Abstract
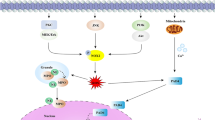
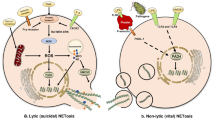
Tumor-associated neutrophils (TANs) play a major role during cancer development and progression in the tumor microenvironment. Neutrophil elastase (NE) is a serine protease normally expressed in neutrophil primary granules. Formation of neutrophil extracellular traps (NETs), a mechanism used by neutrophils, has been traditionally associated with the capture and killing of bacteria. However, there are recent discoveries suggesting that NE secretion and NETs formation are also involved in the tumor microenvironment. Here, we focus on how NE and NETs play a key regulatory function in the tumor microenvironment, such as tumor proliferation, distant metastasis, tumor-associated thrombosis, and antitumor activity. Additionally, the potential use of NETs, NE, or associated molecules as potential disease activity biomarkers or therapeutic targets will be introduced.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
Abbreviations
- CXCL:
-
C-X-C motif chemokine
- CXCR:
-
C-X-C chemokine receptor
- DNase:
-
Deoxyribonuclease
- LPS:
-
Lipopolysaccharide
- MPO:
-
Myeloperoxidase
- NE:
-
Neutrophil elastase
- NET:
-
Neutrophil extracellular trap
- PAD4:
-
Protein arginine deiminase 4
- PMA:
-
Phorbol-12-myristate-13-acetate
- PMN:
-
Polymorphonuclear neutrophil
- RA:
-
Rheumatoid arthritis
- ROS:
-
Reactive oxygen species
- SLE:
-
Systemic lupus erythematosus
- TAN:
-
Tumor-associated neutrophil
- TGF-β:
-
Transforming Growth factor-β
- TLR:
-
Toll-like receptor
References
Casanova-Acebes M, Pitaval C, Weiss LA, Nombela-Arrieta C, Chevre R, AG N et al (2013) Rhythmic modulation of the hematopoietic niche through neutrophil clearance. Cell 153(5):1025–1035
Lawrence SM, Corriden R, Nizet V (2018) The ontogeny of a neutrophil: mechanisms of granulopoiesis and homeostasis. Microbiol Mol Biol Rev 82(1):e00057–17
Borregaard N (2010) Neutrophils, from marrow to microbes. Immunity 33(5):657–670
Nathan C (2006) Neutrophils and immunity: challenges and opportunities. Nat Rev Immunol 6(3):173–182
Brinkmann V, Zychlinsky A (2007) Beneficial suicide: why neutrophils die to make NETs. Nat Rev Microbiol 5(8):577–582
Bainton DF, Ullyot JL, Farquhar MG (1971) The development of neutrophilic polymorphonuclear leukocytes in human bone marrow. J Exp Med 134(4):907–934
Shaul ME, Fridlender ZG (2017) Neutrophils as active regulators of the immune system in the tumor microenvironment. J Leukoc Biol 102(2):343–349
Wu L, Saxena S, Awaji M, Singh RK (2019) Tumor-associated neutrophils in cancer: going pro. Cancers 11(4):P5641–20
Tecchio C, Scapini P, Pizzolo G, Cassatella MA (2013) On the cytokines produced by human neutrophils in tumors. Semin Cancer Biol 23(3):159–170
Hanahan D, Weinberg RA (2011) Hallmarks of cancer: the next generation. Cell 144(5):646–674
Ocana A, Nieto-Jimenez C, Pandiella A, Templeton AJ (2017) Neutrophils in cancer: prognostic role and therapeutic strategies. Mol Cancer 16(1):137
Swierczak A, Mouchemore KA, Hamilton JA, Anderson RL (2015) Neutrophils: important contributors to tumor progression and metastasis. Cancer Metastasis Rev 34(4):735–751
Coffelt SB, Wellenstein MD, de Visser KE (2016) Neutrophils in cancer: neutral no more. Nat Rev Cancer 16(7):431–446
Fridlender ZG, Sun J, Kim S, Kapoor V, Cheng G, Ling L et al (2009) Polarization of tumor-associated neutrophil phenotype by TGF-beta: “N1” versus “N2” TAN. Cancer Cell 16(3):183–194
