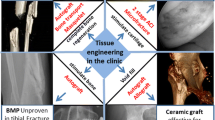
Abstract
Bone is one of the few tissues to display a true potential for regeneration. Fracture healing is an obvious example where regeneration occurs through tightly regulated sequences of molecular and cellular events which recapitulate tissue formation seen during embryogenesis. Still in some instances, bone regeneration does not occur properly (i.e. critical size lesions) and an appropriate therapeutic intervention is necessary. Successful replacement of bone by tissue engineering will likely depend on the recapitulation of this flow of events. In fact, bone regeneration requires cross-talk between microenvironmental factors and cells; for example, resident mesenchymal progenitors are recruited and properly guided by soluble and insoluble signaling molecules. Tissue engineering attempts to reproduce and to mimic this natural milieu by delivering cells capable of differentiating into osteoblasts, inducing growth factors and biomaterials to support cellular attachment, proliferation, migration, and matrix deposition. In the last two decades, a significant effort has been made by the scientific community in the development of methods and protocols to repair and regenerate tissues such as bone, cartilage, tendons, and ligaments. In this same period, great advancements have been achieved in the biology of stem cells and on the mechanisms governing “stemness”. Unfortunately, after two decades, effective clinical translation does not exist, besides a few limited examples. Many years have passed since cell-based regenerative therapies were first described as “promising approaches”, but this definition still engulfs the present literature. Failure to envisage translational cell therapy applications in routine medical practice evidences the existence of unresolved scientific and technical struggles, some of which still puzzle researchers in the field and are presented in this chapter.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Bosch P, Musgrave DS, Lee JY et al (2000) Osteoprogenitor cells within skeletal muscle. J Orthop Res 18:933–944
Doherty MJ, Ashton BA, Walsh S et al (1998) Vascular pericytes express osteogenic potential in vitro and in vivo. J Bone Miner Res 13:828–838
Friedenstein AJ, Piatetzky S II, Petrakova KV (1966) Osteogenesis in transplants of bone marrow cells. J Embryol Exp Morphol 16:381–390
Huang JI, Beanes SR, Zhu M et al (2002) Rat extramedullary adipose tissue as a source of osteochondrogenic progenitor cells. Plast Reconstr Surg 109:1033–1041, discussion 1042–1043
Levy MM, Joyner CJ, Virdi AS et al (2001) Osteoprogenitor cells of mature human skeletal muscle tissue: an in vitro study. Bone 29:317–322
Mizuno S, Glowacki J (1996) Three-dimensional composite of demineralized bone powder and collagen for in vitro analysis of chondroinduction of human dermal fibroblasts. Biomaterials 17:1819–1825
Schantz JT, Hutmacher DW, Chim H et al (2002) Induction of ectopic bone formation by using human periosteal cells in combination with a novel scaffold technology. Cell Transplant 11:125–138
Zuk PA, Zhu M, Mizuno H et al (2001) Multilineage cells from human adipose tissue: implications for cell-based therapies. Tissue Eng 7:211–228
Antonucci I, Stuppia L, Kaneko Y et al (2011) Amniotic fluid as a rich source of mesenchymal stromal cells for transplantation therapy. Cell Transplant 20:789–795
Poloni A, Maurizi G, Babini L et al (2011) Human mesenchymal stem cells from chorionic villi and amniotic fluid are not susceptible to transformation after extensive in vitro expansion. Cell Transplant 20:643–654
Ioan-Facsinay A, Kloppenburg M (2011) An emerging player in knee osteoarthritis: the infrapatellar fat pad. Arthritis Res Ther 15:225
Fan J, Varshney RR, Ren L et al (2009) Synovium-derived mesenchymal stem cells: a new cell source for musculoskeletal regeneration. Tissue Eng Part B Rev 15:75–86
Corrao S, La Rocca G, Lo Iacono M et al (2013) Umbilical cord revisited: from Wharton's jelly myofibroblasts to mesenchymal stem cells. Histol Histopathol 28:1235–1244
