Abstract
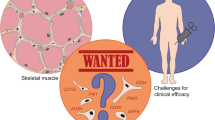
In 1978, Partridge et al. first demonstrated that mouse myoblasts intramuscularly transplanted into recipient mice fuse with recipient myofibers. In 1989, the same research group showed that wild-type myoblasts successfully restored dystrophin expression in host mdx mice. Based on this report, several clinical trials of myoblast transfer for Duchenne muscular dystrophy (DMD) have been performed, but none has been successful in restoration of muscle function. Meanwhile, information about molecular regulation of satellite cells/myoblasts and cellular and molecular regulation of muscle regeneration has accumulated, and new types of stem cells with multipotency have been identified in skeletal muscle. The mesoangioblast is one such stem cell. Notably, mesoangioblasts have been demonstrated to be deliverable to damaged muscle by intra-arterial injection. In addition to skeletal muscle-resident stem cells, in 2007, Yamanaka and his colleagues reported the induction of embryonic stem (ES) cell-like pluripotent stem cells from human fibroblasts via the ectopic expression of SOX2, OCT3/4, KLF4, and c-MYC and named them “induced pluripotent stem cells (iPS cells).” The next year, generation of iPS cells from cells of patients with DMD was reported. To utilize iPS cells for regenerative medicine for muscular dystrophies, several protocols for derivation of skeletal muscle from human ES/iPS cells have been developed. Lastly, efficient genome-editing tools have emerged as a technology to obtain genetically corrected autologous cells. To make full use of these new tools in regenerative medicine, we need to understand how skeletal muscle stem cells are born, how they participate in regeneration of muscle fibers, and how the process is impaired in dystrophin-null muscle.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Mauro A (1961) Satellite cell of skeletal muscle fibers. J Biophys Biochem Cytol 9:493–495
Schultz E, Gibson MC, Champion T (1978) Satellite cells are mitotically quiescent in mature mouse muscle: an EM and radioautographic study. J Exp Zool 206:451–456
Blau HM, Webster C, Pavlath GK (1983) Defective myoblasts identified in Duchenne muscular dystrophy. Proc Natl Acad Sci U S A 80:4856–4860
Blau HM, Webster C, Pavlath GK, Chiu CP (1985) Evidence for defective myoblasts in Duchenne muscular dystrophy. Adv Exp Med Biol 182:85–110
Partridge TA, Grounds M, Sloper JC (1978) Evidence of fusion between host and donor myoblasts in skeletal muscle grafts. Nature 273:306–308
Partridge TA, Morgan JE, Coulton GR, Hoffman EP, Kunkel LM (1989) Conversion of mdx myofibers from dystrophin negative to dystrophin positive by injection of normal myoblasts. Nature 337:176–179
Law PK, Goodwin TG, Fang Q et al (1992) Feasibility, safety, and efficacy of myoblast transfer therapy on Duchenne muscular dystrophy boys. Cell Transplant 1:235–244
Mendell JR, Kissel JT, Amato AA et al (1995) Myoblast transfer in the treatment of Duchenne muscular dystrophy. N Engl J Med 333:832–838
Tremblay JP, Malouin F, Roy R et al (1993) Results of a triple blind clinical study of myoblast transplantations without immunosuppressive treatment in young boys with Duchenne muscular dystrophy. Cell Transplant 2:99–112
Mouly V, Aamiri A, Périé S et al (2005) Myoblast transfer therapy: is there any light at the end of the tunnel? Acta Myol 24:128–133
Ikemoto M, Fukada S, Uezumi A et al (2007) Autologous transplantation of SM/C-2.6(+) satellite cells transduced with micro-dystrophin CS1 cDNA by lentiviral vector into mdx mice. Mol Ther 15:2178–2185
Collins CA, Olsen I, Zammit PS et al (2005) Stem cell function, self-renewal, and behavioral heterogeneity of cells from the adult muscle satellite cell niche. Cell 122:289–301
Gilbert PM, Havenstrite KL, Magnusson KE et al (2010) Substrate elasticity regulates skeletal muscle stem cell self-renewal in culture. Science 329:1078–1081
Skuk D, Goulet M, Roy B et al (2007) First test of a “high-density injection” protocol for myogenic cell transplantation throughout large volumes of muscles in a Duchenne muscular dystrophy patient: eighteen months follow-up. Neuromuscul Disord 17:38–46
Skuk D, Goulet M, Trembley JP (2011) Transplanted myoblasts can migrate several millimeters to fuse with damaged myofibers in nonhuman primate skeletal muscle. J Neuropathol Exp Neurol 70:770–778
Périé S, Trollet C, Mouly V et al (2014) Autologous myoblast transplantation for oculopharyngeal muscular dystrophy: a phase I/IIa clinical study. Mol Ther 22:219–225
De Angelis L, Berghella L, Coletta M et al (1999) Skeletal myogenic progenitors originating from embryonic dorsal aorta coexpress endothelial and myogenic markers and contribute to postnatal muscle growth and regeneration. J Cell Biol 147:869–878
Dellavalle A, Sampaolesi M, Tonlorenzi R et al (2007) Pericytes of human skeletal muscle are myogenic precursors distinct from satellite cells. Nat Cell Biol 9:255–267