Fridlender ZG, Albelda SM (2012) Tumor-associated neutrophils: friend or foe? Carcinogenesis 33(5):949–955
Jamieson T, Clarke M, Steele CW, Samuel MS, Neumann J, Jung A et al (2012) Inhibition of CXCR2 profoundly suppresses inflammation-driven and spontaneous tumorigenesis. J Clin Invest 122(9):3127–3144
Antonio N, Bonnelykke-Behrndtz ML, Ward LC, Collin J, Christensen IJ, Steiniche T et al (2015) The wound inflammatory response exacerbates growth of pre-neoplastic cells and progression to cancer. EMBO J 34(17):2219–2236
Gordon-Weeks AN, Lim SY, Yuzhalin AE, Jones K, Markelc B, Kim KJ et al (2017) Neutrophils promote hepatic metastasis growth through fibroblast growth factor 2-dependent angiogenesis in mice. Hepatology (Baltimore, Md) 65(6):1920–1935
Zhou SL, Dai Z, Zhou ZJ, Wang XY, Yang GH, Wang Z et al (2012) Overexpression of CXCL5 mediates neutrophil infiltration and indicates poor prognosis for hepatocellular carcinoma. Hepatology (Baltimore, Md) 56(6):2242–2254
Wilson CL, Jurk D, Fullard N, Banks P, Page A, Luli S et al (2015) NFkappaB1 is a suppressor of neutrophil-driven hepatocellular carcinoma. Nat Commun 6:6818
Mensurado S, Rei M, Lanca T, Ioannou M, Goncalves-Sousa N, Kubo H et al (2018) Tumor-associated neutrophils suppress pro-tumoral IL-17+ gammadelta T cells through induction of oxidative stress. PLoS Biol 16(5):e2004990
Hernandez-Ilizaliturri FJ, Jupudy V, Ostberg J, Oflazoglu E, Huberman A, Repasky E et al (2003) Neutrophils contribute to the biological antitumor activity of rituximab in a non-Hodgkin’s lymphoma severe combined immunodeficiency mouse model. Clin Cancer Res 9(16 Pt 1):5866–5873
Stockmeyer B, Beyer T, Neuhuber W, Repp R, Kalden JR, Valerius T et al (2003) Polymorphonuclear granulocytes induce antibody-dependent apoptosis in human breast cancer cells. J Immunol (Baltimore, Md : 1950) 171(10):5124–5129
Simons MP, O'Donnell MA, Griffith TS (2008) Role of neutrophils in BCG immunotherapy for bladder cancer. Urol Oncol 26(4):341–345
Challacombe JM, Suhrbier A, Parsons PG, Jones B, Hampson P, Kavanagh D et al (2006) Neutrophils are a key component of the antitumor efficacy of topical chemotherapy with ingenol-3-angelate. J Immunol (Baltimore, Md : 1950) 177(11):8123–8132
Takeshima T, Pop LM, Laine A, Iyengar P, Vitetta ES, Hannan R (2016) Key role for neutrophils in radiation-induced antitumor immune responses: potentiation with G-CSF. Proc Natl Acad Sci USA 113(40):11300–11305
Otten MA, Rudolph E, Dechant M, Tuk CW, Reijmers RM, Beelen RH et al (2005) Immature neutrophils mediate tumor cell killing via IgA but not IgG Fc receptors. J Immunol (Baltimore, Md : 1950) 174(9):5472–5480
Lichtenstein A, Kahle J (1985) Anti-tumor effect of inflammatory neutrophils: characteristics of in vivo generation and in vitro tumor cell lysis. Int J Cancer 35(1):121–127
Fouret P, du Bois RM, Bernaudin JF, Takahashi H, Ferrans VJ, Crystal RG (1989) Expression of the neutrophil elastase gene during human bone marrow cell differentiation. J Exp Med 169(3):833–845
Molldrem JJ, Komanduri K, Wieder E (2002) Overexpressed differentiation antigens as targets of graft-versus-leukemia reactions. Curr Opin Hematol 9(6):503–508
Pulford KA, Erber WN, Crick JA, Olsson I, Micklem KJ, Gatter KC et al (1988) Use of monoclonal antibody against human neutrophil elastase in normal and leukaemic myeloid cells. J Clin Pathol 41(8):853–860
