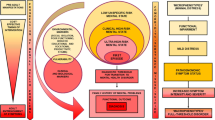
Abstract
Mental health is a key health issue faced by young people globally. Young people bear the largest burden of mental illness, with the majority of adult-type mental illnesses emerging during the transition from childhood to adulthood. This developmental timing of mental illness onset can significantly disrupt a young person’s life course. Despite young people being disproportionately impacted by mental illness, they have the worst access to mental health care. Traditional models of care are out-dated and reflect neither the pattern of mental disorder onset nor the unique cultural and developmental needs of young people. Although reform in the delivery of youth mental health services has gained traction, this transformational task is still in its infancy. Here, we outline current service innovations and describe future directions to enhance and strengthen youth models of care.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Mokdad AH, Forouzanfar MH, Daoud F, Mokdad AA, El Bcheraoui C, Moradi-Lakeh M, et al. Global burden of diseases, injuries, and risk factors for young people’s health during 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2016;387:2383–401.
Insel TR, Fenton WS. Psychiatric epidemiology: it’s not just about counting anymore. Arch Gen Psychiatry. 2005;62:590–2.
Kessler RC, Berglund P, Demler O, ** R, Merikangas KR, Walters EE. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005;62:593–602.
Gibb SJ, Fergusson DM, Horwood LJ. Burden of psychiatric disorder in young adulthood and life outcomes at age 30. Br J Psychiatry. 2010;197:122–7.
McGorry PD. The specialist youth mental health model: strengthening the weakest link in the public mental health system. Med J Aust. 2007;187:S53–6.
Hosie A, Vogl G, Carden J, Hoddinott J, Lim S. A way forward: equip** Australia’s mental health system for the next generation: EY and ReachOut Australia; 2015.
Access Economics. The economic impact of youth mental illness and the cost effectiveness of early intervention. Melbourne: Access Economics Pty Limited; 2009.
Patel V, Saxena S, Lund C, Thornicroft G, Baingana F, Bolton P, et al. The Lancet Commission on global mental health and sustainable development. Lancet. 2018;392:1553–98.
Burgess PM, Pirkis JE, Slade TN, Johnston AK, Meadows GN, Gunn JM. Service use for mental health problems: findings from the 2007 National Survey of Mental Health and Wellbeing. Aust N Z J Psychiatry. 2009;43:615–23.
Hetrick SE, Bailey AP, Smith KE, Malla A, Mathias S, Singh SP, et al. Integrated (one-stop shop) youth health care: best available evidence and future directions. Med J Aust. 2017;207:S5–18.
Rickwood DJ, Deane FP, Wilson CJ. When and how do young people seek professional help for mental health problems? Med J Aust. 2007;187:S35–9.
Rickwood DJ, Mazzer KR, Telford NR. Social influences on seeking help from mental health services, in-person and online, during adolescence and young adulthood. BMC Psychiatry. 2015;15:40.
Lawrence D, Johnson S, Hafekost J, Boterhoven De Haan K, Sawyer M, Ainley J, et al. The mental health of children and adolescents. Report on the second Australian Child and Adolescent Survey of Mental Health and Wellbeing. Canberra: Department of Health; 2015.
Singh SP, Paul M, Ford T, Kramer T, Weaver T, McLaren S, et al. Process, outcome and experience of transition from child to adult mental healthcare: multiperspective study. Br J Psychiatry. 2010;197:305–12.
Perera RH, Rogers SL, Edwards S, Hudman P, Malone C. Determinants of transition from child and adolescent to adult mental health services: a Western Australian pilot study. Aust Psychol. 2017;52:184–90.
Dunn V. Young people, mental health practitioners and researchers co-produce a Transition Preparation Programme to improve outcomes and experience for young people leaving Child and Adolescent Mental Health Services (CAMHS). BMC Health Serv Res. 2017;17:293.
Singh SP. Transition of care from child to adult mental health services: the great divide. Curr Opin Psychiatry. 2009;22:386–90.
Arnett JJ, Žukauskienė R, Sugimura K. The new life stage of emerging adulthood at ages 18–29 years: implications for mental health. Lancet Psychiatry. 2014;1:569–76.
Sawyer SM, Azzopardi PS, Wickremarathne D, Patton GC. The age of adolescence. Lancet Child Adolesc Health. 2018;2:223–8.
Lebel C, Beaulieu C. Longitudinal development of human brain wiring continues from childhood into adulthood. J Neurosci. 2011;31:10937–47.
Twenge JM, Park H. The decline in adult activities among U.S. adolescents, 1976-2016. Child Dev. 2019;90:638–54.
Australian Institute of Health and Welfare. Australia’s welfare 2017. Australia’s welfare series no. 13. AUS 214. Canberra: AIHW; 2017.
Parent AS, Teilmann G, Juul A, Skakkebaek NE, Toppari J, Bourguignon JP. The timing of normal puberty and the age limits of sexual precocity: variations around the world, secular trends, and changes after migration. Endocr Rev. 2003;24:668–93.
Weinberger AH, Gbedemah M, Martinez AM, Nash D, Galea S, Goodwin RD. Trends in depression prevalence in the USA from 2005 to 2015: widening disparities in vulnerable groups. Psychol Med. 2018;48:1308–15.
Collishaw S. Annual research review: secular trends in child and adolescent mental health. J Child Psychol Psychiatry. 2015;56:370–93.
Sellers R, Warne N, Pickles A, Maughan B, Thapar A, Collishaw S. Cross-cohort change in adolescent outcomes for children with mental health problems. J Child Psychol Psychiatry. 2019;60:813.
