Abstract
Background
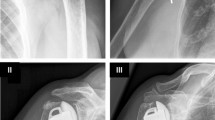
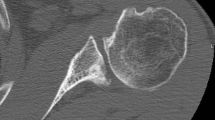
Cementless surface replacement of the shoulder represents an alternative to conventional stemmed anatomic prostheses. Glenoid erosion is a well-known complication in hemiarthroplasty. However, there is limited data concerning radiographic evaluation and prognostic factors for this phenomenon.
Objectives
The aim of our study was to determine the development of glenoid erosion following shoulder resurfacing using a new measurement technique and detect potential prognostic factors.
Materials and methods
We performed a retrospective analysis on 38 shoulders undergoing humeral head resurfacing with a mean follow-up of 65.4 ± 43 months. Clinical and radiographic evaluation followed a standardized protocol including pre- and postoperative Constant score, active range of motion, and X‑rays in true anteroposterior view. Three independent observers performed measurements of glenoid erosion.
Results
We found good interobserver reliability for glenoid erosion measurements (intraclass correlation coefficient [ICC] 0.74–0.78). Progressive glenoid erosion was present in all cases, averaging 5.5 ± 3.9 mm at more than 5 years’ follow-up. Male patients demonstrated increased glenoid bone loss within the first 5 years (p < 0.04). The mean Constant score improved to 55.4 ± 23.6 points at the latest follow-up. Younger age was correlated to increased functional outcome. Revision rate due to painful glenoid erosion was 37%.
Conclusions
Glenoid erosion can be routinely expected in patients undergoing humeral head resurfacing. Painful glenoid erosion leads to deterioration in functional outcome and necessitates revision surgery in a high percentage of cases.
Zusammenfassung
Hintergrund
Der zementfreie Oberflächenersatz der Schulter stellt eine Alternative zur konventionellen anatomischen Schaftprothese dar. Eine bekannte Komplikation der Hemiendoprothetik ist die Glenoiderosion, ein Substanzverlust der Schultergelenkpfanne.
Ziel der Arbeit
Ziel unserer Arbeit war die Validierung einer radiologischen Messmethode zur Quantifizierung der Glenoiderosion nach Implantation eines Oberflächenersatz der Schulter. Zudem sollten der zeitliche Verlauf und prognostische Faktoren des progredienten Pfannensubstanzverlusts aufgedeckt werden.
Material und Methoden
Es wurde eine retrospektive klinische und radiologische Analyse von 38 Oberflächenersatzprothesen im Mittel 65,4 ± 43 Monate postoperativ durchgeführt. Anhand eines standardisierten Protokolls wurden der Constant-Score, das aktive Bewegungsausmaß sowie Röntgenparameter bestimmt. Die radiologische Messung der Glenoiderosion erfolgte durch 3 unabhängige Untersucher.
Ergebnisse
Eine fortschreitende Glenoiderosion konnte in allen Fällen nachgewiesen werden und betrug 5 Jahre postoperativ im Mittel 5,5 ± 3,9 mm. Insbesondere männliche Patienten zeigten einen erhöhten Glenoidsubstanzverlust innerhalb der ersten 5 Jahre (p < 0,04). Die Messmethode zur Bestimmung der Glenoiderosion wies eine gute Interobserver-Reliabilität auf (ICC 0,74–0,78). Im Gesamtkollektiv verbesserte sich der Constant-Score von 20,2 ± 13 Punkten auf 55,4 ± 23,6 Punkte, wobei ein niedrigeres Alter mit besseren funktionellen Ergebnissen korrelierte (p = 0,03). Die Revisionsrate aufgrund schmerzhafter Glenoiderosion betrug 37 %.
Diskussion
Nach Implantation einer Schulterkappenprothese kann regelmäßig das Auftreten einer Glenoiderosion beobachtet werden. Eine schmerzhafte Glenoiderosion mit resultierendem Funktionsverlust führt zu hohen Revisionsraten.