Korkmaz B, Moreau T, Gauthier F (2008) Neutrophil elastase, proteinase 3 and cathepsin G: physicochemical properties, activity and physiopathological functions. Biochimie 90(2):227–242
Papayannopoulos V, Metzler KD, Hakkim A, Zychlinsky A (2010) Neutrophil elastase and myeloperoxidase regulate the formation of neutrophil extracellular traps. J Cell Biol 191(3):677–691
Belorgey D, Bieth JG (1998) Effect of polynucleotides on the inhibition of neutrophil elastase by mucus proteinase inhibitor and alpha 1-proteinase inhibitor. Biochemistry 37(46):16416–16422
Honda M, Kubes P (2018) Neutrophils and neutrophil extracellular traps in the liver and gastrointestinal system. Nat Rev Gastroenterol Hepatol 15(4):206–221
Ruemmele FM, Targan SR, Levy G, Dubinsky M, Braun J, Seidman EG (1998) Diagnostic accuracy of serological assays in pediatric inflammatory bowel disease. Gastroenterology 115(4):822–829
Zhou G, Song Y, Yang W, Guo Y, Fang L, Chen Y et al (2016) ASCA, ANCA, ALCA and many more: are they useful in the diagnosis of inflammatory bowel disease? Dig Dis (Basel, Switzerland) 34(1–2):90–97
Uchiyama K, Naito Y, Takagi T, Mizushima K, Hirai Y, Hayashi N et al (2012) Serpin B1 protects colonic epithelial cell via blockage of neutrophil elastase activity and its expression is enhanced in patients with ulcerative colitis. Am J Physiol Gastrointest Liver Physiol 302(10):G1163–G1170
Kato S, Ochiai M, Sakurada T, Ohno S, Miyamoto K, Sagara M et al (2008) Increased expression of long pentraxin PTX3 in inflammatory bowel diseases. Dig Dis Sci 53(7):1910–1916
Darrah E, Andrade F (2012) NETs: the missing link between cell death and systemic autoimmune diseases? Front Immunol 3:428
Dale DC, Person RE, Bolyard AA, Aprikyan AG, Bos C, Bonilla MA et al (2000) Mutations in the gene encoding neutrophil elastase in congenital and cyclic neutropenia. Blood 96(7):2317–2322
Grenda DS, Murakami M, Ghatak J, **a J, Boxer LA, Dale D et al (2007) Mutations of the ELA2 gene found in patients with severe congenital neutropenia induce the unfolded protein response and cellular apoptosis. Blood 110(13):4179–4187
Chin AC, Lee WY, Nusrat A, Vergnolle N, Parkos CA (2008) Neutrophil-mediated activation of epithelial protease-activated receptors-1 and -2 regulates barrier function and transepithelial migration. J Immunol (Baltimore, Md: 1950) 181(8):5702–5710
Hattar K, Oppermann S, Ankele C, Weissmann N, Schermuly RT, Bohle RM et al (2010) c-ANCA-induced neutrophil-mediated lung injury: a model of acute Wegener’s granulomatosis. Eur Respir J 36(1):187–195
Massberg S, Grahl L, von Bruehl ML, Manukyan D, Pfeiler S, Goosmann C et al (2010) Reciprocal coupling of coagulation and innate immunity via neutrophil serine proteases. Nat Med 16(8):887–896
Lerman I, Hammes SR (2018) Neutrophil elastase in the tumor microenvironment. Steroids 133:96–101
Houghton AM, Rzymkiewicz DM, Ji H, Gregory AD, Egea EE, Metz HE et al (2010) Neutrophil elastase-mediated degradation of IRS-1 accelerates lung tumor growth. Nat Med 16(2):219–223
Caruso JA, Akli S, Pageon L, Hunt KK, Keyomarsi K (2015) The serine protease inhibitor elafin maintains normal growth control by opposing the mitogenic effects of neutrophil elastase. Oncogene 34(27):3556–3567
Ho AS, Chen CH, Cheng CC, Wang CC, Lin HC, Luo TY et al (2014) Neutrophil elastase as a diagnostic marker and therapeutic target in colorectal cancers. Oncotarget 5(2):473–480
