Abstract
Aims/hypothesis
Glomerular lipid accumulation is a defining feature of diabetic kidney disease (DKD); however, the precise underlying mechanism requires further elucidation. Recent evidence suggests a role for proprotein convertase subtilisin/kexin type 9 (PCSK9) in intracellular lipid homeostasis. Although PCSK9 is present in kidneys, its role within kidney cells and relevance to renal diseases remain largely unexplored. Therefore, we investigated the role of intracellular PCSK9 in regulating lipid accumulation and homeostasis in the glomeruli and podocytes under diabetic conditions. Furthermore, we aimed to identify the pathophysiological mechanisms responsible for the podocyte injury that is associated with intracellular PCSK9-induced lipid accumulation in DKD.
Methods
In this study, glomeruli were isolated from human kidney biopsy tissues, and glomerular gene-expression analysis was performed. Also, db/db and db/m mice were used to perform glomerular gene-expression profiling. We generated DKD models using a high-fat diet and low-dose intraperitoneal streptozocin injection in C57BL/6 and Pcsk9 knockout (KO) mice. We analysed cholesterol and triacylglycerol levels within the kidney cortex. Lipid droplets were evaluated using BODIPY staining. We induced upregulation and downregulation of PCSK9 expression in conditionally immortalised mouse podocytes using lentivirus and siRNA transfection techniques, respectively, under diabetic conditions.
Results
A significant reduction in transcription level of PCSK9 was observed in glomeruli of individuals with DKD. PCSK9 expression was also reduced in podocytes of animals under diabetic conditions. We observed significantly higher lipid accumulation in kidney tissues of Pcsk9 KO DKD mice compared with wild-type (WT) DKD mice. Additionally, Pcsk9 KO mouse models of DKD exhibited a significant reduction in mitochondria number vs WT models, coupled with a significant increase in mitochondrial size. Moreover, albuminuria and podocyte foot process effacement were observed in WT and Pcsk9 KO DKD mice, with KO DKD mice displaying more pronounced manifestations. Immortalised mouse podocytes exposed to diabetic stimuli exhibited heightened intracellular lipid accumulation, mitochondrial injury and apoptosis, which were ameliorated by Pcsk9 overexpression and aggravated by Pcsk9 knockdown in mouse podocytes.
Conclusions/interpretation
The downregulation of PCSK9 in podocytes is associated with lipid accumulation, which leads to mitochondrial dysfunction, cell apoptosis and renal injury. This study sheds new light on the potential involvement of PCSK9 in the pathophysiology of glomerular lipid accumulation and podocyte injury in DKD.
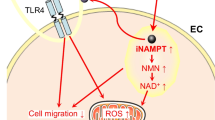
Graphical Abstract








Similar content being viewed by others
Abbreviations
- ABCA1:
-
ATP-binding cassette transporter A1
- BAX:
-
B cell lymphoma-2-associated X
- Bcl-2:
-
B cell lymphoma-2
- CMV:
-
Cytomegalovirus
- DKD:
-
Diabetic kidney disease
- GBM:
-
Glomerular basement membrane
- HBSS:
-
Hanks’ Balanced Salt Solution
- HFD:
-
High-fat diet
- IgAN:
-
IgA nephropathy
- IRB:
-
Institutional Review Board
- KO:
-
Knockout
- LDL-C:
-
LDL-cholesterol
- LDLR:
-
LDL-cholesterol receptor
- Lv-PCSK9:
-
CMV-mPCSK9 lentivirus
- PCSK9:
-
Proprotein convertase subtilisin/kexin type 9
- PGC-1α:
-
Peroxisome proliferator-activated receptor, gamma, coactivator 1, alpha
- qRT-PCR:
-
Quantitative real-time PCR
- siPcsk9 :
-
Pcsk9 siRNA
- STZ:
-
Streptozocin
- TEM:
-
Transmission electron microscopy
- TU:
-
Transfection units
- WT:
-
Wild-type
- ZO-1:
-
Zonula occludens-1
References
Umanath K, Lewis JB (2018) Update on diabetic nephropathy: core curriculum 2018. Am J Kidney Dis 71:884–895. https://doi.org/10.1053/j.ajkd.2017.10.026
Kwon S, Hyeon JS, Jung Y et al (2023) Urine myo-inositol as a novel prognostic biomarker for diabetic kidney disease: a targeted metabolomics study using nuclear magnetic resonance. Kidney Res Clin Pract 42:445–459. https://doi.org/10.23876/j.krcp.22.152
