Abstract
Purpose
To compare the diagnostic performance for detecting vascular involvement and determining resectability differences regarding pancreatic ductal adenocarcinoma (PDAC) between contrast-enhanced CT and MRI.
Methods
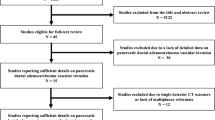
This retrospective study evaluated 82 patients (73 years, 46 men) with PDAC who underwent both preoperative contrast-enhanced CT and MRI from January 2008 to March 2021. Two radiologists independently categorized vascular involvements for celiac, superior mesenteric, splenic, and common hepatic arteries, and portal, superior mesenteric, and splenic veins into no tumor contact, solid soft-tissue contact ≤ 180°, or solid soft-tissue contact > 180°. The radiologists also classified resectability into resectable, borderline resectable, or locally advanced. Receiver-operating-characteristic (ROC) analysis was conducted to evaluate the diagnostic performances for detecting vascular involvements which were confirmed by pathological or intraoperative findings. The proportion of resectability classifications was compared between CT and MRI by the Fisher’s exact test.
Results
No statistical difference was found in the diagnostic performances for detecting vascular involvement in CT (area under the ROC curve [AUC], 0.50–0.89) and MRI (AUC, 0.51–0.75) (P = 0.06–> 0.99). Resectability on CT were 79% and 68%, 20% and 26%, and 1% and 6% for resectable, borderline resectable, and locally advanced tumors for reviewers 1 and 2; those on MRI were 87% and 81%, 12% and 13%, and 1% and 6%, respectively. The proportion of resectability classifications was not different between CT and MRI (P = 0.48 and = 0.15 for reviewers 1 and 2, respectively).
Conclusion
The diagnostic performance for detecting vascular involvement and determining resectability of PDAC on contrast-enhanced MRI were comparable with pancreatic protocol CT.



Similar content being viewed by others
References
NCCN clinical practice guidelines in oncology: pancreatic adenocarcinoma, version 2. 2021.
Schima W, Ba-Ssalamah A, Kolblinger C, Kulinna-Cosentini C, Puespoek A, Gotzinger P. Pancreatic adenocarcinoma. Eur Radiol 2007; 17:638-649
Zins M, Matos C, Cassinotto C. Pancreatic Adenocarcinoma Staging in the Era of Preoperative Chemotherapy and Radiation Therapy. Radiology 2018; 287:374-390
Joo I, Lee JM, Lee ES, et al. Preoperative CT Classification of the Resectability of Pancreatic Cancer: Interobserver Agreement. Radiology 2019; 293:343-349
Motosugi U, Ichikawa T, Morisaka H, et al. Detection of pancreatic carcinoma and liver metastases with gadoxetic acid-enhanced MR imaging: comparison with contrast-enhanced multi-detector row CT. Radiology 2011; 260:446-453
Noda Y, Goshima S, Takai Y, et al. Detection of pancreatic ductal adenocarcinoma and liver metastases: comparison of Gd-EOB-DTPA-enhanced MR imaging vs. extracellular contrast materials. Abdom Radiol (NY) 2020; 45:2459-2468
Lee JK, Kim AY, Kim PN, Lee MG, Ha HK. Prediction of vascular involvement and resectability by multidetector-row CT versus MR imaging with MR angiography in patients who underwent surgery for resection of pancreatic ductal adenocarcinoma. Eur J Radiol 2010; 73:310-316
Hanley JA, McNeil BJ. A method of comparing the areas under receiver operating characteristic curves derived from the same cases. Radiology 1983; 148:839-843
Mavros MN, Moris D, Karanicolas PJ, Katz MHG, O'Reilly EM, Pawlik TM. Clinical Trials of Systemic Chemotherapy for Resectable Pancreatic Cancer: A Review. JAMA Surg 2021;
Ichikawa T, Haradome H, Hachiya J, et al. Pancreatic ductal adenocarcinoma: preoperative assessment with helical CT versus dynamic MR imaging. Radiology 1997; 202:655-662
Koelblinger C, Ba-Ssalamah A, Goetzinger P, et al. Gadobenate dimeglumine-enhanced 3.0-T MR imaging versus multiphasic 64-detector row CT: prospective evaluation in patients suspected of having pancreatic cancer. Radiology 2011; 259:757-766
Ahmed SA, Mourad AF, Hassan RA, et al. Preoperative CT staging of borderline pancreatic cancer patients after neoadjuvant treatment: accuracy in the prediction of vascular invasion and resectability. Abdom Radiol (NY) 2021; 46:280-289
Park SJ, Jang S, Han JK, et al. Preoperative assessment of the resectability of pancreatic ductal adenocarcinoma on CT according to the NCCN Guidelines focusing on SMA/SMV branch invasion. Eur Radiol 2021;
Cardia PP, Penachim TJ, Prando A, Torres US, D'Ippolito G. Non-contrast MR angiography using three-dimensional balanced steady-state free-precession imaging for evaluation of stenosis in the celiac trunk and superior mesenteric artery: a preliminary comparative study with computed tomography angiography. Br J Radiol 2017; 90:20170011
Cloyd JM, Heh V, Pawlik TM, et al. Neoadjuvant Therapy for Resectable and Borderline Resectable Pancreatic Cancer: A Meta-Analysis of Randomized Controlled Trials. J Clin Med 2020; 9
Davenport MS, Viglianti BL, Al-Hawary MM, et al. Comparison of acute transient dyspnea after intravenous administration of gadoxetate disodium and gadobenate dimeglumine: effect on arterial phase image quality. Radiology 2013; 266:452-461
Davenport MS, Caoili EM, Kaza RK, Hussain HK. Matched within-patient cohort study of transient arterial phase respiratory motion-related artifact in MR imaging of the liver: gadoxetate disodium versus gadobenate dimeglumine. Radiology 2014; 272:123-131
McClellan TR, Motosugi U, Middleton MS, et al. Intravenous Gadoxetate Disodium Administration Reduces Breath-holding Capacity in the Hepatic Arterial Phase: A Multi-Center Randomized Placebo-controlled Trial. Radiology 2017; 282:361-368
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
AK: Grant support for research activities from Philips, GE Healthcare, and PanCAN. Other authors report no relevant disclosures or conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Noda, Y., Kawai, N., Kaga, T. et al. Vascular involvement and resectability of pancreatic ductal adenocarcinoma on contrast-enhanced MRI: comparison with pancreatic protocol CT. Abdom Radiol 47, 2835–2844 (2022). https://doi.org/10.1007/s00261-022-03581-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-022-03581-7