Abstract
Rationale
Nicotine discontinuation produces behaviors in rats that are congruent with anhedonia, and these symptoms may be related to the devaluation of non-nicotine reinforcers.
Objective
Four separate experiments were performed to explore the parameters surrounding nicotine-induced reinforcer devaluation.
Methods
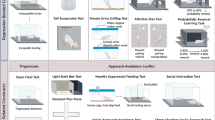
In Experiments 1 and 2, nicotine (0.1 or 0.3 mg/kg) or 0.3 mg/kg nicotine plus 1.0 mg/kg mecamylamine was delivered to rats prior to progressive ratio (PR) schedule sessions in which sucrose was used as a reinforcer. In order to evaluate (a) reinforcer enhancement by nicotine and (b) reinforcer devaluation in the absence of nicotine, all rats experienced two PR schedule sessions per day for 10 days. Experiment 3 involved nicotine (0.3 mg/kg) and a visual stimulus in place of sucrose reinforcement. In Experiment 4, rats received nicotine (0.3 mg/kg) either before or after a single PR schedule session for 10 days.
Results
Experiments 1 and 2 demonstrate that reinforcer devaluation is related to the occupation of nicotinic-acetylcholine receptors. Results from Experiment 3 provide some evidence that devaluation occurs with either sucrose or visual-stimulus reinforcement. Experiment 4 demonstrates that a necessary condition for reinforcer devaluation to occur is the concurrent exposure to the reinforcer and nicotine.
Conclusions
Reinforcer devaluation in rats emerges rapidly in a progressive, orderly fashion that coincides with accumulated exposure to nicotine. These results suggest that reinforcer devaluation may be a feature of nicotine that contributes to the abuse liability of tobacco products.




Similar content being viewed by others
References
Allen SS, Bade T, Hatsukami D, Center B (2008) Craving, withdrawal, and smoking urges on days immediately prior to smoking relapse. Nicotine Tob Res 10:35–45. doi:10.1080/14622200701705076
Arnold J, Roberts D (1997) A critique of fixed and progressive ratio schedules used to examine the neural substrates of drug reinforcement. Pharmacol Biochem Behav 57:441–447. doi:10.1016/S0091-3057(96)00445-5
Baker TB, Brandon TH, Chassin L (2004a) Motivational influences on cigarette smoking. Annu Rev Psychol 55:463–491. doi:10.1146/annurev.psych.55.090902.142054
Baker TB, Piper ME, McCarthy DE, Majeskie MR, Fiore MC (2004b) Addiction motivation reformulated: an affective processing model of negative reinforcement. Psychol Rev 111:33–51. doi:10.1037/0033-295X.111.1.33
Balleine B (1992) Instrumental performance following a shift in primary motivation depends on incentive learning. J Exp Psychol Anim Behav Process 18:236–250. doi:10.1037/0097-7403.18.3.236
Balleine B (2011) Sensation, incentive learning, and the motivational control of goal-directed action. In: Gottfried JA (ed) Neurobiology of sensation and reward. Boca Raton, Florida, chapter 13
Balleine B, Dickinson A (1992) Signalling and incentive processes in instrumental reinforcer devaluation. Q J Exp Psychol B 45:285–301. doi:10.1080/14640749108401271
Barr A, Markou A (2005) Psychostimulant withdrawal as an inducing condition in animal models of depression. Neurosci Biobehav Rev 29:675–706. doi:10.1016/j.neubiorev.2005.03.012
Bruijnzeel AW, Zislis G, Wilson C, Gold M (2007) Antagonism of CRF receptors prevents the deficit in brain reward function associated with precipitated nicotine withdrawal in rats. Neuropsychopharmacology 32:955–963. doi:10.1038/sj.npp.1301192
Bruijnzeel AW, Prado M, Isaac S (2009) Corticotropin-releasing factor-1 receptor activation mediates nicotine withdrawal-induced deficit in brain reward function and stress-induced relapse. Biol Psychiatry 66:110–117. doi:10.1016/j.biopsych.2009.01.010
Bruijnzeel AW, Ford J, Rogers JA, Scheick S, Ji Y, Bishnoi M, Alexander JC (2012) Blockade of CRF1 receptors in the central nucleus of the amygdala attenuates the dysphoria associated with nicotine withdrawal in rats. Pharmacol Biochem Behav 101:62–68. doi:10.1016/j.pbb.2011.12.001
Caggiula A, Donny E, Palmatier M, Lui X, Chaudhri N, Sved A (2009) The role of nicotine in smoking: a dual-reinforcement model. Nebr Symp Motiv 55:91–109