Kim DW, Song SH (2023) A new journey to predict the prognosis of diabetic kidney disease. Kidney Res Clin Pract 42:409–411. https://doi.org/10.23876/j.krcp.23.093
Kimmelstiel P, Wilson C (1936) Intercapillary lesions in the glomeruli of the kidney. Am J Pathol 12:83-98.7
Proctor G, Jiang T, Iwahashi M, Wang Z, Li J, Levi M (2006) Regulation of renal fatty acid and cholesterol metabolism, inflammation, and fibrosis in Akita and OVE26 mice with type 1 diabetes. Diabetes 55:2502–2509. https://doi.org/10.2337/db05-0603
Wang Z, Jiang T, Li J et al (2005) Regulation of renal lipid metabolism, lipid accumulation, and glomerulosclerosis in FVB db/db mice with type 2 diabetes. Diabetes 54:2328–2335. https://doi.org/10.2337/diabetes.54.8.2328
Merscher-Gomez S, Guzman J, Pedigo CE et al (2013) Cyclodextrin protects podocytes in diabetic kidney disease. Diabetes 62:3817–3827. https://doi.org/10.2337/db13-0399
Attie AD (2007) ABCA1: at the nexus of cholesterol, HDL and atherosclerosis. Trends Biochem Sci 32:172–179. https://doi.org/10.1016/j.tibs.2007.02.001
Yoo TH, Pedigo CE, Guzman J et al (2015) Sphingomyelinase-like phosphodiesterase 3b expression levels determine podocyte injury phenotypes in glomerular disease. J Am Soc Nephrol 26:133–147. https://doi.org/10.1681/ASN.2013111213
Ducasa GM, Mitrofanova A, Mallela SK et al (2019) ATP-binding cassette A1 deficiency causes cardiolipin-driven mitochondrial dysfunction in podocytes. J Clin Invest 129:3387–3400. https://doi.org/10.1172/JCI125316
Seidah NG, Benjannet S, Wickham L et al (2003) The secretory proprotein convertase neural apoptosis-regulated convertase 1 (NARC-1): liver regeneration and neuronal differentiation. Proc Natl Acad Sci U S A 100:928–933. https://doi.org/10.1073/pnas.0335507100
Abifadel M, Rabes JP, Devillers M et al (2009) Mutations and polymorphisms in the proprotein convertase subtilisin kexin 9 (PCSK9) gene in cholesterol metabolism and disease. Hum Mutat 30:520–529. https://doi.org/10.1002/humu.20882
Park S, Kim SG, Lee S et al (2023) Genetic variations in HMGCR and PCSK9 and kidney function: a Mendelian randomization study. Kidney Res Clin Pract 42:460–472. https://doi.org/10.23876/j.krcp.22.237
Tong LL, Adler SG (2022) Diabetic kidney disease treatment: new perspectives. Kidney Res Clin Pract 41:S63–S73. https://doi.org/10.23876/j.krcp.21.288
Levy E, Ben DjoudiOuadda A, Spahis S et al (2013) PCSK9 plays a significant role in cholesterol homeostasis and lipid transport in intestinal epithelial cells. Atherosclerosis 227:297–306. https://doi.org/10.1016/j.atherosclerosis.2013.01.023
Rashid S, Tavori H, Brown PE et al (2014) Proprotein convertase subtilisin kexin type 9 promotes intestinal overproduction of triglyceride-rich apolipoprotein B lipoproteins through both low-density lipoprotein receptor-dependent and -independent mechanisms. Circulation 130:431–441. https://doi.org/10.1161/CIRCULATIONAHA.113.006720
Lebeau PF, Byun JH, Platko K et al (2019) Pcsk9 knockout exacerbates diet-induced non-alcoholic steatohepatitis, fibrosis and liver injury in mice. JHEP Rep 1:418–429. https://doi.org/10.1016/j.jhepr.2019.10.009
Roubtsova A, Munkonda MN, Awan Z et al (2011) Circulating proprotein convertase subtilisin/kexin 9 (PCSK9) regulates VLDLR protein and triglyceride accumulation in visceral adipose tissue. Arterioscler Thromb Vasc Biol 31:785–791. https://doi.org/10.1161/ATVBAHA.110.220988
Demers A, Samami S, Lauzier B et al (2015) PCSK9 induces CD36 degradation and affects long-chain fatty acid uptake and triglyceride metabolism in adipocytes and in mouse liver. Arterioscler Thromb Vasc Biol 35:2517–2525. https://doi.org/10.1161/ATVBAHA.115.306032
Cohen CD, Frach K, Schlondorff D, Kretzler M (2002) Quantitative gene expression analysis in renal biopsies: a novel protocol for a high-throughput multicenter application. Kidney Int 61:133–140. https://doi.org/10.1046/j.1523-1755.2002.00113.x