Sampaolesi M, Torrente Y, Innocenzi A et al (2003) Cell therapy of alpha-sarcoglycan null dystrophic mice through intra-arterial delivery of mesoangioblasts. Science 301:487–492
Sampaolesi M, Blot S, D'Antona G et al (2006) Mesoangioblast stem cells ameliorate muscle function in dystrophic dogs. Nature 444:574–579
Takahashi K, Yamanaka S (2006) Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell 126:663–676
Takahashi K, Tanabe K, Ohnuki M, Narita M, Ichisaka T et al (2007) Induction of pluripotent stem cells from adult human fibroblasts by defined factors. Cell 131:861–872
Yu J, Vodyanik MA, Smuga-Otto K et al (2007) Induced pluripotent stem cell lines derived from human somatic cells. Science 318:1917–1920
Park IH, Arora N, Huo H et al (2008) Disease-specific induced pluripotent stem cells. Cell 134:877–886
Weintraub H, Tapscott SJ, Davis RL et al (1989) Activation of muscle-specific genes in pigment, nerve, fat, liver, and fibroblast cell lines by forced expression of MyoD. Proc Natl Acad Sci U S A 86:5434–5438
Rao L, Tang W, Wei Y et al (2012) Highly efficient derivation of skeletal myotubes from human embryonic stem cells. Stem Cell Rev 8:1109–1119
Tanaka A, Woltjen K, Miyake K et al (2013) Efficient and reproducible myogenic differentiation from human iPS cells: prospects for modeling Miyoshi Myopathy in vitro. PLoS One 8, e61540
Buckingham M, Rigby PW (2014) Gene regulatory networks and transcriptional mechanisms that control myogenesis. Dev Cell 28:225–238
Darabi R, Arpke RW, Irion S et al (2012) Human ES- and iPS-derived myogenic progenitors restore dystrophin and improve contractility upon transplantation in dystrophic mice. Cell Stem Cell 10:610–619
Hosoyama T, McGivern JV, Van Dyke JM et al (2014) Derivation of myogenic progenitors directly from human pluripotent stem cells using a sphere-based culture. Stem Cells Transl Med 3:564–574
Cao J, Li X, Lu X, Zhang C, Yu H, Zhao T (2014) Cells derived from iPSC can be immunogenic – yes or no? Protein Cell 5:1–3
Lisa Li H, Nakano T, Hotta A (2014) Genetic correction using engineered nucleases for gene therapy applications. Dev Growth Differ 56:63–77
Arpke RW, Darabi R, Mader TL et al (2013) A new immuno-, dystrophin-deficient model, the NSG-mdx(4Cv) mouse, provides evidence for functional improvement following allogeneic satellite cell transplantation. Stem Cells 31:1611–1620
Koyanagi-Aoi M, Ohnuki M, Takahashi K et al (2013) Differentiation-defective phenotypes revealed by large-scale analyses of human pluripotent stem cells. Proc Natl Acad Sci U S A 110:20569–20574
Kuroda T, Yasuda S, Kusakawa S et al (2012) Highly sensitive in vitro methods for detection of residual undifferentiated cells in retinal pigment epithelial cells derived from human iPS cells. PLoS One 7, e37342
Ben-David U, Benvenisty N (2014) Chemical ablation of tumor-initiating human pluripotent stem cells. Nat Protoc 9:729–740
Goudebege S, Lamarre Y, Dumont N et al (2010) Laminin-111: a potential therapeutic agent for Duchenne muscular dystrophy. Mol Ther 18:2155–2163
Joe AW, Yi L, Natarajan A, Le Grand F, So L et al (2010) Muscle injury activates resident fibro/adipogenic progenitors that facilitate myogenesis. Nat Cell Biol 12:153–163
Judson RN, Zhang RH, Rossi FM (2013) Tissue-resident mesenchymal stem/progenitor cells in skeletal muscle: collaborators or saboteurs? FEBS J 280:4100–4108
Uezumi A, Fukada S, Yamamoto N et al (2010) Mesenchymal progenitors distinct from satellite cells contribute to ectopic fat cell formation in skeletal muscle. Nat Cell Biol 12:143–152
Uezumi A, Ito T, Morikawa D et al (2011) Fibrosis and adipogenesis originate from a common mesenchymal progenitor in skeletal muscle. J Cell Sci 124:3654–3664
Motohashi N, Uezumi A, Yada E et al (2008) Muscle CD31(−) CD45(−) side population cells promote muscle regeneration by stimulating proliferation and migration of myoblasts. Am J Pathol 173:781–791
Tedesco FS, Gerli MF, Perani L et al (2012) Transplantation of genetically corrected human iPSC-derived progenitors in mice with limb-girdle muscular dystrophy. Sci Transl Med 4:140ra89
Acknowledgments
YS and ST are supported by grants from the Research Center Network for Realization of Regenerative Medicine (Japan Science and Technology Agency), Intramural Research Grants for Neurological and Psychiatric Disorders of NCNP(24–9), and Grants-in-Aid for Scientific Research (C) (24590497) (Japan Society for the Promotion of Science).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer Japan
About this chapter
Cite this chapter
Miyagoe-Suzuki, Y., Takeda, S. (2016). Stem Cell-Based Therapy for Duchenne Muscular Dystrophy. In: Takeda, S., Miyagoe-Suzuki, Y., Mori-Yoshimura, M. (eds) Translational Research in Muscular Dystrophy. Springer, Tokyo. https://doi.org/10.1007/978-4-431-55678-7_8
Download citation
DOI: https://doi.org/10.1007/978-4-431-55678-7_8
Published:
Publisher Name: Springer, Tokyo
Print ISBN: 978-4-431-55677-0
Online ISBN: 978-4-431-55678-7
eBook Packages: MedicineMedicine (R0)