655.
T. Hu, J. Zhang, Y. Liu, L. Chen, W. Cen, W. Wu, Q. Huang, X. Sun, S. Stock, M. Zippi, V. Zimmer, Z. Basharat, W. Hong, Evaluation of the risk factors for severe complications and surgery of intestinal foreign bodies in adults: a single-center experience with 180 cases, Gastroenterol Rep (Oxf) 10 (2022) goac036.
R.B. Jeffrey, M.P. Federle, S. Wall, Value of computed tomography in detecting occult gastrointestinal perforation, J Comput Assist Tomogr 7(5) (1983) 825-7.
A. P. Madrona, Intestinal perforation by foreign bodies. The European journal of surgery: Acta chirurgica, 166(4) (2000) 307-309.
A.J. Del Gaizo, C. Lall, B.C. Allen, J.R. Leyendecker, From esophagus to rectum: a comprehensive review of alimentary tract perforations at computed tomography, Abdom Imaging 39(4) (2014) 802-23.
A. Lambert, Abscess of the liver of unusual origin, NY Med J 2 (1898) 177–178.
Funding
Supported by Suzhou Science and Technology for Youths for Promoting Health through Science and Education Project, No. KJXW2023064. Supported by Jiangsu Medical Vocational College Campus Collaborative Innovation Research Project, No. 20239604.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, L., Chen, XY., Ji, D. et al. Foreign body-intestinal canal angle guides management of ingested foreign bodies in the lower gastrointestinal tract. Abdom Radiol (2024). https://doi.org/10.1007/s00261-024-04404-7
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00261-024-04404-7