Jung DS, Lee SH, Kwak SJ et al (2012) Apoptosis occurs differentially according to glomerular size in diabetic kidney disease. Nephrol Dial Transplant 27(1):259–266. https://doi.org/10.1093/ndt/gfr301
Srinivasan K, Viswanad B, Asrat L, Kaul CL, Ramarao P (2005) Combination of high-fat diet-fed and low-dose streptozotocin-treated rat: a model for type 2 diabetes and pharmacological screening. Pharmacol Res 52:313–320. https://doi.org/10.1016/j.phrs.2005.05.004
Reed MJ, Meszaros K, Entes LJ et al (2000) A new rat model of type 2 diabetes: the fat-fed, streptozotocin-treated rat. Metabolism 49:1390–1394. https://doi.org/10.1053/meta.2000.17721
Takemoto M, Asker N, Gerhardt H et al (2002) A new method for large scale isolation of kidney glomeruli from mice. Am J Pathol 161:799–805. https://doi.org/10.1016/S0002-9440(10)64239-3
Mundel P, Reiser J, Zuniga Mejia Borja A et al (1997) Rearrangements of the cytoskeleton and cell contacts induce process formation during differentiation of conditionally immortalized mouse podocyte cell lines. Exp Cell Res 236:248–258. https://doi.org/10.1006/excr.1997.3739
Lois C, Refaeli Y, Qin XF, Van Parijs L (2001) Retroviruses as tools to study the immune system. Curr Opin Immunol 13:496–504. https://doi.org/10.1016/S0952-7915(00)00247-8
Nam BY, Kim DK, Park JT et al (2015) Double transduction of a Cre/LoxP lentiviral vector: a simple method to generate kidney cell-specific knockdown mice. Am J Physiol Renal Physiol 309:F1060–F1069. https://doi.org/10.1152/ajprenal.00251.2015
Lee SH, Moon SJ, Paeng J et al (2015) Podocyte hypertrophy precedes apoptosis under experimental diabetic conditions. Apoptosis 20(8):1056–1071. https://doi.org/10.1007/s10495-015-1134-0
Gundersen HJ, Seefeldt T, Osterby R (1980) Glomerular epithelial foot processes in normal man and rats. Distribution of true width and its intra- and inter-individual variation. Cell Tissue Res 205:147–155. https://doi.org/10.1007/BF00234450
Choi SY, Suh KS, Choi DE, Lim BJ (2010) Morphometric analysis of podocyte foot process effacement in IgA nephropathy and its association with proteinuria. Ultrastruct Pathol 34:195–198. https://doi.org/10.3109/01913121003648402
Picard M, White K, Turnbull DM (2013) Mitochondrial morphology, topology, and membrane interactions in skeletal muscle: a quantitative three-dimensional electron microscopy study. J Appl Physiol (1985) 114:161–171. https://doi.org/10.1152/japplphysiol.01096.2012
Medina-Gomez G, Gray S, Vidal-Puig A (2007) Adipogenesis and lipotoxicity: role of peroxisome proliferator-activated receptor gamma (PPARgamma) and PPARgammacoactivator-1 (PGC1). Public Health Nutr 10:1132–1137. https://doi.org/10.1017/S1368980007000614
Martinez-Garcia C, Izquierdo A, Velagapudi V et al (2012) Accelerated renal disease is associated with the development of metabolic syndrome in a glucolipotoxic mouse model. Dis Model Mech 5:636–648. https://doi.org/10.1242/dmm.009266
Nakamura T, Ushiyama C, Osada S, Hara M, Shimada N, Koide H (2001) Pioglitazone reduces urinary podocyte excretion in type 2 diabetes patients with microalbuminuria. Metabolism 50:1193–1196. https://doi.org/10.1053/meta.2001.26703
Zhang G, Li Q (2019) Inflammation induces lipid deposition in kidneys by downregulating renal PCSK9 in mice with adriamycin-induced nephropathy. Med Sci Monit 25:5327–5335. https://doi.org/10.12659/MSM.917312
Byun JH, Lebeau PF, Platko K et al (2022) Inhibitory antibodies against PCSK9 reduce surface CD36 and mitigate diet-induced renal lipotoxicity. Kidney360 3:1394–1410. https://doi.org/10.34067/KID.0007022021
Wilson PC, Yoshiharu Muto, Nicolas Ledru et al (2021) Single cell transcriptional and chromatin accessibility profiling redefine cellular heterogeneity in the adult human kidney. Nat Commun 12(1):2190. https://doi.org/10.1038/s41467-021-22368-w
Wilson PC, Wu HJ, Kirita YH et al (2019) The single-cell transcriptomic landscape of early human diabetic nephropathy. Proc Natl Acad Sci USA 116(39):19619–19625. https://doi.org/10.1073/pnas.1908706116