Carton S, Le Houezec J, Lagrue G, Jouvent R (2002) Early emotional disturbances during nicotine patch therapy in subjects with and without a history of depression. J Affect Disord 72:195–199. doi:10.1016/S0165-0327(01)00468-2
Centers for Disease Control and Prevention (2008) Smoking-attributable mortality, years of potential life lost, and productivity losses- United States 2000-2004. Morb Mortal Wkly Rep 57:1226–1228
Chaudhri N, Cagguila A, Donny E, Palmatier M, Liu X, Sved A (2006) Complex interactions between nicotine and nonpharmacological stimuli reveal multiple roles for nicotine in reinforcement. Psychopharmacology (Berl) 184:353–366. doi:10.1007/s00213-005-0178-1
Cook J, Spring B, McChargue D, Doran N (2010) Effects of anhedonia on days to relapse among smokers with a history of depression: a brief report. Nicotine Tob Res 12:978–982. doi:10.1093/ntr/ntq118
Cryan J, Bruijnzeel AW, Skjei K, Markou A (2003) Bupropion enhances brain reward function and reverses the affective and somatic aspects of nicotine withdrawal in the rat. Psychopharmacology (Berl) 168:347–358. doi:10.1007/s00213-003-1445-7
Dar R, Frenk H (2004) Do smokers self-administer pure nicotine? A review of the evidence. Psychopharmacology (Berl) 173(1–2):18–26
Donny EC, Caggiula AR, Mielke MM, Booth S, Gharib MA, Hoffman A, Maldovan V, Shupenk OC, McCallum SE (1999) Nicotine self-administration in rats on a progressive ratio schedule of reinforcement. Psychopharmacology (Berl) 147:135–142. doi:10.1007/s002130051153
Donny EC, Chaudhri N, Caggiula A, Evans-Martin FF, Booth S, Gharib MA, Clements LA, Sved A (2003) Operant responding for a visual reinforcer in rats is enhanced by noncontingent nicotine: implications for nicotine self-administration and reinforcement. Psychopharmacology (Berl) 169:68–76. doi:10.1007/s00213-003-1473-3
Dwoskin L, Smith A, Wooters T, Zhang Z, Crooks P, Bardo M (2009) Nicotinic receptor-based therapeutics and candidates for smoking cessation. Biochem Pharmacol 78:732–743. doi:10.1016/j.bcp.2009.06.002
Ep**-Jordan MP, Watkins SS, Koob GF, Markou A (1998) Dramatic decreases in brain reward function during nicotine withdrawal. Nature 393:76–79. doi:10.1038/30001
Flaherty CF (1997) Incentive relativity New York. Cambridge University Press, NY
Harris A, Manbeck K, Schmidt C, Shelley D (2013) Mecamylamine elicits withdrawal-like signs in rats following a single dose of nicotine. Psychopharmacology (Berl) 225:291–302. doi:10.1007/s00213-012-2814-x
Henningfield JE, Shiffman S, Ferguson SG, Gritz ER (2009) Tobacco dependence and withdrawal: science base, challenges and opportunities for pharmacotherapy. Pharmacol Ther 123:1–16. doi:10.1016/j.pharmthera.2009.03.011
Hogarth L, Balleine B, Corbit L, Killcross S (2013) Associative learning mechanisms underpinning the transition from recreational drug use to addiction. Ann N Y Acad Sci 1282:12–24. doi:10.1111/j.1749-6632.2012.06768.x
Hughes JR (2007) Effects of abstinence from tobacco: etiology, animal models, epidemiology, and significance: a subjective review. Nicotine Tob Res 9:329–339. doi:10.1080/14622200701188927
Hughes JR, Hatsukami DD (1986) Signs and symptoms of tobacco withdrawal. Arch Gen Psychiatry 43:289–294. doi:10.1001/archpsyc.1986.01800030107013
Hughes JR, Hatsukami DK (1992) Signs and symptoms of tobacco withdrawal syndrome: a brief review and update. Int J Smok Cess 1:21–26
Hughes JR, Higgins S, Bickel W (1994) Nicotine withdrawal versus other drug withdrawal syndromes: similarities and dissimilarities. Addiction 89:1461–1470. doi:10.1111/j.1360-0443.1994.tb03744.x
Japuntich S, Smith S, Jorenby D, Piper M, Fiore M, Baker T (2007) Depression predicts smoking early but not late in a quit attempt. Nicotine Tob Res 9:677–686. doi:10.1080/14622200701365301
Johnson PM, Hollander JA, Kenny PJ (2008) Decreased brain reward function during nicotine withdrawal in C57BL6 mice: evidence from intracranial self-stimulation (ICSS) studies. Pharmacol Biochem Behav 90:409–415. doi:10.1016/j.pbb.2008.03.024
Kenny PJ, Markou A (2001) Neurobiology of the nicotine withdrawal syndrome. Pharmacol Biochem Behav 70:531–549
