Abstract
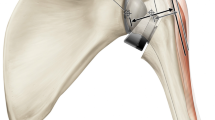
The Biomet Comprehensive® Reverse Shoulder Arthroplasty (RSA) is newer designed third-generation reverse prosthesis. Based on the concept originally developed by Grammont, the Biomet Comprehensive® RSA utilizes initial design of the reverse ball-and-socket implant while adding some newly developed technologic changes in order to avoid specific complications such as scapular notching or baseplate failure. One of these important advances in design, the Versa-Dial® glenosphere, allows for an infinite number of offset combinations in all direction on the glenoid side. When this technology is used in combination with two available sized baseplates, which have improved fixation features, it allows the surgeon to place the implant in the best bone stock and in the best possible position to prevent complications. In addition, the Biomet Comprehensive® Shoulder is based upon the concept of an universal humeral stem component platform system, which allows any humeral stem type or size to be used in this RSA system. It also makes conversion of an anatomic shoulder arthroplasty or fracture hemiarthroplasty (HA) to RSA much easier. This chapter will present the design considerations and biomechanical rationales of the Biomet Comprehensive® RSA. The surgical procedure is presented in details in order to clearly define the different technical steps for successful prosthesis implantation. Finally, newer concepts of implant placement and fixation will be discussed as our efforts to improve this technology continue.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Jasty M, Bragdon C, Burke D, O’Connor D, Lowenstein J, Harris WH. In vivo skeletal responses to porous-surfaced implants subjected to small induced motions. J Bone Joint Surg Am. 1997;79(5):707–14.
Frankle M, Siegal S, Pupello D, Saleem A, Mighell M, Vasey M. The reverse shoulder prosthesis for glenohumeral arthritis associated with severe rotator cuff deficiency. A minimum two-year follow-up study of sixty patients. J Bone Joint Surg Am. 2005;87:1697–705.
Harman M, Frankle M, Vasey M, Banks S. Initial glenoid component fixation in “reverse” total shoulder arthroplasty: a biomechanical evaluation. J Shoulder Elbow Surg. 2005;14(1 Suppl S):162S–7S.
Cuff D, Pupello D, Virani N, Levy J, Frankle M. Reverse shoulder arthroplasty for the treatment of rotator cuff deficiency. J Bone Joint Surg Am. 2008;90(6):1244–51.
Lombardi AV Jr, Berend KR, Mallory TH, Skeels MD, Adams JB. Survivorship of 2000 tapered titanium porous plasma-sprayed femoral components. Clin Orthop Relat Res. 2009;467(1):146–54.
Henninger HB, Barg A, Anderson AE, Bachus KN, Burks RT, Tashjian RZ. Effect of lateral offset center of rotation in reverse total shoulder arthroplasty: a biomechanical study. J Shoulder Elbow Surg. 2012;21(9):1128–35.
Kelly JD 2nd, Humphrey CS, Norris TR. Optimizing glenosphere position and fixation in reverse shoulder arthroplasty, part one: the twelve-mm rule. J Shoulder Elbow Surg. 2008;17:589–94.
Nyffeler RW, Werner CM, Simmen BR, Gerber C. Analysis of a retrieved delta III total shoulder prosthesis. J Bone Joint Surg Br. 2004;86:1187–91.
Nyffeler RW, Werner CM, Gerber C. Biomechanical relevance of glenoid component positioning in the reverse delta III total shoulder prosthesis. J Shoulder Elbow Surg. 2005;14:524–8.
Edwards TB, Trappey GJ, Riley C, O’Connor DP, Elkousy HA, Gartsman GM. Inferior tilt of the glenoid component does not decrease scapular notching in reverse shoulder arthroplasty: results of a prospective randomized study. J Shoulder Elbow Surg. 2012;21(5):641–6.
Simovitch R, Zumstein M, Lohri E, Helmy M, Gerber C. Predictors of scapular notching in patients managed with the delta III reverse shoulder replacement. J Bone Joint Surg Am. 2007;89:588–600.
Wiater JM, Moravek JE Jr, Budge MD, Koueiter DM, Marcantonio D, Wiater BP. Clinical and radiographic results of cementless reverse total shoulder arthroplasty: a comparative study with 2 to 5 years of follow-up. J Shoulder Elbow Surg. 2014. pii: S1058-2746(13)00607-1.
Groh GI, Groh GM. Complications rates, reoperation rates, and the learning curve in reverse shoulder arthroplasty. J Shoulder Elbow Surg. 2014;23(3):388–94.
Acevedo DC, Vanbeek C, Lazarus MD, Williams GR, Abboud JA. Reverse shoulder arthroplasty for proximal humeral fractures: update on indications, technique, and results. J Shoulder Elbow Surg. 2014;23(2):279–89.
Gutiérrez S, Luo ZP, Levy J, Frankle MA. Arc of motion and socket depth in reverse shoulder implants. Clin Biomech (Bristol, Avon). 2009;24(6):473–9.
Oh JH, Shin SJ, McGarry MH, Scott JH, Heckmann N, Lee TQ. Biomechanical effects of humeral neck-shaft angle and subscapularis integrity in reverse total shoulder arthroplasty. J Shoulder Elbow Surg. 2014. pii: S1058-2746(13) 563-6.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Berhouet, J., Sperling, J.W., Dines, D.M. (2016). The Biomet Comprehensive© Reverse Total Shoulder System Design Considerations and Surgical Techniques. In: Frankle, M., Marberry, S., Pupello, D. (eds) Reverse Shoulder Arthroplasty. Springer, Cham. https://doi.org/10.1007/978-3-319-20840-4_32
Download citation
DOI: https://doi.org/10.1007/978-3-319-20840-4_32
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-20839-8
Online ISBN: 978-3-319-20840-4
eBook Packages: MedicineMedicine (R0)