Gong L, Cumpian AM, Caetano MS, Ochoa CE, De la Garza MM, Lapid DJ et al (2013) Promoting effect of neutrophils on lung tumorigenesis is mediated by CXCR2 and neutrophil elastase. Mol Cancer 12(1):154
Foekens JA, Ries C, Look MP, Gippner-Steppert C, Klijn JG, Jochum M (2003) The prognostic value of polymorphonuclear leukocyte elastase in patients with primary breast cancer. Cancer Res 63(2):337–341
Lerman I, Garcia-Hernandez ML, Rangel-Moreno J, Chiriboga L, Pan C, Nastiuk KL et al (2017) Infiltrating myeloid cells exert protumorigenic actions via neutrophil elastase. Mol Cancer Res 15(9):1138–1152
Davis RJ, Moore EC, Clavijo PE, Friedman J, Cash H, Chen Z et al (2017) Anti-PD-L1 efficacy can be enhanced by inhibition of myeloid-derived suppressor cells with a selective inhibitor of PI3Kdelta/gamma. Cancer Res 77(10):2607–2619
Pivetta E, Danussi C, Wassermann B, Modica TM, Del Bel BL, Canzonieri V et al (2014) Neutrophil elastase-dependent cleavage compromises the tumor suppressor role of EMILIN1. Matrix Biol 34:22–32
El Rayes T, Catena R, Lee S, Stawowczyk M, Joshi N, Fischbach C et al (2015) Lung inflammation promotes metastasis through neutrophil protease-mediated degradation of Tsp-1. Proc Natl Acad Sci USA 112(52):16000–16005
Grosse-Steffen T, Giese T, Giese N, Longerich T, Schirmacher P, Hansch GM et al (2012) Epithelial-to-mesenchymal transition in pancreatic ductal adenocarcinoma and pancreatic tumor cell lines: the role of neutrophils and neutrophil-derived elastase. Clin Dev Immunol 2012:720768
Wada Y, Yoshida K, Tsutani Y, Shigematsu H, Oeda M, Sanada Y et al (2007) Neutrophil elastase induces cell proliferation and migration by the release of TGF-alpha, PDGF and VEGF in esophageal cell lines. Oncol Rep 17(1):161–167
Inoue H, Kazawa T, Sato Y, Satodate H, Sasajima K, Kudo SE et al (2004) In vivo observation of living cancer cells in the esophagus, stomach, and colon using catheter-type contact endoscope, “Endo-Cytoscopy system”. Gastrointest Endosc Clin N Am 14(3):589–594. x-xi
Yamashita J, Ogawa M, Abe M, Hayashi N, Kurusu Y, Kawahara K et al (1997) Tumor neutrophil elastase is closely associated with the direct extension of non-small cell lung cancer into the aorta. Chest 111(4):885–890
Mittendorf EA, Alatrash G, Qiao N, Wu Y, Sukhumalchandra P, St John LS et al (2012) Breast cancer cell uptake of the inflammatory mediator neutrophil elastase triggers an anticancer adaptive immune response. Cancer Res 72(13):3153–3162
Topic A, Ljujic M, Nikolic A, Petrovic-Stanojevic N, Dopudja-Pantic V, Mitic-Milikic M et al (2011) Alpha-1-antitrypsin phenotypes and neutrophil elastase gene promoter polymorphisms in lung cancer. Pathol Oncol Res 17(1):75–80
Foekens JA, Ries C, Look MP, Gippner-Steppert C, Klijn JG, Jochum M (2003) Elevated expression of polymorphonuclear leukocyte elastase in breast cancer tissue is associated with tamoxifen failure in patients with advanced disease. Br J Cancer 88(7):1084–1090
Rotondo R, Barisione G, Mastracci L, Grossi F, Orengo AM, Costa R et al (2009) IL-8 induces exocytosis of arginase 1 by neutrophil polymorphonuclears in nonsmall cell lung cancer. Int J Cancer 125(4):887–893
Mayadas TN, Cullere X, Lowell CA (2014) The multifaceted functions of neutrophils. Annu Rev Pathol 9:181–218
Tomizawa N, Ohwada S, Ohya T, Kawashima Y, Takeyoshi I, Morishita Y (1999) The effect of neutrophil elastase inhibitor in hepatectomy with ischemia in dogs. J Surg Res 81(2):230–237