Twenge JM. Time period and birth cohort differences in depressive symptoms in the U.S., 1982–2013. Soc Indic Res. 2015;121:437–54.
McGorry PD, Tanti C, Stokes R, Hickie IB, Carnell K, Littlefield LK, et al. Headspace: Australia’s National Youth Mental Health Foundation - where young minds come first. Med J Aust. 2007;187:S68–70.
McGorry PD, Goldstone SD, Parker AG, Rickwood DJ, Hickie IB. Cultures for mental health care of young people: an Australian blueprint for reform. Lancet Psychiatry. 2014;1:559–68.
McLaren S, Belling R, Paul M, Ford T, Kramer T, Weaver T, et al. ‘Talking a different language’: an exploration of the influence of organizational cultures and working practices on transition from child to adult mental health services. BMC Health Serv Res. 2013;13:254.
Correll CU, Galling B, Pawar A, Krivko A, Bonetto C, Ruggeri M, et al. Comparison of early intervention services vs treatment as usual for early-phase psychosis: a systematic review, meta-analysis, and metaregression. JAMA Psychiatry. 2018;75:555–65.
van der Gaag M, Smit F, Bechdolf A, French P, Linszen DH, Yung AR, et al. Preventing a first episode of psychosis: meta-analysis of randomized controlled prevention trials of 12 month and longer-term follow-ups. Schizophr Res. 2013;149:56–62.
McGorry PD. Early intervention in psychosis: obvious, effective, overdue. J Nerv Ment Dis. 2015;203:310–8.
McGorry PD, Hickie IB, Yung AR, Pantelis C, Jackson HJ. Clinical staging of psychiatric disorders: a heuristic framework for choosing earlier, safer and more effective interventions. Aust N Z J Psychiatry. 2006;40:616–22.
Illback RJ, Bates T. Transforming youth mental health services and supports in Ireland. Early Interv Psychiatry. 2011;5:S22–7.
Iyer SN, Boksa P, Lal S, Shah J, Marandola G, Jordan G, et al. Transforming youth mental health: a Canadian perspective. Ir J Psychol Med. 2015;32:51–60.
Vyas NS, Birchwood M, Singh SP. Youth services: meeting the mental health needs of adolescents. Ir J Psychol Med. 2014;32:13–9.
McGorry P, Bates T, Birchwood M. Designing youth mental health services for the 21st century: examples from Australia, Ireland and the UK. Br J Psychiatry. 2013;202:S30–5.
Rickwood D, Paraskakis M, Quin D, Hobbs N, Ryall V, Trethowan J, et al. Australia’s innovation in youth mental health care: the headspace centre model. Early Interv Psychiatry. 2019;13:159–66.
Rickwood DJ, Mazzer KR, Telford NR, Parker AG, Tanti CJ, McGorry PD. Changes in psychological distress and psychosocial functioning in young people visiting headspace centres for mental health problems. Med J Aust. 2015;202:537–42.
Scott EM, Hermens DF, Naismith SL, White D, Whitwell B, Guastella AJ, et al. Thoughts of death or suicidal ideation are common in young people aged 12 to 30 years presenting for mental health care. BMC Psychiatry. 2012;12:234.
Rickwood DJ, Telford NR, Parker AG, Tanti CJ, McGorry PD. Headspace – Australia’s innovation in youth mental health: who are the clients and why are they presenting? Med J Aust. 2014;200:108–11.
Hilferty F, Cassells R, Muir K, Duncan A, Christensen D, Mitrou F, et al. Is headspace making a difference to young people’s lives? Final report of the independent evaluation of the headspace program. Sydney: Social Policy Research Centre; 2015.
Headspace. Annual report 2018–2019. Headspace National Youth Mental Health Foundation; 2019.
Rickwood D, Nicholas A, Mazzer K, Telford N, Parker A, Tanti C, et al. Satisfaction with youth mental health services: further scale development and findings from headspace – Australia’s National Youth Mental Health Foundation. Early Interv Psychiatry. 2017;11:296–305.
O’Keeffe L, O’Reilly A, O’Brien G, Buckley R, Illback R. Description and outcome evaluation of Jigsaw: an emergent Irish mental health early intervention programme for young people. Ir J Psychol Med. 2015;32:71–7.
Malla A, Iyer S, Shah J, Joober R, Boksa P, Lal S, et al. Canadian response to need for transformation of youth mental health services: ACCESS Open Minds (Esprits ouverts). Early Interv Psychiatry. 2019;13:697–706.
McGorry P, Trethowan J, Rickwood D. Creating headspace for integrated youth mental health care. World Psychiatry. 2019;18:140–1.
Hiscock H, Neely RJ, Lei S, Freed G. Paediatric mental and physical health presentations to emergency departments, Victoria, 2008-15. Med J Aust. 2018;208:343–8.
McGorry PD, Hamilton MP. Broken promises and missing steps in mental health reform. Med J Aust. 2017;206:487–9.
McGorry PD, Ratheesh A, O’Donoghue B. Early intervention - an implementation challenge for 21st century mental health care. JAMA Psychiatry. 2018;75:545–6.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
McGorry, P.D., Mei, C. (2020). Unmet Needs in Youth Mental Health: Transforming Models of Care to Improve Outcomes. In: Pompili, M., McIntyre, R., Fiorillo, A., Sartorius, N. (eds) New Directions in Psychiatry. Springer, Cham. https://doi.org/10.1007/978-3-030-42637-8_11
Download citation
DOI: https://doi.org/10.1007/978-3-030-42637-8_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-42636-1
Online ISBN: 978-3-030-42637-8
eBook Packages: MedicineMedicine (R0)