Bianco P, Gehron Robey P (2000) Marrow stromal stem cells. J Clin Invest 105:1663–1668
Bianco P, Riminucci M, Gronthos S et al (2001) Bone marrow stromal stem cells: nature, biology, and potential applications. Stem Cells 19:180–192
Gronthos S, Simmons PJ (1995) The growth factor requirements of STRO-1-positive human bone marrow stromal precursors under serum-deprived conditions in vitro. Blood 85:929–940
Lennon DP, Haynesworth SE, Young RG et al (1995) A chemically defined medium supports in vitro proliferation and maintains the osteochondral potential of rat marrow-derived mesenchymal stem cells. Exp Cell Res 219:211–222
Locklin RM, Oreffo RO, Triffitt JT (1999) Effects of TGFbeta and bFGF on the differentiation of human bone marrow stromal fibroblasts. Cell Biol Int 23:185–194
Quito FL, Beh J, Bashayan O et al (1996) Effects of fibroblast growth factor-4 (k-FGF) on long-term cultures of human bone marrow cells. Blood 87:1282–1291
Bartholomew A, Patil S, Mackay A et al (2001) Baboon mesenchymal stem cells can be genetically modified to secrete human erythropoietin in vivo. Hum Gene Ther 12:1527–1541
Chuah MK, Van Damme A, Zwinnen H et al (2000) Long-term persistence of human bone marrow stromal cells transduced with factor VIII-retroviral vectors and transient production of therapeutic levels of human factor VIII in nonmyeloablated immunodeficient mice. Hum Gene Ther 11:729–738
Daga A, Muraglia A, Quarto R et al (2002) Enhanced engraftment of EPO-transduced human bone marrow stromal cells transplanted in a 3D matrix in non-conditioned NOD/SCID mice. Gene Ther 9:915–921
Mizuno H, Zuk PA, Zhu M et al (2002) Myogenic differentiation by human processed lipoaspirate cells. Plast Reconstr Surg 109:199–209, discussion 210-211
Luria EA, Panasyuk AF, Friedenstein AY (1971) Fibroblast colony formation from monolayer cultures of blood cells. Transfusion 11:345–349
Lange C, Kaltz C, Thalmeier K et al (1999) Hematopoietic reconstitution of syngeneic mice with a peripheral blood-derived, monoclonal CD34-, Sca-1+, Thy-1(low), c-kit + stem cell line. J Hematother Stem Cell Res 8:335–342
Hoogduijn MJ, Verstegen MM, Engela AU et al (2014) No evidence for circulating mesenchymal stem cells in patients with organ injury. Stem Cells Dev 23:2328–2335
Breton P, Freidel M (1993) Hydroxyapatite in orthognathic surgery. Animal experimentation and clinical applications. Rev Stomatol Chir Maxillofac 94:115–119
Chappard D, Zhioua A, Grizon F et al (1993) Biomaterials for bone filling: comparisons between autograft, hydroxyapatite and one highly purified bovine xenograft. Bull Assoc Anat (Nancy) 77:59–65
Erickson D (1991) Binding bone. Will new bioceramic coatings improve orthopedic implants? Sci Am 265:101–102
Heise U, Osborn JF, Duwe F (1990) Hydroxyapatite ceramic as a bone substitute. Int Orthop 14:329–338
Oonishi H (1991) Orthopaedic applications of hydroxyapatite. Biomaterials 12:171–178
Langstaff S, Sayer M, Smith TJ et al (1999) Resorbable bioceramics based on stabilized calcium phosphates. Part I: rational design, sample preparation and material characterization. Biomaterials 20:1727–1741
Johnson KD, Frierson KE, Keller TS et al (1996) Porous ceramics as bone graft substitutes in long bone defects: a biomechanical, histological, and radiographic analysis. J Orthop Res 14:351–369
Kuhne JH, Bartl R, Frisch B et al (1994) Bone formation in coralline hydroxyapatite. Effects of pore size studied in rabbits. Acta Orthop Scand 65:246–252
Sartoris DJ, Holmes RE, Resnick D (1992) Coralline hydroxyapatite bone graft substitutes: radiographic evaluation. J Foot Surg 31:301–313
Misch CE, Dietsh F (1993) Bone-grafting materials in implant dentistry. Implant Dent 2:158–167
Mastrogiacomo M, Papadimitropoulos A, Cedola A et al (2007) Engineering of bone using bone marrow stromal cells and a silicon-stabilized tricalcium phosphate bioceramic: evidence for a coupling between bone formation and scaffold resorption. Biomaterials 28:1376–1384
Steinert AF, Rackwitz L, Gilbert F et al (2012) Concise review: the clinical application of mesenchymal stem cells for musculoskeletal regeneration: current status and perspectives. Stem Cells Transl Med 1:237–247