Yamaguchi Y, Akizuki E, Ichiguchi O, Matsumura F, Goto M, Miyanari N et al (1997) Neutrophil elastase inhibitor reduces neutrophil chemoattractant production after ischemia-reperfusion in rat liver. Gastroenterology 112(2):551–560
Doi K, Horiuchi T, Uchinami M, Tabo T, Kimura N, Yokomachi J et al (2002) Neutrophil elastase inhibitor reduces hepatic metastases induced by ischaemia-reperfusion in rats. Eur J Surg Acta Chir 168(8–9):507–510
Chawla A, Alatrash G, Philips AV, Qiao N, Sukhumalchandra P, Kerros C et al (2016) Neutrophil elastase enhances antigen presentation by upregulating human leukocyte antigen class I expression on tumor cells. Cancer Immunol Immunother 65(6):741–751
Aikawa N, Kawasaki Y (2014) Clinical utility of the neutrophil elastase inhibitor sivelestat for the treatment of acute respiratory distress syndrome. Ther Clin Risk Manag 10:621–629
Aikawa N, Ishizaka A, Hirasawa H, Shimazaki S, Yamamoto Y, Sugimoto H et al (2011) Reevaluation of the efficacy and safety of the neutrophil elastase inhibitor, Sivelestat, for the treatment of acute lung injury associated with systemic inflammatory response syndrome; a phase IV study. Pulm Pharmacol Ther 24(5):549–554
Stevens T, Ekholm K, Granse M, Lindahl M, Kozma V, Jungar C et al (2011) AZD9668: pharmacological characterization of a novel oral inhibitor of neutrophil elastase. J Pharmacol Exp Ther 339(1):313–320
von Nussbaum F, Li VM, Allerheiligen S, Anlauf S, Barfacker L, Bechem M et al (2015) Freezing the bioactive conformation to boost potency: the identification of BAY 85-8501, a selective and potent inhibitor of human neutrophil elastase for pulmonary diseases. ChemMedChem 10(7):1163–1173
Brinkmann V, Reichard U, Goosmann C, Fauler B, Uhlemann Y, Weiss DS et al (2004) Neutrophil extracellular traps kill bacteria. Science (New York, NY) 303(5663):1532–1535
Wang Y, Li M, Stadler S, Correll S, Li P, Wang D et al (2009) Histone hypercitrullination mediates chromatin decondensation and neutrophil extracellular trap formation. J Cell Biol 184(2):205–213
Urban CF, Reichard U, Brinkmann V, Zychlinsky A (2006) Neutrophil extracellular traps capture and kill Candida albicans yeast and hyphal forms. Cell Microbiol 8(4):668–676
Saitoh T, Komano J, Saitoh Y, Misawa T, Takahama M, Kozaki T et al (2012) Neutrophil extracellular traps mediate a host defense response to human immunodeficiency virus-1. Cell Host Microbe 12(1):109–116
Abi Abdallah DS, Lin C, Ball CJ, King MR, Duhamel GE, Denkers EY (2012) Toxoplasma gondii triggers release of human and mouse neutrophil extracellular traps. Infect Immun 80(2):768–777
Walker MJ, Hollands A, Sanderson-Smith ML, Cole JN, Kirk JK, Henningham A et al (2007) DNase Sda1 provides selection pressure for a switch to invasive group A streptococcal infection. Nat Med 13(8):981–985
Branzk N, Lubojemska A, Hardison SE, Wang Q, Gutierrez MG, Brown GD et al (2014) Neutrophils sense microbe size and selectively release neutrophil extracellular traps in response to large pathogens. Nat Immunol 15(11):1017–1025
Berthelot JM, Le Goff B, Neel A, Maugars Y, Hamidou M (2017) NETosis: at the crossroads of rheumatoid arthritis, lupus, and vasculitis. Joint Bone Spine 84(3):255–262
Yipp BG, Kubes P (2013) NETosis: how vital is it? Blood 122(16):2784–2794
Fuchs TA, Abed U, Goosmann C, Hurwitz R, Schulze I, Wahn V et al (2007) Novel cell death program leads to neutrophil extracellular traps. J Cell Biol 176(2):231–241
Sollberger G, Tilley DO, Zychlinsky A (2018) Neutrophil extracellular traps: the biology of chromatin externalization. Dev Cell 44(5):542–553