Similar content being viewed by others
Abbreviations
- A:
-
Glenoid depth
- CI:
-
Confidence interval
- ICC:
-
Intraclass correlation coefficient
- PACS:
-
Picture archiving and communication system
- R:
-
Distance spinoglenoidal notch to joint line
- R′:
-
Distance humeral center of rotation to joint line
- R*:
-
Distance joint line to lateral edge of acromion
- SD:
-
Standard deviation
References
Al-Hadithy N, Domos P, Sewell MD, Naleem A, Papanna MC, Pandit R (2012) Cementless surface replacement arthroplasty of the shoulder for osteoarthritis: results of fifty Mark III Copeland prosthesis from an independent center with four-year mean follow-up. J Shoulder Elbow Surg 21(12):1776–1781. https://doi.org/10.1016/j.jse.2012.01.024
Bailie DS, Llinas PJ, Ellenbecker TS (2008) Cementless humeral resurfacing arthroplasty in active patients less than fifty-five years of age. J Bone Joint Surg Am 90(1):110–117. https://doi.org/10.2106/JBJS.F.01552
Ball CM, Galatz LM, Yamaguchi K (2001) Meniscal allograft interposition arthroplasty for the arthritic shoulder: description of a new technique. Tech Shoulder Elb Surg 2:247:254
Boileau P, Walch G (1997) The three-dimensional geometry of the proximal humerus. J Bone Joint Surg Br 79:857–865
Carroll RM, Izquierdo R, Vazquez M, Blaine TA, Levine WN, Bigliani LU (2004) Conversion of painful hemiarthroplasty to total shoulder arthroplasty: long-term results. J Shoulder Elbow Surg 13:599–603. https://doi.org/10.1016/j.jse.2004.03.016
Constant CR, Murley AH (1987) A clinical method of functional assessment of the shoulder. Clin Orthop 214:160–164
Copeland S (2006) The continuing development of shoulder replacement: “reaching the surface”. J Bone Joint Surg Am 88:900–905
Elhassan B, Ozbaydar M, Diller D, Higgins LD, Warner JJ (2009) Soft-tissue resurfacing of the glenoid in the treatment of glenohumeral arthritis in active patients less than fifty years old. J Bone Joint Surg Am 91(268):419–424. https://doi.org/10.2106/JBJS.H.00318
Franta AK, Lenters TR, Mounce D, Neradilek B, Matsen FA 3rd (2007) The complex characteristics of 282 unsatisfactory shoulder arthroplasties. J Shoulder Elbow Surg 16:555–562. https://doi.org/10.1016/j.jse.2006.11.004
Gartsman GM, Roddey TS, Hammerman SM (2000) Shoulder arthroplasty with or without resurfacing of the glenoid in patients who have osteoarthritis. J Bone Joint Surg Am 82:26–34
Geervliet PC, van den Bekerom MPJ, Spruyt P, Curvers M, van Noort A, Visser CPJ (2017) Outcome and revision rate of uncemented resurfacing (C.A.P.) after 5–8 years. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-017-2688-9
Hasan SS, Leith JM, Campbell B, Kapil R, Smith KL, Matsen FA 3rd (2002) Characteristics of unsatisfactory shoulder arthroplasties. J Shoulder Elbow Surg 11:431–441. https://doi.org/10.1067/mse.2002.125806
Krishnan SG, Nowinski R, Harrison D, Burkhead WZ (2007) Humeral hemiarthroplasty with biologic resurfacing of the glenoid for glenohumeral arthritis; two to fifteen-year outcomes. J Bone Joint Surg Am 89:727–734. https://doi.org/10.2106/JBJS.E.01291
Lee KT, Bell S, Salmon J (2009) Cementless surface replacement arthroplasty of the shoulder with biologic resurfacing of the glenoid. J Shoulder Elbow Surg 18(6):915–919. https://doi.org/10.1016/j.jse.2009.01.014
Levine WM, Djurasovic M, Glasson JM, Pollock RG, Flatow EL, Bigliani LU (1997) Hemiarthroplasty for glenohumeral arthritis: results correlated to degree of glenoid wear. J Shoulder Elbow Surg 6:449–454
Levy O, Copeland SA (2001) Cementless surface replacement arthroplasty of the shoulder. 5‑ to 10-year results with the Copeland mark-2 prosthesis. J Bone Joint Surg Br 83:213–221