Kidney Interactive Transcriptomics (2024) Kidney Interactive Transcriptomics: an online analyzer for kidney single cell datasets. Available from: http://humphreyslab.com/SingleCell/. Accessed: 20 November 2022
Da Dalt L, Ruscica M, Bonacina F et al (2019) PCSK9 deficiency reduces insulin secretion and promotes glucose intolerance: the role of the low-density lipoprotein receptor. Eur Heart J 40:357–368. https://doi.org/10.1093/eurheartj/ehy357
Mbikay M, Sirois F, Mayne J et al (2010) PCSK9-deficient mice exhibit impaired glucose tolerance and pancreatic islet abnormalities. FEBS Lett 584:701–706. https://doi.org/10.1016/j.febslet.2009.12.018
Virtue S, Vidal-Puig A (2010) Adipose tissue expandability, lipotoxicity and the metabolic syndrome — an allostatic perspective. Biochim Biophys Acta 1801:338–349. https://doi.org/10.1016/j.bbalip.2009.12.006
Han SH, Wu MY, Nam BY et al (2017) PGC-1alpha protects from notch-induced kidney fibrosis development. J Am Soc Nephrol 28:3312–3322. https://doi.org/10.1681/ASN.2017020130
Baek J, Lee YH, Jeong HY, Lee SY (2023) Mitochondrial quality control and its emerging role in the pathogenesis of diabetic kidney disease. Kidney Res Clin Pract 42:546–560. https://doi.org/10.23876/j.krcp.22.233
Ruospo M, Saglimbene VM, Palmer SC et al (2017) Glucose targets for preventing diabetic kidney disease and its progression. Cochrane Database Syst Rev (6):CD010137. https://doi.org/10.1002/14651858.CD010137.pub2
Simon P, Ramee MP, Boulahrouz R et al (2004) Epidemiologic data of primary glomerular diseases in western France. Kidney Int 66:905–908. https://doi.org/10.1111/j.1523-1755.2004.00834.x
Baass A, Dubuc G, Tremblay M et al (2009) Plasma PCSK9 is associated with age, sex, and multiple metabolic markers in a population-based sample of children and adolescents. Clin Chem 55:1637–1645. https://doi.org/10.1373/clinchem.2009.126987
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Acknowledgements
We especially thank S. W. Park (Department of Biochemistry and Molecular Biology, Yonsei University College of Medicine, Seoul, South Korea) for providing experimental mice. Some of the results presented in the current article were included in the PhD thesis by Jimin Park. The graphical abstract was created using scidraw.io.
Data availability
The data supporting the findings of the present study are available from the corresponding author upon reasonable request.
Funding
This work was supported by grants from the Korea Healthcare Technology R&D Project, Ministry of Health and Welfare, Republic of Korea (H14C2003000016), the National Research Foundation of Korea (NRF-2019R1A6A3A13094020), the National Natural Science Foundation of China (82000689), the Postdoctoral Science Foundation of China (2021M691212) and the Natural Science Foundation of Jilin Province, China (20210101455JC).
Authors’ relationships and activities
The authors declare that there are no relationships or activities that might bias, or be perceived to bias, their work.
Contribution statement
T-HY conceived and supervised the project and designed the experiments. MW and C-YY performed all experiments. JP, GK and BYN performed sample preparation for TEM, image acquisition and data analysis. SK conducted BODIPY 493/503 staining and subsequent image analysis. MW and C-YY interpreted data. T-HY, C-YY and MW wrote the manuscript. JTP, SHH and S-WK reviewed the article critically for important intellectual content. All authors contributed to the analysis and discussion of the data. All authors revised and approved the manuscript in its final form. T-HY is the guarantor of this work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, M., Yoon, CY., Park, J. et al. The role of PCSK9 in glomerular lipid accumulation and renal injury in diabetic kidney disease. Diabetologia (2024). https://doi.org/10.1007/s00125-024-06191-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00125-024-06191-8