Barnado A, Crofford LJ, Oates JC (2016) At the bedside: neutrophil extracellular traps (NETs) as targets for biomarkers and therapies in autoimmune diseases. J Leukoc Biol 99(2):265–278
Yang H, Biermann MH, Brauner JM, Liu Y, Zhao Y, Herrmann M (2016) New insights into neutrophil extracellular traps: mechanisms of formation and role in inflammation. Front Immunol 7:302
Papayannopoulos V (2018) Neutrophil extracellular traps in immunity and disease. Nat Rev Immunol 18(2):134–147
Hakkim A, Furnrohr BG, Amann K, Laube B, Abed UA, Brinkmann V et al (2010) Impairment of neutrophil extracellular trap degradation is associated with lupus nephritis. Proc Natl Acad Sci USA 107(21):9813–9818
Pinegin B, Vorobjeva N, Pinegin V (2015) Neutrophil extracellular traps and their role in the development of chronic inflammation and autoimmunity. Autoimmun Rev 14(7):633–640
Lood C, Blanco LP, Purmalek MM, Carmona-Rivera C, De Ravin SS, Smith CK et al (2016) Neutrophil extracellular traps enriched in oxidized mitochondrial DNA are interferogenic and contribute to lupus-like disease. Nat Med 22(2):146–153
Warnatsch A, Ioannou M, Wang Q, Papayannopoulos V (2015) Inflammation. Neutrophil extracellular traps license macrophages for cytokine production in atherosclerosis. Science (New York, NY) 349(6245):316–320
Caudrillier A, Kessenbrock K, Gilliss BM, Nguyen JX, Marques MB, Monestier M et al (2012) Platelets induce neutrophil extracellular traps in transfusion-related acute lung injury. J Clin Invest 122(7):2661–2671
de Jong HK, Koh GC, Achouiti A, van der Meer AJ, Bulder I, Stephan F et al (2014) Neutrophil extracellular traps in the host defense against sepsis induced by Burkholderia pseudomallei (melioidosis). Intensive Care Med Exp 2(1):21
Lee SK, Kim SD, Kook M, Lee HY, Ghim J, Choi Y et al (2015) Phospholipase D2 drives mortality in sepsis by inhibiting neutrophil extracellular trap formation and down-regulating CXCR2. J Exp Med 212(9):1381–1390
Sakurai K, Miyashita T, Okazaki M, Yamaguchi T, Ohbatake Y, Nakanuma S et al (2017) Role for neutrophil extracellular traps (NETs) and platelet aggregation in early sepsis-induced hepatic dysfunction. In vivo (Athens, Greece) 31(6):1051–1058
Jorch SK, Kubes P (2017) An emerging role for neutrophil extracellular traps in noninfectious disease. Nat Med 23(3):279–287
Wong SL, Demers M, Martinod K, Gallant M, Wang Y, Goldfine AB et al (2015) Diabetes primes neutrophils to undergo NETosis, which impairs wound healing. Nat Med 21(7):815–819
Yazdani HO, Chen HW, Tohme S, Tai S, van der Windt DJ, Loughran P et al (2017) IL-33 exacerbates liver sterile inflammation by amplifying neutrophil extracellular trap formation. J Hepatol 68(1)130–139
Huang H, Tohme S, Al-Khafaji AB, Tai S, Loughran P, Chen L et al (2015) Damage-associated molecular pattern-activated neutrophil extracellular trap exacerbates sterile inflammatory liver injury. Hepatology (Baltimore, Md) 62(2):600–614
Fuchs TA, Brill A, Duerschmied D, Schatzberg D, Monestier M, Myers DD Jr et al (2010) Extracellular DNA traps promote thrombosis. Proc Natl Acad Sci USA 107(36):15880–15885
van der Windt DJ, Sud V, Zhang H, Varley PR, Goswami J, Yazdani HO et al (2018) Neutrophil extracellular traps promote inflammation and development of hepatocellular carcinoma in nonalcoholic steatohepatitis. Hepatology (Baltimore, Md) 68(4):1347–1360