Herrmann RP, Sturm MJ (2014) Adult human mesenchymal stromal cells and the treatment of graft versus host disease. Stem Cells Cloning 7:45–52
Battiwalla M, Barrett AJ (2014) Bone marrow mesenchymal stromal cells to treat complications following allogeneic stem cell transplantation. Tissue Eng Part B Rev 20:211–217
El-Ghannam A (2005) Bone reconstruction: from bioceramics to tissue engineering. Expert Rev Med Devices 2:87–101
Giannoni P, Scaglione S, Daga A et al (2010) Short-time survival and engraftment of bone marrow stromal cells in an ectopic model of bone regeneration. Tissue Eng Part A 16:489–499
Martino G, Pluchino S (2006) The therapeutic potential of neural stem cells. Nat Rev Neurosci 7:395–406
Sart S, Ma T, Li Y (2014) Preconditioning stem cells for in vivo delivery. Biores Open Access 3:137–149
Giannoni P, Cancedda R (2004) Regulatory issues: down to the bare bones. In: Petit H, Quarto R (eds) Engineering bone. Landes Bioscience Publishers, Georgetown, TX, pp 205–219
Pietila M, Lehtonen S, Narhi M et al (2010) Mitochondrial function determines the viability and osteogenic potency of human mesenchymal stem cells. Tissue Eng Part C Methods 16:435–445
Voog J, Jones DL (2010) Stem cells and the niche: a dynamic duo. Cell Stem Cell 6:103–115
Chastain SR, Kundu AK, Dhar S et al (2006) Adhesion of mesenchymal stem cells to polymer scaffolds occurs via distinct ECM ligands and controls their osteogenic differentiation. J Biomed Mater Res A 78:73–85
Hamidouche Z, Hay E, Vaudin P et al (2008) FHL2 mediates dexamethasone-induced mesenchymal cell differentiation into osteoblasts by activating Wnt/beta-catenin signaling-dependent Runx2 expression. FASEB J 22:3813–3822
Lee JW, Juliano R (2004) Mitogenic signal transduction by integrin- and growth factor receptor-mediated pathways. Mol Cells 17:188–202
Discher DE, Janmey P, Wang YL (2005) Tissue cells feel and respond to the stiffness of their substrate. Science 310:1139–1143
Engler AJ, Sen S, Sweeney HL et al (2006) Matrix elasticity directs stem cell lineage specification. Cell 126:677–689
Vogel V, Sheetz M (2006) Local force and geometry sensing regulate cell functions. Nat Rev Mol Cell Biol 7:265–275
Dahl KN, Engler AJ, Pajerowski JD et al (2005) Power-law rheology of isolated nuclei with deformation map** of nuclear substructures. Biophys J 89:2855–2864
Dalby MJ, Gadegaard N, Herzyk P et al (2007) Nanomechanotransduction and interphase nuclear organization influence on genomic control. J Cell Biochem 102:1234–1244
Balasundaram G, Sato M, Webster TJ (2006) Using hydroxyapatite nanoparticles and decreased crystallinity to promote osteoblast adhesion similar to functionalizing with RGD. Biomaterials 27:2798–2805
Hollister SJ, Maddox RD, Taboas JM (2002) Optimal design and fabrication of scaffolds to mimic tissue properties and satisfy biological constraints. Biomaterials 23:4095–4103
Zhang L, Rodriguez J, Raez J et al (2009) Biologically inspired rosette nanotubes and nanocrystalline hydroxyapatite hydrogel nanocomposites as improved bone substitutes. Nanotechnology 20:175101
Place ES, Evans ND, Stevens MM (2009) Complexity in biomaterials for tissue engineering. Nat Mater 8:457–470
Eisenbarth E, Velten D, Breme J (2007) Biomimetic implant coatings. Biomol Eng 24:27–32
Nicula R, Luthen F, Stir M et al (2007) Spark plasma sintering synthesis of porous nanocrystalline titanium alloys for biomedical applications. Biomol Eng 24:564–567
Dalby MJ, McCloy D, Robertson M et al (2006) Osteoprogenitor response to semi-ordered and random nanotopographies. Biomaterials 27:2980–2987
Dalby MJ, McCloy D, Robertson M et al (2006) Osteoprogenitor response to defined topographies with nanoscale depths. Biomaterials 27:1306–1315
Yim EK, Pang SW, Leong KW (2007) Synthetic nanostructures inducing differentiation of human mesenchymal stem cells into neuronal lineage. Exp Cell Res 313:1820–1829
Kundu AK, Putnam AJ (2006) Vitronectin and collagen I differentially regulate osteogenesis in mesenchymal stem cells. Biochem Biophys Res Commun 347:347–357
