Abstract
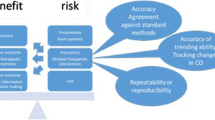
Thoracic electrical bioimpedance (TEB) is a non-invasive method used to evaluate beat-by-beat stroke volume (SV) and, when the heart rate (HR) is known, cardiac output (CO). Given the fact that in the electrical impedance signal it is easy to identify the start and end of systole, when an electrocardiographic signal is available this method can also be used for the beat-to-beat measurement of the left ventricular pre-ejection period (PEP), the left ventricular ejection time (LVET), and the PEP/LVET ratio (Weissler quotient), which is widely considered an excellent index for monitoring left ventricular contractility (Fig. 1).
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Preview
Unable to display preview. Download preview PDF.
Similar content being viewed by others
References
Kubiceck WG (1996) Development and evaluation of an impedance cardiac output system. Aerospace Med 12: 1208–1212
Sramek B (1982) Cardiac output by electrical impedance. Med Electronics 4: 93–97
Bernstein DP (1986) A new stroke volume equation for thoracic electrical impedance: theory and rationale. Crit Care Med 14: 904–909
Shoemaker WC, Howard Belzbere et al (1998) Multicenter study of non-invasive monitoring systems as alternatives to invasive monitoring of acutely ill emergency patients. Chest 114: 1643–1652
Young JD, Mc Quillón P et al (1993) Comparison of thoracic electrical bioimpedance and thermodilution for the measurement of cardiac index in patients with severe sepsis. Brit J Anaesth 70: 58–62
Jensen L, Yakimets J, Teo KK (1995) A review of impedance cardiography. Heart Lung 24: 183–193
Spiering W, Van Es PN, De Leeuw PW (1998) Comparison of impedance cardiography and dye dilution method for measuring cardiac output. Heart 79: 437–441
Stetz CW, Miller RG et al. (1982) Reliability of the thermodilution method in the determination of cardiac output in clinical practice. Am Rev Respir Dis 126: 1001–1004
Cropp GJA, Burton AC (1965) Theoretical considerations and model experiments on the validity of indicator dilution methods for measurements of variable flow. Circ Res 18: 26–48
Scheuer-Leeser M, Morguet A et al (1997) Some aspects to the pulsation error in blood-flow calculations by indicator-dilution techniques. Med Biol Eng Comput 15: 118–123
Mackenzie JD, Haites NE et al (1986) Method of assessing the reproducibility of blood flow measurements…factors influencing the performance of thermodilution cardiac out-put. Br Heart J 55: 14–24
Petros S, Engelmann L (2001) Validity of an abbreviated indirect calorimetry protocol for measurement of resting expenditures in mechanically ventilated and spontaneously breathing critically ill patients. Crit Care Med 27: 1164–1168
Bland JM, Altman GD (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet I: 307–310
Bland JM, Altman GD (1995) Comparing methods of measurement: why plotting difference against standard method in misleading. Lancet 346: 1085–1987
Van der Meer BJM, De Vries JPPM, Schreuder WO et al (1997) Impedance cardiography in cardiac surgery patients: abnormal body weight gives unreliable cardiac output measurements. Acta Anaesthesiol Scand 41: 708–712
Young GS, Mc Quillón P (1993) Comparison of thoracic electrical bioimpedance and thermo- dilution for the measurement of cardiac index in patients with severe sepsis. Br J Anaesth 70: 58–62
Shoemaker WC, Wo CC, Yu S et al (2000) Invasive and non invasive hemodynamic monitoring of acutely ill sepsis and septic shock patients in the emergency department. Eur J Emerg Med 7: 169–75
Tani H, Singer W, McPhee BR et al (2000) Splanchnic mesenteric capacitance in the posmral tachycardia syndrome (POTS). Anat Neurosci 86: 107–113
Rosenberg P, Yoncy CW (2000) Non invasive assessment of hemodynamics: an emphasis on bioimpedance cardiography. Curr Opin Cardiol 15: 151–155
Spiess BD, Patel MA, Soltow LO, Wright IH (2001) Comparison of bioimpedance versus thermodilution cardiac output during cardiac surgery: evaluation of a second generation bioimpedance device. J Cardiothorac Vase Anaesth 15: 567–573
Sargerman WS, Riffenpurgh RH, Spiess BD (2002) Equivalence of bioimpedance and thermodilution in measuring cardiac index after cardiac surgery. J Cardiothorac Vase Anaesth 16: 8–14
Garrard CL, Weissler AM, Dodge HT (1970) The relationship of alterations in systolic time intervals to ejection fraction in patients with cardiac disease. Circulation 11: 455
Marik PE, Pendelton JE, Smith R (1997) A comparison of hemodynamic parameters derived from transthoracic electrical bioimpedance with those parameters obtained by hemodilution and ventricular angiography. Crit Care Med 25: 1545–1550
Bonjer FM, Van Der Berg JW, Dirken NJ (1952) The origin of the variations of body impedance occurring during the cardiac cycle. Circulation 12: 415–420
Balestra B, Malacrida R, Leonardi L et al (1992) Esophageal electrodes allow precise assessment of cardiac output by bioimpedance. Crit Care Med 20: 62–67
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2003 Springer-Verlag Italia
About this paper
Cite this paper
Favaro, M., Allaria, B., Resta, M. (2003). Thoracic impedance tracing in perioperative hemodynamic monitoring: a technique to be revisited. In: Gullo, A. (eds) Anaesthesia, Pain, Intensive Care and Emergency Medicine — A.P.I.C.E.. Springer, Milano. https://doi.org/10.1007/978-88-470-2215-7_12
Download citation
DOI: https://doi.org/10.1007/978-88-470-2215-7_12
Publisher Name: Springer, Milano
Print ISBN: 978-88-470-0194-7
Online ISBN: 978-88-470-2215-7
eBook Packages: Springer Book Archive