Levy O, Copeland SA (2004) Cementless surface replacement arthroplasty (Copeland CSRA) for osteoarthritis of the shoulder. J Shoulder Elbow Surg 13:266–271. https://doi.org/10.1016/j.jse.2004.01.005
Nicholson GP, Goldstein JL, Romeo AA, Cole BJ, Hayden JK, Twigg SL, McCarty LP, Detterline AJ (2007) Lateral meniscus allograft biologic glenoid arthroplasty in total shoulder arthroplasty for young shoulders with degenerative joint disease. J Shoulder Elbow Surg 16(5):261–266. https://doi.org/10.1016/j.jse.2007.03.003
Parsons IM, Millett PJ, Warren JJ (2004) Glenoid wear after shoulder hemiarthroplasty: quantitative radiographic analysis. Clin Orthop Relat Res 421:120–125. https://doi.org/10.1097/01.blo.0000119249.61696.f1
Pritchett JW (2011) Long-term results and patient satisfaction after shoulder resurfacing. J Shoulder Elbow Surg. https://doi.org/10.1016/j.jse.2010.08.014
Raiss P, Kasten P, Baumann F, Moser M, Rickert M, Loew M (2009) Treatment of osteonecrosis of the humeral head with cementless surface replacement arthroplasty. J Bone Joint Surg Am 91(2):340–349. https://doi.org/10.2106/JBJS.H.00560
Raiss P, Weiter M, Sowa B, Zeifang F, Loew M (2015) Results of cementless humreal head resurfacing with cemented glenoid components. Int Orthop 39:277–284. https://doi.org/10.1007/s00264-014-2540-6
Rispoli DM, Sperling JW, Athwal GS, Schleck CD, Cofield RH (2006) Humeral head replacement for the treatment of osteoarthritis. J Bone Joint Surg Am 88(12):2637–2644. https://doi.org/10.2106/JBJS.E.01383
Soudy K, Szymanski C, Lalanne C, Bourgault C, Thiounn A, Cotten A, Maynou C (2017) Results and limitations of humeral head resurfacing: 105 cases at a mean follow-up of 5 years. Orthop Traumatol Surg Res 103:415–420. https://doi.org/10.1016/j.otsr.2016.12.015
Sperling JW, Cofield RH, Rowland CM (2004) Minimum fifteen-year follow-up of Neer hemiarthroplasty and total shoulder arthroplasty in patients age fifty years or younger. J Shoulder Elbow Surg 13(6):604–613. https://doi.org/10.1016/j.jse.2004.03.013
Sperling JW, Cofield RH, Rowland CM (1998) Neer hemiarthroplasty and Neer total shoulder arthroplasty in patients fifty years old or less. Long-term results. J Bone Joint Surg Am 80:464–473
Thomas SR, Wilson AJ, Chambler A, Harding I, Thomas M (2005) Outcome of Copeland surface replacement shoulder arthroplasty. J Shoulder Elbow Surg 14:485–491. https://doi.org/10.1016/j.jse.2005.02.011
Wirth MA, Tapscott RS, Southworth C, Rockwood CA Jr. (2006) Treatment of glenohumeral arthritis with a hemiarthroplasty: a minimum five-year follow-up outcome study. J Bone Joint Surg Am 88:964–973. https://doi.org/10.2106/JBJS.D.03030
Wirth MA (2009) Humeral head arthroplasty and meniscal allograft resurfacing of the glenoid. J Bone Joint Surg Am 91:1109–1119. https://doi.org/10.2106/JBJS.H.00677
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
B.S. Werner and F. Gohlke declare to be under consultancy contracts with Wright/Tornier. J. Stehle, A. Abdelkawi, P. Plumhoff, and R. Hudek declare that they have no competing interests.
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975 (in its current revised form). Informed consent was obtained from all patients included in the study.
Rights and permissions
About this article
Cite this article
Werner, B.S., Stehle, J., Abdelkawi, A. et al. Progressive glenoid bone loss caused by erosion in humeral head resurfacing. Orthopäde 46, 1028–1033 (2017). https://doi.org/10.1007/s00132-017-3483-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00132-017-3483-6