Kenny PJ, Markou A (2005) Conditioned nicotine withdrawal profoundly decreases the activity of brain reward systems. J Neurosci 25:6208–6212. doi:10.1523/JNEUROSCI. 4785-04.2005
Kirshenbaum AP, Bickel WK, Olsen DM (2009) A quantitative analysis of the ubiquitous substance-abuse relapse curve. J Subst Abuse Treat 36:8–17. doi:10.1016/j.jsat.2008.04.001
Koob GF (1996) Drug addiction: the yin and yang of hedonic homeostasis. Neuron 16:893–896. doi:10.1016/S0896-6273(00)80109-9
Koob GF, Le Moal M (2005) Plasticity of reward neurocircuitry and the ‘dark side’ of drug addiction. Nat Neurosci 8:1442–1444. doi:10.1038/nn1105-1442
Kosten T, Markou A, Koob G (1998) Depression and stimulant dependence: neurobiology and pharmacotherapy. J Nerv Ment Dis 186:737–745
LeSage MG, Burroughs D, Pentel PR (2006) Effects of nicotine withdrawal on performance under a progressive-ratio schedule of sucrose pellet delivery in rats. Pharmacol Biochem Behav 83:585–591. doi:10.1016/j.pbb.2006.03.021
Leventhal A, Francione Witt C, Zimmerman M (2008) Associations between depression subtypes and substance use disorders. Psychiatry Res 161:43–50. doi:10.1016/j.psychres.2007.10.014
Leventhal A, Ameringer K, Osborn E, Zvolensky M, Langdon J (2013) Anxiety and depressive symptoms and affective patterns of tobacco withdrawal. Drug Alcohol Depend 133:324–329. doi:10.1016/j.drugalcdep.2013.06.015
Levin ED, Morgan MM, Galvez C, Ellison GD (1987) Chronic nicotine and withdrawal effects on body weight and food and water consumption in female rats. Psyhiol Behav 39:441–444. doi:10.1016/0031-9384(87)90370-2
Liu X, Palmatier M, Caggiula A, Donny E, Sved A (2007) Reinforcement enhancing effect of nicotine and its attenuation by nicotine antagonists in rats. Psychopharmacology (Berl) 194:463–473. doi:10.1007/s00213-007-0863-3
Lopez M, Balleine B, Dickinson A (1992) Incentive learning following reinforcer devaluation is not conditional upon the motivational state during re-exposure. Q J Exp Psychol B 45:265–284. doi:10.1080/14640749208401006
Malin DH, Lake JR, Newlin-Maultsby P, Roberts LK, Lanier JG, Carter VA, Cunningham JS, Wilson OB (1992) Rodent model of nicotine abstinence syndrome. Pharmacol Biochem Behav 43:779–784. doi:10.1016/0091-3057(92)90408-8
Marcinkiewcz C, Prado M, Isaac S, Marshall A, Rylkova D, Bruijnzeel AW (2009) Corticotropin-releasing factor within the central nucleus of the amygdala and the nucleus accumbens shell mediates the negative affective state of nicotine withdrawal in rats. Neuropsychopharmacology 34:1743–1752. doi:10.1038/npp.2008.231
McClernon F, Hiott F, Westman E, Rose J, Levin E (2006) Transdermal nicotine attenuates depression symptoms in nonsmokers: a double-blind, placebo-controlled trial. Psychopharmacology (Berl) 189:125–133. doi:10.1007/s00213-006-0516-y
Mokdad AH, Marks JS, Stroup DF, Gerberding JL (2004) Actual causes of death in the United States. JAMA 291:1238–1245
Olausson P, Jentsch JD, Taylor JR (2004) Repeated nicotine exposure enhances responding with conditioned reinforcement. Psychopharmacology (Berl) 173:98–104. doi:10.1007/s00213-003-1702-9
Palmatier MI, Coddington SB, Liu X, Donny EC, Caggiula AR, Sved AF (2008) The motivation to obtain nicotine-conditioned reinforcers depends on nicotine dose. Neuropharmacology 55:1425–1430. doi:10.1016/j.neuropharm.2008.09.002
Palmatier MI, Marks KR, Jones SA, Freeman KS, Wissman KM, Sheppard AB (2013) The effect of nicotine on sign-tracking and goal-tracking in a Pavlovian conditioned approach paradigm in rats. Psychopharmacology (Berl) 226:247–259
Pergadia ML, Der-Avakian A, D’Sousa MS, Madden PA, Heath AC, Shiffman S, Markou A, Pizzagalli DA (2014) Association between nicotine withdrawal and reward responsiveness in humans and rats. J Am Med Assoc Psych. doi:10.1001/jamapsychiatry.2014.1016
Perkins KA (1999) Baseline-dependency of nicotine: A review. Behav Pharmaoclogy 10:597–615
Perkins KA, Karelitz JL (2013) Reinforcement enhancing effects of nicotine via smoking. Psychopharmacology (Berl) 228:479–486. doi:10.1007/s00213-013-3054-4