Demers M, Krause DS, Schatzberg D, Martinod K, Voorhees JR, Fuchs TA et al (2012) Cancers predispose neutrophils to release extracellular DNA traps that contribute to cancer-associated thrombosis. Proc Natl Acad Sci USA 109(32):13076–13081
Levi M (2016) Management of cancer-associated disseminated intravascular coagulation. Thromb Res 140(Suppl 1):S66–S70
Guglietta S, Chiavelli A, Zagato E, Krieg C, Gandini S, Ravenda PS et al (2016) Coagulation induced by C3aR-dependent NETosis drives protumorigenic neutrophils during small intestinal tumorigenesis. Nat Commun 7:11037
Ho-Tin-Noe B, Carbo C, Demers M, Cifuni SM, Goerge T, Wagner DD (2009) Innate immune cells induce hemorrhage in tumors during thrombocytopenia. Am J Pathol 175(4):1699–1708
Cedervall J, Zhang Y, Huang H, Zhang L, Femel J, Dimberg A et al (2015) Neutrophil extracellular traps accumulate in peripheral blood vessels and compromise organ function in tumor-bearing animals. Cancer Res 75(13):2653–2662
Cools-Lartigue J, Spicer J, McDonald B, Gowing S, Chow S, Giannias B et al (2013) Neutrophil extracellular traps sequester circulating tumor cells and promote metastasis. J Clin Invest 123(8):3446–3458
Tohme S, Yazdani HO, Al-Khafaji AB, Chidi AP, Loughran P, Mowen K et al (2016) Neutrophil extracellular traps promote the development and progression of liver metastases after surgical stress. Cancer Res 76(6):1367–1380
Millrud CR, Kagedal A, Kumlien Georen S, Winqvist O, Uddman R, Razavi R et al (2017) NET-producing CD16(high) CD62L(dim) neutrophils migrate to tumor sites and predict improved survival in patients with HNSCC. Int J Cancer 140(11):2557–2567
Cedervall J, Olsson AK (2016) Immunity gone astray – NETs in cancer. Trends Cancer 2(11):633–634
Zhang LM, Chen JH (2015) Progression of NETs correlating with tumor-related diseases. Asian Pac J Cancer Prev 16(17):7431–7434
Chang X, Han J (2006) Expression of peptidylarginine deiminase type 4 (PAD4) in various tumors. Mol Carcinog 45(3):183–196
Chang X, Han J, Pang L, Zhao Y, Yang Y, Shen Z (2009) Increased PADI4 expression in blood and tissues of patients with malignant tumors. BMC Cancer 9:40
Li P, Li M, Lindberg MR, Kennett MJ, **ong N, Wang Y (2010) PAD4 is essential for antibacterial innate immunity mediated by neutrophil extracellular traps. J Exp Med 207(9):1853–1862
Li P, Wang D, Yao H, Doret P, Hao G, Shen Q et al (2010) Coordination of PAD4 and HDAC2 in the regulation of p53-target gene expression. Oncogene 29(21):3153–3162
Li P, Yao H, Zhang Z, Li M, Luo Y, Thompson PR et al (2008) Regulation of p53 target gene expression by peptidylarginine deiminase 4. Mol Cell Biol 28(15):4745–4758
Conflicts of Interest
The authors have nothing to disclose.
Funding
This work was supported by the grants from the National Institute of Health, T32AI 106704-01A1 (AEO), CA214865-01 (AT) and GM095566-06 (AT).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 The Editor(s) (if applicable) and The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Huang, H., Zhang, H., Onuma, A.E., Tsung, A. (2020). Neutrophil Elastase and Neutrophil Extracellular Traps in the Tumor Microenvironment. In: Birbrair, A. (eds) Tumor Microenvironment. Advances in Experimental Medicine and Biology, vol 1263. Springer, Cham. https://doi.org/10.1007/978-3-030-44518-8_2
Download citation
DOI: https://doi.org/10.1007/978-3-030-44518-8_2
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-44517-1
Online ISBN: 978-3-030-44518-8
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)