Franceschi RT, **ao G (2003) Regulation of the osteoblast-specific transcription factor, Runx2: responsiveness to multiple signal transduction pathways. J Cell Biochem 88:446–454
**ao G, Jiang D, Thomas P et al (2000) MAPK pathways activate and phosphorylate the osteoblast-specific transcription factor, Cbfa1. J Biol Chem 275:4453–4459
Keselowsky BG, Collard DM, Garcia AJ (2005) Integrin binding specificity regulates biomaterial surface chemistry effects on cell differentiation. Proc Natl Acad Sci U S A 102:5953–5957
Fu RH, Wang YC, Liu SP et al (2011) Differentiation of stem cells: strategies for modifying surface biomaterials. Cell Transplant 20:37–47
Uygun BE, Stojsih SE, Matthew HW (2009) Effects of immobilized glycosaminoglycans on the proliferation and differentiation of mesenchymal stem cells. Tissue Eng Part A 15:3499–3512
Benoit DS, Schwartz MP, Durney AR et al (2008) Small functional groups for controlled differentiation of hydrogel-encapsulated human mesenchymal stem cells. Nat Mater 7:816–823
Gorsline RT, Tangkawattana P, Lannutti JJ et al (2010) Accelerated chondrogenesis in nanofiber polymeric scaffolds embedded with BMP-2 genetically engineered chondrocytes. J Biomed Sci Eng 3:908–916
Anderson JM, Kushwaha M, Tambralli A et al (2009) Osteogenic differentiation of human mesenchymal stem cells directed by extracellular matrix-mimicking ligands in a biomimetic self-assembled peptide amphiphile nanomatrix. Biomacromolecules 10:2935–2944
Chen XD, Dusevich V, Feng JQ et al (2007) Extracellular matrix made by bone marrow cells facilitates expansion of marrow-derived mesenchymal progenitor cells and prevents their differentiation into osteoblasts. J Bone Miner Res 22:1943–1956
Bianco P, Robey PG (2001) Stem cells in tissue engineering. Nature 414:118–121
Quarto R, Mastrogiacomo M, Cancedda R et al (2001) Repair of large bone defects with the use of autologous bone marrow stromal cells. N Engl J Med 344:385–386
Vacanti CA, Bonassar LJ, Vacanti MP et al (2001) Replacement of an avulsed phalanx with tissue-engineered bone. N Engl J Med 344:1511–1514
Araki R, Uda M, Hoki Y et al (2013) Negligible immunogenicity of terminally differentiated cells derived from induced pluripotent or embryonic stem cells. Nature 494:100–104
Nazor KL, Altun G, Lynch C et al (2012) Recurrent variations in DNA methylation in human pluripotent stem cells and their differentiated derivatives. Cell Stem Cell 10:620–634
Meng X, Su RJ, Baylink DJ et al (2013) Rapid and efficient reprogramming of human fetal and adult blood CD34+ cells into mesenchymal stem cells with a single factor. Cell Res 23:658–672
Takahashi K, Yamanaka S (2006) Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell 126:663–676
Downing TL, Soto J, Morez C et al (2013) Biophysical regulation of epigenetic state and cell reprogramming. Nat Mater 12:1154–1162
Dellatore SM, Garcia AS, Miller WM (2008) Mimicking stem cell niches to increase stem cell expansion. Curr Opin Biotechnol 19:534–540
Thibault RA, Scott Baggett L, Mikos AG et al (2010) Osteogenic differentiation of mesenchymal stem cells on pregenerated extracellular matrix scaffolds in the absence of osteogenic cell culture supplements. Tissue Eng Part A 16:431–440
Berry FB, Mirzayans F, Walter MA (2006) Regulation of FOXC1 stability and transcriptional activity by an epidermal growth factor-activated mitogen-activated protein kinase signaling cascade. J Biol Chem 281:10098–10104
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer Science+Business Media New York
About this protocol
Cite this protocol
Quarto, R., Giannoni, P. (2016). Bone Tissue Engineering: Past–Present–Future. In: Gnecchi, M. (eds) Mesenchymal Stem Cells. Methods in Molecular Biology, vol 1416. Humana Press, New York, NY. https://doi.org/10.1007/978-1-4939-3584-0_2
Download citation
DOI: https://doi.org/10.1007/978-1-4939-3584-0_2
Published:
Publisher Name: Humana Press, New York, NY
Print ISBN: 978-1-4939-3582-6
Online ISBN: 978-1-4939-3584-0
eBook Packages: Springer Protocols