Piasecki TM, Fiore MC, Baker TB (1998) Profiles in discouragement: two studies of variability in the time course of smoking withdrawal symptoms. J Abnorm Psychol 107:238–251. doi:10.1037/0021-843X.107.2.238
Piper ME, Schlam TR, Cook JW, Sheffer MA, Smith SS, Loh WY, Bolt DM, Kim SY, Kaye JT, Hefner KR, Baker TB (2011) Tobacco withdrawal components and their relations with cessation success. Psychopharmacology (Berl) 216:569–578. doi:10.1007/s00213-011-2250-3
Richardson NR, Roberts DC (1996) Progressive ratio schedules in drug self-administration studies in rats: a method to evaluate reinforcing efficacy. J Neurosci Methods 66:1–11. doi:10.1016/0165-0270(95)00153-0
Rowlett JK, Massey BW, Kleven MS, Woolverton WL (1996) Parametric analysis of cocaine self-administration under a progressive-ratio schedule in rhesus monkeys. Psychopharmacology (Berl) 125:361–370
Small E, Shah HP, Davenport JJ, Geier JE, Yavarovich KR, Yamada H, Sabarinath SN, Derendorf H, Pauly JR, Gold MS, Bruijnzeel AW (2009) Tobacco smoke exposure induces nicotine dependence in rats. Psychopharmacology (Berl) 208:143–158. doi:10.1007/s00213-009-1716-z
Solomon R, Corbit J (1973) An opponent-process theory of motivation II. Cigarette addiction. J Abnorm Psychol 81:158–171
Stafford D, LeSage MG, Glowa JR (1998) Progressive-ratio schedules of drug delivery in the analysis of drug self-administration: a review. Psychopharmacology 139(3):169–184
Stolerman IP, Jarvis MJ (1995) The scientific case that nicotine is addictive. Psychopharmacology (Berl) 117:2–10. doi:10.1007/BF02245088
Vlachou S, Markou A (2011) Intracranial self-stimulation. In: Olmstead M (ed) Animal models of drug addiction. pp 3–56
Watkins S, Koob GF, Markou A (2000) Neural mechanisms underlying nicotine addiction: acute positive reinforcement and withdrawal. Nicotine Tob Res 2:19–37. doi:10.1080/14622200050011277
Weatherly JN, King BM, Uran EL (2003) Upcoming food-pellet reinforcement alters rats’ lever pressing for liquid sucrose delivered by a progressive-ratio schedule. Behav Process 63(2):73–86. doi:10.1016/S0376-6357(03)00033-0
Weaver M, Sweitzer M, Coddington S, Sheppard J, Verdecchia N, Caggiula AR, Sved AF, Donny EC (2012) Precipitated withdrawal from nicotine reduces reinforcing effects of a visual stimulus for rats. Nicotine Tob Res 14:824–832. doi:10.1093/ntr/ntr293
Wojnicki FE, Babbs RK, Corwin RW (2010) Reinforcing efficacy of fat, as assessed by progressive ratio responding, depends upon availability not amount consumed. Physiol Behav 100(4):316–321. doi:10.1016/j.physbeh.2010.03.004
Xue Y, Domino E (2008) Tobacco/nicotine and endogenous brain opioids. Prog Neuropsychopharmacol Biol Psychiatry 32:1131–1138. doi:10.1016/j.pnpbp.2007.12.012
Acknowledgments
Research reported in this publication was supported by an Institutional Development Award (IDeA) from the National Institute of General Medical Sciences of the National Institutes of Health under grant number 8P20GM103449. Its contents are solely the responsibility of the authors and do not necessarily represent the official views of NIGMS or NIH. The authors would like to express their gratitude to many research assistants that contributed to data acquisition: Samantha Giglio, Mallory Hyland, Michael Lavelle, Jesse Suhaka, Susan Longchamp, and Ryan Collins. Furthermore, the helpful guidance of Jim Nichols (DVM) and Angela Irvine of the Saint Michael’s College IACUC was much appreciated, and we owe our gratitude to Dr. Matthew Palmatier for sharing a software program used to conduct the experiments. We would also like to thank Dr. John Hughes of the University of Vermont for his insightful comments on the data presentation and interpretation and to the anonymous reviewers for their explicit recommendations.
Conflict of interest
The authors acknowledge no financial conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kirshenbaum, A., Green, J., Fay, M. et al. Reinforcer devaluation as a consequence of acute nicotine exposure and withdrawal. Psychopharmacology 232, 1583–1594 (2015). https://doi.org/10.1007/s00213-014-3792-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-014-3792-y